Asperger syndrome is a neurodevelopmental profile, now classified under Autism Spectrum Disorder (ASD) Level 1, characterized by significant social communication differences, restricted interests, and sensory sensitivities in children who have no language delays or intellectual disability. Research shows that more than 90% of individuals on the autism spectrum experience atypical sensory processing, pointing to deeper nervous system involvement that most conventional approaches don’t address.
If you’ve been reading about Asperger syndrome in children, you’ve probably already pieced together that the label itself has changed. But here’s what hasn’t changed: the kids who fit this profile are real, the challenges they face are real, and most parents are still getting answers that stop at what without ever getting to why.
Your child may be incredibly bright. They might have an encyclopedic knowledge of trains, dinosaurs, or space. But they’re also struggling to make friends, getting overwhelmed by sensory input, or falling apart at the slightest change in routine. You’ve probably heard “it’s neurological” from every specialist. What you haven’t heard is which part of the neurology, and what you can actually do about it.
What Is Asperger Syndrome in Children?
Asperger syndrome was historically used to describe children who showed significant social and behavioral differences but had no language delays or intellectual disability. The name came from Austrian pediatrician Hans Asperger, who in 1944 described children in his care who struggled to form friendships, engaged in one-sided conversations about narrow interests, and didn’t pick up on social cues the way other children did.
In 2013, the DSM-5 eliminated Asperger’s as a standalone diagnosis. Children who would have previously received that label are now diagnosed with Autism Spectrum Disorder, Level 1, sometimes called “high-functioning autism.” The three severity levels are:
- Level 1, Requires support (formerly Asperger’s)
- Level 2, Requires substantial support
- Level 3, Requires very substantial support
According to Cureus, the Asperger profile is characterized by impaired social interaction, a limited range of interests, and repetitive behaviors without clinically significant language or cognitive delays.
Many families and self-advocates still use the term Asperger syndrome because it carries meaning and community. It’s not wrong to use it. What matters is understanding that this population of children, bright, verbal, socially struggling, often sensory-sensitive, has a very specific neurological profile that deserves a much deeper look than most providers offer.
Signs of Asperger Syndrome in Children
No two children with Asperger’s look exactly the same. But there are consistent patterns parents notice, often well before any formal diagnosis.
Social Communication Differences
Children with Asperger syndrome typically have well-developed vocabulary and grammar, sometimes startlingly advanced for their age. But using language socially is a different skill entirely, and that’s where things break down.
Common signs include:
- Long, one-sided conversations about a single topic of interest
- Difficulty reading facial expressions, body language, or tone of voice
- Trouble understanding sarcasm, idioms, and figurative language
- Struggles with the back-and-forth rhythm of conversation
- Preferring adults or much younger children over same-age peers
- Social isolation or confusion about why peers don’t respond the way they expect
Kids with Asperger’s often want to connect. The frustration isn’t from indifference; it’s from genuinely not knowing how. This distinction matters. They’re not being rude. Their nervous system processes social signals differently.
Restricted Interests and Repetitive Behaviors
This is the feature that often stands out most clearly. A child with Asperger’s doesn’t just like trains; they often know every train line, every locomotive model, and every piece of historical detail. This intense focus isn’t really a quirk. It’s how their nervous system finds predictability and regulation in a world that otherwise feels overwhelming.
Watch for:
- Obsessive focus on one or two narrow topics
- Distress when these routines or interests are interrupted
- Repetitive movements, sometimes called stimming, such as hand-flapping, rocking, or finger movements
- Rigid adherence to routines, with significant dysregulation when routines change
- Collecting and organizing objects or information by category
Sensory Sensitivities
Sensory sensitivity is one of the most under-discussed features of Asperger syndrome in children, and it’s one of the most important neurologically. Research published in NCBI indicates that more than 90% of individuals on the autism spectrum experience atypical sensory perceptions across multiple senses.
