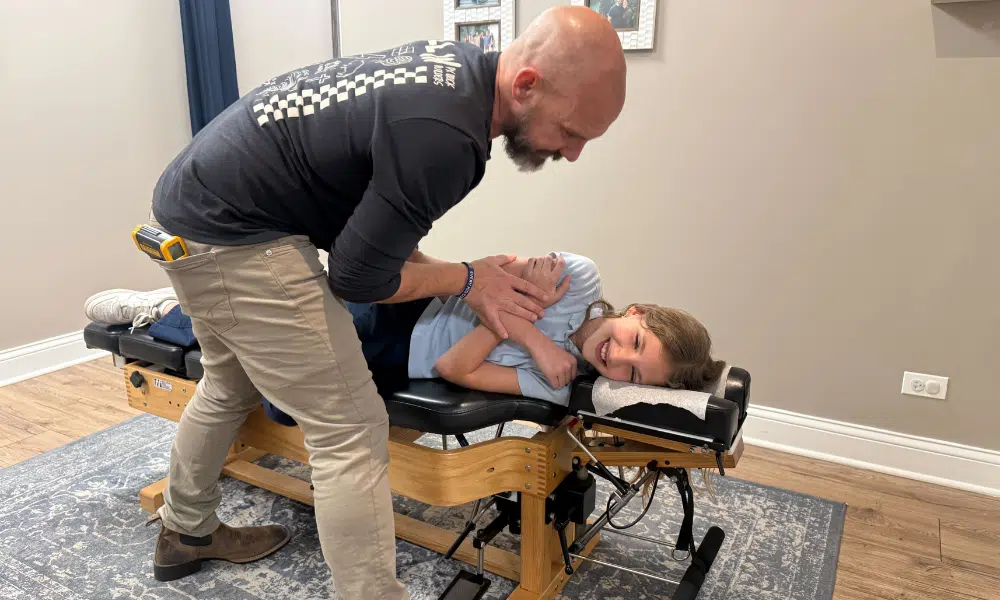
Maybe your child doubles over in pain, clutching their stomach. They’re nauseous, pale, and can barely function, but every test comes back normal. If this pattern sounds familiar, your child may be dealing with abdominal migraines, a condition that affects up to 4% of school-aged children and leaves many families searching for answers.
Unlike traditional migraines that cause head pain, abdominal migraines strike the gut, producing episodes of intense stomach pain, nausea, and vomiting that can last anywhere from one hour to three full days. And here’s what makes it so frustrating for parents: there’s no blood test, no scan, and no imaging study that can confirm the diagnosis. It’s a clinical call based on symptoms and patterns.
But what if the real answer isn’t just in the stomach, or even the head? What if abdominal migraines in children are actually a sign that the nervous system, specifically the gut-brain connection, isn’t functioning the way it should? That’s exactly what we’re going to explore in this article, and it’s the perspective that most pediatric GI specialists and neurologists haven’t yet discussed.
What Are Abdominal Migraines?
An abdominal migraine is a type of migraine that primarily affects the digestive system rather than the head. It’s classified as a functional abdominal pain disorder under the Rome IV criteria, which means the pain is real and often severe, but it isn’t caused by any detectable structural damage or disease in the digestive tract.
These episodes hit suddenly, produce moderate to severe midline abdominal pain (usually centered around the belly button), and then resolve completely between attacks. Kids go back to feeling normal until the next episode, which could be weeks or months later.
Abdominal migraines are considered a subtype of migraine, part of the same family as migraine headaches and cyclical vomiting syndrome. In fact, research shows that these conditions share a common root, disruption in the gut-brain axis, the two-way communication highway between the brain and the digestive system.
The condition most commonly affects children between the ages of 3 and 10, with the average age of onset around 7 years old. It occurs more frequently in girls than boys, and there’s almost always a family history of migraines. If you or your partner deal with migraines, your child has a significantly higher chance of developing abdominal migraines.
Symptoms of Abdominal Migraines in Children
Recognizing abdominal migraines can be tricky because the traits overlap with so many other digestive conditions. Here’s what to watch for:
The hallmark symptom is intense, midline abdominal pain, typically centered around the belly button or described as a dull, achy feeling across the middle of the stomach. This pain is severe enough to interfere with normal activities like school, play, and eating.
Along with stomach pain, children often experience nausea and vomiting, loss of appetite, a noticeably pale or flushed appearance (pallor), sensitivity to light and sound, and, sometimes, a headache.
