If you’ve been told your child is just being naughty when they crash into walls, spin for hours without getting dizzy, or seem not to hear you calling their name…you’re not alone. What looks like attention-seeking or deliberate defiance might actually be hyposensitivity, a neurological condition where the sensory system is stuck on “low volume,” leaving kids constantly searching for more input just to feel normal.
Studies estimate that up to 16% of children have sensory processing issues, and while hypersensitivity gets most of the attention, under-responsivity changes kids’ lives too. Children with hyposensitivity aren’t being difficult on purpose; their nervous systems simply aren’t getting the sensory feedback they need to regulate their bodies and behavior. In this article, we’ll cover how to identify hyposensitivity, why it develops neurologically, and what actually helps.
What is Hyposensitivity?
Hyposensitivity is a condition in which the nervous system responds less to sensory information around it. It’s also known as sensory underresponsivity, which means that there’s a decreased sensitivity to sensory input.
Hyposensitivity is a common occurrence in children with Autism Spectrum Disorder. Kids with hyposensitivity are literally “under-responsive to sensory stimuli,” their nervous systems have a higher sensory threshold, meaning they need more intense input before their brains register that something is happening. Think of it like their sensory volume is turned way down, so they’re constantly trying to turn it up by seeking more and more stimulation.
Many kids experience difficulties processing sensory information at times. For some children, sensory input is too much, leading them to become hypersensitive. On the other hand, for others, the sensory input isn’t enough, and they become hyposensitive. Both of these conditions are two sides of one issue: problems with sensory modulation, which is the nervous system’s ability to regulate responses to sensory input.
Established research indicates that 1 in 6 kids in the U.S. struggles to process sensory input. Hyposensitivity falls under this sensory integration dysfunction and represents a fundamental problem with how the Autonomic Nervous System regulates sensory information. This complex pattern of differences in sensory processing is why a comprehensive neurological assessment is so important.
Hyposensitivity vs. Hypersensitivity: What’s the Difference?
Parents often confuse these two conditions because they sound similar and both involve sensory processing challenges. But they’re actually opposite problems with very different behaviors.
Hypersensitivity (sensory over-responsivity) happens when a child’s nervous system reacts too strongly to sensory input. These kids experience sensory avoidance—they try to escape or minimize exposure to certain stimuli because everything feels too intense. A child with hypersensitivity might:
- Cover their ears in moderately loud environments
- Refuse to wear certain clothing textures
- Become overwhelmed in crowded or bright spaces
- Avoid messy play or certain food textures
- Have meltdowns when their routine changes
Hyposensitivity (sensory underresponsivity), on the other hand, occurs when a child’s nervous system doesn’t respond strongly enough to sensory input. These kids display sensory seeking behavior; they actively pursue intense sensory experiences because normal levels of input don’t register. A child with hyposensitivity might:
- Crash into furniture and people
- Seek out loud noises and play music at maximum volume
- Have a high pain threshold and not react to injuries
- Constantly touch everything and everyone
- Never seem to sit still or settle down

The key difference: Hypersensitive kids are trying to get away from sensory input. Hyposensitive kids are trying to get more of it.
Here’s where it gets complicated: many children, especially those with Autism Spectrum Disorder, show both patterns across different sensory systems. Your child might be hypersensitive to sounds but hyposensitive to touch. This mixed presentation is actually quite common and points to overall nervous system dysregulation rather than a simple sensory preference.
Traits of Hyposensitivity
To understand hyposensitivity, we need to recognize that children may experience everyday sights, sounds, smells, and textures differently from adults. What seems strong to adults may be weak and lifeless to their systems. But this isn’t just about perception; it’s about how their nervous system processes and responds to sensory information.
