If your child has been diagnosed with Tourette’s Syndrome, or you’re watching them struggle with tics that came out of nowhere, you’re likely feeling confused, overwhelmed, and looking for real answers. You’ve probably been told your child will “grow out of it,” or that medication is the only option, or that there’s simply “no known cause.”
Here’s what most parents don’t hear: Tourette’s Syndrome is a neurological condition, and that means the nervous system is at the center of the story. At PX Docs, we’ve worked with families dealing with tic disorders, and we’ve seen firsthand that when you address the root neurological dysfunction, not just the tics themselves, the whole picture can begin to change.
In this article, we’re going to walk you through everything you need to know about Tourette’s Syndrome, from the basics all the way to a deeper neurological perspective that most doctors never discuss.
What Is Tourette’s Syndrome?
Tourette’s Syndrome (TS) is a neurodevelopmental disorder of the nervous system that causes sudden, involuntary, repetitive movements and vocalizations called tics. It’s classified under the broader category of tic conditions and typically first appears in childhood, most often between the ages of 5 and 10 years.
For a diagnosis of Tourette’s Syndrome, a child must have at least two motor tics and at least one vocal tic that have been present for more than a year, starting before age 18. The tics can’t be explained by another medical condition or substance.
One of the biggest misunderstandings about Tourette’s Syndrome is that it always involves swearing. That specific tic, called coprolalia, actually affects only about 10% of people with TS. Most children experience much more subtle tics that often go unnoticed by others.
TS affects roughly 1 in 160 school-aged children, though many experts believe the true number is higher because mild cases go undiagnosed. It occurs 3 to 4 times more frequently in boys than girls, and it’s important for parents to know that TS is not a degenerative condition; individuals with Tourette’s have a normal life expectancy.
Types of Tics
Tics come in many forms, and understanding the difference helps parents recognize what their child is actually experiencing.
Simple Tics
Simple motor tics are quick, brief movements involving a small number of muscle groups. These include:
- Eye blinking
- Facial grimacing
- Shoulder shrugging
- Head jerking
- Nose twitching.
Simple vocal tics include:
- Throat clearing
- Sniffing
- Grunting
- Coughing
- Barking sounds.
Complex Tics
Complex motor tics involve coordinated patterns using multiple muscle groups. A child might:
- Touch objects repeatedly
- Hop
- Jump
- Twist
- Make movements that look intentional but aren’t.
Complex vocal tics can include:
- Repeating one’s own words (palilalia)
- Echoing what others say (echolalia)
- Or in rarer cases, using socially inappropriate language (coprolalia).
Something many parents aren’t told about is the premonitory urge, a physical sensation or uncomfortable buildup that happens right before a tic. Many kids describe it like needing to sneeze. The tic brings temporary relief, which is why suppressing tics creates intense internal pressure that eventually has to be released.
Tics also tend to follow a predictable pattern over time. They usually begin in the head and face, then may spread to the shoulders, torso, and limbs. The intensity and complexity of tics often peak between ages 10 and 12, then typically lessen through the late teen years. For many people, tics decrease significantly or even resolve by early adulthood.
What Causes Tourette’s Syndrome?
While genetics does play a role in Tourette’s, research confirms that TS runs in families, but that’s not the whole story.
What science has consistently pointed to is dysfunction in the cortico-striatal-thalamo-cortical (CSTC) circuits, the neural pathways connecting the cortex, basal ganglia, and thalamus. The basal ganglia normally function like a filter for the brain, helping suppress unwanted movements while allowing intentional ones. In Tourette’s Syndrome, dopamine signaling within these circuits becomes disrupted, causing the filtering mechanism to break down. The result is involuntary motor and vocal tics that escape through gaps in the brain’s movement control system.
A 2023 study published in Brain provided strong evidence that striatal dopamine dysfunction is a core driver of motor tics in Tourette’s Syndrome, reinforcing the connection between disrupted neurotransmitter signaling and tic production.
