It’s a known fact that teens are struggling, and the signs are no longer subtle. Social situations that were once manageable now lead to shutdowns. Anxiety has intensified beyond typical teenage stress. Sensory sensitivities interfere with daily life. Rigid thinking patterns cause meltdowns when routines change.
Many parents have raised these concerns with pediatricians and were told that development varies or that more time was needed. Now, in middle or high school, the challenges are unmistakable. The difficulties affect school, relationships, and emotional regulation, and they cannot be explained away as normal adolescence.
Autism doesn’t suddenly begin in the teen years. Those neurological differences have likely always been there. What often changes is the environment—when academic, social, and emotional demands increase, the strategies your teen once used to cope may no longer feel like enough.
What Is Autism Spectrum Disorder?
Autism Spectrum Disorder (ASD) is a neurodevelopmental condition characterized by differences in social communication, interaction patterns, and behavioral responses. According to the CDC, approximately 1 in 31 children is diagnosed with Autism, with rates continuing to rise. While boys are diagnosed roughly four times more often than girls, this gap is narrowing as we recognize that girls often mask their signs more effectively.
The Four Core Areas
When psychologists evaluate for Autism, they’re looking at challenges across four domains:
- Social Communication: Teens with Autism often struggle with conversation flow, interpret language literally, and miss sarcasm or implied meanings.
- Social Interaction: Reading social cues feels like learning a second language. They might have trouble with eye contact, facial expressions, or understanding the unspoken rules of peer relationships.
- Restricted Interests and Repetitive Behaviors: Intense, focused interests that interfere with other activities. Repetitive behaviors like stimming (hand-flapping, rocking), strict routines, or distress when plans change.
- Sensory Processing Differences: This is where Autism often “begins in the body.” Fluorescent lights might feel painfully bright. Cafeteria noise might be overwhelming chaos. Some teens seek intense sensory input while others avoid specific sensations.
Beyond the Behavioral Checklist
Here’s what conventional diagnostic criteria often miss: the physical signs that point to underlying nervous system dysfunction.
Teens with Autism consistently present with patterns that behavioral checklists don’t ask about:
- Chronic digestive issues (research shows up to 70% of children with Autism experience gut problems)
- Sleep disturbances that have persisted since infancy
- Immune dysregulation, frequent illness despite “normal” lab work
- Motor coordination challenges
- Temperature regulation issues
These aren’t separate problems. They’re all manifestations of the same nervous system dysfunction that drives the social and behavioral challenges.
Why Are Some Teens Diagnosed Late?
If your teen is being evaluated at 13, 15, or 17, you’ve probably asked: How did we miss this?
The truth is, Autism didn’t suddenly appear. The neurological patterns were likely present all along—but your teen may have been working incredibly hard to keep up. As the demands of adolescence increase, it can simply become harder to compensate the way they once did.
The Masking Phenomenon
Many teens, especially girls, successfully hide their Autism signs through intense effort. This is called “masking,” and it’s exhausting work.
They watch other kids and copy their behaviors. They memorize social scripts. They force eye contact. They suppress stimming in public. They spend enormous energy trying to blend in.
This works through elementary school when social rules are simpler. But middle school hits with complex social hierarchies, increased academic expectations, and constant transitions. High school adds pressure to develop independence and navigate relationships.
Suddenly, the nervous system that was barely compensating can’t keep up.
Neurologically, Here’s What’s Happening
Masking requires constant activation of the Sympathetic Nervous System. Your teen is running their stress response at full throttle all day, every day.
Think of the Sympathetic Nervous System as your car’s gas pedal and the parasympathetic as the brake. In teens with Autism and Dysautonomia, the gas pedal is stuck down, and the brake barely works. They’re revving at high RPMs constantly, which exhausts their system and makes everything—sensory processing, emotional regulation, social interaction—harder than it should be.
What appears as “signs suddenly appearing” is actually a nervous system exhausted from years of compensating, finally unable to maintain the masking behaviors.
Published research shows that girls with Autism are diagnosed an average of 18 months later than boys. Girls are more skilled at social mimicry; their restricted interests often center on socially acceptable topics, they internalize struggles through anxiety rather than externalizing through meltdowns, and they face more intense social expectations, making the eventual collapse more dramatic.
Looking Back: Signs That Were Missed
When teens are diagnosed with Autism in adolescence, parents often recognize early warning signs that were dismissed:
- Infant colic and sleep problems were early Dysautonomia
- Chronic ear infections signaled immune dysregulation
- Sensory sensitivities dismissed as “preferences”
- Delayed motor milestones indicated cerebellar dysfunction
- “Sensitive” or “shy” labels masked nervous system overwhelm
Pediatricians often said, “They’ll grow out of it.” Your instincts were right; the nervous system was already struggling.
The Professional Autism Evaluation Process
A professional autism evaluation involves multiple appointments over several weeks. The process includes:
- Initial Consultation: An extensive 2-3 hour interview about developmental history from pregnancy through current day—prenatal/birth history, early milestones, medical history, school performance, and current functioning.
