Strabismus in children is one of the most common eye conditions in childhood, affecting roughly 2 to 4 percent of children under the age of six. Left unaddressed, it can lead to amblyopia (often called “lazy eye”), loss of depth perception, and long-term challenges with vision, learning, and even self-confidence.
PX Docs have spent years helping parents understand that many childhood challenges, including those affecting vision and eye coordination, have roots that extend beyond the eye itself. In this article, we’ll walk you through everything you need to know about strabismus in children, from the conventional basics to the neurological connections that most parents and even many providers overlook.
What Is Strabismus?
Strabismus is when the eyes aren’t properly aligned. Instead of both eyes pointing at the same object at the same time, one eye may turn in a different direction, inward, outward, upward, or downward, while the other stays focused straight ahead.
This misalignment can be constant or intermittent. Some children have eyes that cross all the time, while others only show misalignment when they’re tired, sick, or focusing on something up close. The affected eye can also switch; sometimes the right eye drifts, sometimes the left.
Here’s why this matters so much for your child’s development: when both eyes are aligned, the brain receives two slightly different images and merges them into a single three-dimensional picture. That’s how we perceive depth and distance. But when strabismus is present, each eye sends a different image to the brain. In young children, the brain often responds by ignoring the input from the misaligned eye entirely, and that’s how amblyopia develops.
The earlier strabismus is identified and addressed, the better the outcomes. The brain’s visual pathways develop rapidly during the first several years of life, and early intervention gives your child the best chance of developing strong binocular vision.
Types of Strabismus in Children
Not all strabismus looks the same. Understanding the different types can help you communicate more clearly with your child’s eye care provider and better understand what you’re seeing at home.
- Exotropia is when one eye drifts outward, away from the nose. This type is often intermittent at first; you might notice it when your child is daydreaming, tired, or looking at something far away. Over time, intermittent exotropia can become more frequent and eventually constant if left unaddressed.
- Hypertropia and hypotropia involve vertical misalignment, one eye sitting higher or lower than the other. These are less common but can be associated with cranial nerve dysfunction, particularly involving the fourth cranial nerve (trochlear nerve).
- Esotropia is the most common form of strabismus in young children. This is when one or both eyes turn inward toward the nose, which most people think of as “crossed eyes.” Congenital (infantile) esotropia typically appears within the first six months of life and often requires early intervention. Accommodative esotropia, on the other hand, usually appears between ages 2 and 3 and is associated with farsightedness. In this type, the child’s eyes cross because they’re working extra hard to focus.
Each type of strabismus can have different underlying causes and may require different care approaches. That’s why a thorough evaluation isn’t just helpful, it’s essential.
What Causes Strabismus in Children?
This is where the conventional conversation usually gets pretty surface-level. Most medical sources will tell you the exact cause is “unknown” in many cases, or they’ll list a handful of risk factors and leave it at that.
Let’s go deeper.
Six muscles attach to each eye and control its movement. These muscles are directed by three specific cranial nerves:
- The oculomotor nerve (cranial nerve III)
- The trochlear nerve (cranial nerve IV)
- The abducens nerve (cranial nerve VI).
All three of these nerves originate in the brainstem. For your child’s eyes to move together smoothly and stay aligned, these nerves need to send accurate, coordinated signals to the eye muscles.
When the brain and brainstem aren’t communicating efficiently with the eye muscles, misalignment can result, and that’s strabismus at its core. It’s often a neurological coordination issue, not just an eye problem.
The recognized causes and risk factors for strabismus in children include:
- Refractive errors, particularly farsightedness (hyperopia), which forces the eyes to strain and can pull them out of alignment
- Family history, children with a parent or sibling who has strabismus are at significantly higher risk
- Prematurity and low birth weight, research published in JAMA Pediatrics found that premature infants weighing under 2,000 grams at birth had a 61% increased risk of developing strabismus
- Neurological conditions such as cerebral palsy, Down syndrome, and hydrocephalus
- Birth trauma and birth interventions, including cesarean delivery and neonatal intensive care stays, have been connected to increased strabismus risk
- Eye injuries or cataracts that disrupt normal visual development
- Central nervous system abnormalities that affect how cranial nerves develop and function
What’s striking about this list is how many of these risk factors are neurological in nature. Prematurity, birth trauma, and neurological conditions aren’t just eye issues. They’re nervous system issues that happen to show up in the eyes.
