Your child constantly interrupts, melts down during phone calls, and demands reassurance again and again—despite consistent parenting strategies like reward charts, time-outs, and one-on-one attention.
The behavior isn’t improving, and explanations like ADHD, anxiety, or “some kids are just like this” don’t fully explain what’s happening.
What’s often missed is the neurological driver behind extreme attention-seeking behavior. When a child’s nervous system is chronically dysregulated and stuck in fight-or-flight, attention-seeking becomes compulsive rather than intentional. We’ll talk about why behavioral strategies alone often stall, and how objective nervous system measurements can clarify what’s really going on.
Understanding the Difference: Normal vs. Neurologically-Driven Attention-Seeking
Attention-seeking behavior describes actions a child takes to gain the attention of caregivers, teachers, or peers. For infants and toddlers, this is completely normal—crying when hungry, calling for parents, seeking comfort.
Normal attention-seeking responds to positive attention. When you give a developmentally typical child focused one-on-one time, the demanding behaviors decrease. It’s situational, worse when tired, hungry, or during transitions, and gradually improves as the child matures.
Dysregulated attention-seeking looks different. It’s compulsive rather than responsive. Your child can’t seem to stop, even when they’re getting plenty of positive reinforcement. The behavior doesn’t improve with consistent boundaries or special time. Sometimes it escalates.
This is where nervous system regulation comes in. When a child’s Autonomic Nervous System is stuck in fight-or-flight mode, their behavior reflects that internal chaos. The gas pedal (Sympathetic Nervous System) is pressed down, and the brake pedal (Parasympathetic Nervous System) isn’t engaging properly. Every interaction feels high-stakes. Every moment without direct attention triggers a stress response.
This neurological component explains why some children don’t respond to even the most dedicated behavioral interventions. You can’t reward-chart your way out of autonomic dysregulation.
Recognizing When It’s More Than Behavior
Certain patterns, particularly when they persist despite consistent, loving intervention, suggest nervous system dysfunction rather than purely behavioral causes:
- Physical manifestations: Hitting, kicking, or pushing when not receiving immediate attention. Self-harm behaviors like head-banging or scratching. These are desperate regulation attempts when internal systems are overwhelmed.
- Verbal patterns: Constant interrupting, even mid-sentence. Asking the same questions repeatedly despite receiving clear answers. Yelling or making loud noises, specifically when caregivers are engaged with someone else.
- Emotional displays: Meltdowns lasting 30+ minutes when a sibling gets attention. Demanding reassurance multiple times within an hour. Complete emotional collapse when not the center of every interaction.
Red flags that signal nervous system involvement:
- The behaviors don’t respond to positive reinforcement despite consistent implementation
- The intensity escalates despite consistent boundaries
- The attention-seeking is accompanied by sleep problems, chronic digestive issues, frequent illnesses, or sensory sensitivities
When you see these red flags, you’re not looking at a behavioral disorder alone. You’re looking at a nervous system crying out for regulation.
What Conventional Pediatrics Misses
Ask any pediatrician or child psychologist about extreme attention-seeking, and you’ll hear familiar explanations: unmet emotional needs, ADHD, anxiety, trauma history, or simply boredom. These factors absolutely play a role. But here’s what conventional pediatrics consistently misses: these explanations address symptoms, not the root neurological dysfunction.
The limitation becomes clear when you implement every recommended strategy and see minimal improvement. You’ve increased one-on-one time, established consistent routines, and worked with therapists. Yet the extreme attention-seeking persists.
Why? Because behavioral interventions require a regulated nervous system to take hold. When the Autonomic Nervous System can’t maintain its baseline, all the strategies built on that foundation have limited effectiveness.
The Nervous System Connection No One Talks About
Your Autonomic Nervous System operates like a car with two pedals. The sympathetic branch (gas pedal) activates your body for action. The parasympathetic branch (brake pedal) helps you rest, digest, connect socially, and recover from stress.
When a child’s nervous system gets stuck in sympathetic dominance—gas pedal constantly pressed—their entire physiology reflects that chronic activation. Heart rate variability decreases. Muscle tension increases. Digestion slows. Sleep quality deteriorates. Immune function suffers.
And behaviorally? The child can’t downregulate. They can’t self-soothe. The attention-seeking becomes compulsive—a desperate attempt to get the nervous system back to baseline through external regulation since internal regulation isn’t working.