Hyposensitivity can affect any of the eight sensory systems: visual, auditory, olfactory (smell), gustatory (taste), tactile (touch), vestibular (balance and movement), proprioceptive (body awareness), and interoceptive (internal body signals). Each child’s pattern is unique, but here are the most common presentations:
Hearing Hyposensitivity
Many kids with Sensory Processing Disorder have difficulties with sound processing. But unlike hypersensitive kids, these children tune out noises around them. Common traits of auditory hyposensitivity include:
- Ignoring their name being called
- Needing directions repeated frequently
- Loving making loud noises like stomping feet
- Unable to locate where sounds come from
Smell Hyposensitivity
Other children with hyposensitivity notice that the scents barely register for kids with smell hyposensitivity. These kids might:
- Sniff people or objects to engage with them
- Crave extreme foods like onions or vinegar
- Struggle telling smells apart
Vision Hyposensitivity
The world appears visually bland for a child with vision hyposensitivity. A child with visual sensory-seeking may struggle with:
- Spotting specific things, among others
- Tracking moving stuff like balls
- Judging distance and depth
Balance Hyposensitivity
The world may seem flat and stationary to children who lack sensory input about their body position. As they seek lots of movement, kids with balance hyposensitivity tend to enjoy:
- Spin, swing, or bounce for long periods without dizziness
- Flip upside down frequently
- Always be in motion
When nerves don’t get enough sensory feedback, children seek stimulation through sight, sound, smell, touch, and movement without realizing their brains and bodies need it.
Touch Hyposensitivity
Children with tactile hyposensitivity have a decreased response to touch, temperature, and pain, which can be dangerous. They may not flinch when touching something hot or notice when they’re injured. They often:
- Prefer tight clothing or heavy blankets
- Tend to mouth non-food items
- May be mistaken for bullies because their touch is too intense for others.
In severe cases, some engage in self-injurious behaviors not because they want to hurt themselves, but because they genuinely can’t feel it the way others would.
Proprioception Hyposensitivity
Proprioception is the body’s awareness of where it is in space and how much force it’s using. Kids with proprioceptive hyposensitivity:
- Frequently bump into furniture and people
- Struggle to judge their own strength
- Often have poor handwriting because they can’t gauge pressure.
They constantly shift positions because they can’t “feel” their body unless it’s moving, and are drawn to heavy work like pushing or carrying because the joint compression gives them the input they need.
Interoception Hyposensitivity
Interoception covers awareness of internal signals—hunger, thirst, needing the bathroom, and emotional states. Children with interoceptive hyposensitivity struggle to recognize these cues, which means they may:
- Not notice hunger
- Miss bathroom signals until it’s an emergency
- Fail to identify their own emotions.
Since interoception is the foundation of self-regulation, this is often why sensory processing issues and emotional dysregulation go hand in hand.
Many children display a mix of hyper- and hyposensitivity across different systems. A child might be hyposensitive to touch while being hypersensitive to sound. This is why a comprehensive neurological assessment matters.
How Hyposensitivity Affects Daily Life
For parents, it’s easy to focus on individual behaviors—the crashing, the loudness, the apparent defiance. But what we’re actually seeing is a child whose nervous system is stuck in constant search mode, desperately seeking the sensory input needed just to feel regulated and normal.
At home, hyposensitivity can create constant tension. Your child may:
- Break things “accidentally” because they can’t gauge their strength
- Hurt siblings during play without understanding why everyone’s upset
- Refuse to come to dinner because they don’t feel hungry
- Have bathroom accidents because they didn’t notice the signals
- Wake up multiple times at night seeking movement or pressure input
- Struggle with basic self-care like brushing teeth or washing because they can’t feel when it’s “enough.”
At school, these children often face misunderstanding and punishment. Teachers may describe them as:
- “Always out of their seat.”
- “Can’t keep their hands to themselves.”
- “Disruptive and attention-seeking.”
- “Not listening” or “refusing to follow directions.”
But here’s the truth: these children aren’t being defiant. Their nervous systems are literally not receiving the sensory information they need to sit still, gauge appropriate touch, or process verbal instructions at normal volumes.
Socially, hyposensitivity can be isolating. Other children may:
- Avoid your child because their hugs hurt or they’re “too rough.”
- Not understand why your child is “always in their face.”
- Misinterpret sensory-seeking behaviors as aggression or weirdness
The emotional toll on both child and parent can’t be overstated. Many parents tell us they feel like they’ve tried everything—occupational therapy, sensory diets, behavior charts, consequences—and nothing creates lasting change. That’s because these interventions, while helpful, often don’t address the root neurological dysfunction driving the sensory seeking.
