Watching your child suddenly collapse to the ground, their body stiffening and jerking in seizure-like movements, is every parent’s nightmare. Imagine undergoing extensive testing and receiving a confusing diagnosis—vasovagal syncope—and getting sent home with little explanation beyond “drink more water and eat more salt.”
For parents whose children suffer from sudden seizures or convulsions, receiving news that traditional anti-epileptic medications are ineffective can heighten fears enormously. Negative EEG readings and lack of improvement despite medical care lead many physicians to scratch their heads over what could be behind these dramatic episodes.
Conventional medicine often points toward epilepsy as the diagnosis. According to the World Health Organization, around 50 million people are diagnosed with epilepsy worldwide, and approximately one-quarter are children. However, the culprit of these fainting episodes may be something entirely different: vasovagal syncope seizures.
Because these fainting episodes mimic epileptic seizures without necessarily responding to medications for epilepsy, these convulsive spells can be easily confused. Older studies have suggested that as many as 30% of people with cardiovascular syncope have been misdiagnosed with epilepsy.
We’ll shed light on the distinguishing features of vasovagal syncope seizures, the warning signs that appear before episodes, their causes, the critical role of the vagus nerve, and drug-free care solutions that target the root of the issue.
What Are Vasovagal Syncope Seizures?
A vasovagal syncope seizure occurs when reduced blood flow to the brain temporarily causes loss of consciousness. This occurrence is typically accompanied by seizure-like shaking, stiffness, or jerking movements of the muscles, symptoms that often resemble an epileptic episode.
Medical professionals may also refer to this condition as neurocardiogenic syncope or convulsive syncope—all terms describing the same phenomenon, in which the nervous system’s overreaction causes a dramatic drop in blood pressure and a slowing of the heart rate, reducing blood flow to the brain.
Unlike epileptic seizures, vasovagal syncope seizures are triggered by situational changes in heart rate and blood circulation rather than abnormal electrical activity in the brain. During a vasovagal episode, the vagus nerve, which helps regulate the parasympathetic “rest and digest” functions, overreacts to triggers like extreme emotional distress or sudden position changes.
Heart rate slows dramatically (bradycardia), and blood vessels widen, allowing blood to pool in the legs. This combination causes blood pressure to drop abruptly, reducing oxygen to the brain and leading to temporary loss of consciousness. When cerebral hypoperfusion (inadequate blood supply to the brain) lasts from 6-8 seconds, the brain’s oxygen deprivation can trigger automatic motor responses—the convulsive, seizure-like activity parents observe.
Research shows that about 20% of the population is affected by syncope, with a portion experiencing vasovagal seizures. Still, differentiating between epilepsy, psychogenic non-epileptic seizures (PNES), and syncope-related seizures remains complex. Telltale signs lie in the detailed history and witness accounts, rather than in testing.
Fortunately, understanding how the vagus nerve underlies certain seizure presentations can help guide appropriate non-drug care options. Addressing nervous system dysregulation through Neurologically-Focused Chiropractic Care lends personalized solutions beyond conventional one-size-fits-all anti-seizure medications.
Understanding the Vagus Nerve During a Vasovagal Episode
The vagus nerve, a critical component for nervous system regulation, plays a central role in triggering vasovagal seizures. Known as the “wandering nerve” extending from the brain to the abdomen, the vagus helps control digestion, breathing, heart rate, inflammation, and other parasympathetic “rest and regulate” functions.
Any dysfunction along the intricately networked vagus neural communication, however, can lead to sudden cardiovascular shifts. Research shows that when the vagus nerve overreacts, it sends excessive signals that slow the heart rate dramatically (sometimes briefly stopping it—asystole) while simultaneously widening blood vessels throughout the body. This can then abruptly lower heart rate and blood pressure, reduce blood flow to the brain, and result in a brief loss of consciousness.
The vagus nerve regulates cardiovascular autonomic control, including heart rate, blood pressure, and blood vessel tone. When functioning properly, it helps your body respond appropriately to different situations and maintains stable blood flow to the brain.
Those with existing vagus nerve dysfunction from early trauma, chronic anxiety, or nervous system imbalance stand most susceptible to vasovagal seizures. Restoring healthy vagal tone and neural coordination helps prevent recurrence.
Recognizing the Warning Signs Before Your Child Faints
One of the most important things parents can learn is recognizing prodromal symptoms—the warning signs that appear 30-60 seconds before loss of consciousness, providing a critical window to lie down and prevent injury.
Most children experiencing vasovagal syncope will report feeling dizzy or lightheaded as the first warning sign.
