Atonic seizures, often called “drop attacks,” are terrifying to witness. One moment, a child is sitting or standing, the next they’ve suddenly lost all muscle tone and collapsed without warning. Families dealing with these seizures often live on constant alert, bracing for the next fall and the injuries that can come with it.
Most parents are given a familiar explanation: abnormal electrical activity in the brain, an unclear cause, and medications as the primary solution, especially when atonic seizures appear alongside conditions like Lennox-Gastaut syndrome. But this explanation leaves out a critical piece of the puzzle. From a neurological perspective, these seizures don’t simply start in the brain; they reflect a deeper pattern of nervous system dysregulation that often begins much earlier in development.
In this article, we’ll explore what atonic seizures look like through a nervous system lens, why factors like early stress and vagus nerve dysfunction matter, and how addressing the root neurological imbalance, rather than only suppressing symptoms, can open new possibilities for healing and long-term stability.
What Are Atonic Seizures?
Atonic seizures are a type of seizure characterized by sudden and complete loss of muscle tone. The word “atonic” literally means “without tone.” Your child’s muscles suddenly go completely limp. This can happen multiple times a day.
Also called drop seizures or drop attacks, these seizures cause children who are standing to fall directly to the ground with no ability to break their fall. If sitting, their head and upper body slump forward. Research indicates most atonic seizures last less than 15 seconds, but during those seconds, muscle control disappears entirely. Your child may drop what they’re holding, their eyelids droop, and if standing, they’ll fall, which is why head injuries are a common complication.
During an atonic seizure, muscles go limp (like a rag doll). This differs from tonic seizures, where muscles become stiff and rigid (like a tree trunk). Most children remain partially conscious during the episode, though awareness is reduced. After it ends, some return to normal activity quickly, while others need time to recover.
Atonic seizures can be focal motor atonic seizures (starting on one side of the brain, affecting one body part) or generalized onset atonic seizures (affecting both sides of the brain and the whole body). The generalized type is more common and causes complete collapse. These seizures typically begin in childhood and are particularly associated with certain epilepsy syndromes, especially Lennox-Gastaut syndrome.
Types of Atonic Seizures and Associated Syndromes
Atonic seizures aren’t one-size-fits-all. Understanding the types and their associations with specific epilepsy syndromes helps you better understand your child’s diagnosis.
- Generalized onset tonic seizures are the predominant epileptic seizures in Lennox-Gastaut syndrome, affecting both sides of the brain from the start and causing loss of muscle tone throughout the entire body. The person typically isn’t fully aware during the event.
- Focal Motor Atonic Seizures start in one brain area and affect muscle tone in just one body part—one arm goes limp, or one side of the face droops. These can sometimes spread to become generalized.
- Lennox-Gastaut Syndrome (LGS) is the syndrome most strongly linked with atonic seizures. This severe form of epilepsy begins in early childhood and involves multiple seizure types. Children with LGS often experience developmental delays.
- Epilepsy with Myoclonic-Atonic Seizures (formerly Doose syndrome) is an uncommon syndrome that only accounts for 2% of childhood epilepsies. It features myoclonic-atonic seizures, brief muscle jerks immediately followed by loss of tone and falling. Beginning between ages two and six, many children with this syndrome eventually outgrow their seizures or achieve good control, though the active phase can be challenging.
Not every child with atonic seizures has one of these syndromes. Some have them as part of less-defined epilepsy or in isolation. The distinction matters because prognosis and care approaches vary significantly.
What Causes Atonic Seizures?
Atonic seizures are traditionally explained as sudden surges of synchronized electrical activity in the brain, affecting regions that control muscle tone, such as the cerebellum and motor cortex. Genetic mutations, structural brain abnormalities, metabolic conditions, or birth-related injuries are often cited as contributing factors.
However, even when these causes are identified, they do not fully account for why some children develop atonic seizures while others with similar findings do not.
Conventional care focuses on suppressing seizure activity through medications or surgical interventions, addressing the electrical symptom rather than the underlying cause. A neurological root-cause perspective shifts the focus upstream, examining how early disruptions to the developing nervous system, prenatal stress, birth trauma, or autonomic dysregulation, can predispose a child to these seizures long before abnormal electrical activity appears.
The Neurological Root Cause: Understanding the “Perfect Storm”
Atonic seizures aren’t always random genetic bad luck or mysterious brain electricity. They’re often the end result of a “Perfect Storm,” a series of stressors and injuries to the nervous system that accumulate over time, starting as early as pregnancy.
At PX Docs, through detailed neurological assessments using INSiGHT scans, we can see patterns of nervous system dysfunction that precede and contribute to seizure activity. The foundation for seizures is often laid months or years before the first drop attack. The “Perfect Storm” unfolds in three stages:
Prenatal Stress and Programming
Your child’s nervous system begins developing in the womb. High maternal stress during pregnancy—emotional challenges, physical demands, medical complications—can affect how your baby’s Autonomic Nervous System develops.