The “Perfect Storm” of Sensory Disruption
Hyposensitivity develops early due to overwhelming stressors during childhood, known as the “Perfect Storm.” This isn’t a single event causing the problem; it’s a cascade of stressors hitting the developing nervous system during critical developmental windows.
Prenatal Stress
The “Perfect Storm” begins even before birth, when a mom’s emotional or physical stress, infections, inflammation, or toxins can affect the baby’s growing brain and nerves, making them extra sensitive. Prenatal stress affects how the baby’s Autonomic Nervous System develops—specifically the balance between the sympathetic (“gas pedal”) and parasympathetic (“brake pedal”) branches. Research links pregnancy issues to many neurological issues, including higher sensory dysfunction in kids later on.
Think of it this way: if the baby’s developing nervous system is stuck with the gas pedal pressed down due to maternal stress, infections, or inflammation, that “sympathetic dominance” pattern gets locked in before birth. This establishes a baseline of dysregulation that shapes how the child processes sensory information once they’re born.
Birth Trauma
Established research proves there’s a link between cesarean delivery and other birth trauma with the neurological development of infants. Medical interventions, restricted positioning during labor, or traumatic deliveries can damage the delicate nerve pathways—especially in the upper cervical spine where the brainstem meets the spinal cord. This can cause issues like Autism Spectrum Disorder, Sensory Processing Disorder, and other neurological problems like ADHD.
These issues can result in the emergence of neurological irritation areas called subluxation. A subluxation is misalignment, fixation, and neurological interference in the spine that disrupts communication between the brain and the body by placing abnormal stress on the nervous system. This disruption can lead to dysautonomia, an imbalance in the Autonomic Nervous System (ANS) that impairs essential bodily functions, including heart rate, digestion, respiratory control, and, critically, sensory processing and regulation.
Environmental Stress
After birth, recurring issues such as ear infections and overuse of antibiotics can put additional strain on the system. Other factors like exposure to harmful chemicals, poor diet, chronic inflammation, or ongoing emotional stress continue to push the nervous system further into dysfunction. Each stressor adds another layer of interference, making it harder and harder for the child’s sensory systems to process information accurately.
By the time parents notice the sensory-seeking behaviors—the crashing, the loud noises, the inability to sit still—the nervous system has been under stress for months or even years. The combination of these events creates a “Perfect Storm” that can lead to neurological hyposensitivity.
Here’s the key insight most practitioners miss: hyposensitivity isn’t a behavioral problem or even primarily a sensory problem; it’s a nervous system regulation problem. When the Autonomic Nervous System is stuck in sympathetic dominance (gas pedal down, brake pedal not working), the child’s ability to modulate and process sensory input breaks down.
Getting to the Roots: Specialized Neurological Care
While occupational therapy, physical therapy, and counseling can help manage hyposensitivity symptoms, they often plateau because they don’t address the underlying cause. If there’s interference in the nervous system itself, specifically, subluxation causing dysautonomia, sensory strategies alone won’t fully restore function. It’s like adjusting your TV’s brightness when the cable connection is faulty. Until you fix the connection, you won’t get a clear picture.
