Crohn’s Disease in children is a chronic inflammatory bowel condition in which the immune system attacks the digestive tract, causing recurring abdominal pain, diarrhea, growth delays, and systemic inflammation. Approximately 20–25% of all Crohn’s diagnoses occur before age 18, and emerging research links disease activity to reduced vagal tone and autonomic nervous system dysfunction, a root cause that conventional gastroenterology rarely addresses.
Watching your child struggle with relentless stomach pain, unpredictable diarrhea, and stunted growth is exhausting and frightening. If your child has been diagnosed with Crohn’s Disease, or you’re still searching for answers, you’ve probably heard some version of “we don’t fully know what causes it.” That answer is frustrating. And honestly? It’s incomplete.
The truth is, while conventional medicine excels at managing Crohn’s symptoms, it rarely asks a deeper question: why is your child’s immune system stuck in an inflammatory loop it can’t escape? What controls that loop? And what happens when that controller is offline?
We look at pediatric gut health through a neurological lens that most providers never consider. The answer to “why won’t the inflammation stop?” often lives not in the gut itself, but in the nervous system, specifically, the vagus nerve and its role as the body’s most powerful anti-inflammatory regulator. This article covers everything parents need to know about Crohn’s Disease in children, from the basics of diagnosis and care to the contributing neurological root causes that conventional care often misses.
What Is Crohn’s Disease in Children?
Crohn’s Disease is a form of Inflammatory Bowel Disease (IBD) characterized by chronic, recurring inflammation anywhere along the digestive tract, from the mouth to the anus, though most commonly the lower small intestine and colon. Unlike ulcerative colitis, which affects only the colon’s inner lining, Crohn’s inflammation penetrates the full thickness of the intestinal wall and can leave gaps of healthy tissue between inflamed segments.
In the United States, an estimated 100,000 American youth currently live with this diagnosis, and that number has been rising steadily over recent decades. What’s important to understand is that Crohn’s Disease in children often presents differently than it does in adults, with growth delays, delayed puberty, and fatigue as primary complaints, sometimes before gut signs even appear.
This is a lifelong condition, but “lifelong” doesn’t have to mean “constantly suffering.” Remission is achievable, and the right approach, including addressing root causes, makes a significant difference in long-term outcomes.
Symptoms of Crohn’s Disease in Children
Crohn’s symptoms vary depending on where inflammation is most active, and they can shift over time. The hallmark is a relapsing-remitting pattern: flares followed by periods of relative calm.
Gut-related symptoms include:
- Chronic or recurring abdominal pain and cramping
- Diarrhea, often urgent, sometimes with blood or mucus
- Nausea, vomiting, and reduced appetite
- Constipation (less common but possible when strictures develop)
- Perianal sores, fistulas, or abscesses
Systemic and developmental symptoms include:
- Unexplained weight loss or failure to gain weight appropriately
- Stunted growth and delayed puberty, often among the earliest signs in children
- Chronic fatigue and low energy
- Anemia from nutrient malabsorption or blood loss
- Low-grade fevers
Extraintestinal symptoms, affecting areas outside the gut, occur in 35% of patients with IBD and include:
- Joint pain or swelling
- Skin rashes (particularly erythema nodosum)
- Eye inflammation.
These manifestations are a critical clue: they signal that this is a systemic inflammatory condition, not just a gut problem.
That systemic nature is exactly why understanding nervous system regulation matters so much.
What Causes Crohn’s Disease in Children?
The honest answer from mainstream medicine is nobody fully knows. The leading explanation is that Crohn’s results from an abnormal immune response; the immune system attacks the digestive tract as if it were a foreign invader, and then can’t turn itself off. Several factors are thought to contribute:
- Genetics: Children with a first-degree relative with IBD carry a significantly higher risk of 4-8x. Multiple gene variants have been identified, including NOD2/CARD15, which affects how immune cells respond to bacteria in the gut.
- Microbiome disruption: Research consistently links Crohn’s to imbalances in gut bacteria, less microbial diversity, reduced populations of protective strains like Faecalibacterium prausnitzii, and overgrowth of inflammatory species. Antibiotic exposure in early childhood is a documented risk factor, likely due to its impact on the developing microbiome.