Episodes follow a stereotypical pattern, meaning they tend to look similar each time they occur. The pain typically lasts at least one hour, with the average episode running about 17 hours. Some attacks can stretch up to 72 hours. Between episodes, your child returns to their normal baseline with no lingering symptoms.
Here’s an important distinction: if your child has ongoing, daily stomach pain, that’s less likely to be abdominal migraines and more likely another functional GI condition. Abdominal migraines are episodic; they come in clear attacks separated by symptom-free periods.
Common Triggers and Risk Factors
Understanding what triggers abdominal migraines is critical for prevention. While each child’s triggers may differ, research has identified several common patterns.
- Family history is the strongest risk factor. Studies show that up to 90% of children with abdominal migraines have a first-degree relative with migraine headaches.
- Stress and emotional upset are among the most frequently reported triggers. This makes sense when you understand the gut-brain connection; emotional stress activates the central nervous system, which then sends disruptive signals to the digestive system. School transitions, family changes, social pressures, and performance anxiety can all serve as triggers.
- Sleep disruption is another major factor. Kids who don’t get enough sleep or who have irregular sleep schedules are more prone to attacks. Sleep is when the nervous system does its most important repair and regulation work, so disrupted sleep means a nervous system that’s already running on empty.
- Dietary triggers play a role for some children, though research suggests food triggers may actually be less common in abdominal migraines than in traditional migraines. That said, known triggers can include chocolate, cheese, processed meats with nitrates, citrus fruits, MSG-containing foods, and caffeine. Skipping meals, which causes blood sugar drops, is also a common trigger.
Other recognized triggers include travel (especially long car rides), motion sickness, bright or flickering lights, extended fasting, and dehydration. Keeping a diary of your child’s episodes, including what they ate, how they slept, and what was happening emotionally in the days leading up to an attack, can help you identify their specific trigger pattern.
Why Abdominal Migraines Are Really a Nervous System Problem
Here’s where most articles on abdominal migraines stop: they describe the symptoms, list the triggers, and offer medication options. But they miss the bigger picture. Abdominal migraines aren’t just a stomach problem. They’re often a nervous system problem that shows up in the stomach.
The gut-brain axis is a complex, bidirectional communication network connecting the brain and the digestive system. The Autonomic Nervous System, specifically the parasympathetic and sympathetic branches, connects directly to the enteric nervous system, the network of over 100 million neurons lining the gut that scientists call the “second brain.”
Signals travel back and forth constantly between the gut and the brain, transmitted through spinal and vagal afferent nerves to the brainstem and sensory processing circuits. The vagus nerve is the primary highway for this communication, transmitting signals in both directions and regulating everything from gut motility and enzyme secretion to inflammation and pain perception.
When this system works properly, digestion runs smoothly. But when the nervous system becomes dysregulated, when it gets stuck in a state of stress and imbalance, that communication breaks down. And that’s when problems like abdominal migraines can emerge.
Researchers have identified that the most accepted explanation for functional abdominal pain disorders like abdominal migraines involves visceral hypersensitivity, meaning the gut becomes overly sensitive to normal sensations. The brain-gut axis starts secreting excitatory neurotransmitters abnormally, and serotonin plays a particularly important role.
Serotonin affects gut sensation, motility, and secretion, and approximately 90% of the body’s serotonin is produced in the gut. When the vagus nerve isn’t functioning optimally, serotonin signaling gets disrupted, contributing to the pain attacks, nausea, and motility changes characteristic of abdominal migraines.
This is exactly what we see in the pattern of nervous system dysregulation: the Autonomic Nervous System loses its balance between the sympathetic “gas pedal” (fight-or-flight) and the parasympathetic “brake pedal” (rest, digest, and regulate).
Sympathetic Dominance and Vagus Nerve Dysfunction
When your child’s nervous system gets stuck in sympathetic dominance, meaning the “gas pedal” is floored while the “brake pedal” barely works, every system controlled by the Autonomic Nervous System is affected. And the digestive system is one of the first to suffer.
Think about it this way. Your body was designed so that digestion happens during the parasympathetic “rest and digest” state. Blood flow goes to the gut, enzymes are released, motility kicks in, and everything moves along. But when the Sympathetic Nervous System is dominant, the body diverts resources away from digestion. Blood flow shifts to the muscles. Gut motility slows down. The immune system in the gut becomes dysregulated. And the vagus nerve, the master regulator of all these digestive processes, can’t do its job properly.
This is the connection that conventional medicine is just starting to explore. Research published in the Journal of Neurogastroenterology and Motility has shown that abdominal variants of migraine, including abdominal migraines and cyclical vomiting syndrome, share a common pathophysiological root in the gut-brain axis mechanism, and that autonomic dysfunction plays a central role.
