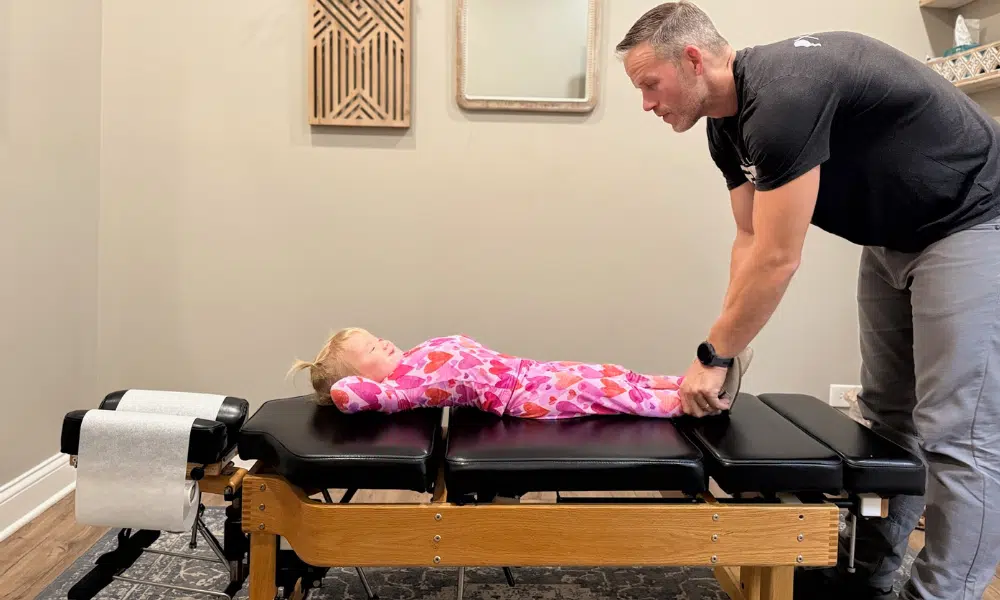
A sensory diet is a personalized plan of physical activities and sensory experiences designed to provide your child’s brain and body with the specific input they need to stay focused, calm, and organized throughout the day. Coined by occupational therapist Patricia Wilbarger in 1984, the term describes a scheduled set of sensory-based activities—not a food plan—tailored to your child’s unique neurological needs.
As a parent, you’ve probably noticed that your child functions better after certain activities. Maybe they’re calmer after jumping on a trampoline, more focused after chewing crunchy snacks, or more regulated after a bear hug. That’s not a coincidence. Your child’s nervous system is hungry for specific types of input, and when it doesn’t get what it needs, you’ll see the meltdowns, the zoning out, the inability to sit still, or the refusal to participate.
If your child has been diagnosed with Sensory Processing Disorder, Autism, or ADHD, chances are an occupational therapist has already mentioned a sensory diet. But here’s what most parents aren’t told: the sensory activities themselves are only addressing the surface. The real question is why your child’s nervous system needs so much external help to regulate in the first place.
What Does a Sensory Diet Include?
A sensory diet includes individualized activities that target one or more of the body’s sensory systems: tactile (touch), vestibular (movement and balance), proprioceptive (body awareness through muscles and joints), auditory (sound), visual (sight), olfactory (smell), and gustatory (taste). An occupational therapist typically designs the plan based on your child’s specific sensory profile.
The activities fall into two general categories depending on your child’s needs.
For children who are overresponsive and easily overwhelmed by sounds, textures, or movement, calming activities such as deep pressure, weighted blankets, slow rocking, and quiet spaces can help lower their arousal levels.
For children who are underresponsive, sluggish, hard to engage, or seeming “checked out,” alerting activities like jumping, spinning, crunchy foods, and bright visual stimulation can help wake their system up.
Common sensory diet activities include:
- Heavy work like pushing, pulling, or carrying weighted objects
- Vestibular input from swinging, spinning, or bouncing on a trampoline
- Tactile experiences like play-dough, sensory bins filled with rice or beans, or finger painting
- Oral motor input from chewing gum or crunchy snacks
- Auditory input from calming music or noise-canceling headphones.
