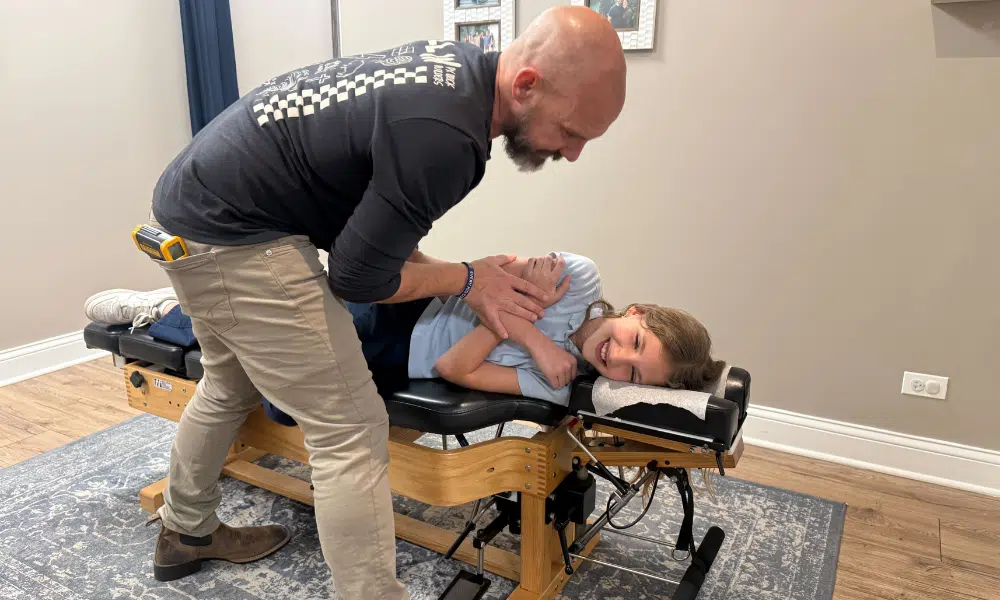
As a parent, you’ve likely found yourself in this situation: Your child is sick, and the pediatrician prescribes antibiotics. You know these medications can help fight bacterial infections, but you can’t help wondering about potential side effects. Will your child experience an upset stomach? Can antibiotics cause constipation?
You’re not alone in these concerns.
Children in the U.S. are prescribed an average of 1-2 antibiotics each year. While antibiotic-associated diarrhea affects approximately 21% of children, constipation, though less common, still occurs in about 8% of children taking these medications.
While these medications can be lifesavers, they often come with unintended consequences for your child’s delicate digestive system. We’ll explain the connection between antibiotics and constipation in children, why the conventional approach often falls short, and what you can do to support your child’s health during and after care.
What Are Antibiotics and How Do They Work?
Antibiotics are powerful medications designed to fight bacterial infections by killing bacteria or preventing them from reproducing. They work by disrupting bacterial cell walls, interfering with protein synthesis, or blocking reproduction processes.
These medications fall into two main categories: broad-spectrum antibiotics (affecting a wide range of bacteria) versus narrow-spectrum antibiotics (targeting specific types). Broad-spectrum antibiotics cast the widest net, making them effective against many infections, but also posing the greatest risk to your child’s beneficial gut bacteria.
Here’s the catch: Antibiotics can’t distinguish between “bad” bacteria causing an infection and “good” bacteria essential for your child’s health.
The most commonly prescribed pediatric antibiotics include:
- Amoxicillin (Amoxil) – Often the first choice for ear infections and strep throat
- Amoxicillin-Clavulanate (Augmentin) – Broad-spectrum for resistant infections
- Azithromycin (Z-pack) – Popular for respiratory infections
- Cephalosporins (Cefdinir, Cephalexin) – Used for UTIs and skin infections
- Clindamycin – Highest risk for gut disruption, used for skin and dental infections
The broader the spectrum and the longer the course, the greater the impact on your child’s delicate gut microbiome.
The Gut Microbiome: A Delicate Ecosystem
Your child’s digestive system is home to trillions of microscopic inhabitants, bacteria, viruses, and fungi comprising 300 to 500 different bacterial species, collectively known as the gut microbiome.
This microscopic community influences far more than just digestion:
- Immune system function (70-80% of immune cells reside in the gut)
- Brain health and behavior via the gut-brain axis
- Metabolism and weight regulation
- Mood and mental health
- Inflammation throughout the body
Research indicates that up to 40% of your child’s stool volume consists of bacteria. When antibiotics kill these beneficial microorganisms, digestive function can change dramatically.
This disruption can lead to dysbiosis, an imbalance where harmful bacteria or yeast may overgrow while beneficial species are depleted.
From a PX Docs perspective, the gut microbiome is intricately linked to nervous system function through the gut-brain axis. When antibiotics disrupt this ecosystem, it can impact more than digestion; it can affect your child’s nervous system function, behavior, and overall well-being.
Do Antibiotics Cause Constipation?
While antibiotic-associated diarrhea is more common, antibiotics can indeed cause constipation. One study found that an upset stomach after antibiotics occurred in 9.3% of children, and constipation resulted in 8%.
