Profound Autism is a classification used to describe children on the most significantly affected end of the Autism spectrum—those with an IQ below 50 or who are nonverbal or minimally verbal, requiring round-the-clock support for daily living throughout their lifetime. It affects roughly 1 in 4 children with Autism, and these children face challenges that go far beyond what most people picture when they hear the word “Autism.”
If you’re a parent reading this, you already know the weight of that reality—the sleepless nights, the safety concerns, the meltdowns that aren’t tantrums but genuine neurological overwhelm. You’ve probably noticed that much of the Autism conversation today doesn’t apply to your child’s experience.
We’re going to walk through what profound Autism really looks like, what the latest research tells us about why it happens, and what options exist beyond the conventional approaches that may have left you stuck. At PX Docs, we believe understanding the neurological root causes behind profound Autism opens doors that many parents don’t know exist.
What Is Profound Autism?
Profound Autism is a proposed classification, not yet an official diagnosis in the DSM-5, that describes children and adults on the Autism spectrum with the most significant support needs. The term was formally endorsed by a 2021 Lancet Commission on the Future of Care and Research in Autism, and gained major traction when the CDC released its first-ever prevalence data on the category in 2023.
To meet the criteria for profound Autism, a child must have an IQ below 50 and/or be nonverbal or minimally verbal. But these clinical criteria only scratch the surface. Children with profound Autism typically need help with every basic activity of daily living—dressing, bathing, eating, and using the bathroom. They often can’t be left unsupervised for even a few minutes due to safety risks, including self-injurious behaviors, elopement (wandering), and seizures.
The 2021 Lancet Commission made the case that lumping these children into the same “Autism spectrum disorder” category as someone who lives independently does a disservice to everyone. When all Autism is discussed as one condition, children with the most severe needs get overlooked in research, policy, and resource allocation.
It’s not about creating a hierarchy. It’s about ensuring that children who need 24/7 care actually receive it, and that the research community stops treating them as invisible.
How Common Is Profound Autism?
The landmark 2023 CDC study published in Public Health Reports analyzed data from over 20,000 eight-year-old children with Autism across 15 U.S. sites. The findings: 26.7% of children with Autism met the criteria for profound Autism—roughly 1 in 4 children on the spectrum, or about 4.6 per 1,000 eight-year-olds.
The data revealed that profound Autism was more common among girls than boys, more common among Black children, and more common in lower socioeconomic families. Children born preterm or with low birth weight were also more likely to be affected. These patterns raise important questions about the role that prenatal stress, birth complications, and environmental factors play in the most severe forms of Autism.
Notably, while overall Autism prevalence nearly tripled between 2000 and 2016, most of that increase came from milder cases.
What Are the Signs and Symptoms of Profound Autism?
The signs of profound Autism are more intense and pervasive than what many parents associate with Autism Spectrum Disorder. Here’s what families typically observe:
- Communication challenges are often the most immediately apparent feature. Many children with profound Autism are completely nonverbal. Others may have a handful of words or sounds but can’t use them functionally to communicate needs or thoughts. Some rely on gestures, picture boards, or augmentative and alternative communication (AAC) devices, though even these tools can be challenging to implement.
- Significant intellectual disability is present in most cases. By definition, children with profound Autism have an IQ below 50, reflecting major differences in how they process information and learn new skills. This doesn’t mean they aren’t capable of growth—it means they need radically different approaches.
- Self-injurious behaviors like head-banging, biting, scratching, or hitting themselves are heartbreakingly common. These aren’t willful acts of defiance; they’re often the only way an overwhelmed nervous system can express distress when verbal communication isn’t available.
- Severe sensory sensitivities are almost universal. A child with profound Autism may be hypersensitive to sounds, lights, textures, or smells, or undersensitive and seeking intense input through rocking, spinning, or mouthing objects. These reflect how the nervous system processes (or fails to process) sensory information.
- Seizures and epilepsy co-occur at high rates. A 2017 review found that epilepsy is significantly more common in children with profound Autism than in those with milder forms. This comorbidity adds another layer of medical complexity and safety concern for families.
- Daily living dependency means these children need hands-on help with virtually everything, eating, toileting, dressing, and bathing. Structured routines become essential, and even small changes to those routines can trigger severe distress.
