Feeding therapy for kids is a specialized intervention provided by speech-language pathologists or occupational therapists to help children who struggle with eating, drinking, or accepting a variety of foods due to sensory, oral-motor, behavioral, or neurological barriers. It uses individualized strategies, including sensory desensitization, oral-motor exercises, and play-based food exposure to expand a child’s diet safely.
If mealtimes have become a battleground, food refusals, gagging, meltdowns, and a child who’ll only eat a handful of “safe” foods, you’re not alone. Feeding difficulties affect an estimated 25–45% of typically developing children and up to 80% of children with developmental delays. For many families, feeding therapy becomes the next step, and it can genuinely help.
But here’s what most families never hear: the sensory aversions, oral-motor struggles, gut discomfort, and anxiety around new foods aren’t just habits. In many cases, they’re signs of a dysregulated nervous system. Until that underlying imbalance is addressed, even the best feeding therapy can feel like pushing water uphill.
What Is Feeding Therapy?
Feeding therapy is a specialized intervention for children who struggle with eating, drinking, or accepting a variety of foods. It’s typically provided by speech-language pathologists (SLPs) or occupational therapists (OTs) with additional feeding and swallowing training.
The goal isn’t to force a child to eat. It’s to identify the specific barriers, sensory, oral-motor, behavioral, or some combination, and address them systematically. A feeding therapist will assess:
- Oral-motor skills (how well the tongue, lips, and jaw coordinate for chewing and swallowing)
- Sensory processing (responses to taste, texture, temperature)
- Swallowing safety
- Mealtime behaviors.
Sessions may include oral-motor exercises, sensory desensitization, play-based food exposure, and parent coaching. Care plans are highly individualized.
Signs Your Child Might Benefit from Feeding Therapy
Not every picky eater needs feeding therapy. But there’s a meaningful difference between a child who prefers mac and cheese over broccoli and a child who’s genuinely struggling. Signs a feeding evaluation may be warranted include:
- Difficulty latching, slow weight gain, or excessive feeding time in infancy
- Gagging, coughing, or choking during feedings
- Eating fewer than 20 foods, or refusing entire food groups
- Extreme sensitivity to textures, smells, or the appearance of food
- Gagging or vomiting at the sight or smell of non-preferred foods
- Meltdowns or high anxiety around mealtimes
- Refusing to sit at the table or be near foods they don’t eat
- Eating only very specific brands or presentations of preferred foods
If these struggles are affecting your child’s nutrition, growth, or family life, pursue a professional evaluation sooner rather than later.
What Causes Feeding Difficulties in Children?
Feeding difficulties in children are caused by multiple overlapping factors, including sensory processing differences, oral-motor dysfunction, gastrointestinal issues, and neurological conditions like Autism and ADHD. In many cases, these causes share a common root: Autonomic Nervous System dysfunction that disrupts the neurological foundation needed for safe, comfortable eating.
- Sensory Processing Differences: The mouth is one of the most sensory-rich areas of the body. Eating involves simultaneous input from taste, texture, temperature, smell, and proprioception. For children with sensory processing differences, this flood of information triggers defensive responses, gagging, refusal, and distress. Research consistently shows that children with Sensory Processing Disorder are significantly more likely to experience feeding difficulties, and feeding problems are often among the earliest observable signs that a child’s sensory system is dysregulated.
- Oral-Motor Dysfunction: Eating requires remarkably complex motor coordination. When oral-motor development is delayed or disrupted, due to low muscle tone, poor coordination, or structural issues, chewing and swallowing become genuinely hard work. Children may tire quickly during meals, pocket food in their cheeks, or only tolerate soft textures.
- Gastrointestinal Issues: Feeding is no fun when eating hurts. GERD, chronic constipation, gut motility problems, and food sensitivities can all make eating uncomfortable. Studies show that children with GERD are more likely to struggle with feeding difficulties, yet it’s frequently underdiagnosed in this population.
- Behavioral, Anxiety, and Neurological Factors: For some children, feeding difficulties are primarily driven by anxiety, ARFID, fear of choking, or conditioned aversion following a traumatic experience. Children with Autism Spectrum Disorder, ADHD, and other neurological differences experience feeding difficulties at much higher rates than the general population, often reflecting the same underlying nervous system dysregulation driving their other challenges.
Children with feeding difficulties frequently also experience Sensory Processing Disorder, emotional dysregulation, sleep disturbances, and chronic digestive issues like constipation or reflux. This co-occurrence isn’t coincidental; these conditions share a common neurological root in dysautonomia, an imbalance within the Autonomic Nervous System where the sympathetic “fight or flight” response is overactivated and the parasympathetic “rest, digest, and regulate” response, driven primarily by the vagus nerve, can’t keep up.
