An estimated 70 million people worldwide are living with dysautonomia, a disorder of the Autonomic Nervous System that disrupts everything from heart rate and blood pressure to digestion, temperature regulation, and even immune function.
For teenagers like Francesca, this invisible illness turned daily life into a constant battle against seizures, insomnia, anxiety, depression, constipation, and autoimmune issues. Francesca’s journey began at age seven when she was diagnosed with absence seizures and prescribed epilepsy medications, which she would continue to take for the next seven years. As she entered her teenage years and faced increasing stress from school and life, her seizures worsened, eventually escalating to grand mal seizures.
Unfortunately, Francesca’s story is not unique. This is the reality for millions of children and families struggling with dysautonomia and orthostatic intolerance—conditions that affect the body’s automatic control systems. While Postural Orthostatic Tachycardia Syndrome (POTS) is one of the most commonly discussed types, affecting approximately 1 in 100 teenagers in the United States, dysautonomia encompasses many different conditions that all share a common thread: dysfunction of the body’s automatic control systems.
Additionally, we now know that dysautonomia plays a major role in the development of Autism Spectrum Disorder, Sensory Processing Disorder, PANDAS/PANS, anxiety, and even such common conditions as constipation and digestive conditions.
In this article, we’ll explore dysautonomia, its effects on children and teens, and the unique approach to care offered by PX Docs’ Neurologically-Focused Chiropractic Care. The goal is to empower parents and caregivers with the knowledge and resources they need to advocate for their child’s health.
What is Dysautonomia?
To grasp the complexities of dysautonomia, it’s important to first understand the Autonomic Nervous System (ANS) and its critical role in nervous system regulation and maintaining overall health and well-being. The ANS is responsible for controlling involuntary functions such as heart rate, blood pressure, digestion, and temperature regulation—all functions that occur automatically without our conscious control.
This incredibly intricate system goes far beyond basic physiological functions and also plays a role in immune system activation and regulation, controlling inflammation, generating speech and communication, processing and integrating sensory information, and even regulating our behavior and emotions.
The ANS consists of two main branches that work together to keep our bodies functioning optimally:
- The Sympathetic Nervous System (SNS): Often referred to as the “fight or flight” response, the SNS activates during times of stress or perceived danger. It increases heart rate and blood pressure and diverts blood flow to the muscles, preparing the body for action.
- The Parasympathetic Nervous System (PNS): Known as the “rest, regulation, and digestion” response, the PNS helps the body conserve energy and recover after periods of stress. It slows heart rate, promotes digestion, and facilitates relaxation.
In a healthy individual, the sympathetic and Parasympathetic Nervous Systems work together seamlessly, responding to internal and external stimuli to maintain balance.
However, in children with dysautonomia, this delicate balance is disrupted, leading to a wide range of symptoms and challenges.

Why Is Dysautonomia So Prevalent Today?
Unfortunately, for the past couple of generations, we’ve allowed chronic stress, anxiety, and toxicity to invade our culture like never before.
Never before have our families been exposed to such unrelenting levels of stress and tension, as well as a daily bombardment of toxic chemicals that come from every component of our environment, such as our food supply, air pollution, contaminated water, cleaning and other household supplies, makeup, clothing, vaccinations, medications, and more.
For example, studies show that when a woman is exposed to chronic stress even before conception, it can negatively affect the self-regulation and stress resilience of her offspring far down the road, even generationally.
Established studies have shown that high amounts of stress and anxiety during pregnancy lead to a “shared supply” of stress and tension going to the fetus and the developing baby’s brain and nervous system, increasing their risk of everything from autism to asthma to obesity later on in life. Additional studies demonstrate that when mothers experience prenatal stress, cortisol crosses the placenta, affecting the developing baby.
Then from there we now know that birth interventions and physical trauma to the delicate brainstem and neurospinal regions of the infant from things like forceps, vacuum extraction, induction, and c-section can damage the vagus nerve and disrupt autonomic function as well, triggering dysautonomia in infants and leading to a cascade or “Perfect Storm” of downstream neurophysiological effects and chronic health conditions in kids.
By far and away, the most overlooked aspect of chronic health challenges in kids is dysautonomia. And in turn, the most overlooked and easily missed trigger of this neurological storm and imbalance is birth trauma.