Children with abdominal migraines have been shown to have significantly lower gastric emptying times and reduced antral motility during pain episodes, direct evidence that the nervous system’s control of gut function is impaired. It’s also been noted that sympathetic hyperactivity may account for symptoms like pallor during episodes, further supporting the role of autonomic imbalance.
Even the research community itself has acknowledged this connection. A 2020 review noted that noninvasive vagal nerve stimulation has shown promise in reducing pain intensity in migraine patients, essentially confirming that restoring vagus nerve function is a key piece of the puzzle.
The “Perfect Storm” of How Nervous System Dysfunction Develops in Children
So how does a child’s nervous system get stuck in this state of imbalance in the first place? At PX Docs, we’ve identified a pattern we call The “Perfect Storm,” a sequence of early-life stressors that accumulate and interact to disrupt a child’s neurological development.
It often starts before birth. Prenatal stress, including maternal anxiety, depression, chronic stress during pregnancy, and even fertility challenges, exposes the developing fetus to elevated stress hormones like cortisol. These hormones cross the placenta and can alter the development of the Autonomic Nervous System during its most critical growth period.
Then comes the birth process itself. Interventions like C-sections, forceps delivery, vacuum extraction, and induction can create physical stress on the infant’s delicate upper cervical region and brainstem, exactly where the vagus nerve originates.
After birth, early childhood stressors pile on. Frequent antibiotic use disrupts the gut microbiome. Chronic ear infections signal immune system dysregulation. Colic, reflux, and constipation, often dismissed as “normal baby stuff”, are actually early warning signs that the nervous system isn’t properly regulating digestive function.
These different types of stressors all contribute to subluxation, a state of misalignment, fixation, and neurological interference that disrupts the normal function of the nervous system.
When you add all these factors together, you get a child whose nervous system has been under stress since before day one. By the time abdominal migraines show up (often between ages 3 and 10), the pattern of dysregulation has been building for years. And that’s why addressing just the symptoms, without looking at the underlying nervous system dysfunction, so often falls short.
A Neurologically-Focused Approach
This is where Neurologically-Focused Chiropractic Care offers something different. Rather than chasing the symptoms of abdominal migraines, this approach looks at the nervous system itself, specifically the Autonomic Nervous System balance and vagus nerve function that directly control digestive function.
It’s important to note that INSiGHT scanning technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for abdominal migraines or any other condition, not even back pain. Instead, these INSiGHT Scans help track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
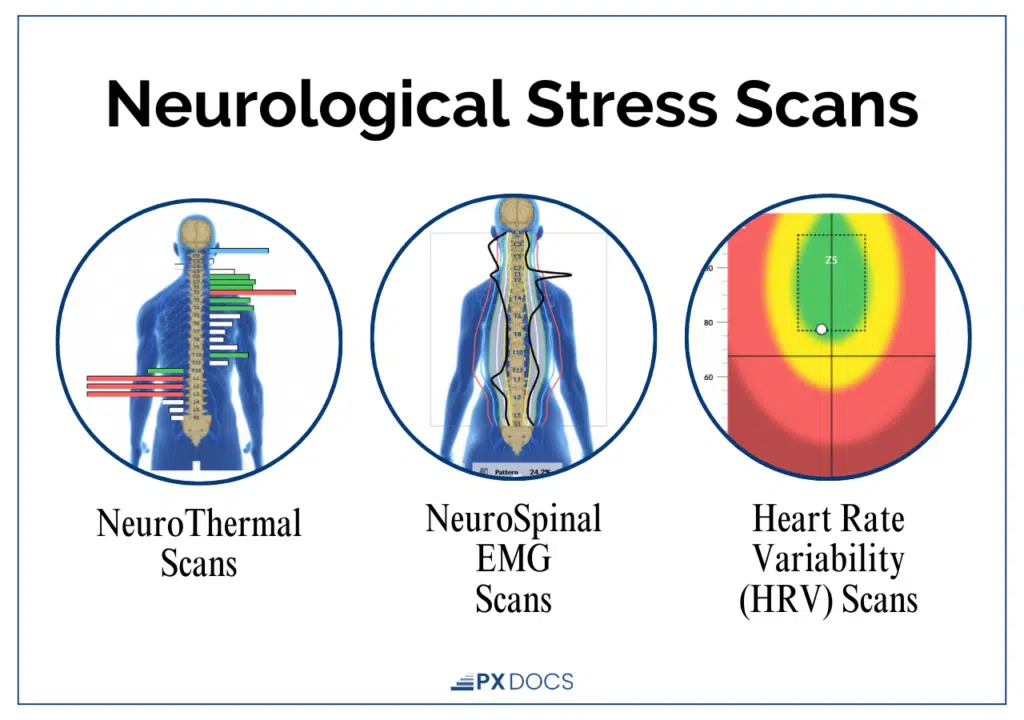
INSiGHT Scanning Technology uses three primary assessments to objectively measure nervous system function:
- Heart Rate Variability (HRV) Analysis measures the balance between the sympathetic and parasympathetic branches of the Autonomic Nervous System. For children with abdominal migraines, this scan can reveal whether the nervous system is stuck in sympathetic dominance, the very pattern researchers have linked to functional GI disorders.