- Environmental triggers: IBD rates are notably higher in developed, industrialized countries and have risen sharply since the mid-20th century. Diet quality, dynamics of the hygiene hypothesis, and environmental toxin exposure are all implicated.
- Immune dysregulation: The immune system’s T-helper cells mount an exaggerated response to normal gut bacteria, generating an inflammatory cascade that won’t resolve. Pro-inflammatory cytokines, particularly TNF-alpha, IL-1, and IL-6, drive tissue destruction.
Here’s what the conventional model almost never asks: what controls whether that inflammatory cascade can resolve? The answer leads directly to the nervous system and to a pathway most gastroenterologists never discuss.
The Missing Link is Your Child’s Nervous System
The nervous system, specifically the Autonomic Nervous System and its primary parasympathetic driver, the vagus nerve, directly controls whether gut inflammation resolves or persists. When Autonomic Nervous System dysfunction is present, the body loses its ability to complete the inflammatory cycle, creating the chronic, relapsing pattern that defines Crohn’s Disease in children.
The gut doesn’t operate independently. It’s one of the most heavily innervated organs in the body, connected to the brain through what researchers call the gut-brain axis. This bidirectional communication highway regulates digestion, immune activity, gut motility, mucosal barrier function, and, critically, the resolution of inflammation.
Think of the Autonomic Nervous System like a car with a gas pedal and a brake. The sympathetic branch (fight-or-flight) hits the gas, it activates immune responses, ramps up inflammation, and diverts resources to deal with perceived threats. The parasympathetic branch (rest-digest-regulate) applies the brake; it calms the system, finishes inflammatory cycles, repairs tissue, and restores balance.
In a healthy child, these two systems work together. After the immune system does its job, clearing a pathogen and healing tissue damage, the brake kicks in and inflammation resolves.
In children with nervous system dysregulation, the brake is compromised. The gas pedal stays pushed down. Inflammation activates, escalates, and never fully turns off, exactly the pattern we see in Crohn’s Disease.
The key to the brake? The vagus nerve.
How Does the Vagus Nerve Control Inflammation in the Gut?
The vagus nerve is the longest cranial nerve in the body, running from the brainstem down through the neck, chest, and abdomen to innervate the heart, lungs, liver, and, most importantly here, the entire gut. It carries signals in both directions: sensory information from organs up to the brain, and regulatory commands back down to the body.
One of the vagus nerve’s most critical, and least discussed, functions is controlling inflammation through what scientists call the cholinergic anti-inflammatory pathway. Here’s how it works:
When the vagus nerve detects inflammation in body tissues, it signals the brainstem, which evaluates the response and sends efferent signals back down the vagus. These signals trigger the release of acetylcholine, the vagus nerve’s primary neurotransmitter, which directly suppresses the production of pro-inflammatory cytokines, including TNF-alpha, IL-1, and IL-6. These are the exact cytokines driving the tissue destruction in Crohn’s Disease.
In other words, a healthy, well-functioning vagus nerve is what allows inflammation to do its job and then stop. It’s the body’s built-in off switch for excessive immune activation.
When the vagus nerve isn’t functioning well, when its tone is low, and its signaling is weak, that off switch doesn’t work properly. The immune system activates, cytokines flood the gut tissue, and the inflammatory response has no efficient mechanism to resolve. The fire alarm keeps ringing even after the fire’s been dealt with. Or worse, the alarm keeps ringing because the gut-immune system genuinely can’t complete its response without adequate vagal input to finish the cycle.
Research supports this connection. Studies measuring heart rate variability (HRV), a well-validated indirect measure of vagal tone, consistently find reduced HRV in patients with IBD, with lower readings correlating with greater disease activity and more frequent flares. This isn’t a coincidence. It reflects reduced parasympathetic regulation in children who should have the nervous system resources to modulate their own inflammatory responses.
How Does the “Perfect Storm” Lead to Crohn’s Disease in Children?
So why would a child’s vagus nerve be functioning poorly in the first place? This is where the “Perfect Storm” framework becomes essential for parents of children with Crohn’s.