How Long Does Feeding Therapy Take?
There’s no universal timeline. Some children with mild sensory-based picky eating make significant progress in three to six months of weekly sessions. Children with more complex profiles, tube dependency, anxiety, or underlying neurological conditions may need a year or more. One thing is consistent across the research: early intervention produces better outcomes. The longer feeding difficulties persist, the more entrenched the patterns become.
What Is the Root Cause of Feeding Difficulties That Most Providers Miss?
The root cause most feeding therapy providers miss is nervous system dysregulation—specifically, an imbalance in the Autonomic Nervous System that keeps a child locked in a sympathetic “fight or flight” state. When the nervous system can’t shift into parasympathetic mode, sensory processing, swallowing coordination, gut motility, and emotional regulation around food are all compromised simultaneously.
Here’s the conversation that rarely happens in a feeding therapy office, but should.
Feeding difficulties, whether they show up as sensory aversions, oral-motor dysfunction, GI issues, or anxiety, are almost always downstream effects of how a child’s nervous system is functioning. The feeding difficulty is the symptom. Nervous system dysregulation is the root cause.
Think of it like a gas pedal and a brake pedal. The Sympathetic Nervous System (fight-or-flight) is the gas pedal; it heightens sensory sensitivity and shuts down digestion. The Parasympathetic Nervous System (rest-and-digest) is the brake pedal; it calms the body and creates the safety needed to tolerate new sensory experiences. For many children who struggle with feeding, the gas pedal is chronically stuck. They’re trying to eat in a state of fight-or-flight.
Sensory exposure exercises and oral-motor drills can only do so much when the nervous system is too dysregulated to integrate new experiences.
The Vagus Nerve Connection
The vagus nerve runs from the brainstem through the neck, throat, chest, and abdomen. It’s the primary highway of the Parasympathetic Nervous System and controls nearly every function involved in feeding:
- Swallowing
- Gag reflex sensitivity
- Esophageal motility
- Gastric emptying
- Gut function.
When vagal tone is low and brainstem communication is disrupted, all of those functions are compromised; the child gags more easily, food moves through the gut poorly, and sensory sensitivity is amplified. Research links low vagal tone to increased sensory sensitivity, emotional dysregulation, and GI dysfunction, all hallmarks of children who struggle most with feeding.
How the “Perfect Storm” Sets the Stage
At PX Docs, we use a framework called the “Perfect Storm” to explain how neurological dysregulation develops long before a child’s feeding difficulties ever become obvious. It unfolds in three stages.
- Stage 1—Early Neurological Stress (Before Birth): The story often starts in the womb. Prenatal stress, maternal health challenges, and difficult birth experiences—C-sections, vacuum extraction, forceps, prolonged labor, cord complications—create neurological stress at the most critical window of development. The vagus nerve and the Autonomic Nervous System are especially vulnerable during this period. Many children enter the world with their nervous system already tilted toward sympathetic dominance before they’ve taken their first breath.
- Stage 2—Toxic Load and Early Childhood Stressors: Once born, today’s environment piles on more strain. Frequent antibiotic use, reflux medications, gut dysbiosis, chronic ear infections, formula feeding challenges, and environmental toxins all burden a developing neuro-immune system. These stressors show up early—as colic, reflux, constipation, poor sleep, and sensory overload—and they’re often the same children who later struggle with feeding.
- Stage 3—Disrupted Sensory-Motor Development: As these stressors stack up, the neurological foundation required for eating doesn’t develop the way it’s designed to. Vagus nerve dysfunction impairs swallowing and gut motility. Sensory processing becomes dysregulated. Oral-motor coordination lags. The child who won’t tolerate textures, gags at smells, or melts down at the sight of a new food isn’t being difficult; their nervous system simply doesn’t have the regulatory capacity to handle the experience safely.
By the time a parent is worried about food refusal at 18 months, the neurological stage has often been set for years. Feeding therapy addresses the downstream effects. The question PX Docs practitioners ask is: what’s happening upstream, in the nervous system, that’s making feeding so hard?
How Does Subluxation Contribute to Feeding Difficulties?
Subluxation is a pattern of neurological dysfunction in the spine characterized by three components: misalignment within the neurospinal system, fixation or restricted joint motion, and neurological interference that disrupts communication between the brain and body. When subluxation occurs in the upper cervical spine near the brainstem and the origin of the vagus nerve, it can directly impair the neurological functions required for safe, comfortable eating.