The Different Types of Dysautonomia
Dysautonomia is a term used to describe several different conditions that share a common thread: a malfunctioning Autonomic Nervous System. When the ANS is not functioning properly, it can disrupt heart rate, blood pressure, digestion, temperature regulation, and other essential functions.
Dysautonomia conditions can be classified as primary, secondary, or idiopathic:
- Primary dysautonomia means the autonomic dysfunction is the main disease process itself. This includes rare genetic conditions like familial dysautonomia (also called Riley-Day syndrome), which affects the development of sensory and autonomic nerves.
- Secondary dysautonomia results from another underlying condition. Many children develop autonomic dysfunction secondary to conditions like diabetes, autoimmune conditions, Ehlers-Danlos syndrome, Chiari malformation, or even infections.
- Idiopathic dysautonomia means the root cause is unknown—and this describes the majority of cases we see in children today.
Some common examples of dysautonomia include:
- Postural Orthostatic Tachycardia Syndrome (POTS): A condition characterized by a rapid increase in heart rate upon standing, often accompanied by dizziness, fatigue, and shortness of breath. Studies suggest POTS affects approximately 1 in 100 teenagers in the United States.
- Neurocardiogenic Syncope (NCS): A condition that causes sudden drops in blood pressure, called orthostatic hypotension, leading to fainting or near-fainting episodes.
- Gastroparesis: A condition in which the stomach takes too long to empty, causing nausea, vomiting, and bloating.
- Multiple System Atrophy (MSA): This condition is caused by a progressive death of certain nerve cells in the brain and spinal cord, and can cause a person to suddenly lose their balance, become stiff, have a tremor, or even faint.
While those conditions are the most commonly discussed conditions linked to dysautonomia in the conventional medical world today, we now know that dysautonomia plays a significant role in much more common childhood conditions such as autism, sensory challenges, seizures, autoimmune conditions (allergies, asthma, etc.), PANS/PANDAS, and so much more.
The Role of the Vagus Nerve in Autonomic Regulation
One of the most important components of the Autonomic Nervous System is the vagus nerve, a long, wandering nerve that extends from the brainstem to the abdomen. The vagus nerve plays a crucial role in regulating many of the body’s vital functions, including heart rate, digestion, and immune response. We now know that the vagus nerve also plays a crucial role in regulating inflammation and our social, emotional, and behavioral functions.
When functioning properly, the vagus nerve helps to promote relaxation and recovery by activating the Parasympathetic Nervous System. However, when it is not working optimally, it can contribute to the development of dysautonomia and its associated symptoms.
Research has shown that stimulating the vagus nerve through techniques such as deep breathing, meditation, and Neurologically-Focused Chiropractic adjustments can help to improve autonomic function and reduce the signs of dysautonomia.
What Causes Dysautonomia?
One word—stress.
We live in a world absolutely overrun by stress, and simply put, consistent exposure to stress is the leading cause of dysautonomia. But the story of stress is not just for us adults and parents. Our kids are exposed to more stress, tension, toxicity, and anxiety than ever before. And they are exposed to it earlier than ever before.
The “Perfect Storm” of Dysautonomia
At PX Docs, we often refer to the “Perfect Storm” concept when discussing the underlying causes of dysautonomia and other chronic health conditions in children. This concept suggests that a combination of factors, often beginning early in life, can create a cascading effect that leads to the development of dysautonomia and related challenges.
The three main components of “The Perfect Storm” include:
- Prenatal stress: Maternal stress during pregnancy can impact the child’s developing nervous system by affecting the fetus through the release of stress hormones, potentially increasing the risk of dysautonomia later in life.
- Birth interventions and trauma: Complications during labor and delivery can cause physical trauma to the infant’s nervous system and specifically the brainstem and vagus nerve regions, potentially leading to neural miscommunication, which is critical for autonomic regulation.
- Early childhood stressors: Exposure to stress during early years can impact a child’s developing Autonomic Nervous System, potentially leading to symptoms of dysautonomia.
- Overuse of antibiotics and exposure to toxins: In today’s over-medicalized and industrialized world, even our infants and toddlers are exposed to excessive amounts of toxins, chemicals, and medications, especially antibiotics.
Other Potential Causes and Risk Factors of Dysautonomia
In addition to “The Perfect Storm” factors, several other potential causes and risk factors have been identified for dysautonomia, including:
- Familial dysautonomia from genetic factors: Some research suggests that certain genetic variations may increase an individual’s susceptibility to developing familial dysautonomia. While there is no single ‘dysautonomia gene,’ studies have identified several genetic markers that are more common in people with autonomic dysfunctions.