Children may be hypersensitive (over-responsive) or hyposensitive (under-responsive), or both, depending on the sense:
- Hypersensitivity to sounds, lights, certain textures, or smells
- Strong food aversions based on texture, not taste
- Emotional overreaction to physical sensations that don’t bother other children
- Low pain perception or seeming indifferent to cold or heat
- Seeking intense sensory input (crashing, spinning, deep pressure)
Children with Asperger syndrome frequently also experience ADHD, anxiety, Sensory Processing Disorder, and emotional dysregulation. This co-occurrence isn’t coincidental; these conditions share a common root in Autonomic Nervous System dysfunction, specifically sympathetic dominance and vagal nerve suppression driven by subluxation.
What looks like a behavioral problem is often a nervous system stuck in overdrive. The meltdowns, the shutdowns, the inflexibility, these are downstream effects of a nervous system that can’t properly regulate sensory input. This is closely related to what’s seen in Sensory Processing Disorder, which frequently co-occurs with the Asperger’s profile.
Emotional Regulation Challenges
Children with Asperger syndrome often struggle to identify, name, and manage their emotions, a pattern sometimes called alexithymia. They may have very intense emotional reactions with limited ability to bring themselves back to calm. Tantrums and meltdowns in older children, difficulty with transitions, and extreme responses to unexpected changes are all connected to this underlying dysregulation.
What Causes Asperger Syndrome?
The standard answer is genetics combined with “brain differences.” And yes, there’s a genetic component; children with a first-degree relative on the spectrum do have higher rates themselves. But genetics alone can’t explain why rates of ASD have climbed 300% over recent decades. Genes simply don’t shift that fast across a population.
What conventional medicine hasn’t fully integrated is the role of the developing nervous system, and specifically, the role of early neurological stress.
How Does the “Perfect Storm” Lead to Asperger Syndrome?
At PX Docs, we use a concept called the “Perfect Storm” to explain why so many children today are presenting with neurodevelopmental challenges that previous generations rarely saw at this scale.
The “Perfect Storm” refers to a sequence of early neurological stressors that, when they accumulate during the most sensitive windows of development, can overwhelm a child’s developing nervous system and set the stage for ongoing dysregulation.
There are three core components:
1. Early Neurological Stress (Prenatal and Perinatal)
The story often starts before birth. Fertility struggles, prenatal stress, and elevated cortisol levels during pregnancy have all been linked to altered fetal brain development. The developing Autonomic Nervous System, especially the vagus nerve, is exquisitely sensitive during this window.
Then comes birth. Birth trauma, including prolonged labor, fetal distress, forceps or vacuum extraction, induction, and C-section delivery, can cause physical stress to the infant’s upper neck and brainstem region. This is where the vagus nerve exits, and where subluxation, neurological interference involving misalignment, fixation, and disruption of nervous system function, most commonly takes hold.
2. Toxic Load and Early Childhood Stressors
Once born, children today face an unprecedented environmental load. Environmental toxins, heavy metals, pesticides, plastics, air pollutants, combined with medical stressors like frequent antibiotic use, reflux medications, and aggressive vaccine schedules, create cumulative strain on an already-stressed developing neuro-immune system.
This toxic load disrupts the gut microbiome, elevates systemic inflammation, and places ongoing demand on a nervous system that may already be struggling to stay regulated.
3. Nervous System Dysregulation and Subluxation
The cumulative effect of these stressors is nervous system dysregulation, and at its core, subluxation. Subluxation is more than a structural issue. It’s a state of neurological interference that disrupts the normal function, regulation, and adaptability of the nervous system as a whole. It occurs when physical, chemical, or emotional stress overwhelms the nervous system’s ability to adapt.
When subluxation is present at the brainstem and upper cervical levels, it creates the conditions for dysautonomia, an imbalance between the sympathetic (“fight-or-flight”) and parasympathetic (“rest, regulate, digest”) branches of the Autonomic Nervous System.
Think of it like a gas pedal and a brake pedal. In a healthy nervous system, both work and the driver can modulate speed. In a child with Asperger’s, the gas pedal is often stuck down, the sympathetic system is chronically overactivated, while the brake pedal (parasympathetic/vagal tone) barely registers. That’s why sensory input feels overwhelming. That’s why transitions are catastrophic. That’s why social situations feel threatening even when they’re not.
How Is Asperger Syndrome Diagnosed?
