You finally figured out sleep. Your toddler was going down easily, staying asleep, and you were reclaiming your evenings. Then suddenly—out of nowhere—it all fell apart. Bedtime turns into a battle. Night wakings are back. Naps are disappearing.
What you’re dealing with is toddler sleep regression, one of the most exhausting and misunderstood parts of early childhood development.
Most resources will tell you this is normal, give you a few routine tips, and send you on your way. That’s partially true, but there’s a layer to toddler sleep regression that almost nobody talks about: what’s happening inside your child’s nervous system. For some kids, regressions are mild and brief. For others, they’re severe, prolonged, and connected to bigger patterns of dysregulation that show up across sleep, behavior, digestion, and immune health. This article covers both.
What Is Toddler Sleep Regression?
A toddler sleep regression is when a child who was previously sleeping well suddenly has significant trouble falling asleep, staying asleep, or napping, without an obvious external cause like illness or travel.
The word “regression” can feel alarming, but it’s really just a disruption. Your child hasn’t forgotten how to sleep or unlearned their routine. What’s happening is that their brain and body are undergoing rapid changes, which are temporarily hijacking their ability to settle down and stay asleep.
Regressions typically last anywhere from weeks to months. Most children do cycle back to better sleep on their own with consistent support, but the experience while you’re in the middle of it can be genuinely grueling.
When Does Toddler Sleep Regression Happen?
Toddler sleep regressions tend to cluster around predictable developmental windows. Here’s when parents are most likely to encounter them:
The 12-Month Sleep Regression
Right around the first birthday, many toddlers hit a rough patch with sleep. They’re transitioning from two naps to one, which will significantly shift their sleep schedule. Language is exploding, walking is starting, and separation anxiety often peaks around this time. The nap transition alone can cause overtiredness as their bodies adjust to longer wake windows.
The 18-Month Sleep Regression
The 18-month sleep regression is considered one of the toughest. At this age, toddlers are becoming fiercely independent, developing strong opinions, and testing limits, including at bedtime. Separation anxiety is still very real. They’re acquiring language fast, which creates cognitive excitement that doesn’t turn off easily. Molars are coming in. A lot is happening at once.
Night wakings increase, naps become difficult, bedtime resistance escalates, and early morning waking often returns. Parents often describe this period as feeling like they’ve been teleported back to the newborn phase.
The 2-Year Sleep Regression
At age 2, another wave hits. Toddlers are transitioning out of cribs, potty training is starting, imagination is expanding (hello, nightmares), and autonomy battles are in full swing. The cognitive leap happening at 2 years old is significant; children are processing the world in much more complex ways, and that heightened awareness can make settling down at night genuinely difficult.
The 2-year-old sleep regression often gets worse before it gets better, especially if there are additional life stressors like a new sibling, a daycare transition, or a move.
The 3-Year Sleep Regression
Less commonly discussed but very real: around age 3, another round of sleep disruption can occur. Three-year-olds are navigating expanded social awareness, fears that feel very real to them, and an active imagination that generates vivid dreams.
Bedtime resistance and night wakings often resurface, and the content of what’s keeping them up shifts from physical discomfort to emotional and imaginative triggers.
Signs Your Toddler Is in a Sleep Regression
The clearest indicator is a sudden change in a child who had been sleeping well. Common signs include:
- Increased night wakings after a period of sleeping through
- Difficulty falling asleep at nap time or bedtime despite clear tiredness
- Bedtime resistance, stalling, crying, climbing out, calling for you repeatedly
- Shortened naps or refusing to nap altogether
- Early morning waking (the dreaded 4 or 5 AM start to the day)
- Clinginess and increased separation anxiety at bedtime
- Fussiness and mood changes during the day from cumulative sleep loss
It’s worth noting that these signs can also indicate illness, teething discomfort, or environmental issues, so rule those out first. But if your child appears healthy and the disruption correlates with a developmental leap, a life change, or one of the age windows above, sleep regression is the likely culprit.
Why Does Toddler Sleep Regression Happen?
The conventional explanation focuses on developmental milestones, and that’s accurate, as far as it goes.
- Developmental milestones create neurological activity that doesn’t switch off neatly at bedtime. When a toddler is mastering walking, talking, or problem-solving, their brain is building new neural pathways at an accelerated rate. That biological process doesn’t pause when you turn the lights off.
- Separation anxiety peaks multiple times throughout toddlerhood. For a child who doesn’t yet fully understand time and permanence, being separated from their parent at bedtime can feel genuinely alarming, not just emotionally inconvenient.
- Nap transitions disrupt the balance of daytime and nighttime sleep. Moving from two naps to one (around 12-18 months) or dropping naps entirely (around 3-4 years) shifts everything and creates a period of adjustment as the body recalibrates sleep timing and consolidation.
- Life changes, such as a new sibling, starting daycare, or moving, activate a stress response in toddlers that directly impacts sleep. These don’t have to be dramatic events. Even small changes in routine can be enough.
These are real, valid explanations. But they explain the trigger, not why some children sail through regressions in two weeks while others are in chaos for months. That gap points to something deeper.
