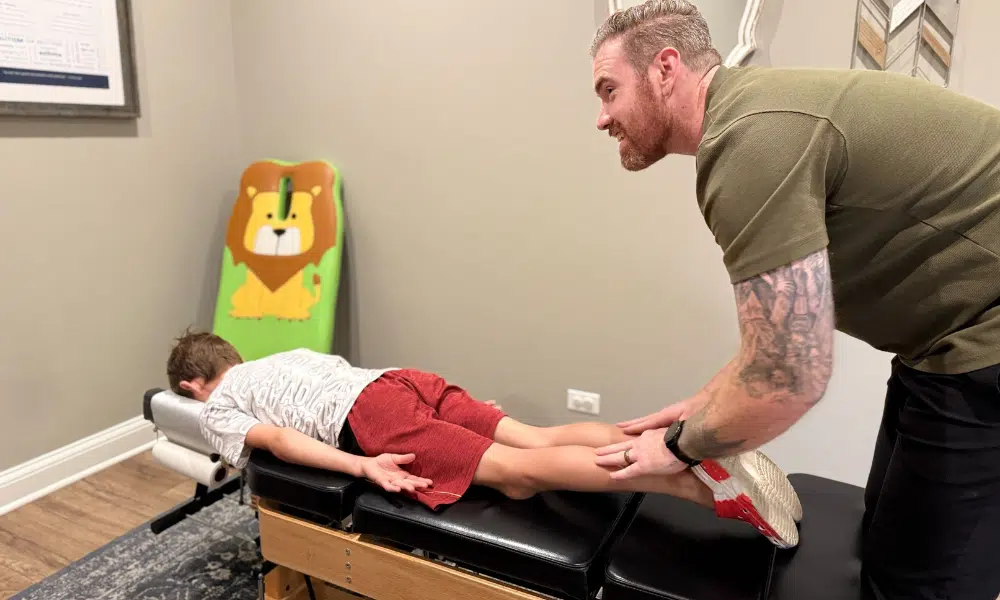
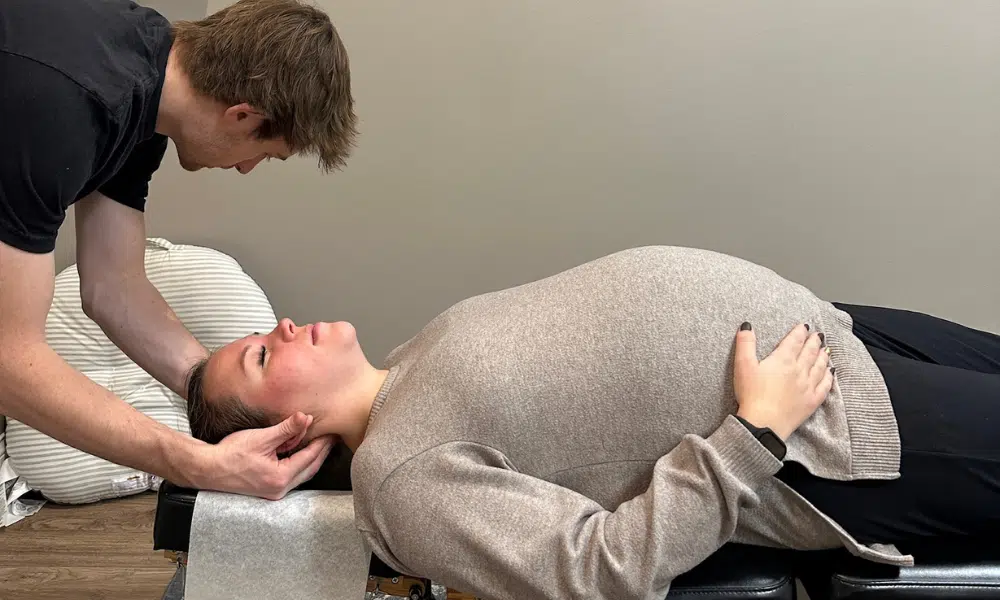
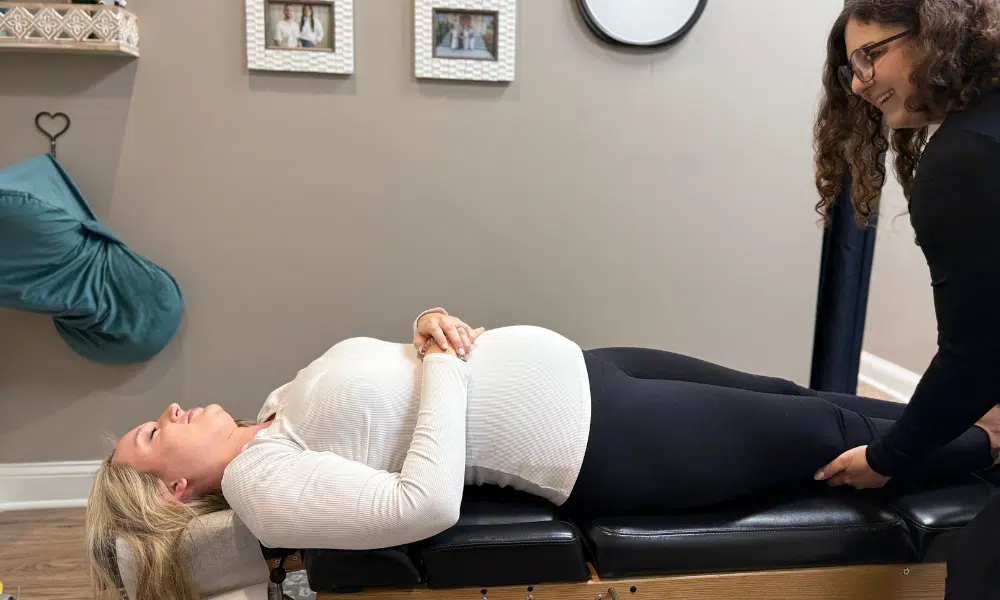
Preeclampsia is a serious pregnancy complication affecting 5-8% of pregnancies in the United States. It’s characterized by high blood pressure combined with signs of organ damage, typically developing after 20 weeks of pregnancy. With proper care, most women with preeclampsia deliver healthy babies and recover fully.
But you’re looking for more than the basics. You want to understand why this happens to some women and not others. While conventional medicine focuses on placental dysfunction, emerging research points to something deeper: nervous system dysregulation.
Your Autonomic Nervous System’s inability to adapt to the massive cardiovascular demands of pregnancy may be the root cause.
What Is Preeclampsia?
Preeclampsia is persistent high blood pressure (140/90 mm Hg or higher) after 20 weeks of pregnancy, combined with organ dysfunction. The diagnostic criteria no longer require protein in urine; doctors now recognize that preeclampsia can develop through kidney dysfunction, liver problems, severe headaches, visual disturbances, or low platelet counts.
The condition exists on a spectrum from mild to severe features (160/110 mm Hg or higher with significant organ involvement). It can also develop up to six weeks after delivery.
While these are diagnostic markers, preeclampsia represents something more fundamental: a systemic condition where your cardiovascular system, kidneys, liver, brain, and blood clotting mechanisms all show dysfunction simultaneously. Your Autonomic Nervous System is struggling to coordinate the massive adaptations pregnancy requires.