Signs and Symptoms
Strabismus isn’t always obvious, especially in mild or intermittent cases. Watch for:
- Eyes that visibly don’t line up
- Head tilting or turning to compensate
- Squinting or closing one eye (especially in bright light)
- In older children, complaints of double vision, headaches, or difficulty reading
An important note: some babies appear to have crossed eyes when they actually don’t. This is called pseudostrabismus, and it typically happens because of a wide, flat nasal bridge or extra skin folds near the inner eyelid. True strabismus doesn’t resolve on its own; it needs professional evaluation.
If your baby’s eyes are still crossing or wandering after 4 to 6 months of age, or if you notice any of these signs at any point in childhood, get a comprehensive eye exam with a pediatric ophthalmologist.
How Strabismus Affects Your Child’s Development
Strabismus isn’t just a cosmetic concern; it can have real consequences for your child’s visual development, learning, and emotional well-being.
When one eye is misaligned, the brain receives conflicting information. In young children, the brain often resolves this conflict by suppressing the image from the weaker eye. Over time, this leads to amblyopia, a condition where one eye develops significantly weaker vision because the brain has essentially stopped using it. Research suggests that up to 50% of children with unaddressed strabismus develop some degree of amblyopia.
Beyond vision loss, strabismus affects depth perception, your child’s ability to judge how far away objects are. This impacts everything from catching a ball to pouring a glass of water to navigating stairs safely.
There’s also a significant psychosocial impact. Studies have found that children with noticeable strabismus often experience higher levels of anxiety, social inhibition, and difficulty with peer relationships. The emotional toll is real, and it’s something parents should take seriously.
For children who develop strabismus after age 6, the consequences can be different; double vision becomes more likely because the brain has already developed the habit of using both eyes.
The Nervous System Connection
Here’s where things get interesting, and where PX Docs brings a perspective that most sources on strabismus simply don’t offer.
Remember those three cranial nerves we talked about? The oculomotor, trochlear, and abducens nerves all originate in the brainstem, the same area of the nervous system that controls breathing, heart rate, digestion, sleep cycles, and overall neurological regulation. The brainstem is essentially the body’s “air traffic control center,” coordinating communication between the brain and the rest of the body.
When the brainstem and upper cervical region experience stress or dysfunction, whether from birth trauma, prenatal stress, or other early-life challenges, the effects can ripple outward in ways that most providers don’t connect back to the source. Eye coordination issues are just one potential expression of that broader neurological dysfunction.
Think about it this way: the same nervous system pathways that control eye muscle coordination also influence motor tone and development, vestibular function and balance, sensory processing, and overall nervous system regulation. Many children with strabismus also show signs of challenges in these other areas, and that’s not a coincidence. It’s a pattern.
The “Perfect Storm”: Understanding the Root Causes
At PX Docs, we talk about The Perfect Storm, a concept that explains how multiple early-life stressors can accumulate and interact to overwhelm a child’s developing nervous system, leading to dysfunction that shows up in many different ways.
The three core components of The Perfect Storm include:
Prenatal stress and maternal health challenges. When a mother experiences significant stress during pregnancy, whether from fertility challenges, anxiety, illness, or environmental factors, elevated stress hormones like cortisol can cross the placenta and impact the developing fetal nervous system. This can affect the development of cranial nerves and brainstem structures during those critical growth windows.
Birth interventions and trauma. Procedures like C-sections, vacuum extraction, forceps delivery, and prolonged labor can create physical stress on the infant’s delicate brainstem and upper cervical spine. The upper neck region is where the brainstem transitions into the spinal cord, and it’s also where the cranial nerves that control eye movement originate and exit. Even “routine” birth interventions can create tension and dysfunction in this area.