- Autism Diagnostic Observation Schedule (ADOS-2): A 45-60 minute semi-structured assessment where the evaluator observes your teen in specific activities designed to reveal social communication patterns and behaviors.
- Autism Diagnostic Interview-Revised (ADI-R): A 2-3 hour structured parent interview focusing on language development, social interactions, and repetitive behaviors—both currently and at ages 4-5 to establish early patterns.
- Additional Assessments: May include cognitive testing, adaptive functioning scales, and screening for anxiety, depression, or ADHD.
After 4-8 weeks, you’ll receive a comprehensive report documenting whether your teen meets DSM-5 criteria for Autism Spectrum Disorder, the level of support recommended, and specific recommendations.
What These Tests Can’t Measure
Here’s the critical limitation: these assessments excel at documenting observable behavioral patterns, but they can’t measure the neurological basis that actually causes and contributes to those patterns.
The ADOS-2 can tell you that your teen makes eye contact 40% less than typical peers. The ADI-R documents restricted interests since age 4.
What these tests don’t assess:
- Autonomic Nervous System balance
- Vagus nerve function
- Subluxation patterns
- Nervous system adaptability
Professional autism testing provides detailed descriptions of the signs. But it doesn’t explain why those signs exist at the neurological level. It’s like a mechanic documenting everything wrong with your car without ever looking under the hood to see what’s causing those problems.
The Nervous System Connection: Beyond Behavioral Signs
Conventional Autism evaluations are thorough in cataloging observable behaviors. What they typically miss is why these patterns exist at the neurological level.
Understanding Subluxation
What most autism evaluations miss is the role of subluxation, a neurological interference that disrupts how the nervous system functions, regulates, and adapts. Subluxation isn’t about bones being “out of place.” It’s about the nervous system being stuck in dysfunctional patterns that prevent proper communication between the brain and body.
Think of subluxation like static on a phone line. The wires are connected, but the signal gets distorted. Your teen’s brain might be sending messages about emotional regulation, sensory processing, or social connection, but those messages don’t arrive clearly because of neurological interference.
Dysautonomia: The Core Imbalance
At the heart of Autism’s neurological pattern is Dysautonomia—an imbalance in the Autonomic Nervous System. The Autonomic Nervous System controls everything you don’t consciously think about: heart rate, digestion, immune function, sleep-wake cycles, stress responses.
In teens with Autism, the sympathetic branch (fight-or-flight) is overactive while the parasympathetic branch (rest-regulate-digest) is underactive. This keeps the body in constant stress, which explains why your teen might struggle with sleep, have digestive issues, get sick frequently, and have difficulty calming down.
Dysautonomia explains the physical signs that behavioral checklists often overlook: chronic constipation or diarrhea, sleep problems, frequent illness, temperature regulation issues, difficulty transitioning between activities, and sensory overload.
This is why behavioral interventions alone often fall short. You can teach social skills, but if your teen’s nervous system is stuck in survival mode, they can’t access those skills when stressed. Nervous system dysfunction must be addressed first.
The “Perfect Storm”: How Early Life Stress Impacts Teen Development
Autism doesn’t begin in adolescence; it builds over time through what we call the “Perfect Storm.” This describes the accumulation of neurological stress that happens when multiple stressors hit the developing nervous system during critical periods.
Preconception/Prenatal/Birth (Foundation)
Preconception stress, pregnancy stress, birth interventions (C-section, forceps, vacuum, induction, etc.) create the first layer of nervous system dysfunction. Physical trauma to the infant’s upper cervical spine and brainstem during delivery is particularly significant.
Early Childhood (Accumulation)
Repeated antibiotic courses, exposure to toxins, emotional stress, etc.
This stress accumulates and often shows up early as chronic ear infections, gut issues, sleep problems, developmental delays—these aren’t separate problems, they’re signs the nervous system is overwhelmed.
The vagus nerve is the major communication highway between the brain and the digestive system. When subluxation affects the upper cervical spine where the vagus nerve originates, it disrupts this gut-brain connection. This explains why 70% of children with Autism experience chronic digestive issues.
Teen Breaking Point (Manifestation)
Increased social demands, academic pressure, hormonal changes, and expectations of independence push an already stressed nervous system past its breaking point.
This explains why you might have told doctors “something’s wrong” when your child was 2 or 5, but they said “wait and see.” Your instincts were right; the nervous system was already struggling.
INSiGHT Scans: Objective Nervous System Assessment
While behavioral checklists rely on subjective observations, INSiGHT scans provide objective measurements of what’s happening inside the nervous system. These aren’t diagnostic tools for Autism, but they reveal the neurological patterns that contribute to Autism-related challenges.
INSiGHT scans measure three critical aspects:
- Heart Rate Variability (HRV) measures the balance between your Sympathetic Nervous System (the “gas pedal”) and Parasympathetic Nervous System (the “brake pedal”). In teens with Autism, we typically see sympathetic dominance—the gas pedal is stuck down with minimal braking ability.