Preeclampsia affects 5-8% of US pregnancies—roughly one in 12-20 women. Rates have increased 25% over the last two decades. This rise points to environmental factors, increased maternal age, higher obesity rates, and critically, the accumulated stress load modern life places on women’s nervous systems.
Symptoms & Warning Signs
Many women have no symptoms. High blood pressure is often detected during routine prenatal visits before you feel anything wrong, which is why consistent prenatal care matters.
Common warning signs include:
- Severe headaches
- Vision changes including blurred vision, spots, or light sensitivity
- Upper abdominal pain under your ribs on the right side (from liver swelling)
- Sudden swelling of face, hands, or around the eyes (not normal foot swelling)
- Shortness of breath beyond typical pregnancy breathlessness
These signals indicate your body’s regulatory systems are under severe stress. Your nervous system is sending urgent signals that adaptation has failed. Seek immediate care for: persistent severe headaches with vision changes, chest pain, severe abdominal pain, nausea/vomiting in the second/third trimester, or decreased urination.
Listen, if your doctor keeps dismissing these signs, you need a second opinion fast. Preeclampsia can progress rapidly.
What Causes Preeclampsia?
Conventional medicine focuses on placental dysfunction. During early pregnancy, blood vessels in the uterine wall should widen dramatically to accommodate increased blood flow. In preeclampsia, this remodeling fails. Vessels stay narrow and stiff, reducing placental blood flow. The placenta responds by releasing factors that damage blood vessels throughout your body, causing inflammation, fluid leakage (swelling), and vasoconstriction (raised blood pressure).