- Autoimmune conditions: Dysautonomia is linked to autoimmune dysfunctions like PANS/PANDAS, lupus, rheumatoid arthritis, and Multiple Sclerosis (MS), in which the immune system mistakenly attacks healthy nerve cells, causing damage to the Autonomic Nervous System.
- Chronic illnesses: Certain chronic health conditions, such as diabetes, Lyme disease, and Parkinson’s disease, are often accompanied by signs of dysautonomia. These conditions can damage the nerves and blood vessels that regulate autonomic function, leading to dysautonomia symptoms.
- Ehlers-Danlos syndrome (EDS): This connective tissue condition is increasingly recognized as a significant contributor to dysautonomia, particularly POTS. The hypermobile joints and stretchy tissues associated with EDS can affect blood vessel tone and contribute to blood pooling and orthostatic intolerance.
- Chiari malformation: This structural defect, where brain tissue extends into the spinal canal, can compress the brainstem and disrupt autonomic function. Many children with Chiari malformation experience dysautonomia symptoms, including dizziness, fainting, and temperature dysregulation.
- Mast Cell Activation Syndrome (MCAS): This condition involves the abnormal release of inflammatory mediators from mast cells, which can trigger or worsen dysautonomia symptoms. MCAS and dysautonomia often occur together, creating a complex cycle of inflammation and nervous system dysfunction.
- Post-viral syndromes and Long COVID: Following viral infections, some children develop persistent autonomic dysfunction. This has become particularly apparent with Long COVID, where children continue experiencing fatigue, orthostatic intolerance, and other dysautonomia symptoms long after the initial infection resolves.
While these factors can increase the risk of developing dysautonomia, it’s important to note that not everyone who experiences them will go on to develop the condition. Conversely, some individuals may develop dysautonomia without any identifiable risk factors.
Signs of Dysautonomia in Children
Dysautonomia can manifest in a wide range of signs that affect multiple body systems, making it challenging for parents and healthcare providers to recognize and diagnose the condition. This is often called an “invisible illness” because children may not look sick, yet they struggle with symptoms that make it difficult to attend school, participate in activities, and live normal lives.
One hallmark sign of dysautonomia is orthostatic intolerance—difficulty maintaining an upright posture. When a child stands up, their body should automatically adjust blood pressure and heart rate to maintain proper blood flow to the brain. In children with dysautonomia, this automatic adjustment doesn’t happen properly, leading to dizziness, lightheadedness, and sometimes fainting.
This happens because of blood pooling—when blood collects in the legs and lower body rather than being efficiently pumped back to the heart and brain. You might notice your child’s legs turn purple or mottled when standing, or they complain of heavy, achy legs.
These are some of the most common signs in children:
Physical Signs
- Digestive issues: Nausea, vomiting, bloating, constipation, and diarrhea are common in children with dysautonomia due to autonomic dysfunction affecting the gastrointestinal tract.
- Altered tone and coordination: Dysautonomia can affect motor tone and coordination, leading to frequent imbalances and gross and fine motor challenges in children.
- Immunosuppression and inflammation: When dysautonomia and sympathetic dominance set in, the immune system weakens, and the entire body and brain can become stuck in a chronic inflammatory cycle.
- Fatigue and weakness: Children with dysautonomia often experience chronic fatigue and may have difficulty keeping up with their peers in physical activities. This isn’t just “being tired”—it’s a profound exhaustion that doesn’t improve with rest.
- Dizziness and fainting: Orthostatic hypotension, or the inability to regulate blood pressure and heart rate when changing positions (e.g., standing up from sitting), can cause dizziness, lightheadedness, and even fainting (syncope). Some children experience near-syncope episodes multiple times per day.
- Rapid or slow heart rate: Dysautonomia can cause tachycardia (rapid heart rate) or bradycardia (slow heart rate), which may be accompanied by palpitations or chest discomfort. Heart rates may spike 30+ beats per minute just from standing up.
- Temperature dysregulation: Children may struggle to regulate body temperature, experiencing episodes of feeling extremely hot or cold, excessive sweating, or an inability to sweat properly.