But here’s the question that conventional medicine rarely asks: what’s disrupting these brain circuits in the first place?
The CDC has noted that several environmental risk factors may be associated with TS, including smoking during pregnancy, pregnancy complications, low birthweight, and infection. These aren’t just random risk factors; they’re stressors that directly impact the developing nervous system.
The “Perfect Storm”: What’s Really Behind Nervous System Dysfunction
At PX Docs, we recognize that complex nervous system dysfunction doesn’t appear out of nowhere. It’s typically the end result of accumulated stressors during the most vulnerable periods of neurological development. We call this The “Perfect Storm.”
The “Perfect Storm” identifies three core components that set the stage for nervous system dysfunction:
- Prenatal Stress and Maternal Health. When a mother experiences chronic stress, anxiety, or health challenges during pregnancy, elevated cortisol crosses the placenta and impacts the baby’s developing nervous system. Prenatal stress can shift the fetal Autonomic Nervous System toward sympathetic dominance, essentially putting the baby’s system on high alert before they’re even born.
- Birth Trauma and Interventions. The birth process itself, especially when it involves interventions like C-sections, forceps, vacuum extraction, or prolonged labor, can create physical stress on the infant’s upper cervical spine and brainstem. This area sits at the crossroads of motor control, autonomic regulation, and vagus nerve function. When birth trauma affects these structures, it can create subluxation, a combination of misalignment, fixation, and neurological interference that disrupts nervous system communication.
- Early Childhood Stressors. After birth, factors like frequent illness, repeated antibiotics, environmental toxins, and chronic stress continue to pile onto an already strained nervous system. Each stressor pushes the child deeper into a pattern of sympathetic dominance, stuck on the “gas pedal” with a nervous system that can’t slow down, regulate, or adapt properly.
When you view Tourette’s Syndrome through this lens, the connection becomes clear. The basal ganglia are highly sensitive to stress, inflammation, and disrupted neurotransmitter signaling. A nervous system that’s been stuck in overdrive since before birth, dealing with sympathetic dominance, vagus nerve dysfunction, and unresolved subluxation, is far more likely to develop the kind of motor control breakdown that shows up as tics.
Co-Occurring Conditions
If your child has Tourette’s Syndrome, they’re very likely dealing with more than just tics. The CDC reports that most children diagnosed with TS have at least one additional mental, behavioral, or developmental condition. According to StatPearls, ADHD or OCD is often seen.
The most common co-occurring conditions include:
ADHD is the single most frequent co-occurring condition, and for many kids, it causes more daily difficulty than the tics themselves. Attention, focus, and impulse control challenges are often the first things parents and teachers notice.
- Obsessive-Compulsive Disorder (OCD) involves intrusive, unwanted thoughts and repetitive behaviors. The prevalence of OCD ranges from 11-80% of patients with TS, depending on the study and diagnostic criteria used.
- Anxiety conditions are extremely common, partly because living with visible tics brings social stress, bullying, and misunderstanding from peers and adults.
- Sensory processing challenges frequently overlap with tic issues. Children with TS often experience heightened sensitivity to sounds, textures, light, and touch, or they may actively seek intense sensory input.
- Sleep difficulties are prevalent, too. Children with TS tend to take longer to fall asleep, experience lower sleep quality, and have more nighttime awakenings. These sleep struggles often make tics, attention, and emotional regulation worse during the day.
At PX Docs, we don’t see these as separate, unrelated problems that each need their own care. We see them as different expressions of the same underlying nervous system dysregulation. When you address the root neurological dysfunction, improvements often show up across the board, not just in tics, but in focus, sleep, anxiety, and sensory processing simultaneously.
Conventional Care Options for Tourette’s Syndrome
Understanding what conventional medicine offers helps you make informed decisions for your child.
Comprehensive Behavioral Intervention for Tics (CBIT) is considered the first-line care for TS. CBIT teaches children to recognize when a tic is about to happen (the premonitory urge) and perform a competing response instead. It also includes relaxation techniques and environmental modifications. Research shows that CBIT can reduce tic severity and avoid medication side effects entirely.