- Surface Electromyography (sEMG) assesses electrical activity of the nervous system along the spine, identifying areas of tension and altered neuromuscular function that may be contributing to nervous system interference.
- Thermal Scanning uses infrared sensors to measure temperature differences along the spine, which can indicate areas of dysautonomia, exactly the type of autonomic imbalance associated with abdominal migraines.
For parents who’ve spent years watching their child suffer through episode after episode with no clear answers, these objective measurements can finally provide the clarity they’ve been searching for. Instead of guessing about what’s wrong, you can see exactly where the nervous system is struggling and track progress over time.
The Connection Between Abdominal Migraines and Other Conditions
Abdominal migraines rarely exist in isolation. Research consistently shows that children with abdominal migraines often have overlapping conditions that point to the same underlying pattern of nervous system dysregulation.
- Cyclical vomiting syndrome shares significant overlap with abdominal migraines, and researchers consider both to be abdominal variants of migraine with a common gut-brain axis root. Many children experience both conditions at different points.
- Anxiety and mood challenges are significantly more common in children with functional abdominal pain disorders. This isn’t surprising when you understand the vagus nerve’s role in emotional regulation; the same nerve that controls digestive function also plays a major role in calming the stress response and regulating mood.
- Sleep disturbances often accompany abdominal migraines. Poor sleep is both a trigger for episodes and a consequence of nervous system dysregulation. When the sympathetic nervous system is dominant, the body can’t transition smoothly through sleep cycles.
- Sensory sensitivities, including sensitivity to light, sound, and certain textures, reflect the broader pattern of a nervous system that’s hypersensitive and struggling to filter stimuli appropriately. These same children may exhibit signs of Sensory Processing Disorder or engage in sensory-seeking behaviors.
If your child has abdominal migraines alongside any of these patterns, it’s not a coincidence. It’s evidence that the underlying issue is neurological, and addressing the nervous system as a whole, rather than each symptom individually, may be the key to lasting improvement.
Do Kids Outgrow Abdominal Migraines?
This is one of the most common questions parents ask, and the answer is both encouraging and important to understand fully.
The good news: Most children will see abdominal migraines resolve over time. Symptoms typically begin fading around puberty, and approximately 60% of children no longer experience abdominal pain episodes by their late teenage years.
The less straightforward news: up to 70% of children with abdominal migraines go on to develop migraine headaches later in adolescence or adulthood. The symptoms shift, from the gut to the head, but the underlying pattern of nervous system dysfunction often persists.
This is a critical point. “Outgrowing” abdominal migraines doesn’t necessarily mean the nervous system has healed. It may simply mean the dysfunction is expressing itself differently as the child’s body develops. The digestive symptoms may resolve, but if the autonomic imbalance remains, it can show up as migraines, anxiety, IBS, or other stress-related conditions later in life.
That’s why addressing the root nervous system dysfunction now, rather than just waiting for children to “grow out of it”, matters so much for long-term health outcomes.
Getting to the Root
Abdominal migraines in children are more than unexplained stomach pain. They’re a window into how the nervous system is functioning, or struggling to function. When the gut-brain axis is disrupted, when vagus nerve signaling falters, and when the Autonomic Nervous System gets stuck in sympathetic dominance, the digestive system is often the first place those problems show up.
Understanding the “Perfect Storm” of factors that can dysregulate a child’s nervous system, and knowing that tools exist to objectively measure and address that dysregulation, gives parents a path forward that goes beyond symptom management.Your child’s stomach pain is real. Their suffering is valid. And there is hope for getting to the root of what’s driving these episodes. Visit the PX Docs directory to find a Neurologically-Focused Chiropractor near you who can help evaluate your child’s nervous system function and create a plan to support their healing journey.