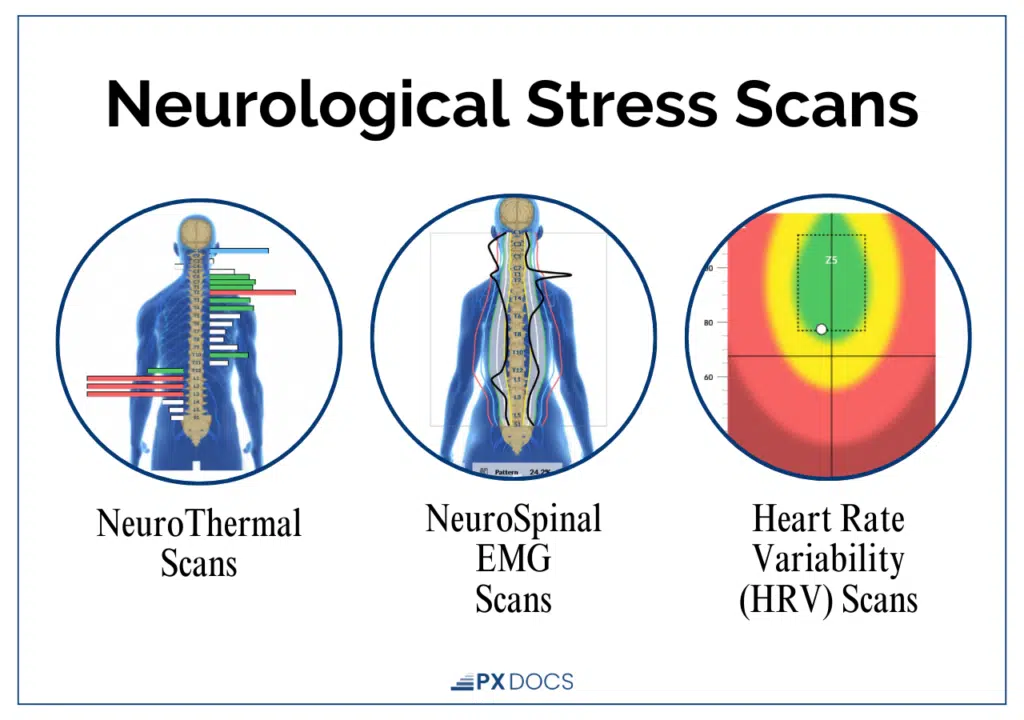
PX Docs use INSiGHT Scans to objectively detect these patterns, giving parents clarity about what’s actually driving their child’s sensory issues rather than guessing. The technology includes three types of scans, each measuring a different aspect of nervous system function:
- NeuroThermal Scans measure temperature differences along the spine that indicate Autonomic Nervous System dysfunction. In children with hyposensitivity, these scans often reveal patterns of sympathetic dominance—the “gas pedal” stuck down—in specific regions that correspond to their sensory challenges.
- NeuroCORE EMG Scans assess electrical activity in muscles along the spine, revealing areas of tension, asymmetry, and neurological disorganization. For hyposensitive children, these scans are particularly telling—they often show excessive muscle tension and poor proprioceptive feedback patterns, especially in the upper cervical and mid-thoracic regions, which explains why these kids struggle with body awareness and coordination.
- Heart Rate Variability (HRV) Scans evaluate the balance between the sympathetic and parasympathetic nervous systems. Low HRV indicates poor nervous system adaptability and regulation—a hallmark finding in children with sensory processing issues.
What makes these scans especially valuable is that they detect neurological changes before you see behavioral improvements. Nervous system healing happens from the inside out—the brain and nerves restore proper function first, then the body learns to express that new regulation in everyday life.
Through gentle, specific adjustments to areas of subluxation—particularly in the upper cervical area—Neurologically-Focused Chiropractic Care restores proper communication between the brain and body. These aren’t aggressive adjustments; they use light touch, about the pressure you’d use to check a tomato for ripeness. When subluxation is reduced, and dysautonomia begins to resolve, families typically see:
- Improved sensory modulation—less need to seek intense input
- Better body awareness and coordination as proprioceptive function improves
- Decreased crashing, banging, and rough physical behaviors
- Improved emotional regulation and longer ability to sit still
- Better interoceptive awareness—recognizing hunger, bathroom needs, and rising emotions
- Improved sleep as the nervous system shifts into parasympathetic “rest and restore” mode
The goal is to remove the neurological interference that’s preventing the sensory systems from working properly in the first place.
First Steps Forward
If your child constantly seeks stimulation, crashes into things, doesn’t seem to feel pain normally, or exhibits possible hyposensitivity challenges, it may be a good idea to get an assessment from a Neurologically-Focused Pediatric Chiropractor.
Check out the PX Docs Directory, which connects families to PX Docs’ global network, to find the right specialist for your child. The answers you’re looking for, and the lasting change you’ve been hoping for, await you.
Your child’s sensory-seeking behaviors aren’t defiance or bad behavior. They’re a cry for help from a dysregulated nervous system, desperate for the input it needs to function. Let’s answer that cry by addressing the root cause and giving your child’s nervous system the support it needs to heal.