The key is that a sensory diet isn’t a one-time fix. It’s a scheduled, ongoing plan woven into your child’s daily routine, before school, during transitions, after overstimulating environments, and at bedtime. And just like a food diet, it needs regular adjustment as your child’s needs shift from day to day.
Why Does My Child Need a Sensory Diet?
Children need a sensory diet when their nervous system can’t independently regulate the amount of sensory input it receives. Research estimates that between 5% and 13% of children in the United States experience significant sensory processing challenges. And those numbers climb much higher in children with neurodevelopmental conditions. Studies show atypical sensory processing affects approximately 40% of children with Autism and up to 95% of those with other neurodevelopmental conditions.
But here’s the part that gets missed: sensory processing difficulties don’t happen in isolation. They’re a signal that something deeper is going on within your child’s Autonomic Nervous System.
Research published in Frontiers in Integrative Neuroscience found that children with sensory modulation issues show atypical patterns of both Sympathetic and Parasympathetic Nervous System activity—meaning their entire Autonomic Nervous System regulation is off balance.
Think of it this way. Your child’s nervous system has a gas pedal (the sympathetic “fight or flight” system) and a brake pedal (the parasympathetic “rest, regulate, and digest” system). In a well-regulated child, these two systems work together smoothly—speeding up when needed, slowing down when it’s time to rest. But in children with sensory processing challenges, the gas pedal is often stuck down, and the brake pedal barely works.
That’s why they can’t filter out the hum of fluorescent lights, why the tag on their shirt feels like sandpaper, or why they crash into everything trying to feel their own body.
A sensory diet helps compensate for this imbalance from the outside in. It gives the nervous system the input it’s craving. But it doesn’t fix why the nervous system is dysregulated in the first place, and that’s where most approaches stop short.
What Are the Signs Your Child Needs a Sensory Diet?
Every child’s sensory profile is different, but there are common patterns that signal the nervous system isn’t processing input correctly. Children who may benefit from a sensory diet often show these signs:
- Sensory seeking behaviors. Constantly moving, jumping, crashing into furniture, chewing on clothing or non-food items, touching everything, seeking out loud noises or intense flavors
- Sensory avoidance behaviors. Covering ears at normal sounds, refusing certain clothing textures (tags, seams, socks), gagging at certain food textures, avoiding messy play, and becoming distressed in bright or busy environments
- Difficulty with transitions. Meltdowns when changing activities, extreme rigidity around routine, inability to shift attention
- Poor body awareness. Bumping into things, trouble with fine motor tasks, difficulty judging personal space, heavy-handedness with objects
- Emotional dysregulation. Going from zero to meltdown with little warning, difficulty calming down once upset, and extreme reactions to minor changes
- Attention and focus challenges. Can’t sit still in class, fidgeting constantly, seems “spaced out” or unable to follow directions
- Sleep difficulties. Trouble falling asleep, restless sleep, frequent night waking, not waking refreshed
What’s important to understand is that these aren’t just behavioral problems; they’re neurological ones. Your child isn’t choosing to be difficult. Their nervous system is literally overwhelmed, underwhelmed, or both at different times throughout the day. A study notes that the current evidence on sensory diets, while promising, remains limited and mixed, which is why understanding the root neurological cause matters so much.
How Do You Create a Sensory Diet for Your Child?
Creating an effective sensory diet starts with understanding your child’s unique sensory profile. Here’s a practical framework to get started:
- Step 1: Observe your child’s patterns. Notice what they seek out (movement? deep pressure? certain textures?) and what they avoid (loud sounds? light touch? busy visual environments?). These preferences are clues to what their nervous system needs.
- Step 2: Work with an occupational therapist. A trained OT can evaluate your child using tools like the Sensory Profile or Sensory Processing Measure to identify specific areas of over- or underresponsiveness. This professional assessment is the foundation for an effective sensory diet.
- Step 3: Build activities into the daily routine. The most effective sensory diets aren’t extra tasks added on top of an already busy schedule. They’re woven into what your child already does—crunchy snacks at breakfast, a mini trampoline session before homework, a weighted lap pad during car rides, and deep pressure squeezes before bed.