But medicine struggles to answer: why do some women’s placentas develop problems while others don’t? And why do some women who develop preeclampsia have perfectly normal placentas?
The Nervous System Connection
Your Autonomic Nervous System, your body’s automatic control system, regulates blood pressure, blood vessel dilation, organ function, and inflammation. All of these malfunctions occur in preeclampsia.
Think of your nervous system like a car with two pedals: the sympathetic “gas pedal” that revs everything up, and the parasympathetic “brake pedal” that slows things down. Pregnancy requires your brake pedal to dominate. Your blood vessels need to relax and expand to accommodate 30-50% more blood volume. Your cardiac output must increase by up to 50%. These massive cardiovascular changes depend on parasympathetic activation, your body shifting into “grow and nurture” mode.
When chronic stress keeps your gas pedal stuck down, your body can’t make these adaptations. Your blood vessels stay constricted. Your stress response system (HPA axis) floods your body with cortisol that directly impairs blood vessel function and increases inflammation. Your cardiovascular system remains in protection mode when it needs to be in growth mode.
Research shows elevated maternal stress during pregnancy significantly increases preeclampsia risk by up to 20-fold. Women experiencing chronic stress show dysregulation in the same pathways that malfunction in preeclampsia: endothelial function, inflammatory responses, and cardiovascular adaptation.
I know how simple that sounds, but when you mess with the nervous system’s ability to regulate, you mess with everything downstream.
The Perfect Storm
Preeclampsia rarely develops out of nowhere. It’s typically the result of what we call the “Perfect Storm,” multiple stressors (prenatal stress, birth trauma, and environmental factors) accumulating before and during pregnancy, creating nervous system dysregulation that prevents adaptation.
The “Perfect Storm” often begins before conception. Fertility struggles, irregular cycles, birth control, hormonal imbalances—these are early warnings that your stress response system and reproductive system aren’t coordinating. These two systems can’t be simultaneously active.
When stress dominates, reproduction suffers.
Then pregnancy hits an already overwhelmed system. Life stressors compound biological demands. Pre-existing conditions like chronic hypertension, diabetes, or autoimmune conditions indicate your regulatory systems were already struggling. The accumulated stress overwhelms your adaptive capacity, and when pregnancy demands massive parasympathetic activation, your body can’t shift gears.
Risk Factors
High-risk factors:
- Previous preeclampsia (20% recurrence—your nervous system established a dysregulation pattern)
- Chronic hypertension (already dysregulated cardiovascular system)
- Chronic kidney disease, diabetes, and autoimmune conditions
- Multiple pregnancy (amplified demands)
Moderate-risk factors:
- First pregnancy, obesity (BMI 30+), family history
- Age 35+ or under 20
- IVF pregnancy
- 10+ years since last pregnancy
The Overlooked Risk: Chronic Stress
Here’s what medicine is starting to recognize: maternal stress during pregnancy increases preeclampsia risk. This isn’t about occasional anxiety. This is a chronic stress response activation that biologically prevents adaptation.
Chronic cortisol elevation directly affects blood vessel function, increases vascular resistance, promotes inflammation, and interferes with placental blood vessel development. The body’s perception of threat triggers the same sympathetic response that makes pregnancy adaptation impossible.
Complications
- Maternal: Eclampsia (seizures), HELLP syndrome (liver/blood condition), organ damage, stroke, placental abruption, pulmonary edema. Long-term cardiovascular disease risk doubles.
- Baby: Fetal growth restriction, preterm birth, low birth weight, placental abruption, stillbirth (rare with monitoring).
The Hidden Impact: Fetal Programming
Here’s what no one’s talking about: what happens during pregnancy programs your baby’s developing nervous system.
When you experience preeclampsia, stress hormones cross the placenta and affect your baby’s developing brain. Research published in Frontiers found that babies exposed to high maternal stress show higher stress reactivity and a dysregulated Autonomic Nervous System. Clinically, this looks like higher rates of colic in infancy, increased sensory sensitivities in toddlerhood, and elevated risk of Anxiety, ADHD, and Sensory Processing Disorder in childhood.
This fetal programming sets the foundation for your child’s own “Perfect Storm.” Understanding this empowers you to support your child’s nervous system development from birth forward.