- Seizures and epilepsy: It is well known that dysautonomia, sympathetic dominance, and vagus nerve dysfunction can contribute to seizures and epileptic conditions.
Cognitive and Emotional Signs
- Sensory processing difficulties: The vagus nerve and Autonomic Nervous System are heavily involved in sensory processing and integration, so when dysautonomia is present, many children struggle with sensory overload, transitions, meltdowns, tantrums, and more.
- Brain fog and difficulty concentrating: Many children with dysautonomia experience cognitive issues, such as difficulty focusing, memory problems, mental fatigue, and other ADHD-like challenges. This is sometimes called “mental clouding” and can significantly impact school performance.
- Anxiety and depression: The chronic nature of dysautonomia and its impact on daily life can take a toll on a child’s mental health, leading to increased anxiety and depression. Additionally, the autonomic dysfunction itself can trigger anxiety-like signs, creating a cycle that’s hard to break.
Seizures, Subluxation, and Dysautonomia
When subluxation occurs, it interferes with the normal function of the nervous system, particularly affecting nerve communication in areas such as the upper cervical spine and brainstem, which directly affects the vagus nerve.
This interference can trigger sympathetic dominance, keeping the body in a chronic “fight or flight” state. As the nervous system becomes overactive, it can lead to dysautonomia, an imbalance in the Autonomic Nervous System that disrupts essential functions such as digestion, heart rate regulation, breathing, motor tone, and immune response. In this state, the body’s ability to maintain a healthy balance is compromised, creating the perfect conditions for neurological imbalances, including seizures.
At the same time, vagus nerve dysfunction—which can be caused by subluxation or prolonged nervous system stress—further impairs the body’s ability to regulate brain activity. The vagus nerve normally plays a key role in calming the brain and modulating electrical signals, but when it’s not functioning properly, the brain becomes more excitable, increasing the risk of seizures.
Together, subluxation, sympathetic dominance, dysautonomia, and vagus nerve dysfunction create a vicious cycle that keeps the nervous system in a state of heightened stress, ultimately making the brain more prone to seizure activity.
PANDAS/PANS and Dysautonomia
PANDAS (Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal Infections) and PANS (Pediatric Acute-onset Neuropsychiatric Syndrome) are complex conditions that often leave parents and traditional medical providers puzzled.
At the heart of PANDAS/PANS lies dysautonomia — the dysfunction of the Autonomic Nervous System. This imbalance between the sympathetic “fight or flight” response and the parasympathetic “rest and regulate” functions can trigger a cascade of neurological and immune system disruptions. Children with PANDAS/PANS often experience a sudden onset of OCD, tics, anxiety, and behavioral changes, which are all closely tied to nervous system regulation.
The vagus nerve, a key player in the Autonomic Nervous System, is particularly affected in PANDAS/PANS. When functioning optimally, it helps regulate inflammation, immune responses, and mood. However, in children with these conditions, vagus nerve dysfunction can contribute to the intense and often puzzling symptoms they experience.
Understanding PANDAS/PANS through the lens of dysautonomia opens up new avenues for care. By addressing the underlying nervous system imbalance, rather than just managing symptoms, we can help restore proper neurological function and support the body’s natural healing processes.
How is Dysautonomia Diagnosed?
One of the biggest frustrations parents face is getting an accurate diagnosis of dysautonomia. Because the signs affect so many different body systems, children are often shuffled between specialists—cardiologists, gastroenterologists, neurologists—with each doctor focusing only on their particular area of expertise and missing the bigger neurological picture.
The challenge is that dysautonomia doesn’t show up on standard blood tests or imaging. Your child’s labs might come back “normal,” even though they’re clearly struggling. This is because dysautonomia is a functional condition of the nervous system, not a structural problem that shows up on an MRI or blood panel.
Conventional Diagnostic Tests
In the conventional medical system, when dysautonomia is suspected, several tests may be ordered:
- Tilt Table Test: This has traditionally been considered the “gold standard” for diagnosing certain types of dysautonomia, particularly POTS and neurocardiogenic syncope. During this test, your child lies flat on a table, which is then tilted upright, while heart rate and blood pressure are continuously monitored. The test reveals how the body responds to positional changes and can identify abnormal drops in blood pressure or increases in heart rate.