The Nervous System Piece Nobody’s Talking About
Your child’s ability to fall asleep, stay asleep, and cycle through deep and restorative sleep is fundamentally regulated by their Autonomic Nervous System. This system has two branches that need to work in balance:
- The Sympathetic Nervous System: The “gas pedal” is activated during stress, threat, or excitement
- The Parasympathetic Nervous System: The “brake pedal” is responsible for rest, digestion, and healing
For a child to fall asleep and stay asleep, the parasympathetic system needs to win at bedtime. The brake has to engage. But for children whose nervous systems are already running hot, already stuck in sympathetic overdrive, that brake doesn’t work the way it should.
Think about it like this: a toddler who’s mildly stressed at bedtime can self-regulate and drift off. A toddler whose nervous system dysregulation has been building since infancy hits bedtime with a nervous system that’s already maxed out.
The developmental triggers that cause normal sleep regression hit a nervous system that has no reserve capacity. The result isn’t a two-week blip; it’s months of fractured sleep, early wakings, and a child who can’t turn off, no matter how tired they are.
This is the critical distinction that conventional sleep advice misses entirely.
The Role of the Vagus Nerve
The vagus nerve is the primary driver of the Parasympathetic Nervous System. It connects the brainstem to the heart, lungs, and gut, and it’s responsible for signaling the body to shift from activation into rest. Vagus nerve dysfunction, when that nerve isn’t firing properly, means the body literally struggles to downshift.
Research shows that sleep architecture disturbances are closely linked to autonomic imbalance. When the sympathetic system dominates, children spend more time in light sleep stages, cycle poorly through deeper phases, and wake more easily.
How the “Perfect Storm” Connects to Sleep Regression
For children who struggle with persistent sleep problems, where regression after regression hits harder than it should, or sleep never fully recovers from the last round, we often see a deeper neurological pattern at work.
At PX Docs, we call this the “Perfect Storm.”
The “Perfect Storm” describes how a sequence of stressors, prenatal stress, birth trauma, and early childhood challenges, creates a cumulative neurological load that keeps a child’s nervous system stuck in sympathetic dominance.
- Maternal stress during pregnancy, whether from life circumstances, fertility treatments, or health complications, means the developing baby’s nervous system is bathed in stress hormones during its most plastic, programmable phase. That nervous system is essentially calibrated for stress from the start.
- Birth Trauma & interventions, particularly with interventional deliveries, forceps, vacuum extraction, prolonged labor, induction, and C-section, subject the delicate structures of the upper neck and brainstem area to significant forces. These areas house the origin points of the vagus nerve and house nuclei that regulate autonomic function. Physical strain here can create lasting neurological interference patterns, which we call subluxation.
- Early childhood itself. Illness, antibiotics, emotional stress, and sensory overload layer on top of a nervous system that was already compromised.
The result is a child who has, as Dr. Ebel puts it, a “stuck” nervous system. Their gas pedal is mashed down. Their brake barely works. And when developmental milestones, the normal triggers for sleep regression, hit this nervous system, the disruption is amplified far beyond what conventional sleep strategies can address.
This is why some children have multiple severe regressions back-to-back. It’s why routine changes feel catastrophic to some toddlers and minor to others. The difference isn’t parenting, it’s neurological load.
And importantly, the sleep disruption rarely travels alone. Parents of these children often also describe chronic constipation, frequent illness, sensory sensitivities, emotional dysregulation, and behavioral challenges. These are all branches of the same underlying imbalance in the nervous system.
Conventional Strategies That Still Matter
Even with a deeper understanding of the neurological picture, consistent routines and environmental strategies play a real role, especially for mild to moderate regressions. Here’s what’s well-supported:
- Maintain a consistent bedtime routine. The sequence of bath, book, bed signals the nervous system that sleep is coming. For a child whose sympathetic system is already elevated, predictability helps lower the activation threshold.
- Watch for overtiredness. An overtired toddler has released cortisol to compensate for fatigue, which makes falling asleep paradoxically harder. Most toddlers need to be asleep, not just starting their routine, within 4.5 to 5 hours of waking from their nap.
- Protect the sleep environment. Dark, cool, and quiet create the sensory conditions where the parasympathetic system can engage. Noise machines can reduce startling, which is especially helpful for children with heightened nervous system sensitivity.
- Stay consistent with nighttime responses. Inconsistency, sometimes rushing in, sometimes waiting, keeps the nervous system in a state of unpredictability, which sustains alertness. Whatever response you choose, repeating it the same way each time helps your toddler’s nervous system learn what to expect.
- Limit screen exposure before bed. Blue light suppresses melatonin, but the more significant issue is that fast-paced visual stimulation activates the sympathetic system. A child watching screens before bed is revving the engine right when you need them to downshift.
- Don’t introduce sleep habits you don’t want to maintain. Rocking or nursing to sleep during a regression teaches the nervous system that adult help is required to complete the transition to sleep, which means every sleep cycle that ends in light sleep (every 45-90 minutes through the night) becomes a waking.