Common Warning Signs (Prodromal Symptoms):
- Feeling dizzy or lightheaded (most common)
- Feeling nauseous or having an upset stomach
- Vision changes, including tunnel vision, blurred vision, or blackout
- Feeling weak, shaky, or unsteady
- Cold, clammy skin or sudden sweating
- Pale or flushed skin color changes
- Increased awareness of the heartbeat
Children with nervous system dysfunction from The “Perfect Storm” may experience more intense or frequent warning signs, as their dysregulated Autonomic Nervous System responds more dramatically to triggers.
The presence of these warning signs distinguishes vasovagal syncope from most epileptic seizures, which typically begin without warning or with a completely different type of aura.
Vasovagal Syncope vs. Epileptic Seizures: How to Tell the Difference
Parents often feel confused when doctors struggle to determine whether their child’s episodes are vasovagal syncope or epileptic seizures. Studies show that 20-30% of people initially diagnosed with epilepsy actually have cardiovascular causes of syncope.
Key Differences:
| Feature | Vasovagal Syncope | Epileptic Seizure |
| Duration | Seconds to 1-2 minutes | 3-5+ minutes |
| Warning Signs | Dizziness, nausea, vision changes | Aura or none |
| Triggers | Position changes, blood, and emotional stress | Often none or sleep-related |
| Unconsciousness | Very brief (5-20 seconds) | Longer (1-5 minutes) |
| Movements | Brief myoclonic jerks; may include tonic-clonic | Rhythmic tonic-clonic typical |
| Tongue Biting | Rare | Common |
| Recovery | Quick, alert within 1 minute | Postictal confusion 15-30 minutes |
| EEG During Episode | Brain wave slowing | Epileptic spike activity |
The most confusing aspect is that vasovagal syncope CAN produce tonic-clonic convulsions. The key difference: in epileptic seizures, movements result from abnormal electrical brain discharges; in convulsive syncope, they result from the brain’s protective response to oxygen deprivation.
The single most reliable differentiator is what happens AFTER consciousness returns: Vasovagal children wake up quickly and are oriented within 60 seconds, while epileptic seizures cause postictal confusion lasting 15-30 minutes or longer.
Underlying Causes: The Perfect Storm Behind Vasovagal Vulnerability
At the root of most chronic pediatric health conditions lies a cascade of events that disrupt normal nervous system development. At PX Docs, we call this “The Perfect Storm.”
Stage 1: Prenatal Stress
Maternal stress during pregnancy can impact the developing fetus’s Autonomic Nervous System, creating baseline dysregulation that makes the child more susceptible to vasovagal syncope.
Stage 2: Birth Trauma – The Primary Overlooked Cause
The most overlooked aspect of childhood vasovagal syncope is birth trauma. Physical stress on an infant’s delicate neck during birth—especially interventional deliveries—can create neurological dysfunction underlying vasovagal episodes for years.
During difficult or traumatic births involving C-sections, forceps, or vacuum extractions, significant forces are placed on the upper cervical spine and the area where the vagus nerve exits the skull. These birth interventions create subluxation and neurological interference in the nervous system’s communication pathways, specifically affecting vagus nerve function and cardiovascular autonomic control.
Common birth trauma factors:
- C-section deliveries: Require pulling the baby through a small incision
- Forceps or vacuum extraction: Create compression and pulling forces
- Prolonged or rapid labor: Extended compression or inadequate accommodation time
- Breech presentation: Abnormal forces during delivery
Stage 3: Triggering Factors in Children with Nervous System Dysfunction
In children without underlying dysfunction, common triggers might cause mild lightheadedness. But when the “Perfect Storm” has created nervous system vulnerability, these same triggering factors can provoke full vasovagal episodes.
Common triggering factors:
- Position changes: Moving from lying/sitting to standing too quickly
- Prolonged standing: School assemblies, church services, waiting in lines
- Seeing blood: Blood draws, injuries, medical procedures
- Medical procedures: Vaccinations, injections, dental work
- Emotional stress: Anxiety, fear, intense emotions
- Hot environments or dehydration
In those with a nervous system imbalance, vasovagal episodes represent a tipping point of dysfunction. Restoring appropriate neural responses and cardiovascular control through conservative care opens the door to preventing recurrences.
