Living with Sensory Processing Disorder (SPD) can be an overwhelming and isolating experience for both children and their families. Sensory processing challenges affect almost 80% of children born by C-section, making it a surprisingly common condition that often goes unrecognized and misunderstood.
For children with Sensory Processing Disorder, everyday experiences such as going to school, playing with friends, transitioning between activities, or even getting dressed and brushing their teeth can be a constant struggle due to their unique ways of perceiving and responding to sensory information.
While occupational therapists have worked with these sensory challenges for decades, many families still find themselves searching for answers when conventional approaches don’t address the underlying cause.
But what if there was a way to address the root cause of SPD and unlock your child’s full potential? In this article, we’ll explore the world of Sensory Processing Disorder, diving into its causes and signs, and how to support a child with SPD through the life-changing power of Neurologically-Focused Chiropractic Care.
What is Sensory Processing Disorder (SPD)?
Sensory integration is the neurological process of organizing sensory information from our bodies and environment so we can use it effectively in daily life. Sensory Processing Disorder is a condition that affects how children perceive and respond to sensory information in their environment. Children with SPD may struggle to process information from one or more senses and may exhibit a range of Sensory Processing Disorder symptoms.
Occupational therapists typically classify these challenges into three main types under what’s called Sensory Modulation Disorder, the most common pattern of SPD:
- Hypersensitivity (Over-responsiveness): Hypersensitive children can be easily overwhelmed by sensory input, such as loud noises, bright lights, or certain textures. They may react strongly to seemingly minor stimuli, like covering their ears in response to a vacuum cleaner.
- Hyposensitivity (Under-responsiveness): Some children with SPD may be under-responsive to sensory information, seeming to have a high tolerance for pain or a lack of awareness of their surroundings. They may not respond when called or may seem clumsy and uncoordinated.
- Sensory Seeking: Some children with SPD actively seek out sensory experiences, craving intense or repetitive stimulation. They may engage in behaviors like spinning, jumping, or crashing into objects, often to the point of disrupting daily activities or putting themselves at risk.
A second type, Sensory Discrimination Disorder, affects the ability to distinguish between different sensations or tell them apart. This can manifest as repeatedly dropping items, difficulty finding items in a backpack even when looking directly at them, difficulty distinguishing between textures, or being unable to tell where their body was touched without looking. There’s also a sensory-based motor condition that affects coordination and motor planning, which we’ll explore further when we discuss proprioception.

Autism Spectrum Disorder vs. SPD and the Impact on Daily Life
Autism Spectrum Disorder and SPD share similar attributes, particularly in how they present in daily life. Research shows that approximately 90% of children with Autism Spectrum Disorder experience sensory processing challenges. However, while sensory issues can be a sign of autism, SPD is its own condition, and it’s important to recognize its unique impact on a child’s life.
The key distinction is that children with SPD typically don’t exhibit the social communication difficulties, restricted interests, or repetitive behaviors that characterize Autism Spectrum Disorder. Kids with SPD often desperately want to engage socially but find it physically overwhelming to tolerate the sensory demands of group settings.
SPD can have a significant impact on various aspects of a child’s life, including:
- Learning and academic performance: Children with SPD may struggle to focus in class, have difficulty with fine motor skills such as handwriting, or become easily distracted by background noise or visual stimuli.
- Social interactions and relationships: Sensory issues can make it challenging for children to engage in play with peers, understand social cues, or cope with the sensory demands of group settings like birthday parties or crowded playgrounds.
- Emotional regulation and behavior: The constant challenges of processing sensory information can lead to frustration, anxiety, and meltdowns, making it difficult for children to manage their emotions and behavior.
- Motor coordination: Poor coordination and clumsiness are common in both SPD and autism, often stemming from disrupted proprioceptive feedback.
At the core of these challenges lies a complex interplay of neurological factors, including proprioception (the sense of body position) and mechanoreception (the sense of movement). When these systems are not functioning optimally, it can lead to the signs and struggles associated with SPD.
Fortunately, by understanding the unique nature and impact of sensory integration disorders and Autism Spectrum Disorder, parents can begin to recognize the unique signs of each in their own children and seek out the support and interventions needed to help them thrive.