Here’s how antibiotics lead to constipation:
- Disruption of gut microbiome: Antibiotics kill beneficial bacteria crucial for maintaining regular bowel movements. These bacteria produce compounds that stimulate intestinal contractions and maintain proper stool consistency.
- Dehydration: Some antibiotics cause nausea and decrease fluid intake. When your child isn’t drinking enough, their colon absorbs more water from the stool, making it harder and more difficult to pass.
- Changes in gut motility: Antibiotics can affect intestinal muscles, potentially slowing the movement of stool through the digestive tract. This means food waste sits longer in the colon, becoming increasingly dehydrated.
- Nervous system impact: Antibiotics can affect the nervous system, potentially leading to dysregulation—a condition where the Autonomic Nervous System doesn’t function properly. This can impact digestive processes and contribute to constipation.
Understanding C. Diff Infection Risk
While focusing on constipation, it’s critical to understand a serious complication: Clostridioides difficile (C. diff) infection. C. diff can overgrow when antibiotics kill off beneficial gut bacteria that normally keep it in check.
Children taking broad-spectrum antibiotics face elevated risk, particularly with clindamycin (highest risk), fluoroquinolones, cephalosporins, and prolonged amoxicillin courses.
Warning signs include:
- Severe watery diarrhea (often 10+ times daily)
- Fever and loss of appetite
- Belly pain or tenderness
- Blood or mucus in stool
C. diff infection can be life-threatening and requires immediate medical attention. If your child develops severe diarrhea during or within several weeks after taking antibiotics, contact your pediatrician right away.
The Neurological Connection: Beyond the Gut
At PX Docs, we recognize a crucial player often overlooked: nervous system regulation. The nervous system, particularly the Autonomic Nervous System, plays a vital role in regulating digestive processes.
The vagus nerve, the longest cranial nerve in your body, serves as the primary communication highway between your child’s brainstem and digestive system. It controls everything from stomach acid production to intestinal contractions to the valve that controls bowel movements. When vagus nerve function is compromised—what we identify as vagus nerve dysfunction—digestive processes, including gut motility, can slow significantly.
In chiropractic terms, subluxation refers to misalignments that can interfere with proper nervous system function. When nervous system function is dysregulated, children often experience digestive challenges, including:
- Slowed gut motility
- Decreased digestive enzyme production
- Impaired nutrient absorption
- Altered gut microbiome balance
Antibiotics increase systemic inflammation throughout the body. This inflammatory response can further stress an already dysregulated nervous system, potentially worsening the communication breakdown between the brain and gut.
“The Perfect Storm”: Compounding Factors
At PX Docs, we refer to “The Perfect Storm” when discussing how various factors, including antibiotic use, converge to create broader health issues. This storm often begins before birth:
- Prenatal and Early Life Stress: High maternal stress during pregnancy can affect fetal nervous system development, including the vagus nerve, which won’t fully mature until your child is several years old.
- Birth Method: Babies born via C-section have significantly different gut bacteria than those born vaginally, missing the initial “seeding” of beneficial bacteria from the birth canal.
- Birth Interventions: Procedures like C-sections, vacuum extraction, or forceps can cause physical trauma to delicate neck structures and impact nervous system function, affecting the vagus nerve’s ability to coordinate digestion.
- Repeated Antibiotic Use: Each course depletes beneficial bacteria while allowing opportunistic organisms to gain ground, especially critical in the first few years of life.
This framework explains why some children take one course of antibiotics and bounce back quickly, while others struggle for weeks or develop a pattern of repeated infections. It’s about the individual stress load on their nervous system.
Natural Ways to Support Gut Health
While our chiropractic approach forms the cornerstone of care, here are ways to support your child’s gut health at home:
- Probiotic Supplementation: Consider a high-quality probiotic containing Lactobacillus and Bifidobacterium species during and after care. There are mixed results, but many parents report improvements, and the safety profile is excellent.
- Prebiotic Fiber: Feed the bacteria already in your child’s gut with bananas, asparagus, onions, garlic, oats, apples, and legumes.
- Fermented Foods: Plain yogurt with live cultures, kefir, and age-appropriate fermented foods provide natural probiotics.
- Fiber-Rich Foods: Focus on both soluble fiber (oats, pears, apples, beans, sweet potatoes) and insoluble fiber (whole grains, carrots, broccoli, leafy greens). Aim for your child’s age + 5 grams of fiber daily.
- Hydration: Children need approximately half their body weight in ounces of water daily.
- Movement: Regular physical activity stimulates digestion and promotes bowel regularity.
The Missing Piece: These strategies address symptoms and support gut restoration; they’re important first steps. However, if your child has tried all of these approaches and still experiences irregular bowel movements, it’s time to look deeper at nervous system function.
Timeline: When Constipation Starts and How Long It Lasts
- During Care Plan (Days 1-10): Constipation typically becomes noticeable around the third to seventh day of care. Bowel movements may decrease in frequency, and stools may become harder and more difficult to pass.