The Autonomic Nervous System has two branches:
- Sympathetic (gas pedal for fight-or-flight)
- Parasympathetic (brake pedal for rest and calm).
Chronic prenatal stress can program a baby to be born with sympathetic dominance—stuck gas pedal, weak brakes. This doesn’t directly cause seizures, but it creates a vulnerable foundation in which the nervous system lacks the regulatory capacity it needs.
Birth Trauma and Physical Injury
Birth interventions, vacuum extraction, forceps, pulling, C-sections, create physical stress on the upper cervical spine and brainstem. The brainstem houses the vagus nerve’s origin and structures that control muscle tone, consciousness, and the seizure threshold.
When birth creates subluxation (dysfunction that interferes with nervous system communication), its effects ripple throughout the entire nervous system. For some babies, this can cause immediate symptoms such as colic or feeding difficulties. For others, dysfunction is subtle but still present, quietly affecting nervous system development.
The Cascade of Stressors
Additional stressors pile on: repeated antibiotics destroying gut bacteria that produce neurotransmitters, ear infections creating chronic vagus nerve inflammation, reflux medications affecting gut health and mineral absorption, sensory challenges revealing regulation problems, and developmental delays. None alone causes seizures, but together in an already struggling system, they create the “Perfect Storm.” The nervous system loses its ability to regulate properly, electrical activity becomes chaotic, and muscle tone maintenance breaks down.
Understanding the “Perfect Storm” changes the question from “Why did my child develop seizures?” to “What can we do to support my child’s nervous system so it can function the way it was designed to?”
The Vagus Nerve Connection
The vagus nerve is the key to understanding why nervous system dysregulation leads to atonic seizures, and why addressing it offers real hope for children who haven’t responded well to medications.
The vagus nerve runs from the brainstem down through the neck into the chest and abdomen. It’s the main parasympathetic component—your body’s “brake pedal” promoting calm, rest, digestion, and healing. Crucially, research shows it’s 80% sensory, constantly sending information from the body to the brain.
In children with atonic seizures, vagus nerve dysfunction is almost always present, happening in two ways:
Birth Trauma to the Vagus Nerve
The vagus nerve exits the skull through the jugular foramen, right next to the upper cervical vertebrae. During difficult births involving pulling, twisting, or forceps-assisted delivery, this area experiences significant force. Subluxation or misalignment can directly compress or irritate the vagus nerve at its origin.
When the vagus nerve is injured or compressed at birth, communication between the brain and body becomes disrupted. The parasympathetic “brake pedal” doesn’t function properly. The child stays stuck in sympathetic dominance—constantly stressed, unable to calm down, struggling with digestion, sleep, and regulation. Crucially for seizures, the brainstem and surrounding structures never develop the stable electrical patterns they need.
Underdevelopment of Vagus Nerve Function
Many children have an underdeveloped vagus nerve system. The nerve isn’t damaged; it just never got the chance to develop properly.
Normal vagus nerve development happens through co-regulation with caregivers, successful feeding, proper sleep cycles, and physical movement. But when a baby is born with prenatal stress programming and birth trauma, they struggle with all these milestones. They can’t latch well, can’t sleep well, and stay in constant sympathetic overdrive. By toddlerhood, these kids have massively dysfunctional vagus nerve systems—weak brakes, stuck gas pedal.
When the nervous system is chronically dysregulated like this, seizure thresholds drop and the brain becomes more susceptible to disorganized electrical activity.
Why This Matters
Understanding vagus nerve dysfunction provides a clear intervention target. Rather than just suppressing seizure activity with medications, which often have significant side effects and don’t work for many children, you can address the nervous system dysfunction that is making seizures more likely.
When you support vagus nerve function and restore autonomic balance, brainstem regulation becomes more stable, seizure threshold increases, sleep improves, allowing nervous system recovery, digestion normalizes, supporting neurotransmitter production, stress responses become appropriate, and the body’s natural healing processes engage.
A Neurological Approach: Addressing the Root Cause
What if instead of just suppressing seizure activity, you could support your child’s nervous system to function the way it was designed to?
Neurologically-Focused Chiropractic Care isn’t about replacing medical care or abruptly stopping medications. It’s about adding a foundational layer that addresses the subluxation, vagus nerve dysfunction, and autonomic imbalance that set the stage for seizures.
At PX Docs, we use INSiGHT scans to measure nervous system function in ways conventional diagnostics don’t—seeing where your child’s system is stuck in sympathetic overdrive, where communication breaks down, and how their body handles stress. These scans provide objective data about the dysautonomia patterns behind the seizures.