What to Do When Your Child Has a Vasovagal Episode
When You Notice Warning Signs:
- Have them lie down flat immediately
- Elevate their legs above heart level
- Loosen tight clothing
- Keep them lying down for 15-30 minutes even after symptoms improve
- Stay calm and reassuring
During Loss of Consciousness:
- Guide them safely to the ground (don’t try to catch a falling child)
- Position on back with legs elevated
- Turn their head to the side if vomiting
- Don’t give anything by mouth while unconscious
- Time the episode’s duration
After Consciousness Returns:
- Keep lying down for 15-30 minutes minimum; standing too soon often triggers a second episode
- Offer water once fully alert
- Check for injuries
- Document triggers, warning signs, and duration
When to Seek Emergency Medical Evaluation
Call 911 or Go to the Emergency Room if:
- Loss of consciousness lasting more than 1-2 minutes
- Chest pain or difficulty breathing
- Irregular heartbeat (cardiac arrhythmias)
- An episode during physical exertion
- Significant injury from falling
- Repeated episodes without recovery between
- First-time episode with no clear trigger
- Family history of sudden cardiac death
After emergency medical evaluation rules out dangerous cardiac causes, many families discover that addressing the underlying nervous system dysfunction through Neurologically-Focused Chiropractic Care provides the missing piece. Visit our PX Docs directory to find a trained pediatric chiropractor.
Diagnosis and Testing Considerations
Since vasovagal seizures closely resemble certain epileptic seizures on the surface, correct diagnosis proves essential to selecting the appropriate care.
Conventional Diagnostic Testing
Medical evaluation typically includes:
Electrocardiogram (ECG): Monitors heart rhythm to detect arrhythmias. In vasovagal syncope, the ECG shows bradycardia or brief asystole, confirming a cardiovascular rather than a neurological origin.
Video-EEG/ECG monitoring: The gold-standard test shows simultaneous video, brain wave, and heart monitoring. This clearly shows that during vasovagal syncope, the EEG demonstrates slowing and flattening (oxygen deprivation response) rather than epileptic spike activity.
Tilt table testing: Reproduces vasovagal episodes in a controlled setting, challenging the Autonomic Nervous System’s ability to maintain blood pressure.
Distinguishing features include:
- Normal EEG findings in more than half of cases
- Changes in heart rhythm, blood pressure, or oxygen levels during episodes
- Absence of typical neurological conditions linked to seizures
- Situational triggers related to emotional distress, fatigue, and body positioning
Why Conventional Testing Often Misses the Root Cause
While these tests successfully identify THAT episodes are vasovagal rather than epileptic, they don’t reveal WHY the nervous system dysfunction exists.
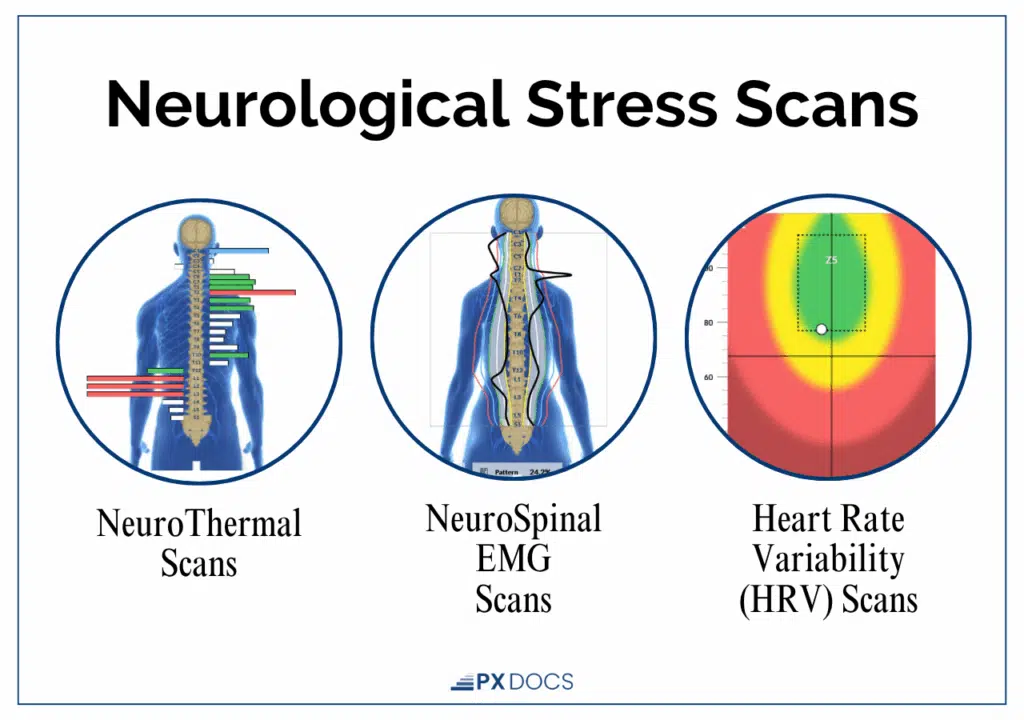
Advanced technologies, such as PX Docs’ INSiGHT Scans, assess and identify areas of subluxation contributing to abnormal sensorimotor processing. While conventional testing confirms vasovagal syncope, INSiGHT scans reveal the “Perfect Storm” factors—birth trauma, subluxation, and nervous system dysfunction—creating vulnerability to these episodes.