Sensory Processing Disorder and ADHD
Sensory Processing Disorder and Attention Deficit Hyperactivity Disorder (ADHD) often co-occur, as both conditions involve challenges with regulating and responding to sensory input.
Children with ADHD may struggle with sensory modulation, leading to either sensory seeking or sensory avoidant behaviors, similar to those seen in SPD.
Research suggests that the underlying neurological imbalances and dysfunction that contribute to SPD may also play a role in the development of ADHD. In particular, dysregulation of the Autonomic Nervous System, known as dysautonomia, has been linked to both conditions. When the “fight or flight” response of the Sympathetic Nervous System becomes overactive, and the “rest and digest” response of the Parasympathetic Nervous System is underactive, it can lead to a state of chronic stress and hyperarousal that affects attention, impulse control, and sensory processing.
Additionally, the vagus nerve, a key component of the Parasympathetic Nervous System, has been implicated in both SPD and ADHD. Dysfunction of the vagus nerve can disrupt the balance between the sympathetic and parasympathetic branches, contributing to symptoms such as difficulty with self-regulation, emotional reactivity, and sensory processing challenges.
In short, the hallmark of ADHD is an overactive and easily distracted brain. That is exactly what sensory difficulties and subluxation do to a developing brain: they overwhelm it with “noise,” distracting it, keeping it off track, and overloading it with unnecessary sensory stimulation.
Addressing underlying neurological imbalances through approaches such as Neurologically-Focused Chiropractic Care can improve sensory integration, attention, and overall well-being for affected children.
The Eight Sensory Systems Involved in SPD
Most people learn about the five traditional senses in school: sight, hearing, touch, taste, and smell. But sensory processing actually involves eight interconnected sensory systems that work together to help us understand and navigate the world around us.
Understanding all eight sensory systems is key to understanding why SPD affects so many different areas of your child’s life:
- Visual system: How we process what we see, including brightness, colors, patterns, and movement
- Auditory system: How we process sounds, including volume, pitch, and the ability to filter background noise
- Tactile system: How we process touch sensations, including texture, temperature, pressure, and pain
- Olfactory system: How we process smells and distinguish between different scents
- Gustatory system: How we process tastes and textures in our mouths
- Vestibular system: The sense of balance and spatial orientation, located in the inner ear, that tells us where our head is in space and whether we’re moving or still
- Proprioception: The sense of body position and movement, knowing where your body parts are without looking at them
- Interoception: The sense of internal body sensations like hunger, thirst, heartbeat, need to use the bathroom, and emotional feelings in the body
When subluxation disrupts the neurological communication between these sensory systems and the brain, children struggle to accurately process sensory input from their environment. It’s like having static on a phone line; the messages are being sent, but they’re getting scrambled or distorted along the way.
The vestibular system and proprioception work closely together to support balance, coordination, and awareness of your body’s position in space. Interoception is often overlooked but incredibly important. Many kids with SPD struggle to recognize when they’re hungry, need the bathroom, or are getting overwhelmed emotionally because their internal sensation processing is off.
The Role of the Nervous System in Sensory Processing
To truly understand Sensory Processing Disorder, it’s essential to explore the intricate workings of the nervous system and how imbalances can lead to the challenges children with SPD face.
The nervous system is the body’s command center, responsible for receiving, interpreting, and responding to sensory input from the environment. In typically developing children, this process occurs seamlessly, allowing them to navigate the world around them with ease.
However, when the nervous system is not functioning optimally, as in the case of SPD, neural processing is disrupted, leading to symptoms and signs of the disorder, such as sensory overload. Altered brain activity patterns make it difficult for the brain to filter, organize, and respond appropriately to incoming sensory information.
Proprioception and Sensory Processing Disorder
Proprioception, the sense of body awareness, movement, and position in space, is crucial in sensory integration and overall neurological development in kids.
Proprioception refers to the body’s ability to sense its position and movement in space, which is crucial for tasks like balance, coordination, and motor control. This significant portion of brain function involves multiple areas, including the motor cortex, cerebellum, and sensory cortex, which work together to ensure smooth, precise movement.