The “Perfect Storm” describes a sequence of early-life neurological stressors that accumulate to create lasting dysfunction in a child’s nervous system, often long before a diagnosis like Crohn’s appears.
It typically begins before birth. Maternal stress during pregnancy elevates cortisol levels that cross the placenta, affecting the developing nervous system of the fetus. Prenatal stress has been shown to affect the development of the Autonomic Nervous System.
Birth trauma is often the turning point. The birth process, especially when it involves interventions like forceps, vacuum extraction, induction, or cesarean delivery, creates intense mechanical forces on the infant’s delicate upper cervical spine and brainstem. This is where the vagus nerve originates. Physical strain to the upper neck creates what we call subluxation, not just a structural misalignment, but a neurological interference that disrupts proper signaling between the brain and the body’s organs.
When subluxation affects the cervical spine near the vagus nerve’s origin, vagal tone suffers. The parasympathetic brake weakens. The sympathetic gas pedal, the fight-or-flight system, begins to dominate.
Early childhood stressors compound the problem. Frequent antibiotic courses, recurrent infections, environmental toxin exposure, and the gut microbiome disruption that comes with all of these continue to push the nervous system toward sympathetic dominance. A child who had birth trauma, early antibiotic exposure, and a history of colic, reflux, or chronic constipation is showing you the early signs of a nervous system that’s been fighting uphill since day one.
By the time dysautonomia is established, that chronic imbalance between the sympathetic and parasympathetic branches, the gut-immune connection is already compromised. The child’s body has a reduced capacity to resolve inflammation, maintain gut barrier integrity, and regulate the immune response to gut bacteria.
The stage is set for a condition like Crohn’s to take hold.
Conventional Care for Crohn’s Disease in Children
It’s important to be clear: conventional medical care for pediatric Crohn’s Disease can be essential and often life-changing. Parents should work closely with a pediatric gastroenterologist and even get multiple opinions from medical providers to find the right fit. The goal of the neurological approach isn’t to replace that partnership; it’s to address a root cause that medications alone cannot.
- Anti-inflammatory medications (5-aminosalicylates, corticosteroids) are often used first to induce remission during active flares. They reduce mucosal inflammation but carry significant side effects with long-term use, particularly for children’s bone density and growth.
- Immunomodulators (azathioprine, methotrexate) help maintain remission by suppressing the broader immune response. They require regular monitoring due to risks of liver toxicity and infection.
- Biologic medications, particularly anti-TNF agents like infliximab (Remicade) and adalimumab (Humira), have transformed outcomes for many children with moderate-to-severe Crohn’s. The REACH trial demonstrated infliximab’s efficacy for inducing and maintaining remission in pediatric patients. These medications directly target the same cytokines (TNF-alpha) that the vagus nerve normally suppresses through the cholinergic pathway, which is a telling parallel.
- Exclusive enteral nutrition (EEN), a liquid diet providing all calories for 6–8 weeks, is increasingly used in Europe and Canada as a first-line induction therapy, particularly for children, given its effectiveness and lack of steroid-related side effects.
- Surgery is reserved for complications like strictures, fistulas, abscesses, or medication-refractory disease. It can provide significant relief but doesn’t cure Crohn’s, as inflammation typically recurs near the resection site.
All of these interventions manage the downstream effects of a dysregulated immune system. None of them addresses the upstream neurological regulation failure. And many families either aren’t seeing enough progress… or know they don’t want medication to be the forever plan.
How Does Neurologically-Focused Chiropractic Care Address Gut Health?
Neurologically-Focused Chiropractic Care is a specialized approach that identifies and addresses subluxation, nervous system dysregulation, and dysautonomia through advanced neurological assessment (INSiGHT Scans) and precise, gentle adjustments tailored to each patient’s individual neurological patterns. Instead of targeting gut inflammation directly, it focuses on restoring the nervous system’s ability to regulate the inflammatory response independently.
The primary mechanism is correcting subluxation, especially if present in the upper cervical spine, where the vagus nerve originates and where birth trauma most commonly creates interference. When subluxation in the upper cervical region is identified and addressed with specific, gentle adjustments, the goal is to reduce neurological interference, improve vagal tone, and restore better parasympathetic signaling throughout the gut-immune axis.