This is where the vagus nerve becomes critical. The vagus nerve is the primary pathway for parasympathetic (brake pedal) function, connecting the brainstem to nearly every major organ and influencing social engagement. When vagal function is compromised, the child struggles to make eye contact, read social cues, or feel safe in connection.
Research on Polyvagal Theory demonstrates how vagal tone determines a child’s capacity for calm social engagement versus defensive stress responses. Kids with poor vagal tone can’t access the neurological state that allows for regulated interaction. They’re stuck in survival mode.
The “Perfect Storm”: How Nervous System Dysfunction Develops
At PX Docs, we refer to the combination of factors that create extreme attention-seeking behavior as the “Perfect Storm.” This describes how a series of events, often beginning early in life, creates a cascading effect that disrupts nervous system development.
Stage 1: Prenatal Stress and In-Utero Programming
The nervous system begins forming in the womb. When a mother experiences chronic stress during pregnancy, her body produces elevated cortisol that crosses the placental barrier and impacts the developing fetal nervous system. The child’s nervous system essentially gets calibrated to expect a high-stress environment, setting the gas pedal sensitivity too high and the brake pedal responsiveness too low.
Stage 2: Birth Trauma and Early Nervous System Injury
Approximately 32% of births in the United States are cesarean sections, and many vaginal births involve interventions like forceps, vacuum extraction, or induction. While these can be life-saving, they also create mechanical stress on the infant’s delicate nervous system.
The upper cervical spine, where the brainstem transitions into the spinal cord, is particularly vulnerable during birth. The vagus nerve can experience compression or irritation during traumatic birth. Remember when your pediatrician said the colic would pass? The latching difficulties were “normal”? Those weren’t random—they were your child’s nervous system signaling distress from day one.
Stage 3: Early Childhood Stressors and Toxic Accumulation
Multiple rounds of antibiotics disrupt the gut-brain axis, affecting neurotransmitter production and emotional regulation. Falls, injuries, and screen time add physical stress to the developing spine and nervous system. Each stressor alone might not tip the scales, but the cumulative effect creates sympathetic lock—the nervous system gets stuck in fight-or-flight mode and can’t find its way back.
The Cascade: From Subluxation to Attention-Seeking
Subluxation is what results from all these accumulated stressors—it’s neurological interference, like static on a phone line. When subluxation disrupts brain-body communication, the nervous system can’t accurately assess whether the environment is safe or threatening. The child’s system becomes hypersensitive to any sign of separation, interpreting it as a survival threat.
Attention-seeking becomes compulsive because it’s the nervous system’s attempt to regulate through external connections. The child isn’t being manipulative or difficult—they’re being dysregulated.
How to Objectively Measure Nervous System Patterns
One of the biggest challenges with nervous system dysfunction is that it can’t be seen on standard medical tests. Blood work looks normal. MRIs come back clear. But the dysregulation is real—and now it’s measurable.
INSiGHT scanning technology provides objective data about how the nervous system is functioning:
- HRV (Heart Rate Variability) Scan measures the variation in time between heartbeats, reflecting how well the Autonomic Nervous System can adapt to stress. Kids with extreme attention-seeking often show erratic patterns—the gas pedal and brake pedal are fighting each other constantly.
- sEMG (Surface Electromyography) Scan maps neuromuscular tension along the spine. High readings in the upper cervical and thoracic regions indicate chronic sympathetic activation—the body is literally holding tension that never releases.
- Thermal Scan detects temperature differences along the spine, revealing autonomic regulation patterns. Asymmetric thermal patterns show the system struggling to maintain balance.
These scans provide validation. They show parents that the behavioral observations they’re making have a physiological basis. The “invisible” dysfunction becomes visible, measurable, and—most importantly—addressable.