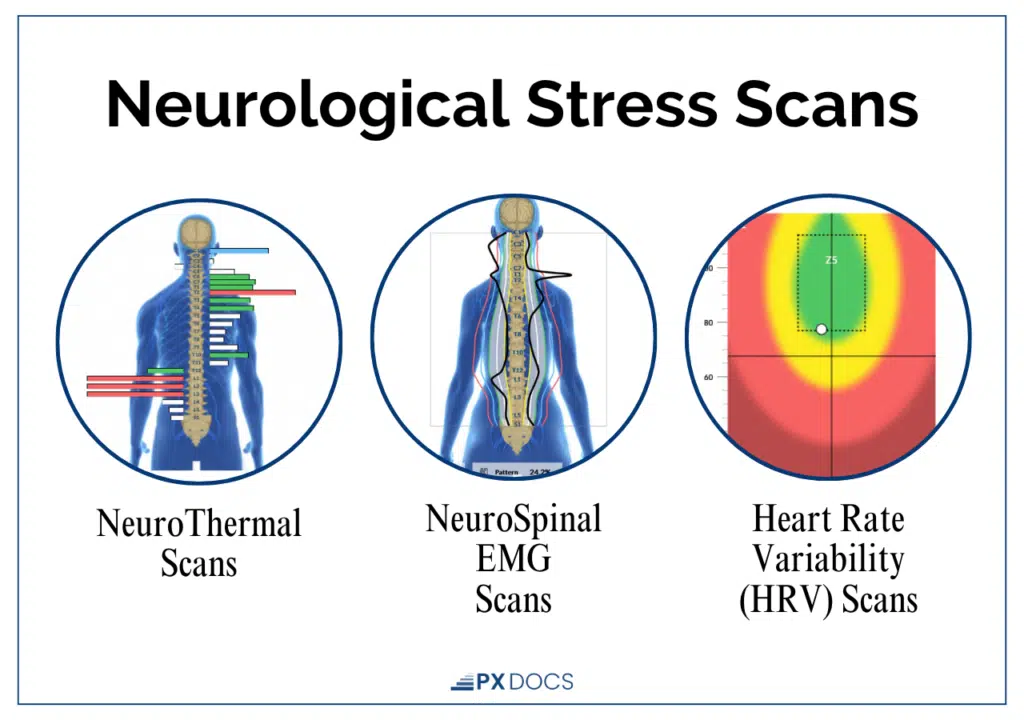
What we typically find:
- High sympathetic tone (stuck gas pedal)
- Weak parasympathetic function (broken brakes)
- Significant stress patterns in the upper cervical spine and brainstem area
- Poor vagus nerve function affects anything from sleep to digestion.
With this information, we create customized care focused on gentle, precise adjustments to the upper cervical spine where subluxation interferes with nervous system function. The goal is restoring your child’s nervous system’s ability to regulate itself. When subluxation is corrected, and vagus nerve function improves, the parasympathetic “brake pedal” starts working, sleep improves (crucial for healing and seizure threshold), digestion normalizes (supporting neurotransmitter production), and the brainstem functions with more stability.
This doesn’t promise overnight miracles, and it is most definitely not a treatment or cure for seizures. Neurological healing takes time, especially when addressing dysfunction building since pregnancy or birth. But we consistently see progressive improvement, not just in seizure frequency, but in overall neurological function. Many families find that as nervous system function improves, they can work with their neurologist to reduce medication dosages or eventually wean off entirely.
For example, Alice’s family spent years navigating a wide range of severe daily seizures that kept their world very small. Many days were spent at home, searching for answers and holding onto hope that something could finally help.
After consistent care and nervous system healing, mom says, “Alice hasn’t had a seizure since April 22nd, 2024. We can breathe. We can smile and laugh again. We make plans with friends and go places and enjoy foods we haven’t touched in over a year. I took her out for ice cream, and her face just lit up when she had her first taste. We’re healing from the months and months of fear and trauma we experienced as a family. We’re so happy and content just to be living this super normal and sometimes even boring life!”
A Path Forward
Atonic seizures aren’t just a brain electricity problem; they’re a sign of a nervous system that’s been dysregulated, often from before birth. Understanding the role of prenatal stress, birth trauma, and early childhood factors shifts how we approach healing.
Neurologically-Focused Chiropractic Care works to restore balance by supporting vagus nerve function, correcting upper cervical subluxation, and improving autonomic regulation. This approach addresses the root causes of dysregulation, complementing, not replacing, medical care. Your child doesn’t have to rely solely on medication. With the right support, their nervous system can function properly, giving them a real chance to heal from the inside out. Find a PX Doc through our directory who specializes in children with seizures to explore a tailored plan for recovery.