This isn’t a claim that chiropractic care treats or cures Crohn’s Disease. It’s a recognition that a nervous system functioning closer to its potential is better equipped to regulate the inflammatory processes that conventional care works so hard to manage pharmacologically.
For children with Crohn’s, this may translate to fewer inflammatory flares, better stress resilience, improved gut motility (also vagally controlled), and potentially better responses to conventional care when the Autonomic Nervous System is better balanced. It’s also particularly relevant for children who have clear “Perfect Storm” histories, difficult births, early antibiotic use, chronic constipation, or colic as infants, suggesting that nervous system dysregulation has been part of the picture from the beginning.
Elizabeth, for example, had extreme IBS and stomach pain along with other gut challenges. With consistent Neurologically-Focused Chiropractic Care, her mom said, “Wow, we are so grateful for where she is now. She has more energy and eats more, especially the foods she loves. Now she is on no daily meds. No more daily vomiting, no more daily pain, also a plus, she has not been sick. She hasn’t had a GERD symptom in over a month. We are so happy she is living a more “normal” life.”
How INSiGHT Scans Reveal the Root Cause
One of the questions parents most often ask is: “How do I know if my child’s nervous system is contributing to their gut health?” That’s where INSiGHT scans provide objective, measurable data.
INSiGHT scanning technology includes three non-invasive assessments:
- Heart Rate Variability (HRV) measures Autonomic Nervous System balance, specifically the ratio of sympathetic to parasympathetic activity. In children with compromised vagal tone, HRV scores are characteristically low, indicating reduced parasympathetic regulation. Research in IBD populations confirms this pattern.
- Surface EMG (sEMG) measures electrical activity in the paraspinal muscles along the spine, identifying areas of neurological tension and subluxation-related dysfunction that may be interfering with normal nerve signaling.
- Neurological Thermal Scan detects temperature asymmetries along the spine caused by autonomic dysregulation, an indicator of where the nervous system is under stress.
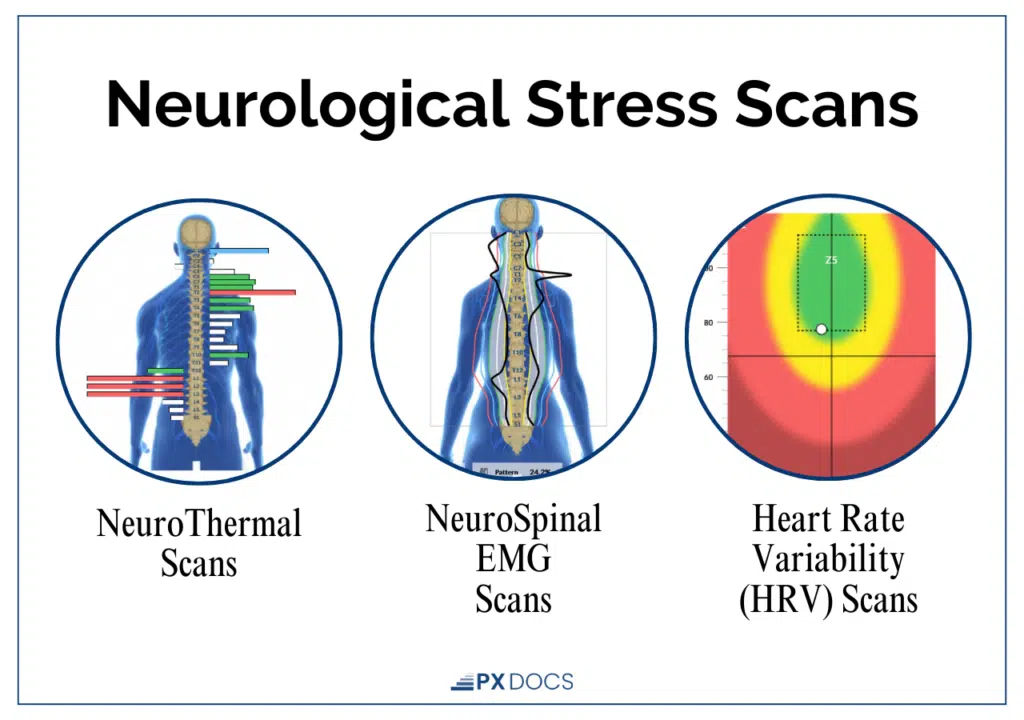
These scans don’t diagnose or treat Crohn’s Disease, or any other condition, not even back pain. What they do is provide a PX Doc with objective data on a child’s neurological state: where the stress and interference are, how significant the dysregulation is, and how the nervous system responds as care progresses. For parents who want to understand the “why” behind their child’s health challenges, this kind of data is often the piece they’ve been missing.