- Step 4: Track and adjust regularly. What works on Monday might not work on Thursday. Your child’s sensory needs shift based on sleep quality, environmental demands, stress levels, and developmental changes. Stay flexible and keep communicating with your OT.
- Step 5: Don’t force it. This is critical. Sensory activities should never feel like punishment or medicine. If your child resists an activity, their nervous system may be telling you it’s too much. Follow their lead and offer choices.
Here’s a practical example of what a sensory diet might look like for a second-grader who is a sensory seeker:
- Morning: Jump on a mini trampoline for 5 minutes, eat crunchy cereal, wear a compression shirt under school clothes
- School arrival: Carry a heavy backpack, do wall push-ups before entering the classroom
- Mid-morning: Use a fidget tool during seated work, sit on a wobble cushion
- Lunch: Crunchy and chewy foods, drink a thick smoothie through a straw
- Afternoon: Movement break with heavy work (carrying books, pushing chairs in), use therapy putty during reading
- After school: Outdoor play with climbing, swinging, and digging
- Evening: Warm bath with deep pressure from towel drying, slow rocking, weighted blanket at bedtime
What Sensory Diet Activities Work for Each Sensory System?
Understanding which sensory system your child needs input for helps you choose the right activities. Here’s a breakdown:
- Proprioceptive activities (body awareness): These are the workhorses of most sensory diets because proprioceptive input is almost universally calming and organizing. Activities include pushing a heavy cart, carrying groceries, doing animal walks (bear crawl, crab walk), climbing, hanging from monkey bars, kneading dough, and doing push-ups against a wall.
- Vestibular activities (movement and balance): Swinging (linear swinging is calming; rotary spinning is alerting), rocking in a rocking chair, rolling down a hill, log rolling on the floor, riding a bike, and using a balance board. Be cautious with vestibular input — it’s powerful and can easily overstimulate.
- Tactile activities (touch): Sensory bins with rice, beans, or sand; finger painting; play dough; water play; brushing with a therapy brush (Wilbarger protocol under OT guidance); and exploring different textures like sandpaper, silk, and bumpy surfaces.
- Auditory activities: Calming music, white noise machines, nature sounds, singing or humming, listening to audiobooks, and using noise-canceling headphones in overwhelming environments. Some children respond well to rhythmic music; others need near-silence.
- Oral motor activities: Chewing gum, crunchy snacks (carrots, pretzels, apples), sucking thick liquids through a straw, blowing bubbles, and using a vibrating toothbrush. Oral motor input provides both proprioceptive and calming sensory input to the jaw and face.
- Visual activities: Lava lamps, bubble tubes, dimmed lighting, reducing visual clutter in the home environment, and using natural light instead of fluorescent bulbs when possible.
What Causes Sensory Processing Challenges in Children?
At PX Docs, we’ve worked with thousands of families whose children struggle with sensory processing challenges. And what we’ve found is that sensory difficulties rarely show up on their own. There’s almost always a deeper neurological story, one that started long before the sensory diet was prescribed.
We call it The “Perfect Storm,” and it follows a predictable pattern with three core components:
Early exposure to neurological stress, like fertility struggles, maternal stress during pregnancy, and birth interventions like C-sections, forceps, vacuum extraction, induction, or prolonged labor, creates early neurological stress. During this sensitive developmental window, the baby’s autonomic nervous system, especially the vagus nerve, is incredibly vulnerable. These early stressors can shift the system toward sympathetic dominance, increased tension, and reduced adaptability from birth.
After birth, environmental toxins, frequent antibiotics, medications, and chronic illness pile on. Parents often recognize these early warning signs—colic, reflux, ear infections, eczema, sleep problems, constipation—but are told they’re “normal” and that their child will grow out of them. They’re not normal. They’re early signs of nervous system dysregulation.
As these early stressors stack up, the child’s neurological foundation doesn’t develop as it should. This leads to subluxation, a condition involving misalignment, fixation, and neurological interference within the neurospinal system, which disrupts brain-body communication. It also leads to vagus nerve dysfunction, dysautonomia (keeping kids stuck in fight-or-flight), sensory processing challenges, and delayed motor development.