That said, CBIT has limitations. It works best for children around age 9 and older who can identify their premonitory urges and stay focused on practicing competing responses. Kids with unaddressed ADHD often struggle with the approach. And finding a trained CBIT therapist remains a real barrier for many families.
Medications used for tics include alpha-adrenergic agonists like clonidine and guanfacine, which are often tried first, especially when ADHD is also present. These can reduce tic intensity, but they carry significant side effects, such as weight gain, fatigue, muscle stiffness, cognitive dulling, and social withdrawal. For many families, the side effects prove more disruptive than the tics themselves.
What’s missing from this picture?
Both CBIT and medications focus on managing tics, suppressing symptoms without ever asking why the nervous system is producing them in the first place. They don’t address the underlying neurological dysfunction driving the motor control breakdown.
The Nervous System Connection
Here’s what the research keeps pointing to, even if mainstream medicine hasn’t fully connected the dots: tics are a sign that a nervous system is struggling to regulate itself.
The basal ganglia don’t operate in isolation. They’re deeply connected to the Autonomic Nervous System, which controls heart rate, digestion, sleep, immune function, and stress responses. When the sympathetic “gas pedal” is jammed on and the parasympathetic “brake pedal” can’t engage properly, the fallout extends far beyond tics.
Think about it: a child with Tourette’s isn’t just having trouble controlling their movements. They’re often also struggling to calm down at night, filter sensory input, regulate attention, manage emotions, and fight off illness. These functions are all governed by the same nervous system.
This is where dysautonomia, an imbalance in the autonomic nervous system, becomes critical to the story. Dysautonomia keeps the body locked in a fight-or-flight state. The vagus nerve, the longest cranial nerve in the body and the primary driver of the parasympathetic “rest, digest, and regulate” response, can’t do its job. Motor signals that should be filtered get through as tics. Sensory input that should be screened becomes overwhelming. Stress responses that should turn off stay stuck on.
How INSiGHT Scans Identify the Root Cause
If the nervous system is at the center of this picture, how do you actually see what’s going on beneath the surface?
This is where INSiGHT scanning technology becomes so valuable for families looking for answers. It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for Tourette’s Syndrome or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
INSiGHT Scans measure three key aspects of neurological function:
- Heart Rate Variability (HRV) measures the balance between the sympathetic (“fight-or-flight”) and parasympathetic (“rest, regulate, and digest”) branches of the Autonomic Nervous System. In children with tics, HRV often reveals significant sympathetic dominance, a nervous system running on overdrive with very little capacity to slow down and regulate.
- Surface Electromyography (sEMG) assesses the electrical activity of muscles along the spine, identifying areas of tension and altered neuromuscular function. In children with tics, this often shows excessive neuromotor tension, especially in the upper cervical and brainstem regions, which are central to motor regulation.
- Thermal Scanning uses infrared sensors to measure temperature differences along the spine, indicating areas of dysautonomia. Temperature asymmetry points to specific regions where the autonomic nervous system is out of balance.