Is There a Root-Cause Approach for Children with Crohn’s Disease?
Crohn’s Disease in children is serious, complex, and deserves the full attention of skilled medical professionals. Biologics have changed lives. Pediatric gastroenterologists do essential work. None of that is in question here.
But if your child has been managing Crohn’s with medication and still isn’t thriving the way you hoped, or if you’ve watched their health decline across multiple systems, not just the gut, it’s worth asking a question that most providers never raise: Is the nervous system part of this picture?
The cholinergic anti-inflammatory pathway is real, well-documented science. Low vagal tone is consistently documented in IBD patients. Birth trauma’s impact on the upper cervical spine is documented. The connection between sympathetic dominance and chronic gut inflammation is documented. What isn’t being discussed enough is what to do about the neurological side of this equation.
That’s the gap PX Docs exists to fill.
If your child carries a history that sounds like the “Perfect Storm,” a difficult birth, early gut issues, recurrent infections, nervous system dysregulation, there’s a PX Doc trained in neurological assessment and care who can help you understand what’s going on beneath the surface. Find a PX Doc near you and start with a neurological consultation that goes further than any gastroenterology workup ever will.
Frequently Asked Questions About Crohn’s Disease in Children
Can Crohn’s Disease go away on its own?
Crohn’s Disease is a chronic condition that does not resolve spontaneously. However, sustained remission is achievable with appropriate care. Conventional treatment uses medications to suppress the immune response, while Neurologically-Focused Chiropractic Care aims to restore the nervous system’s ability to regulate inflammation naturally, potentially supporting longer and more stable periods of remission.
Is chiropractic care safe for children with Crohn’s Disease?
Neurologically-Focused Chiropractic Care uses precise, gentle adjustments specifically tailored to each child’s neurological patterns. It does not directly treat Crohn’s Disease. Instead, it addresses subluxation and nervous system dysregulation that may be contributing to autonomic imbalance. Many families use it alongside gastroenterology and nutritional support as part of a comprehensive care team.
What are the early signs of Crohn’s Disease in children?
Early signs of Crohn’s in children often include unexplained growth delays, chronic fatigue, recurring abdominal pain, and persistent diarrhea. Notably, growth failure and delayed puberty may appear before obvious gut symptoms, making pediatric Crohn’s easy to miss without proactive screening by a gastroenterologist.
How long does it take to see improvement with neurological chiropractic care?
Response times vary based on the severity of subluxation and nervous system dysregulation. Some families report improvements in stress resilience, gut motility, and overall regulation within weeks, while deeper neurological patterns may take several months of consistent care. INSiGHT Scans provide objective data to track nervous system changes throughout the process.
What is the connection between birth trauma and Crohn’s Disease?
Birth interventions such as forceps, vacuum extraction, and cesarean delivery can create mechanical stress on the infant’s upper cervical spine, where the vagus nerve originates. This may lead to subluxation and reduced vagal tone, compromising the body’s ability to regulate inflammation through the cholinergic anti-inflammatory pathway, a factor in the chronic immune dysregulation seen in Crohn’s Disease.
What’s the difference between Crohn’s Disease and ulcerative colitis?
Both are forms of Inflammatory Bowel Disease, but Crohn’s can affect any part of the digestive tract and penetrates the full thickness of the intestinal wall, while ulcerative colitis is limited to the colon’s inner lining. Crohn’s is also more likely to present with extraintestinal symptoms like joint pain, skin rashes, and growth delays in children.