Signs the Regression May Be More Than Routine
Conventional sleep advice works for children with basically regulated nervous systems who hit a developmental bump. But if you’re seeing any of the following, there’s a deeper conversation to have:
- Multiple consecutive regressions with no real return to baseline
- A child who has never been a good sleeper, even in infancy
- Sleep disruption that co-occurs with chronic constipation, frequent illness, sensory sensitivities, or emotional volatility
- Regressions that are dramatically more severe than what most parents describe
- A child who seems exhausted but can’t stop moving or settle
These patterns suggest the nervous system isn’t just bumping up against a developmental milestone; it’s already running in a state of chronic dysregulation. The milestone just made it visible.
This is where Neurologically-Focused Chiropractic Care comes in.
How Neurologically-Focused Chiropractic Care Supports Sleep Regulation
This is where INSiGHT Scans become so useful for parents who are frustrated by conventional explanations.
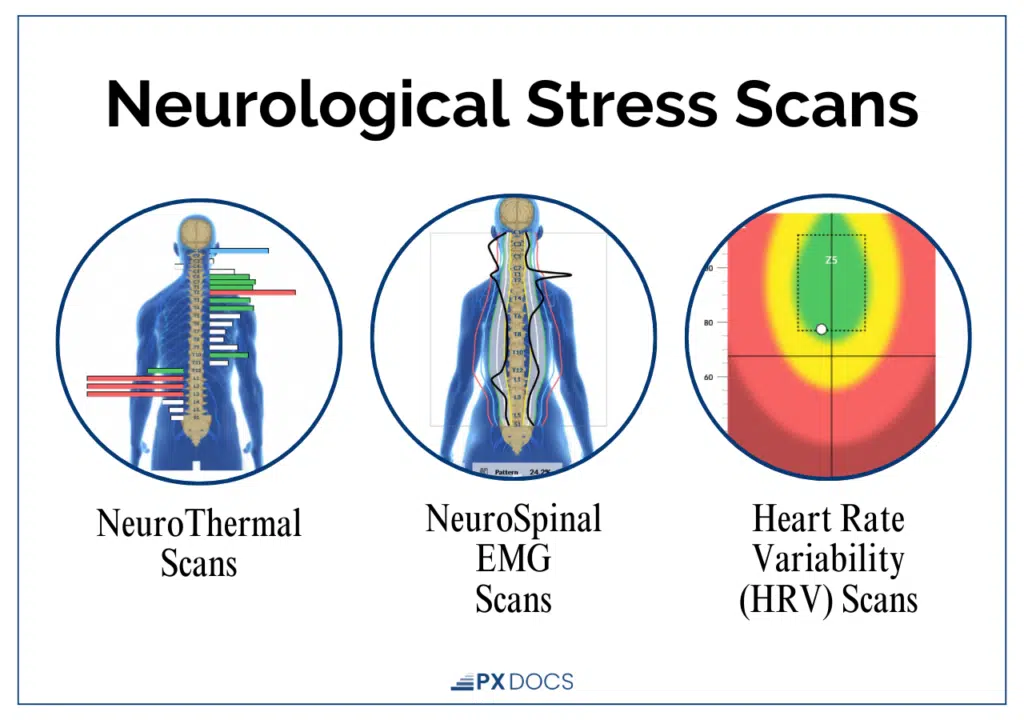
It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for toddler sleep regression or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
These scans measure actual nervous system function, autonomic balance, sympathetic activation levels, and specific patterns of neurological stress, in a way that no blood test or standard pediatric exam captures. For families who’ve been told “everything looks fine” while their child continues to struggle with sleep, this objective window into nervous system function can be revelatory.
When a Neurologically-Focused Chiropractor identifies subluxation, neurological interference patterns, and addresses it through specific, gentle adjustments, what parents consistently report is not just improved sleep in isolation. It’s a global shift: better sleep, better digestion, easier emotional regulation, reduced reactivity. Because all of these systems are downstream of the same nervous system that was dysregulated.
The healing sequence that Dr. Tony Ebel describes at PX Docs follows a predictable order: nervous system stabilization comes first, then the “Core Four” functions, sleep, digestion, immune function, and motor development, begin to come online. Sleep is one of the first places families notice the change because it reflects parasympathetic function so directly.
If your toddler’s sleep regression feels like it’s connected to a bigger picture, this is where to look.
Moving Forward: You’re Not Alone in This
Toddler sleep regression is genuinely hard. The sleep deprivation is real, the frustration is valid, and the exhaustion of doing everything “right” and still not seeing improvement is one of the most common things parents describe when they find PX Docs.
Here’s what we want you to understand: if your child’s sleep regression feels bigger than what the standard advice accounts for, you’re probably right. There’s a reason some kids sail through these windows, and some kids don’t. That reason lives in the nervous system.
Your child’s body is designed to regulate, to rest, and to heal. Sometimes it just needs the neurological interference cleared out of the way first. If you’re ready to find out what’s driving your toddler’s sleep struggles at a deeper level, find a Neurologically-Focused Chiropractor near you through the PX Docs provider directory. A comprehensive evaluation and INSiGHT Scan can give you the objective picture you’ve been missing, and a clear path forward.