- Aggressive behaviors like hitting, kicking, and throwing objects often emerge not from anger but from frustration when a child can’t communicate or when sensory overload becomes unbearable.
Children with profound Autism frequently also experience Sensory Processing Disorder, epilepsy, chronic digestive issues, and emotional dysregulation. These conditions share a common neurological root in Autonomic Nervous System dysfunction and vagus nerve impairment, which disrupts the body’s ability to simultaneously regulate sensory input, immune response, digestion, and emotional state.
What Causes Profound Autism?
This is the question every parent wants answered. The standard response is usually some version of “it’s probably genetic.” While genetics can play a role, that explanation leaves out critical pieces of the puzzle.
Research has identified over 100 genes associated with Autism risk, many of which involve brain development and neural connectivity. But having a genetic predisposition doesn’t mean a child will inevitably develop profound Autism. Genes load the gun, but the environment pulls the trigger.
A comprehensive meta-analysis examining over 60 perinatal and neonatal factors found that several birth-related complications, including abnormal fetal presentation, umbilical cord complications, fetal distress, birth injury or trauma, and low Apgar scores, were associated with increased Autism risk. This is significant because these aren’t random genetic events. They’re environmental stressors that directly impact the developing nervous system during its most vulnerable period.
Children born preterm or with low birth weight face a significantly elevated risk of childhood Autism specifically. Very low birth weight (below 1,500 grams) was associated with a three-fold increase in Autism risk, and very low gestational age (less than 32 weeks) increased risk by 2.5 times. These findings align directly with what we’ve observed clinically: the most intense neurological challenges often trace back to the most stressful beginnings.
The “Perfect Storm”: Why Some Children Are More Severely Affected
At PX Docs, we’ve developed a framework called “The Perfect Storm,” which helps explain why some children end up at the most severe end of the spectrum while others are less affected. It’s not one single event that creates profound Autism—it’s a sequence of neurological stressors that accumulate during the most critical periods of development.
- The first component is early exposure to neurological stress—often beginning before birth. Fertility struggles, maternal stress during pregnancy, and exposure to medications or environmental toxins can all affect how the baby’s nervous system develops. Prolonged exposure to stress hormones like cortisol can alter the developing nervous system, making it more vulnerable to dysfunction.
- The second component is birth trauma and interventions. C-sections, vacuum extraction, forceps, induction, prolonged labor, manual assistance, and fetal distress create physical stress on the infant’s neurological system—particularly the upper cervical spine, brainstem, and vagus nerve. The vagus nerve is the longest cranial nerve in the body and serves as the primary driver of the Parasympathetic Nervous System, regulating heart rate, digestion, immune function, and emotional regulation. When compromised during birth, the downstream effects can be massive.
- The third component is early childhood toxic load. After birth, a child’s developing nervous system faces environmental stressors, antibiotics, medications, infections, toxins, and chronic stress. For a system already compromised by prenatal stress and birth trauma, this additional load can push it past its breaking point.
When these three components converge, and they often do in the children we see with the most severe presentations, the result is deep-seated nervous system dysregulation and pediatric dysautonomia. The child’s Autonomic Nervous System gets stuck in a chronic state of sympathetic dominance, which we call the “gas pedal” being stuck on. The parasympathetic “brake pedal,” driven primarily by the vagus nerve, can’t engage properly.
This Autonomic Nervous System dysfunction affects virtually every system in the body—from gut-brain axis disruption and immune dysregulation to impaired vagal tone and sensory processing breakdown.
How Is Profound Autism Diagnosed and Treated Conventionally?
Diagnosis involves a comprehensive evaluation using standardized assessments of intellectual functioning and communication abilities, as well as tools like the Autism Diagnostic Observation Schedule (ADOS). Children with profound Autism are typically diagnosed earlier, with a median age of 46 months versus 57 months for non-profound Autism, because the severity is harder to miss.
The conventional approach includes Applied Behavior Analysis (ABA), speech and language therapy, occupational therapy, and medications for symptoms like aggression, seizures, and anxiety. Each has real value—ABA can teach foundational skills, speech therapy can open communication pathways through AAC devices, and occupational therapy can improve sensory tolerance.