Formal diagnosis now falls under ASD and is evaluated by developmental pediatricians, neuropsychologists, or psychiatrists using standardized tools such as the ADOS-2 (Autism Diagnostic Observation Schedule) and ADI-R (Autism Diagnostic Interview–Revised).
The diagnostic criteria require:
- Persistent deficits in social communication and interaction across multiple contexts
- Restricted, repetitive patterns of behavior, interests, or activities
- Traits present in early developmental period
- Traits cause significant functional impairment
For children who would have previously received an Asperger’s diagnosis, they typically meet ASD Level 1 criteria, meaning they have the above features but do not have significant language delays or intellectual disability.
Important to note: diagnosis often comes late for this population. The advanced vocabulary can mask the underlying challenges. Girls are particularly underdiagnosed, as research confirms they’re more likely to “mask”, consciously mimicking social behaviors, which delays recognition of what’s actually happening neurologically.
Early evaluation is important. Any child not meeting developmental milestones in the social domain should be assessed. Pediatricians can refer to developmental specialists, and evaluation before age 2 opens access to the most neuroplastic developmental window.
What Does Conventional Care for Asperger Syndrome Look Like?
Conventional care for Asperger syndrome focuses on managing symptoms through behavioral therapies (ABA), speech-language therapy, occupational therapy, CBT for anxiety, and, in some cases, medication, but these approaches work from the outside in without addressing the underlying nervous system state generating the challenges.
Here’s what that typically includes:
- Behavioral therapies like Applied Behavior Analysis (ABA) teach specific social and adaptive behaviors through structured reinforcement. For Level 1 ASD specifically, the focus is typically on social skills, flexible thinking, and managing anxiety.
- Speech-language therapy targets pragmatic language, the social use of communication. Children learn to read conversational cues, understand implied meaning, and engage in reciprocal dialogue.
- Occupational therapy (OT) addresses sensory processing, fine motor skills, and daily living skills. Sensory integration therapy is a common OT specialty for children with significant sensory sensitivities.
- Cognitive Behavioral Therapy (CBT) can be effective for older children with Asperger’s who can engage in self-reflection. It’s particularly useful for anxiety management, which is extremely common in this population (approximately 50%).
- Medication doesn’t target the core features of ASD. The FDA has approved risperidone and aripiprazole for associated signs like severe irritability, self-injury, and aggression, but these are symptom-management tools, not solutions to the underlying neurology.
These therapies have real value. The children who receive them early and consistently do better than those who don’t. We aren’t dismissing them. But they share a common limitation: they work on behavior and skill-building from the outside in, without addressing the neurological state that’s generating the challenges in the first place.
The Nervous System at the Center of The PX Docs Approach
Here’s the conversation most families never have with their pediatrician or developmental specialist: their child’s brain isn’t just “wired differently” in some static, fixed way. Their nervous system is dysregulated, stuck in a chronic state of sympathetic dominance and vagal withdrawal, and that dysregulation is a physiological state that can shift.
The vagus nerve is central to this. Vagus nerve dysfunction disrupts the body’s ability to self-regulate, to calm down after stress, to process sensory input without overwhelm, and to shift flexibly between states of alertness and calm. It also connects directly to social engagement. The “social nervous system”, the polyvagal circuit described in foundational research by Stephen Porges, requires adequate vagal tone to function. When vagal tone is suppressed, social interaction feels physiologically unsafe, even when there’s no actual threat.
This is why children with Asperger’s aren’t just using social skills incorrectly. Their nervous system is literally in a state that makes social engagement harder. Teaching social scripts helps. But helping the nervous system get out of survival mode helps more, and it helps everything else at the same time.
Dysautonomia, that chronic imbalance between sympathetic and parasympathetic function, also drives the gut challenges many children with Asperger’s experience: constipation, picky eating, food sensitivities, and abdominal pain. The gut and the brain communicate constantly through the vagus nerve, and when that communication is disrupted, both suffer.
This isn’t a new concept. Multiple studies have found patterns of autonomic dysregulation in children with ASD, including reduced parasympathetic tone and altered heart rate reactivity during social tasks. A 2025 study found that autistic children specifically showed parasympathetic under-activation at rest compared to typically developing peers. What’s missing is clinical practice that actually targets this dysfunction.