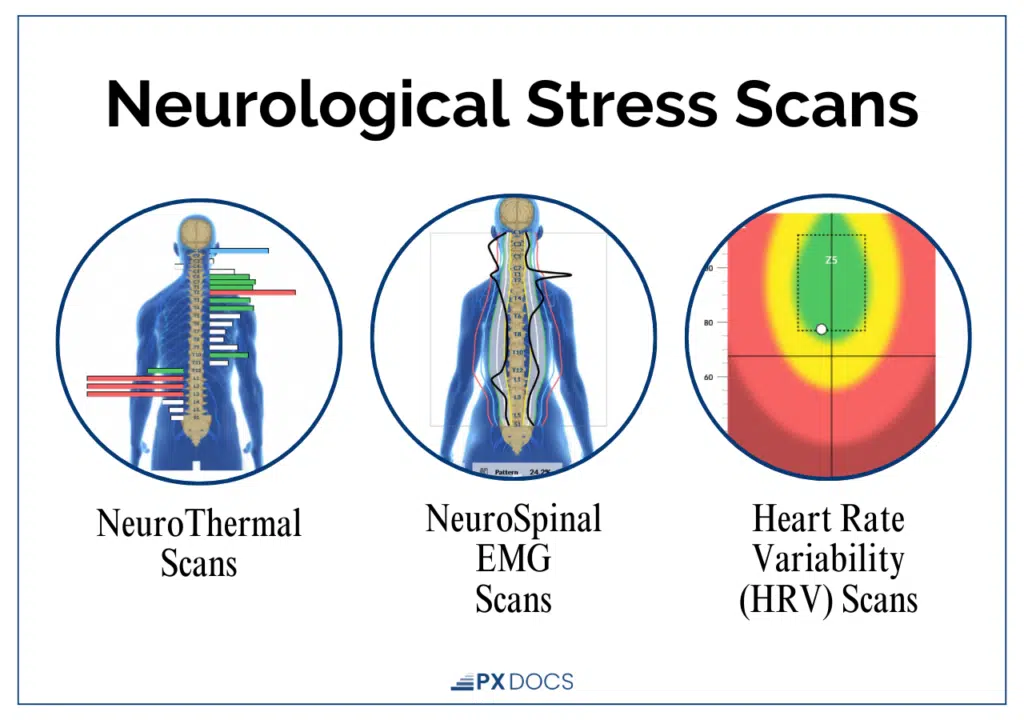
What makes these scans powerful is their ability to detect shifts in neurological function that aren’t visible from the outside. They provide a clear map of where the nervous system is stuck, stressed, and struggling, and give us a roadmap for care.
Neurologically-Focused Chiropractic Care and Tourette’s Syndrome
Neurologically-Focused Chiropractic Care takes a fundamentally different approach than medication or behavioral therapy alone. Instead of trying to suppress tics or train around them, it’s more effective to restore proper function to the nervous system itself, addressing the subluxation, sympathetic dominance, and vagus nerve dysfunction that contribute to the breakdown of motor control.
Gentle, specific chiropractic adjustments target areas of subluxation along the neurospinal system, especially the upper cervical region and brainstem, areas critical for motor regulation, autonomic balance, and vagus nerve function. The goal isn’t to “cure” or “treat” Tourette’s Syndrome. It’s to remove neurological interference so the nervous system can begin to self-regulate the way it was designed to.
As the nervous system shifts out of sympathetic overdrive and toward a more balanced state, families commonly report improvements that extend well beyond tics. Sleep gets better. Anxiety calms down. Focus and attention improve. Sensory sensitivities ease up. Emotional dysregulation starts to stabilize. This makes sense when you understand that these aren’t separate problems; they’re all connected to the same dysregulated nervous system.
Families should also understand that healing takes time. The nervous system didn’t get stuck overnight, and it won’t fully reorganize overnight. Progress often appears first on INSiGHT scans before it’s visible in daily life. This inside-out healing pattern, where neurological function improves before symptoms fully resolve, is a hallmark of Neurologically-Focused Chiropractic Care.
Taking the Next Step for Your Child
Tourette’s Syndrome doesn’t have to define your child’s life. While there’s no overnight fix, understanding the neurological root causes, the subluxation, the sympathetic dominance, and the vagus nerve dysfunction opens up a path forward that conventional medicine alone doesn’t offer.
The nervous system has an extraordinary capacity to heal, adapt, and reorganize when the interference is removed and the right support is in place. That’s exactly what Neurologically-Focused Chiropractic Care is designed to do. We always encourage parents to work alongside their child’s pediatrician or neurologist as part of a comprehensive care team. And if you’d like to explore whether a neurological approach could help your child, visit the PX Docs Directory to find a trained Neurologically-Focused Chiropractor near you.