But the current diagnostic and treatment model focuses almost entirely on observable behaviors. It tells you what a child is doing, but rarely addresses why their nervous system is functioning this way. When a child’s nervous system is stuck in chronic fight-or-flight mode, running on a vagus nerve that isn’t functioning properly, you’ll see exactly the signs described above. For many families, conventional interventions alone plateau because they aren’t designed to address the foundational neurological patterns driving the struggles.
Why Does the Nervous System Matter So Much in Profound Autism?
This is where the conversation about profound Autism needs to go, and where almost no other resource takes it.
Subluxation is far more than just a structural issue – it’s a neurological interference that disrupts the function, regulation, and adaptability of the nervous system. It occurs when stress, whether physical, chemical, or emotional, overwhelms the nervous system.
When subluxation is present—especially in the upper cervical spine and brainstem region—it creates a domino effect of dysfunction throughout the Autonomic Nervous System.
Think of it this way: the Sympathetic Nervous System acts as the body’s “gas pedal” (fight-or-flight), while the Parasympathetic Nervous System, driven primarily by the vagus nerve, acts as the “brake pedal” (rest, digest, and regulate). In children with profound Autism, the gas pedal is stuck on, and the brake pedal can’t engage.
Research on autonomic function in children with Autism has found evidence of heart rate hyperarousal and atypical autonomic reactivity, particularly during social tasks. Studies on vagus nerve stimulation in children with Autism and epilepsy have documented improvements in behavior, mood, and communication, suggesting that when vagus nerve function improves, many of the most challenging symptoms improve along with it.
How Can INSiGHT Scans Help Families Understand Their Child’s Nervous System?
One of the most empowering tools available to families is INSiGHT scanning technology. INSiGHT Scans are a set of three neurological assessment technologies used by Neurologically-Focused Chiropractors:
- NeuroThermal scans (infrared thermography)
- NeuroCore sEMG scans (surface electromyography)
- Heart Rate Variability (HRV) testing.
Together, they objectively measure nervous system function, subluxation patterns, and balance of the Autonomic Nervous System.
HRV testing reveals the balance between sympathetic and parasympathetic branches. For children with profound Autism, readings often show extreme sympathetic dominance. sEMG identifies areas of neurospinal tension and dysfunction, particularly in the upper cervical and lower thoracic regions, correlated with brainstem function and gut-immune challenges. Thermal scanning detects temperature asymmetries, indicating areas of dysautonomia.
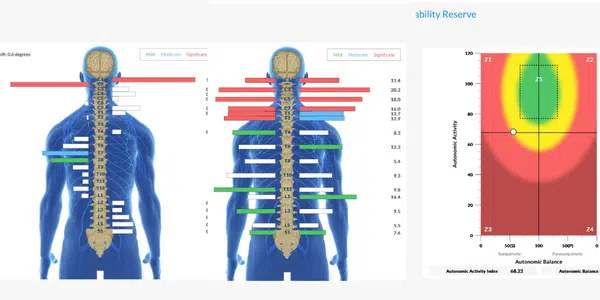
It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for profound Autism or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
When your child can’t tell you how they’re feeling, having measurable insights into their nervous system function is incredibly powerful. Parents can see the patterns of dysregulation and track progress as those patterns shift.
What Does the Healing Journey Look Like for Children with Profound Autism?
Healing from deep neurological patterns takes time—the longer subluxation and nervous system dysregulation have been present, the longer it takes to reorganize.
Neurologically-Focused Chiropractic Care identifies and addresses subluxation through gentle, precise adjustments tailored to each child’s neurological patterns. The goal isn’t to “cure” Autism, it’s to reduce neurological interference, improve vagal tone, and help the nervous system shift out of chronic fight-or-flight mode so that rest, regulation, digestion, and development can take place.
Parents frequently report dramatic shifts in sleep, gut function, emotional regulation, sensory tolerance, and eventually communication. The process isn’t always linear; temporary regressions can occur as the nervous system recalibrates. INSiGHT scans provide objective confirmation that healing is progressing, even when it doesn’t appear to be on the surface.