How Does Neurologically-Focused Chiropractic Care Approach Asperger Syndrome?
Neurologically-Focused Chiropractic Care, the approach practiced by PX Docs doctors, starts where conventional care doesn’t: the nervous system itself.
The goal isn’t to “fix” Asperger syndrome or change who your child is. It’s to clear the neurological interference that’s keeping their system stuck in overdrive, and give their nervous system the conditions to regulate, adapt, and heal from the inside out.
INSiGHT Scanning: Seeing the Nervous System Objectively
Before anything else, a PX Docs doctor needs to see what’s actually happening in the nervous system. That’s where INSiGHT scans come in.
INSiGHT scanning technology uses three objective, non-invasive measurements:
- Heart Rate Variability (HRV) measures the balance between the sympathetic and parasympathetic branches of the Autonomic Nervous System. HRV is a direct window into vagal tone and the child’s overall adaptive capacity.
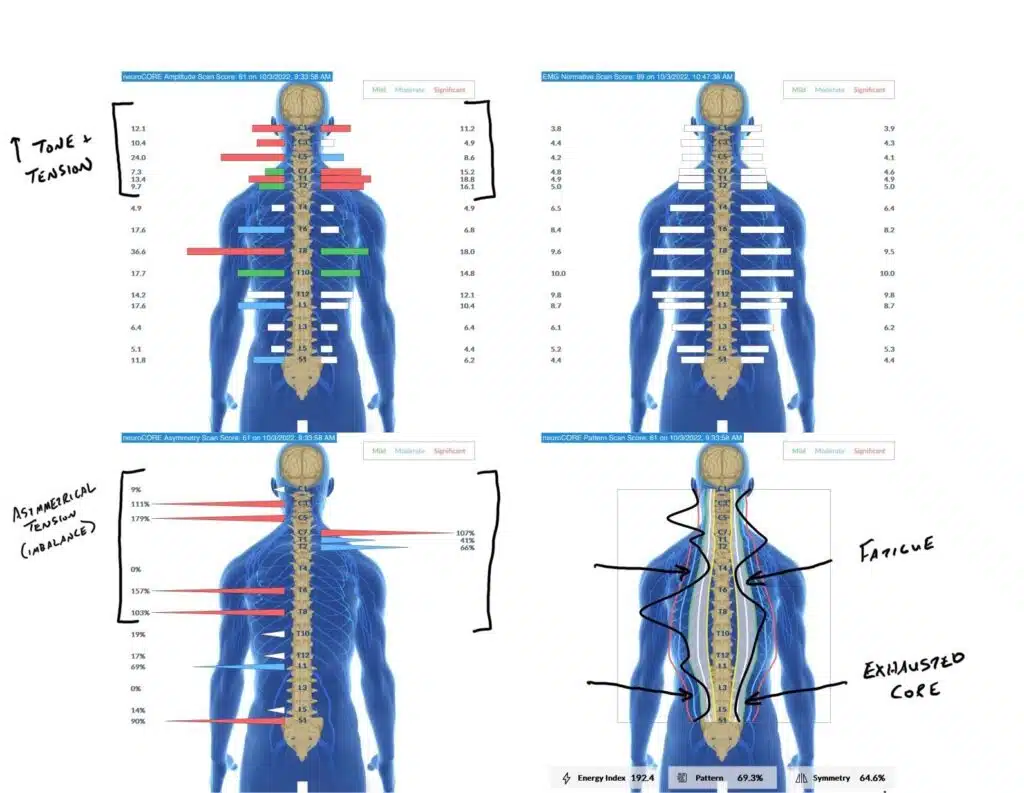
- Surface Electromyography (sEMG) assesses the electrical activity of muscles along the spine, identifying areas of neuromotor tension, asymmetry, and disorganization that reflect subluxation patterns.
- Thermal Scanning uses infrared sensors to measure temperature differences along the spine, revealing areas of dysautonomia and autonomic imbalance.