- Active Stand Test: This simpler version can be done in a doctor’s office. Blood pressure and heart rate are measured while lying down, then immediately upon standing, and again after standing for several minutes. An increase of 30+ beats per minute in teens (or 40+ in younger children) without a significant drop in blood pressure is suggestive of POTS.
- Autonomic Function Testing: More comprehensive autonomic testing may include measures of heart rate variability, sweat testing, breathing tests, and blood flow assessments to evaluate how well the Autonomic Nervous System is functioning.
Limitations of Conventional Care
When children present with symptoms of dysautonomia, they are often met with a lack of understanding and limited care options within the conventional medical system. This is because many healthcare providers are not well-versed in recognizing and caring for autonomic conditions and do not understand nervous system dysregulation much at all.
A general pediatrician is just that, a “generalist” who in today’s traditional healthcare system often functions more as a “refer out specialist” than anything else. If your child complains of gut or digestive problems, you’re sent to a GI specialist. If they get sick often or struggle with autoimmune conditions like allergies and asthma, you’re sent to an immunologist or allergist. If they show any signs of neurological issues (which sadly need to be painfully obvious for a standard pediatrician to spot them) or early warning signs of autism, ADHD, or Sensory Processing Disorder, you’re sent to a neurologist.
You arrive at each of these specialists with the hope of finally getting some answers and explanations as to what’s going on and what’s really causing your child’s struggles, and most importantly, some solutions to address it and help them heal. But so often the opposite happens: you leave with even more questions than answers, and nothing but a recommendation for more medications to stuff down the signs, not actually address the root cause.
Since the majority of children, teens, and young adults struggling with chronic health issues today actually have multiple different “systems” that are offline and dysfunctional, another massive frustration that families like Francesca’s face is this: finding out if they are all tied together.
Another one of the limitations of conventional care plans for dysautonomia is the focus on symptom management rather than addressing the root causes of the condition. Medications such as beta-blockers, midodrine, and fludrocortisone may be prescribed to help regulate heart rate and blood pressure, but they do not address the underlying autonomic dysfunction.
Additionally, many of these medications come with potential side effects that can further compromise a child’s quality of life. For example, beta-blockers can cause fatigue, dizziness, and depression, while fludrocortisone can lead to electrolyte imbalances and edema.
A Neurologically-Focused Approach For Healing the Autonomic Nervous System
At PX Docs, we understand the limitations of conventional care for dysautonomia and believe that a new approach is needed to help children and families achieve optimal health and well-being. Our approach centers on Neurologically-Focused Chiropractic Care, which aims to address the root causes of dysautonomia by restoring balance to the Autonomic Nervous System.
Neurologically-Focused Chiropractic Care is based on the understanding that proper nervous system functioning is essential for overall health and well-being. Interference and dysfunction within the nervous system (known as subluxation) can affect the Autonomic Nervous System and contribute to the development of conditions like dysautonomia. And in turn, dysautonomia and nervous system dysregulation contribute to nearly every single chronic illness out there.
Our Pediatric + Family Chiropractors are specially trained to identify and address subluxations using INSiGHT Scans, which allow us to build customized, individualized care plans for each and every child and to choose the most effective, precise adjustments tailored to each child’s unique needs.