Children with sensory processing challenges frequently also experience ADHD, anxiety, sleep conditions, and digestive issues. This co-occurrence isn’t coincidental; these conditions share the same underlying neurological root of Autonomic Nervous System dysfunction and subluxation that disrupts how the brain receives, processes, and responds to sensory information.
Can Chiropractic Care Help with Sensory Processing Issues?
This is where our approach at PX Docs differs from what you’ll find anywhere else. While a sensory diet addresses sensory input from the outside, Neurologically-Focused Chiropractic Care works to restore the nervous system’s ability to process and regulate that input from the inside.
Our trained PX Docs practitioners use state-of-the-art INSiGHT Scanning Technology to get an objective picture of your child’s nervous system function. This technology includes three components:
- Heart Rate Variability (HRV) Analysis—measures the balance between the sympathetic (“fight or flight”) and parasympathetic (“rest, regulate, and digest”) branches of the autonomic nervous system
- Surface Electromyography (sEMG)—assesses the electrical activity of muscles along the spine, identifying areas of tension and altered neuromuscular function
- Thermal Scanning—uses infrared sensors to measure temperature differences along the spine, which can indicate areas of dysautonomia
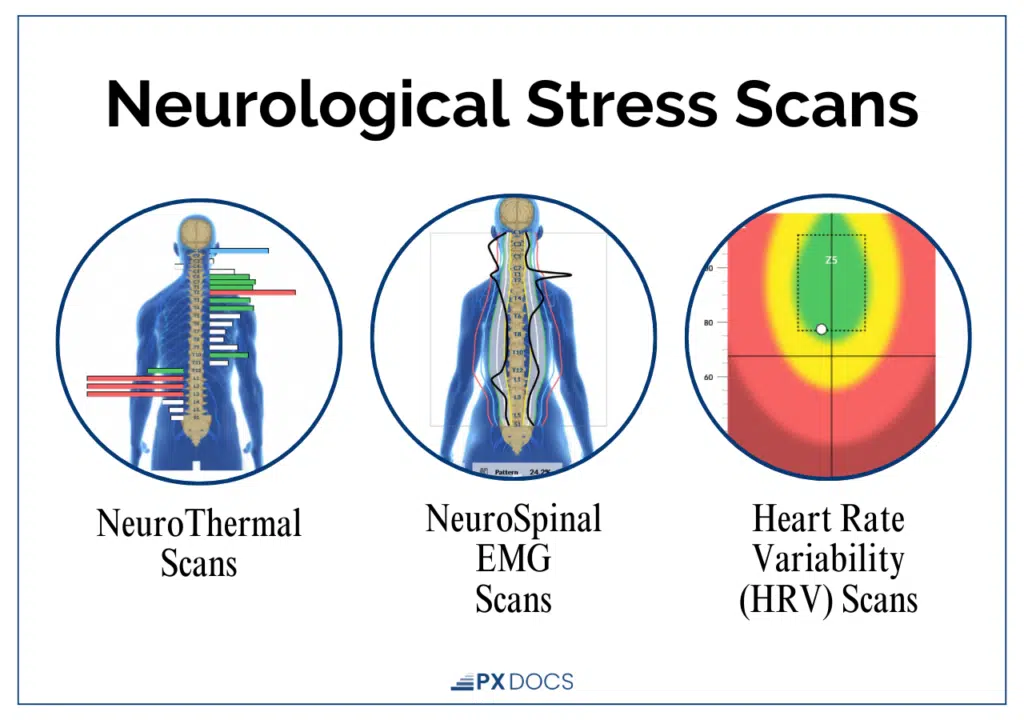
It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for Sensory Processing Disorder or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
When subluxation is present, it alters the sensorimotor input that your child’s brain depends on to properly process sensory information. By restoring proper neurological function through specific, gentle adjustments, we help the nervous system move out of that stuck sympathetic state and back toward balance. For many children, this means the sensory diet activities they’re already doing start working better, because the nervous system can actually receive and process the input.
How to Get the Most Out of Your Child’s Sensory Diet
A sensory diet works best when it’s part of a comprehensive approach. Here’s how to maximize its impact:
- Combine with nervous system support. A sensory diet addresses the input side of the equation. Neurologically-Focused Chiropractic Care addresses the processing side. Together, they create a more complete approach to your child’s sensory challenges.