The atlas (C1) and axis (C2) vertebrae sit in direct proximity to the brainstem and the origin of the vagus nerve. When subluxation is present, it can lead to vagus nerve dysfunction, disrupt sensory pathways regulating oral sensitivity and gag reflex thresholds, and keep the nervous system locked in a state of sympathetic dominance.
Upper cervical subluxation in infants and toddlers often develops during difficult deliveries, the same birth experiences described in the “Perfect Storm.” A Neurologically-Focused Chiropractor evaluates for subluxation and works to correct it, reducing neurological interference and supporting the nervous system’s capacity to regulate.
How Neurologically-Focused Chiropractic Care Supports Children with Feeding Difficulties
It’s important to note that Neurologically-Focused Chiropractic Care is not a treatment or cure for feeding difficulties or any other condition, including back pain. Instead, our approach uses INSiGHT scanning technology and specific chiropractic adjustments to identify the root cause of nervous system dysfunction and dysregulation, and to build customized care plans that help shift the nervous system back into a state of balance, regulation, and resilience.
When a child with feeding difficulties comes to a PX Docs practice, the process starts with objective assessment, not guesswork. PX Docs practitioners use the INSiGHT scanning system, a non-invasive, FDA-registered technology that measures three key markers of nervous system function:
- Heart Rate Variability (HRV) to assess sympathetic/parasympathetic balance
- Surface electromyography (sEMG) to map neurological output along the spine
- Thermal scanning to detect autonomic dysfunction patterns.
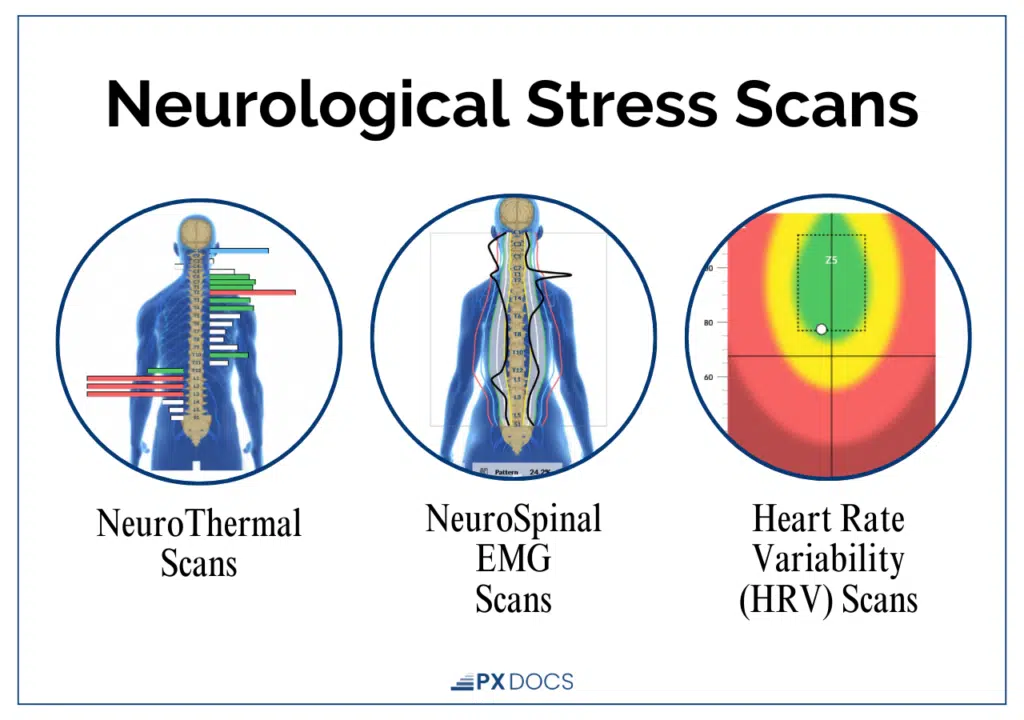
It’s important to note that INSiGHT scanning does not diagnose feeding difficulties or any medical condition.
When subluxation and neurological interference are identified, PX Docs practitioners use gentle, specific pediatric adjustments to correct them, very light, targeted pressure appropriate for a child’s developing spine. The goal is to reduce neurological interference and support the nervous system’s shift from sympathetic dominance toward parasympathetic balance, so the brake pedal works the way it’s supposed to. When the nervous system is better regulated, the gag reflex is often less reactive, gut motility improves, and sensory processing integrates more effectively.
Can Feeding Therapy and Neurologically-Focused Chiropractic Care Work Together?
The best outcomes for children with feeding difficulties typically come from a team approach where feeding therapy and Neurologically-Focused Chiropractic Care address different layers of the same problem. Feeding therapy provides direct skill-building, sensory desensitization, and behavioral support, while NFCC addresses the upstream nervous system dysregulation that makes feeding therapy harder than it needs to be.