A significant portion of the brain’s function is dedicated to proprioception and movement coordination. This means that when proprioceptive input is distorted by subluxation and dysautonomia, it can easily distract and confuse other brain functions, leading to behavioral and emotional dysregulation, difficulty paying attention, and more.
This crucial component of sensory processing becomes easier for parents to understand when we consider how our brains function when we are overwhelmed and overloaded at work, stuck sitting at our desks or in traffic for hours, or juggling an overwhelming, chaotic schedule to keep up with all of life’s demands.
When your brain becomes overloaded, distracted, and anxious, but then you go for a walk or hit the gym for a good workout, how does it make you feel? More relaxed, calm, and focused, right? That is the impact of proprioception and movement stimulation to our brain. It’s calming, regulating, and organizing.
In short, children struggling with Sensory Processing Disorder need to prioritize movement stimulation and optimize proprioceptive input to their overwhelmed and distracted brains to get things back on track. This is why most SPD kids are recommended to begin Occupational Therapy (OT) and other movement-based therapies. But so often, if subluxation and nervous system dysfunction are present, the benefits of OT are going to be limited rather than optimized.
Dysautonomia and Subluxation: An Imbalance in the Autonomic Nervous System
One of the primary culprits behind neurological dysfunction in SPD is a condition called subluxation. Subluxation refers to altered neurosensory function due to reduced movement and proprioceptive input, specifically from the upper neck and throughout the entire neurospinal system, which interferes with proper neurological communication. When subluxation occurs, it can disrupt the flow of sensory information, making it difficult for the brain to interpret and respond accurately to incoming stimuli.
The most common type of sensory input altered by subluxation is called sensorimotor input, which controls both gross and fine motor tone, coordination, and overall function. This is why birth trauma and subluxation are commonly linked to both developmental delays and the most common presentations of SPD, since they directly alter this vital neurodevelopmental function.
Another critical factor in the neurological origins of SPD is dysautonomia, which refers to an imbalance in the Autonomic Nervous System (ANS). The ANS consists of two branches:
- The Sympathetic Nervous System, responsible for the “fight or flight” response
- The Parasympathetic Nervous System, which promotes “rest and digest” functions.
In children with SPD, the Sympathetic Nervous System is often stuck in overdrive, leading to a constant state of heightened arousal and sensitivity to sensory input. At the same time, the Parasympathetic Nervous System may be underactive, making it difficult for the child to relax, regulate their emotions, and process sensory information effectively.
The Vagus Nerve: A Vital Player in Sensory Processing
The vagus nerve, the longest and most complex of the cranial nerves, plays a crucial role in regulating the Autonomic Nervous System and, consequently, in sensory processing. This nerve acts as a major communication highway between the brain and various organs, including the digestive system, heart, and lungs.
When the vagus nerve functions optimally, it promotes calm and relaxation, helping children process sensory information. However, dysfunction can lead to overactivation of the sympathetic nervous system and underactivation of the parasympathetic nervous system, worsening sensory processing difficulties.
By understanding the neurological underpinnings of SPD, including the roles of subluxation, dysautonomia, and the vagus nerve, parents can begin to appreciate the complexity of their child’s challenges and the importance of addressing these underlying imbalances.
“The Perfect Storm” of Factors That Cause Sensory Overload
In many cases, the development of Sensory Processing Disorder can be traced back to a combination of factors that, when occurring together, create a “Perfect Storm” of neurological dysfunction and sensory overload.
This concept highlights the multifaceted nature of SPD and the importance of considering a child’s unique experiences and circumstances when understanding and addressing their challenges.
Some of the key factors that can contribute to the development of SPD include:
- Prenatal stress and maternal health: Prenatal stress during pregnancy can have a profound impact on fetal brain development, potentially setting the stage for neurological imbalances that may later manifest as problems with sensory input.
- Birth trauma and interventions: Birth complications during labor and delivery, such as prolonged labor, forceps or vacuum extraction, or cesarean section, can cause physical and neurological stress to the infant, increasing the risk of subluxation and dysautonomia. Additional risk factors include premature birth, which can affect nervous system development.