- Communicate across environments. Share your child’s sensory diet with teachers, caregivers, and therapists to ensure the strategies remain consistent. A sensory diet that only happens at home won’t carry your child through a full school day.
- Watch for the “hidden” signs. Pay attention to what happens before the meltdown, not just during it. Yawning, rubbing eyes, increased fidgeting, or withdrawal can all signal that your child’s sensory tank is running low.
- Respect the ebbs and flows. Sensory needs change with growth spurts, illness, sleep quality, and seasonal changes. A sensory diet that worked perfectly last month may need adjusting this month. That’s normal.
- Trust your instincts. You know your child better than anyone. If something isn’t working or if you feel like the sensory diet is only putting a Band-Aid on a deeper problem, that instinct is worth following.
What Should You Do Next if Your Child Needs a Sensory Diet?
If you’ve been doing the sensory diet, the OT sessions, the dietary changes, and the accommodations, and your child is still struggling—please know that you’re not failing. It’s possible that the root neurological cause simply hasn’t been addressed yet.
Understanding the nervous system’s role in sensory processing opens up a whole new set of answers. The meltdowns, the sensory overload, the constant need for input, it all starts making sense when you look at it through a neurological lens. If you’re ready to explore what’s happening beneath the surface for your child, we encourage you to visit the PX Docs Directory to find a trained Neurologically-Focused Chiropractor near you. These practitioners specialize in pediatric nervous system assessment using INSiGHT Scans and can help determine whether subluxation and nervous system dysregulation are contributing to your child’s sensory challenges.
Frequently Asked Questions About Sensory Diets
What is a sensory diet?
A sensory diet is a personalized plan of sensory activities scheduled throughout the day to help a child’s nervous system stay regulated, focused, and organized. It’s designed by an occupational therapist based on the child’s specific sensory profile and can include activities targeting proprioception, vestibular input, tactile stimulation, auditory input, and oral motor engagement.
Is a sensory diet related to food?
No. Despite the word “diet,” a sensory diet has nothing to do with food or nutrition. The term was coined by Patricia Wilbarger in 1984 to describe how the nervous system needs a balanced “diet” of sensory input throughout the day, similar to how the body needs balanced nutrition.
How long does a sensory diet take to work?
Many children show immediate benefits from individual sensory activities—calming down after deep pressure or becoming more focused after movement. The cumulative effects of a consistent sensory diet typically become noticeable within a few weeks. However, if the underlying nervous system dysfunction isn’t addressed, the benefits may plateau or require increasingly more input to achieve the same effect.
Can I create a sensory diet at home without an OT?
While you can start incorporating sensory activities at home by observing what calms or alerts your child, a formal sensory diet should be designed by a qualified occupational therapist. They can evaluate your child’s specific sensory profile and ensure the activities are appropriate for their needs. Incorrect sensory input—especially vestibular stimulation—can actually increase dysregulation.
Does my child need a sensory diet forever?
Not necessarily. For some children, a sensory diet is a bridge that helps them develop self-regulation skills over time. As the nervous system matures and learns to process input more effectively—particularly when root-cause nervous system dysfunction is addressed—many children need less structured sensory input. The goal is always to move toward greater independence and self-regulation.
What’s the difference between a sensory diet and sensory integration therapy?
A sensory diet is a home and school program of daily sensory activities, while sensory integration therapy (also called Ayres Sensory Integration or ASI) is a clinical intervention provided by an occupational therapist in a therapeutic setting. The two approaches are complementary; therapy sessions work on improving the brain’s ability to process sensory information, while the sensory diet helps maintain nervous system regulation throughout the day.
Can chiropractic care help with sensory processing challenges?
Neurologically-Focused Chiropractic Care addresses the nervous system dysfunction that often underlies sensory processing challenges. By identifying and addressing subluxation (misalignment, fixation, and neurological interference) in the spine and nervous system, this approach aims to restore proper balance of the Autonomic Nervous System and sensory-motor integration. It works alongside occupational therapy and sensory diet strategies, not as a replacement for them.