- Surface EMG (sEMG) assesses electrical activity of the neuromuscular system, identifying areas of excessive tension where the nervous system is working overtime to compensate for dysfunction.
- Thermal Scanning measures temperature differences along the neurospinal system, indicating areas of Dysautonomia—imbalances in the autonomic nervous system.
Teens with Autism typically show significant sympathetic dominance with excessive, disorganized energy stuck in the nervous system. We often see significant dysfunction in the lower thoracic and lumbar regions, which correlates with the gut-immune challenges common in Autism.
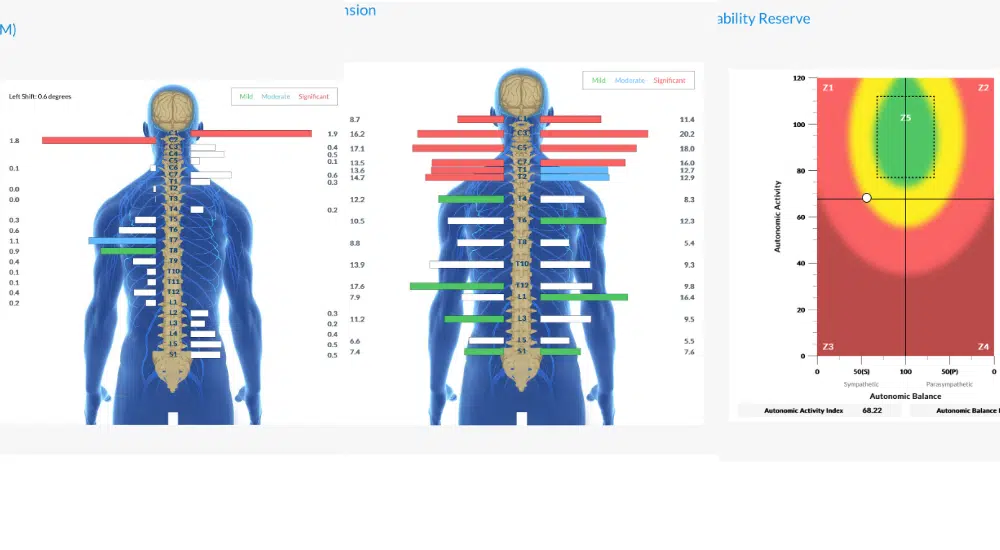
Imagine going to the doctor for chest pain, and they ask, “On a scale of 1-10, how bad is your pain?” versus doing an EKG to see exactly what your heart is doing. That’s the difference between behavioral checklists and INSiGHT scans.
Neurologically-Focused Chiropractic Care for Teens with Autism
Neurologically-Focused Chiropractic Care isn’t about replacing other Autism therapies—it’s about addressing the foundational nervous system dysfunction that affects how well those therapies work.
When your teen’s nervous system is stuck in sympathetic dominance with chronic Dysautonomia, even the best behavioral therapy has limited effectiveness. By reducing subluxation and restoring autonomic balance, Neurologically-Focused Chiropractic Care creates the neurological foundation that allows other interventions to work more effectively, if needed.
A comprehensive support team might include speech therapy, occupational therapy, Applied Behavior Analysis, educational supports, nutritional interventions, and Neurologically-Focused Chiropractic Care. Chiropractic care addresses the control system—the nervous system—that coordinates all other systems.
Important: Neurologically-Focused Chiropractic Care doesn’t diagnose or treat Autism. Chiropractors assess and address subluxation and nervous system dysfunction—the neurological interference that may contribute to Autism-related challenges. A formal diagnosis comes from psychologists or developmental pediatricians. PX Docs providers work collaboratively with these professionals.
Take Rhiannon, for example:
Rhiannon’s challenges began early, with diagnoses including sensory and auditory processing disorders, food allergies, seizure risk, and, eventually, an autism diagnosis. Her mom recalls those years as overwhelming and disorienting, as development regressed and daily life felt turned upside down.
But after finding neurologically focused care and seeing clear changes in her nervous system function, everything began to shift. Today, Rhiannon is thriving as a teenager—graduating with academic honors, working five days a week, and competing as a multi-time World Champion rider—an incredible testament to how far she’s come.
Next Steps: Finding Support for Your Teen
If your teen is struggling with Autism symptoms, understanding the neurological foundation opens doors to addressing root causes rather than just managing the signs.
The conventional path after diagnosis often involves behavioral therapy, psychiatric medications, and school accommodations. These interventions can provide relief and teach valuable skills. But they don’t address the upstream neurological dysfunction, the subluxation, and Dysautonomia that created the signs in the first place.
You’re not choosing between chiropractic care and other therapies. You’re adding a foundational piece that helps everything else work better.Visit the PX Docs Directory to find a qualified practitioner in your area who specializes in working with teens and understands the neurological complexities of Autism.