- Early life stressors and environmental factors: Exposure to toxins, nutritional deficiencies, or emotional stress in the early years of life can further compromise a child’s neurological development and exacerbate sensory processing difficulties.
By understanding the complex interplay of these elements, parents and practitioners can work together to develop targeted interventions that address the root causes of a child’s sensory processing difficulties.
How is Sensory Processing Disorder Assessed?
Occupational therapists typically evaluate SPD using standardized assessment tools, such as the Sensory Profile questionnaire, and clinical observation of how children respond to various sensory experiences. These assessments help identify specific patterns of sensory responsiveness and determine which sensory systems are most affected.
While SPD isn’t included in the Diagnostic and Statistical Manual as a standalone diagnosis, this doesn’t diminish the very real neurological challenges these children face. The lack of official recognition often makes it harder for families to get insurance coverage for therapy, but it doesn’t change the fact that these kids are struggling with genuine nervous system dysfunction.
The PX Docs Approach to Resolving Sensory Issues in Kids
In addition to Neurologically-Focused Chiropractic Care, we recognize that occupational therapy and sensory integration therapy can provide valuable support for children with SPD. These therapeutic interventions help kids develop coping strategies and adapt to sensory challenges. However, if the underlying nervous system dysfunction isn’t addressed first, these therapies often plateau or provide only limited benefit.
At PX Docs, we recognize the critical role that neurological function plays in a child’s overall health and well-being, particularly in the context of Sensory Processing Disorder. Our unique approach, Neurologically-Focused Chiropractic Care, addresses the underlying imbalances and dysfunction that contribute to SPD, providing families with a safe and drug-free path to healing.
Neurologically-Focused Chiropractic Care differs from traditional chiropractic approaches in its specific focus on the nervous system and its relationship to sensory processing. Our doctors undergo extensive training in pediatric neurology and the latest research on SPD, enabling them to develop highly targeted, individualized care plans for each child.
Central to our approach is the use of INSiGHT Scans to determine the precise areas requiring adjustments to address subluxation and dysautonomia. By restoring proper sensory input and balance to the nervous system, we help optimize neurological function and improve the brain’s ability to process and integrate sensory information.
It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for Sensory Processing Disorder or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
Below is an image with a series of three Sensory EMG Scans performed on a child struggling with Sensory Processing Disorder, ADHD, and Anxiety. The first scan on the far left shows that this child’s sensory and proprioceptive systems are entirely overwhelmed and “stuck on” sympathetic overdrive, as evidenced by all the red bars indicating this stuck sensory overload. Then, as care progresses in the middle and far-right scans, you can see his nervous system become much calmer and more sensory-regulated (white and green bars only).
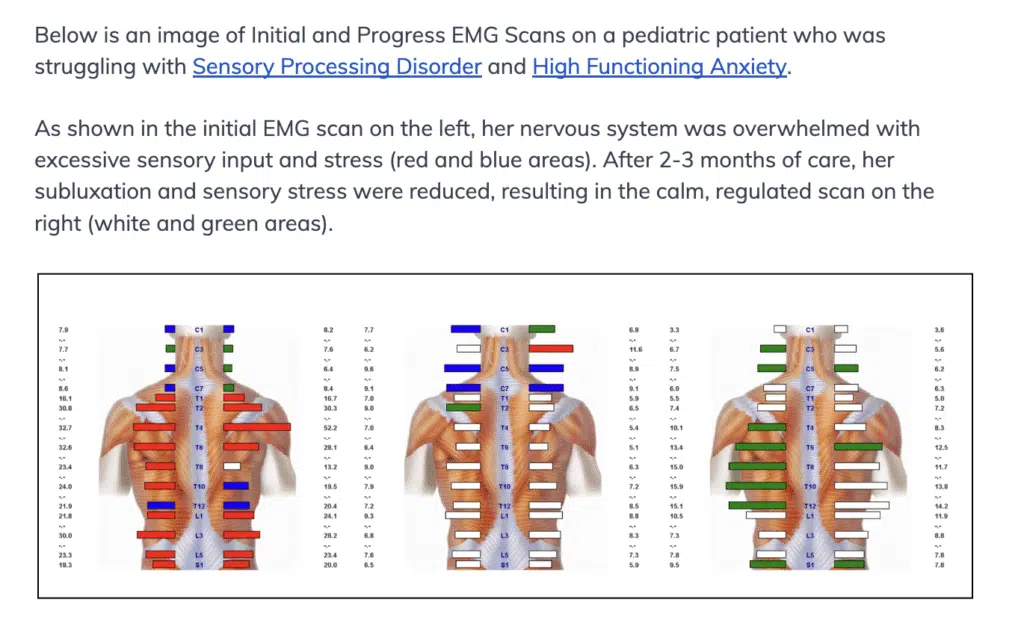
These positive changes on EMG indicate that his subluxation and dysautonomia were vastly improved, and his nervous system is now much calmer, balanced, and regulated. With these functional changes and improvements to his sensory processing and overall nervous system function, this patient experienced far fewer meltdowns and overwhelm, and began to show vastly improved focus, concentration, and emotional regulation during transitions and busy days.