It’s important to note that INSiGHT scans do not diagnose or treat any condition, not even back pain. What they do is give the doctor a detailed, objective map of how the child’s nervous system is functioning, where the stress and interference are concentrated, and how the system is or isn’t adapting. This guides the care plan and tracks progress over time in ways that symptom reporting alone never can.
Children who fit the Asperger profile commonly show a very specific INSiGHT scan pattern: high sympathetic dominance on HRV, significant asymmetry and disorganization on sEMG (often concentrated in the upper cervical and thoracic regions), and thermal findings consistent with autonomic imbalance.
Neurologically-Focused Chiropractic Adjustments
Once subluxation patterns are identified, targeted adjustments help remove neurological interference and restore better function and communication throughout the nervous system. For children with Asperger syndrome, the upper cervical spine, where the brainstem and vagus nerve are most directly affected, is typically the primary focus.
As neurological interference clears, parents often observe a predictable sequence: sleep often improves first, then gut function, then sensory tolerance, then emotional regulation, and eventually, often last, the more complex social and communication features.
This isn’t a miracle or a coincidence. It’s what happens when the nervous system gains access to the parasympathetic regulation it’s been unable to reach. The brake pedal starts working again.
Neurologically-Focused Chiropractic Care doesn’t replace speech therapy, OT, or ABA. It works alongside them, and clinically, families often report that these therapies become significantly more effective once the nervous system is no longer in a chronic state of dysregulation. A child who isn’t in sensory overwhelm can actually use what the therapist is teaching.
Finding Support for Your Child
If your child has been diagnosed with Asperger syndrome or ASD Level 1, you’re likely already working with a team of specialists. That’s the right instinct. Early intervention matters.
What we’d encourage you to add to that picture is a neurological assessment from a PX Docs-trained chiropractor who understands the “Perfect Storm” framework and the role of subluxation and dysautonomia in the Asperger profile. Not as a replacement for your existing team, but as the missing piece.
When the nervous system’s capacity to regulate is restored, everything else becomes more accessible. Your child’s ability to learn, connect, manage sensory input, and move through transitions all gets easier when the system underneath isn’t in crisis mode.
Use the PX Docs directory to find a Neurologically-Focused Chiropractic Care provider near you. As always, work collaboratively with your child’s medical team, and continue any therapies that are providing value. Your child is more than their diagnosis, and their nervous system is more capable of change than most people realize.
Frequently Asked Questions About Asperger Syndrome in Children
Can a child with Asperger syndrome live a normal life?
Yes. Children with Asperger syndrome can thrive, especially with early support that addresses the underlying nervous system dysregulation driving their challenges. When the Autonomic Nervous System shifts out of chronic sympathetic dominance and vagal tone improves, sensory tolerance, emotional regulation, and social engagement often improve significantly.
What is the main difference between Asperger syndrome and ADHD?
Asperger syndrome primarily involves social communication differences and restricted interests, while ADHD centers on attention regulation, impulsivity, and hyperactivity. However, both conditions frequently co-occur because they share a common root in autonomic nervous system dysfunction and sympathetic dominance. Many children carry both diagnoses.
What causes Asperger syndrome in children?
Asperger syndrome results from a combination of genetic predisposition and neurological stressors that accumulate during development. The “Perfect Storm” framework identifies prenatal stress, birth trauma, and early childhood toxic load as key factors that can overwhelm the developing nervous system, leading to subluxation, dysautonomia, and the sensory, social, and regulatory challenges seen in this profile.
Is chiropractic care safe for children with Asperger syndrome?
Neurologically-Focused Chiropractic Care uses precise, gentle adjustments tailored to each child’s individual neurological patterns as measured by INSiGHT Scans. It does not diagnose or treat Asperger syndrome or any condition. Instead, it addresses subluxation and nervous system dysregulation to help restore autonomic balance, which can support improvements in sensory processing, emotional regulation, and overall adaptive capacity.
How long does it take to see improvement with neurological chiropractic care?
Families typically observe improvements in a predictable sequence: sleep often improves first, then gut function, then sensory tolerance, then emotional regulation, and social-communication gains often come last. The timeline varies based on the severity of subluxation and dysautonomia identified on INSiGHT Scans, but many families report early changes within the first few weeks of consistent care.