Research backs this up. Studies have found that cesarean delivery and neonatal intensive care stays are associated with increased strabismus risk, and low birth weight, often a marker of prenatal stress and challenging delivery, is independently linked to a higher risk of developing strabismus.
Early childhood stressors. After birth, factors like chronic illness, antibiotic use, environmental toxins, and other stressors continue to compound. When the nervous system is already operating from a place of dysfunction, these additional challenges further disrupt its ability to regulate and coordinate, including the precise cranial nerve signaling required for proper eye alignment.
The sum of these stressors creates what we call subluxation, not just a structural misalignment, but a neurological interference pattern involving misalignment, fixation, and disrupted nervous system communication. This interference can affect how the brainstem communicates with the cranial nerves that control eye movement, contributing to the coordination problems we see in strabismus.
Subluxation, Dysautonomia, and Eye Coordination
When subluxation is present in the upper cervical and brainstem regions, it creates dysautonomia, an imbalance in the Autonomic Nervous System. Think of it like the “gas pedal” (Sympathetic Nervous System) being stuck on while the “brake pedal” (Parasympathetic Nervous System) can’t do its job.
This autonomic imbalance doesn’t just affect one system; it affects everything the nervous system controls. Digestion, immune function, sleep, emotional regulation, motor coordination, and yes, cranial nerve function.
The vagus nerve, the longest cranial nerve in the body, plays a central role in this picture. It exits through the jugular foramen at the base of the skull, travels alongside the very brainstem structures that house the motor nuclei for cranial nerves III, IV, and VI. When there’s dysfunction in this area, it rarely affects just one system in isolation.
This is why so many children with strabismus also experience other challenges that seem unrelated on the surface, such as sensory processing difficulties, motor delays, digestive issues, sleep problems, or difficulty with focus and attention. They’re not separate problems. They’re different expressions of the same underlying nervous system dysregulation.
How INSiGHT Scans Provide Clarity for Families
This is where our INSiGHT scanning technology becomes so valuable for parents seeking answers. It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for strabismus or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
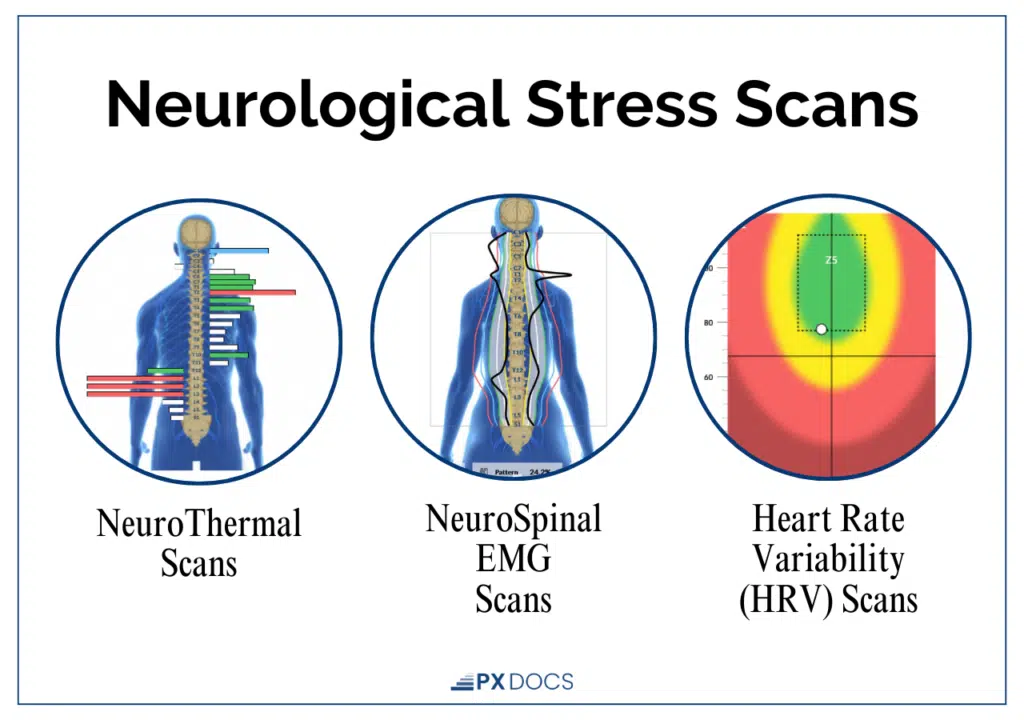
INSiGHT Scans include three primary components:
- Heart Rate Variability (HRV) Analysis measures the balance between the sympathetic (“fight-or-flight”) and parasympathetic (“rest, regulate, and digest”) branches of the Autonomic Nervous System. This tells us whether a child’s nervous system is stuck in overdrive or if it has the flexibility to adapt and regulate.