When the nervous system is better regulated, the brain can learn more effectively. Sensory processing integrates more easily. The gag reflex is less reactive. Families who pursue both often find that progress that had stalled begins moving again.
Start early. Infants who show early feeding struggles, difficulty latching, slow weight gain, colic, or excessive spitting up are ideal candidates for neurological assessment. These are often the first visible signs of the nervous system dysregulation described in the “Perfect Storm.” Waiting to see if a child “grows out of it” is one of the most common decisions parents later regret.
How Do You Find the Right Feeding Support for Your Child?
If your child is struggling with feeding, build a team: start with a feeding evaluation from a speech-language pathologist or OT with specialized feeding training, make sure the medical team has ruled out GI contributors like reflux or constipation, and have your child’s nervous system assessed by a Neurologically-Focused Chiropractor trained in pediatric care. Be sure to ask specifically about INSiGHT scanning. Then share information between providers. A feeding therapist who understands nervous system work and a chiropractor who understands the feeding therapy goals can coordinate for far better outcomes.
Your child deserves a team that’s looking at the whole picture, not just the end of the fork.
Next Steps
Feeding difficulties are real, they’re stressful, and they deserve serious attention. Feeding therapy is a valuable, evidence-based intervention that helps thousands of children expand their diets and develop safer relationships with food.
But it works best when the nervous system is capable of learning and integrating new experiences. For many children, that means addressing the upstream factors, subluxation, vagal dysfunction, and sympathetic dominance that are making feeding hard in the first place.
If your child is struggling with feeding, don’t wait. Get the feeding evaluation. Pursue the therapy. And find out whether their nervous system needs support to make the most of every session. To find a PX Docs practitioner near you, visit the PX Docs directory.
Frequently Asked Questions About Feeding Therapy for Kids
At what age should a child start feeding therapy?
Children can begin feeding therapy as early as infancy if they show signs such as difficulty latching, slow weight gain, or excessive gagging during feedings. There’s no minimum age requirement, and early intervention consistently produces better outcomes. The longer feeding patterns become entrenched, the harder they are to change, so pursuing an evaluation at the first sign of concern is recommended.
Is feeding therapy covered by insurance?
Many insurance plans cover feeding therapy when it’s deemed medically necessary, particularly when provided by a speech-language pathologist or occupational therapist with a physician’s referral. Coverage varies by plan, diagnosis code, and state. Contact your insurance provider directly and ask specifically about coverage for pediatric feeding therapy or dysphagia care.
What’s the difference between picky eating and a feeding disorder?
Picky eating is a normal developmental phase in which a child develops food preferences but still eats a variety of foods for adequate nutrition. A feeding disorder involves persistent difficulty eating that affects nutrition, growth, or daily functioning—such as eating fewer than 20 foods, gagging at the sight or smell of non-preferred foods, or extreme anxiety around mealtimes that disrupts family life.
Can feeding difficulties be a sign of nervous system dysregulation?
Yes. Feeding requires coordination between sensory processing, oral-motor function, gut motility, and emotional regulation—all governed by the Autonomic Nervous System. When the nervous system is stuck in a sympathetic dominant “fight or flight” state, children experience heightened gag reflexes, sensory defensiveness, poor gut motility, and increased anxiety around food. These are neurological signs, not behavioral choices.
How does chiropractic care help children with feeding problems?
Neurologically-Focused Chiropractic Care addresses subluxation—misalignment, fixation, and neurological interference—that can disrupt vagus nerve function and Autonomic Nervous System balance. By reducing this interference through gentle, specific pediatric adjustments, the nervous system can shift toward better parasympathetic regulation, supporting improved sensory processing, swallowing coordination, and gut function. It’s not a treatment for feeding difficulties, but rather an approach to supporting the nervous system function that makes feeding possible.
Does feeding therapy work for children with Autism or ADHD?
Feeding therapy can be effective for children with Autism and ADHD, though progress may be slower due to the underlying neurological differences these children experience. Research shows that children with Autism Spectrum Disorder and ADHD experience feeding difficulties at significantly higher rates than the general population. A combined approach that includes feeding therapy alongside nervous system support often produces better results than feeding therapy alone.
What should I look for in a feeding therapist?
Look for a speech-language pathologist or occupational therapist with specialized training in pediatric feeding and swallowing—not all SLPs or OTs have this expertise. Ask about their approach (SOS Approach to Feeding and responsive feeding methods are well-regarded), their experience with your child’s specific challenges, and whether they coordinate with other providers. A feeding therapist willing to communicate with your child’s chiropractor and other health providers will give you the best team-based outcomes.