Joseph, for example, struggled severely with anxiety, autism spectrum disorder, sensory processing disorder, proprioception, poor posture, ataxia, and low muscle tone. He also had digestive issues and constipation that led to bowel blockages.
But, with consistent care and incredible progress with his neurological scans, mom now says, “Joseph is happier, more relaxed, and there are definite improvements in his bowel function and posture. He is engaging more in conversation, and he’s also been fully weaned off his seizure medicine. Joseph is day by day gaining his health back.”
What Steps Can Parents Take Right Now?
- Don’t give up hope. We’ve seen children with the most significant neurological patterns make meaningful progress when the right foundations are addressed.
- Look into your child’s full history. Prenatal stress, birth experience, early illness, antibiotic use, environmental exposures—understanding “The Perfect Storm” that led to your child’s current neurological state is the first step toward addressing it.
- Find a trained Neurologically-Focused Chiropractor who uses INSiGHT scanning technology. Visit the PX Docs directory to find a practitioner near you.
- Continue the therapies that are helping. Neurologically-Focused Chiropractic Care creates the neurological foundation that makes speech therapy, occupational therapy, and other supports more effective. When a child’s nervous system shifts from survival mode to a regulated state, they become more available for learning and connection.
- Be patient. Deep neurological patterns don’t resolve in weeks. But with consistent care and objective measurements to guide the way, meaningful progress is possible.
The Path Forward
Profound Autism represents one of the most significant challenges a family can face. The conventional approach of behavioral therapy and medication management, while valuable, often leaves families feeling like they’ve hit a ceiling.
Understanding that profound Autism has neurological roots, rooted in nervous system dysregulation, subluxation, and dysautonomia, opens up new possibilities. The “Perfect Storm” framework helps explain how these patterns develop, and INSiGHT scanning technology gives families the objective data they need to understand what’s happening inside their child’s nervous system. If you’re ready to explore a neurologically-focused approach for your child, visit the PX Docs directory to find a trained Neurologically-Focused Chiropractor near you. Your child’s journey toward better regulation and a more connected life may be closer than you think.
If you’re ready to explore a neurologically-focused approach for your child, visit the PX Docs directory to find a trained Neurologically-Focused Chiropractor near you. Your child’s journey toward better regulation and a more connected life may be closer than you think.
Frequently Asked Questions About Profound Autism
Can profound Autism improve over time?
Yes. While profound Autism involves significant neurological challenges, children can make meaningful progress, especially when the underlying nervous system dysfunction is identified and addressed early. Improvements in sleep, sensory tolerance, gut function, and even communication are possible when the nervous system shifts out of chronic sympathetic dominance and toward better regulation.
Is chiropractic care safe for children with profound Autism?
Neurologically-Focused Chiropractic Care uses gentle, precise adjustments specifically tailored to each child’s neurological patterns. It’s not the forceful adjustments many people picture. These techniques are designed for pediatric patients, including those with significant sensory sensitivities and complex medical needs.
What’s the difference between profound Autism and level 3 Autism?
Level 3 Autism is the DSM-5 classification indicating the highest support needs. Profound Autism is a proposed subcategory within level 3, specifically defined as having an IQ below 50 or being nonverbal/minimally verbal. Not all level 3 individuals meet the criteria for profound Autism, but most individuals with profound Autism would be classified as level 3.
How long does it take to see improvement with Neurologically-Focused Chiropractic Care?
Every child’s timeline is different, depending on the severity and duration of their neurological dysfunction. Families often report initial improvements in sleep and digestion within the first few weeks. Deeper changes in sensory processing, emotional regulation, and communication typically take months of consistent care, guided by objective INSiGHT scan data.
Can profound Autism be prevented?
While there’s no guaranteed prevention, understanding the “Perfect Storm” framework helps identify risk factors—prenatal stress, birth trauma, early toxic load—that can be minimized. Supporting nervous system health from conception through early childhood is the best proactive step parents can take.
Is profound Autism the same as severe Autism?
The terms are often used interchangeably, but profound Autism has a specific clinical definition proposed by the 2021 Lancet Commission: IQ below 50 or nonverbal/minimally verbal status, requiring 24/7 care. “Severe Autism” is a broader, less precisely defined term.