- Surface Electromyography (sEMG) assesses the electrical activity of muscles along the spine, identifying areas of tension and altered neuromuscular function. This is particularly relevant for children with strabismus because it can reveal patterns of tension and dysfunction in the upper cervical region, right where those critical cranial nerve pathways originate.
- Thermal Scanning uses infrared sensors to measure temperature differences along the spine, which can indicate areas of dysautonomia and autonomic imbalance.
What makes these scans especially powerful is their ability to detect changes in neurological function before they show up as visible improvements. Think of it like a weather radar detecting clear skies forming on the horizon, even though the storm hasn’t fully passed overhead yet.
For parents of children with strabismus, these scans can reveal whether there’s an underlying pattern of nervous system dysfunction that could be contributing to their child’s eye coordination challenges, information that standard eye exams simply don’t provide.
Working With Your Child’s Full Care Team
At PX Docs, we believe in supporting the whole child. That means we’re not asking you to choose between conventional eye care and a neurological approach; we’re encouraging you to consider both.
Your child’s pediatric ophthalmologist plays a critical role in monitoring eye alignment, prescribing corrective lenses, managing amblyopia, and determining whether surgery is needed. Those are important pieces of the puzzle.
But if your child’s strabismus is connected to a deeper pattern of nervous system dysfunction, especially if you recognize elements of “The Perfect Storm” in their history, then addressing the neurological root causes can support their overall development in ways that eye-focused care alone cannot.
Neurologically-Focused Chiropractic Care focuses on identifying and addressing subluxation in the upper cervical and brainstem region. Gentle, precise adjustments are designed to restore proper communication between the brain, brainstem, and the rest of the body, including the cranial nerves that coordinate eye movement.
Many parents notice that as their child’s overall nervous system function improves, they see positive changes across multiple areas, not just in eye coordination, but in sleep, digestion, behavior, and motor development. That’s because the nervous system controls and coordinates everything.
When to Seek Urgent Evaluation
While most strabismus in children is not an emergency, certain situations warrant immediate medical attention. If your child develops sudden eye misalignment, especially after age 6, it could be a sign of a more serious underlying condition that needs prompt evaluation. Sudden onset strabismus accompanied by headache, vomiting, or changes in consciousness should be evaluated immediately.
Any child with strabismus should be assessed by a pediatric ophthalmologist to rule out conditions like retinoblastoma (a childhood eye tumor) or other structural problems. Always consult with your child’s healthcare provider about any concerns regarding their vision or eye alignment.
Your Child’s Eyes Tell a Story About Their Nervous System
Strabismus in children is common and treatable, and early care—whether through glasses, patching, surgery, or a combination of approaches—can protect your child’s vision and support healthy visual development. But many parents still wonder if there’s more to the story, especially when eye coordination issues appear alongside other signs of nervous system stress.
The eyes don’t work in isolation. The cranial nerves that control eye movement originate in the brainstem, which is closely connected to the overall balance and function of the nervous system. Because of this, challenges with eye coordination can sometimes reflect deeper neurological patterns. For families who suspect there may be more going on, exploring the nervous system side of the picture can be an important next step. If you’d like to learn more about how Neurologically-Focused Chiropractic Care may support your child’s nervous system and development, you can visit the PX Docs Directory to find a qualified practitioner near you.