Benefits of Neurologically-Focused Chiropractic Care for Children with Sensory Processing Disorder
Children who receive Neurologically-Focused Chiropractic Care at PX Docs often experience significant improvements in their sensory processing abilities, as well as a range of other benefits, including:
- Enhanced nervous system regulation and resilience
- Improved ability to self-regulate emotions and behavior
- Better sleep, digestion, and immune function
- Increased focus, attention, and learning ability
- Improved motor coordination and body awareness
- Enhanced brain function and processing speed
- Greater confidence and overall well-being
By addressing the root causes of sensory issues in kids and supporting healthy nervous system development, our approach empowers them to overcome challenges and thrive in all aspects of their lives.
Practical Support Strategies for Sensory Processing Challenges
While addressing the root neurological cause through Neurologically-Focused Chiropractic Care is essential, these practical accommodations can help manage sensory overload in daily life:
Sensory tools that can help:
- Weighted blankets or compression clothing for calming deep pressure input
- Noise-canceling headphones for auditory sensitivities
- Fidget tools to provide movement input during seated activities
- Chewy jewelry or gum for oral sensory input
- Sunglasses for light sensitivity
Environmental modifications:
- Dimmed lighting in overwhelming spaces
- Quiet spaces for sensory breaks
- Reduced visual clutter in bedrooms and play areas
- Predictable routines to reduce anxiety about transitions
Many occupational therapists recommend what’s called a sensory diet, a personalized schedule of therapeutic activities that provide the sensory input your child’s nervous system needs throughout the day. This might include movement breaks, heavy work activities like pushing or pulling, or calming activities like swinging.
These strategies help manage the signs while you address the underlying nervous system dysfunction through chiropractic care. Think of them as helpful tools that work even better once the foundation is solid, when subluxation is corrected, and the nervous system can regulate properly. Your child will need fewer accommodations because they’re actually processing sensory information correctly.
Logan’s Story: A Sensory Success Story
Logan’s parents exhausted every traditional therapy and method to help calm his sensory storm and assist him in managing his emotions, behavior, and sensory cues.
From infancy, Logan struggled with sensory processing issues, contrary to what his pediatrician had assured his parents. His sensory nervous system continued to develop into stress, dysfunction, and everyday challenges. Eventually, his parents discovered the “Perfect Storm” work and learned about the true causes of Sensory Processing Disorder.
They were able to naturally calm Logan’s sensory storm without resorting to drugs or traditional therapies such as PT, OT, and Speech Therapy.
Today, Logan is thriving, excelling in school, and living his best life.
Empowering Families to Embrace Hope and Healing
For parents of children with Sensory Processing Disorder, the journey can often feel overwhelming and isolating. But at PX Docs, we want you to know you are not alone and that there is hope for your child and your family.
If you suspect your child may be struggling with sensory issues or if you have been searching for answers and solutions, we invite you to visit the PX Docs Directory and find a qualified practitioner in your area.
With the right support and intervention, your child can overcome their challenges and unlock their full potential, and your family can experience the joy, connection, and well-being you deserve.