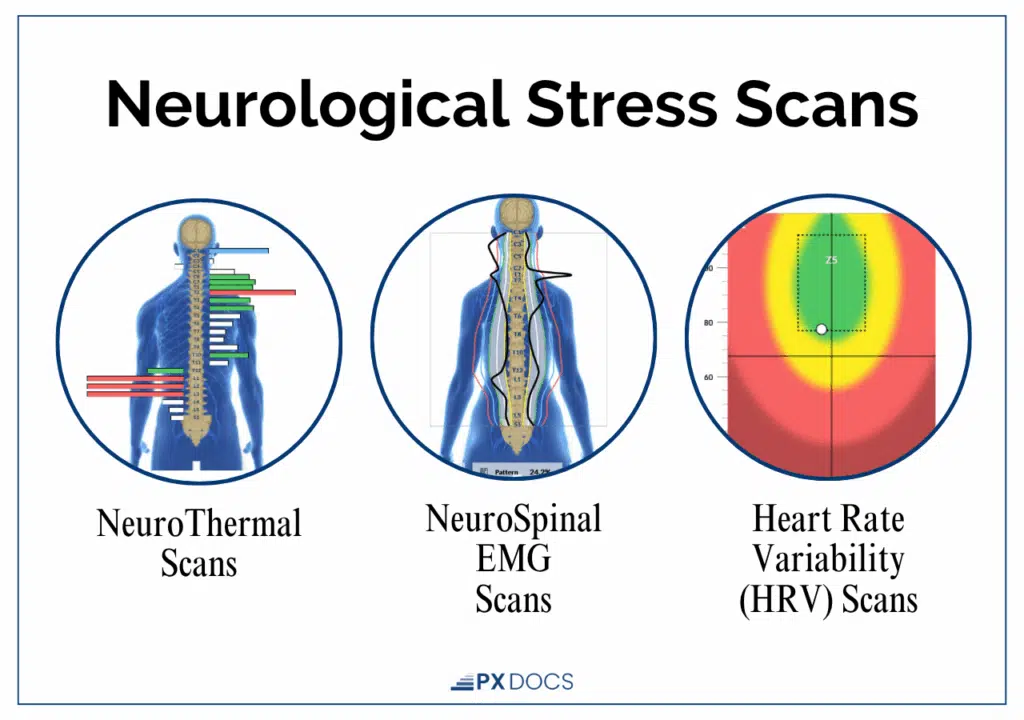
Important disclaimer: These scans reveal neurological function patterns and don’t diagnose medical conditions; they guide care decisions by showing how the nervous system is functioning.
Addressing the Root Cause: How Neurologically-Focused Chiropractic Care Helps
Neurologically-Focused Chiropractic Care is different from traditional chiropractic care. This isn’t about back pain or structural alignment. It’s about targeting subluxation—neurological interference that disrupts brain-body communication—and restoring balance of the Autonomic Nervous System.
The approach uses gentle, specific adjustments to the neurospinal system that target subluxation. Think of it like removing static from a phone line so the signal can come through clearly.
What to Expect:
Care begins with baseline INSiGHT scans to understand exactly how the nervous system is functioning. Progress is tracked through re-scans, providing objective evidence of neurological changes. Nervous system healing follows a specific sequence, and behavioral changes aren’t always the first to come.
This progression reflects the hierarchy of nervous system healing. We often see changes in early “soft signs” first—such as improvements in sleep, digestion, and subtle shifts in behavior—before more noticeable gains in emotional regulation and outward behavior emerge. These early indicators signal that the nervous system is stabilizing, laying the foundation for lasting behavioral change.
Complementary Approaches
Neurologically-Focused Chiropractic Care provides the foundation, but other therapies remain valuable. Occupational therapy, speech therapy, and behavioral strategies all work better when the neurological foundation is stable.
Parents can support healing through co-regulation practices, predictable routines, sensory-friendly environments, limited screen time, nature exposure, and gut-supportive nutrition. These strategies support healing but can’t replace care that addresses subluxation and dysautonomia directly.
From Extreme Attention-Seeking to Regulated Connection
Extreme attention-seeking behavior isn’t a character flaw or a parenting failure; it’s a nervous system crying out for regulation. Your child wants to feel calm and connected. When we remove the neurological interference and give the body what it needs to heal, that extreme attention-seeking can naturally improve—not because we’ve changed the behavior, but because we’ve restored the foundation.
The “Perfect Storm,” prenatal stress, birth trauma, and early childhood stressors, creates the neurological dysfunction that manifests as extreme attention-seeking. Understanding this causation validates your experience, explains why behavioral interventions alone haven’t been enough, and points to a solution that addresses the root cause rather than the symptoms.
Your child isn’t being difficult. Their nervous system is dysregulated. And that’s measurable, addressable, and most importantly, it can heal. Ready to find answers? Visit our directory to find a PX Docs provider near you and schedule an INSiGHT scan. Seeing your child’s nervous system function objectively is the first step toward real, lasting change.