Tracking heart rate variability patterns also quantifies the severity of vagus nerve dysfunction, which guides appropriate management. By directly measuring nervous system dysfunction, the risk of misdiagnosis drops substantially, sparing children unnecessary medications.
The Limitations of Conventional Care
In mainstream medicine, anti-seizure medications such as Dilantin, Tegretol, Keppra, and Depakote are frontline interventions. However, designed to dampen electrical misfiring in the brain, these drugs fail to address the root causes of syncope-based seizures originating from cardiovascular miscommunication. Side effects like drowsiness, nausea, mood changes, and cognitive dulling often exacerbate the quality of life without halting convulsive episodes.
Surprisingly, as many as 20% of people diagnosed with epilepsy suffer from recurrent syncope, explaining why anti-seizure medications prove more harmful than helpful.
When the correct diagnosis is made, conventional care typically recommends lifestyle modifications:
- Increased hydration and salt intake
- Compression stockings
- Avoiding known triggers
- Position change strategies
- Regular exercise
These approaches can reduce episode frequency in mild cases and should be implemented. However, they don’t address why the nervous system remains hypersensitive to normal triggers. When episodes persist despite lifestyle changes, families need an approach that addresses the root neurological dysfunction.
The PX Docs Approach
Rather than overriding nervous system dysfunction with medication, the PX Docs approach identifies and addresses the root triggers of cardiovascular instability and nervous system dysregulation.
Each doctor in our PX Docs Network uses advanced INSiGHT scanning technology to accurately identify nervous system dysfunction and subluxation. These scans provide a “window” into the nervous system, enabling our doctors to pinpoint the exact location and type of subluxation—neurological dysfunction—and interference. This precise information allows doctors to create customized care plans and select specific adjusting techniques for optimal outcomes.
Neurologically-Focused Chiropractic Care works by removing subluxation at the upper cervical spine, where the vagus nerve exits the brainstem. When birth trauma or other “Perfect Storm” factors create neurological interference in this critical area, it disrupts communication pathways, affecting cardiovascular autonomic control.
This approach isn’t about “fixing” bones; it’s about restoring optimal neurological function and autonomic regulation. Gentle, specific adjustments remove interference in the nervous system’s communication pathways, allowing the vagus nerve to function properly and the autonomic nervous system to respond appropriately to triggers.
By addressing the neurological roots established by The Perfect Storm—rather than overriding them with medications or managing around them with lifestyle changes—Neurologically-Focused Pediatric Chiropractic Care offers the missing piece when conventional approaches fail.
As care progresses and INSiGHT scans show nervous system function improving, families typically observe a decrease in episode frequency and severity before symptoms fully resolve. This is inside-out healing—the nervous system regulates first, then symptoms improve as a result.
Restoring Hope and Quality of Life, Naturally
Witnessing a child endure violent convulsions, only to have doctors declare medications ineffective, drains hope and deepens confusion enormously.
At PX Docs, we recognize that these seizure-like presentations stem from nervous system imbalance, triggering shifts in blood flow, not brain misfires as with epileptic episodes. We’re committed to providing Neurologically-Focused Chiropractic Care that addresses the real root of the issue and restores healthy nervous system regulation.
Many children see significant improvement within the first few months of care, addressing nervous system dysfunction. While some children naturally outgrow vasovagal episodes, addressing the underlying neurological imbalance through Neurologically-Focused Chiropractic Care can accelerate this process and reduce episode frequency and severity during recovery.
The goal isn’t to “cure” vasovagal syncope—it’s to remove the neurological interference preventing your child’s body from regulating normally, allowing their innate healing capacity to restore proper autonomic function.If your child has been diagnosed with epilepsy yet medications have proven ineffective—or if you’ve received a vasovagal syncope diagnosis but want to address the underlying cause—consider contacting one of our qualified PX Docs. By visiting our PX Docs directory, you can find a Neurologically-Focused pediatric chiropractor who can develop a drug-free care plan tailored to your child’s needs.