The Nervous System Regulation Approach
This is where we get proactive instead of reactive. Instead of waiting to see if preeclampsia develops, we can support your nervous system’s ability to regulate before pregnancy begins.
Neurologically-Focused Chiropractic Care focuses on correcting subluxation, a neurological dysfunction that interferes with your nervous system’s ability to communicate and regulate. This isn’t about moving bones, relaxing muscles, or helping ligaments. This is neurological care that removes interference, allowing your body to function as designed.
Neurological INSiGHT scans provide objective measurements of nervous system stress patterns and autonomic imbalance. You can see areas of stress shift to regulated as your nervous system heals.
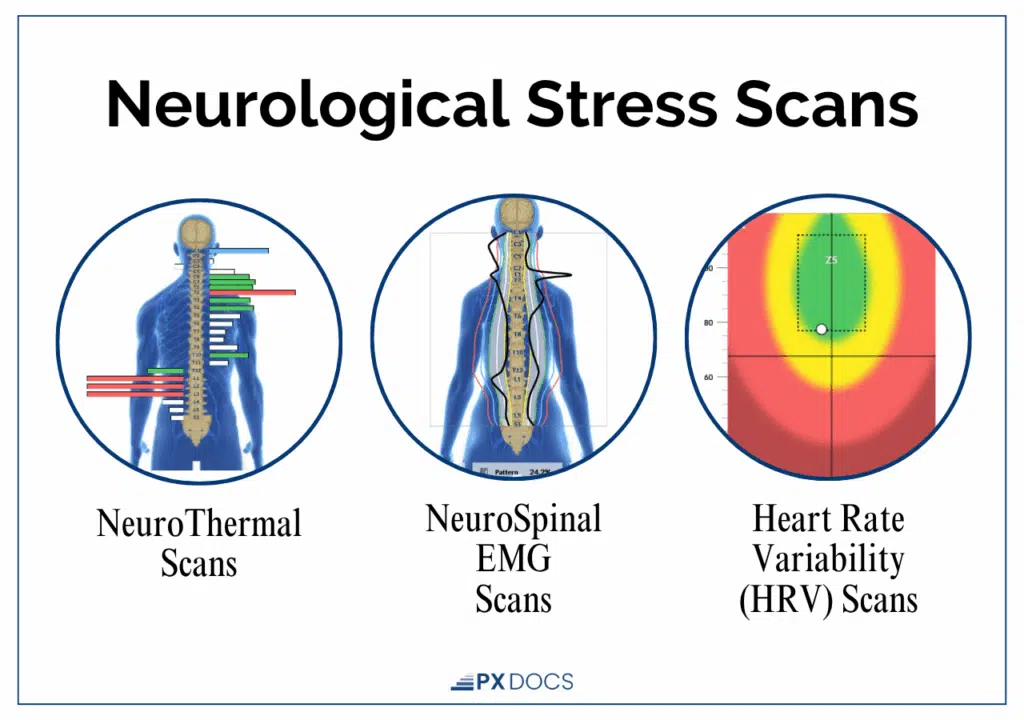
The ideal timeframe is preconception through postpartum and beyond. Supporting regulation before pregnancy allows you to enter with optimal adaptive capacity. This works alongside medical care, not instead of it.
Now, obviously, we can’t control everything, but we can control how our nervous system adapts to stress during preconception, pregnancy, and birth. So even if preeclampsia is a part of your story, how will you and your baby adapt and recover? What are the gentle, least invasive steps you can discuss with your provider for preeclampsia and induction?
- Prostaglandins
- Pumping
- Membrane Sweeps
- Foley Bulb Induction (Cervical Balloon)
A New Understanding of Preeclampsia
Preeclampsia is serious, but understanding root causes empowers prevention. Medical monitoring and care remain essential; blood pressure control, seizure prevention, and appropriate delivery timing save lives.
But we now understand something deeper: preeclampsia represents nervous system dysregulation that can show up as cardiovascular signs. Your Autonomic Nervous System’s inability to shift from sympathetic dominance to parasympathetic activation prevents the adaptations pregnancy requires.

This understanding opens new possibilities. Both you and your baby benefit from balanced autonomic function. Early intervention, supporting nervous system regulation before or during pregnancy, can change outcomes. Find a PX Docs practitioner near you to get evaluated and begin supporting your nervous system’s optimal function. Your body was designed for this. Sometimes it just needs the right support to remember how.