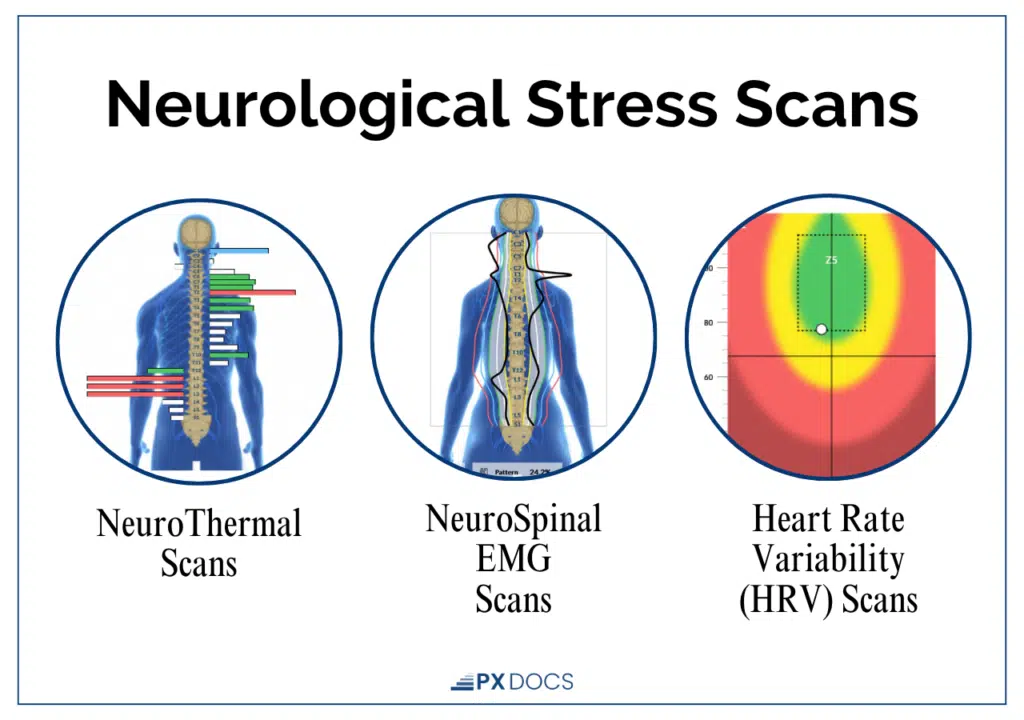
It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for dysautonomia or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
By removing interference in the nervous system and promoting optimal communication between the brain and body, chiropractic care can help restore balance and function to the vagus nerve and Autonomic Nervous System.
Lifestyle Modifications That Can Help
While addressing the root neurological causes of dysautonomia through Neurologically-Focused Chiropractic Care is essential, there are also important lifestyle modifications that can help manage symptoms and improve your child’s quality of life on a day-to-day basis.
These aren’t “cures,” but they can make a real difference in helping your child feel better while their nervous system heals:
- Hydration and Salt Intake: Children with dysautonomia often need significantly more fluids and salt than typical children. Increased sodium helps the body retain fluid, which expands blood volume and reduces the severity of blood pooling and orthostatic hypotension. Many of our families find that adding 3-5 grams of salt daily (through salty snacks, electrolyte drinks, or salt tablets) along with 60-80 ounces of water helps their child feel noticeably better. Always discuss specific amounts with your doctor, as individual needs vary.
- Compression Garments: Compression stockings or compression shorts can help reduce blood pooling in the legs by applying gentle pressure that encourages blood to flow back toward the heart. Look for medical-grade compression (20-30 mmHg) that extends from the feet up to the waist for maximum benefit. Yes, they can be uncomfortable at first, especially for sensory kids, but many families report they make a significant difference in reducing dizziness and fatigue.
- Small, Frequent Meals: Large meals can trigger a drop in blood pressure as blood rushes to the digestive system. Eating smaller meals more frequently throughout the day—five to six small meals instead of three large ones—can help minimize post-meal fatigue and dizziness. Avoiding high-sugar and high-carbohydrate meals can also help stabilize blood sugar and reduce symptoms.
- Strategic Position Changes: Teach your child to change positions slowly—sitting up from lying down, standing up from sitting. Flexing ankles and calf muscles before standing (called “countermaneuvers”) can help pump blood back up toward the heart. Some kids find it helpful to sit on the edge of the bed for a minute before standing up in the morning.
- Temperature Management: Heat can significantly worsen dysautonomia symptoms. Keep your home cool, use fans, take lukewarm showers instead of hot baths, and avoid prolonged sun exposure. On the flip side, some children have trouble regulating in cold environments too, so layered clothing that’s easy to adjust is key.
These lifestyle modifications work best when combined with Neurologically-Focused Care that addresses the root cause. Think of them as supportive tools that help your child function better while their nervous system is healing, not as standalone care plans.
Finding Hope and Answers for Your Child
If you are a parent or caregiver of a child struggling with dysautonomia, it can be a challenging and overwhelming journey. You may feel like you have exhausted all of your options within the conventional medical system and are unsure where to turn next.
At PX Docs, we want you to know that there is hope and that you are not alone. By taking a neurologically-focused approach to dysautonomia with chiropractic care and addressing the root causes, we have seen incredible transformations in the lives of countless children and families, just like Francesca and thousands of others!
If you suspect that your child may be struggling with dysautonomia, or if you have already received a diagnosis but are looking for a more drug-free approach to care, we encourage you to visit the PX Docs Directory to find a qualified pediatric chiropractor near you.