- After Care Plan (Weeks 1-4): Symptoms often persist even after finishing antibiotics. With dietary support, probiotics, proper hydration, and movement, most children see gradual improvement during weeks 2-4.
- Full Recovery (1-3 Months): While constipation signs typically resolve within a month, full gut flora restoration can take weeks to several months, depending on antibiotic type, care plan length, your child’s age, and underlying nervous system function.
- Beyond 3 Months: If constipation persists beyond 4-6 weeks despite following all recommendations, this suggests an underlying issue beyond temporary microbiome disruption. This is where our neurological approach becomes particularly relevant.
When to Call Your Pediatrician
Call if:
- Constipation lasts more than 3 days without improvement
- Severe abdominal pain or bloating
- Blood in stool
- Inability to pass gas
- Vomiting alongside constipation
- Fever developing during or after care
- Signs of dehydration
Seek immediate attention for:
- Severe watery diarrhea (10+ times daily—possible C. diff)
- High fever above 102°F
- Extreme abdominal pain
- Bloody or black stools
A Drug-Free, Neurologically-Focused Path Forward
Antibiotic-induced constipation is more than just a digestive issue—it’s often revealing broader imbalances in the nervous system.
The difference between a child who recovers quickly and one who struggles for weeks often comes down to nervous system resilience. It’s about whether their vagus nerve can coordinate the complex digestive processes needed for normal bowel function. It’s about whether their body can shift from “fight or flight” stress mode into “rest and digest” healing mode.
Using INSiGHT scanning technology, we can objectively measure nervous system function—something conventional medicine doesn’t assess. These scans show us whether your child’s Autonomic Nervous System is stuck in a dysregulated state, preventing proper digestion, and they guide a personalized care plan tailored to your child’s specific nervous system needs.
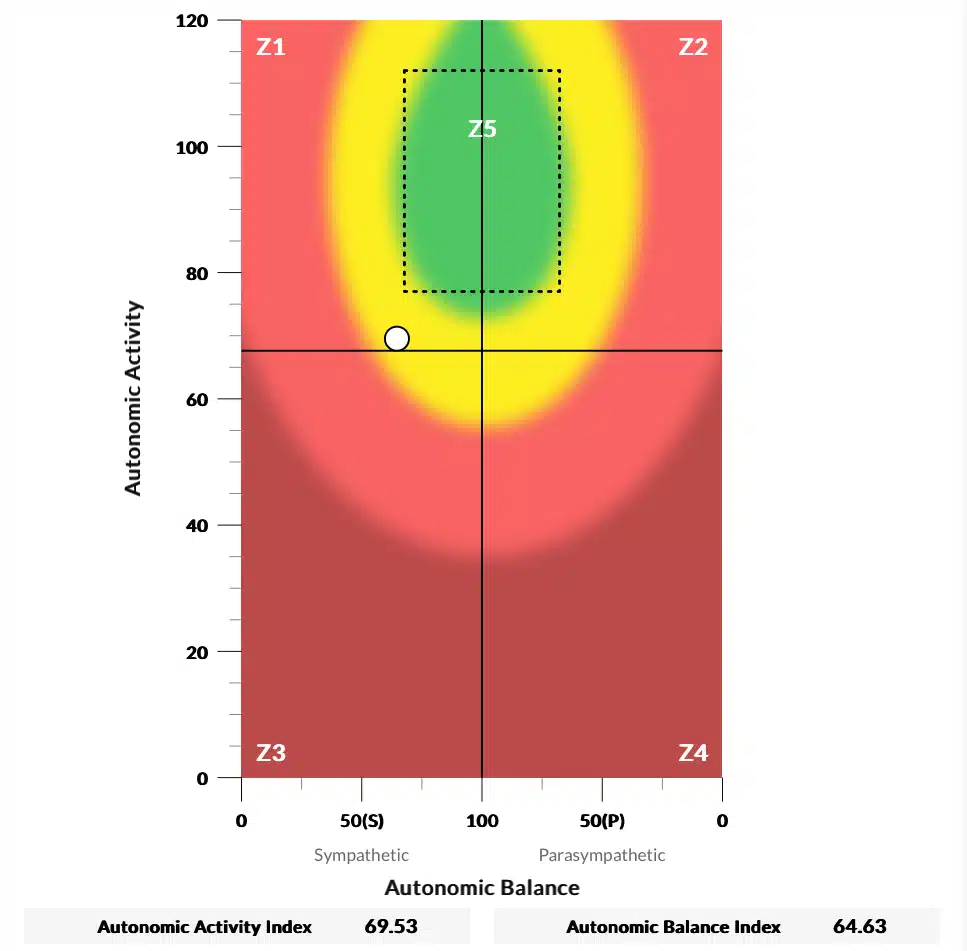
Your child’s struggles with constipation after antibiotics aren’t just “bad luck” or something they need to outgrow. There’s a root cause, and there’s a path forward.
If your child is struggling with constipation or other digestive issues during or after antibiotic use, we encourage you to visit the PX Docs directory to find a PX Doc in your area for a comprehensive evaluation and personalized care plan. Together, we can support your child’s journey toward optimal health and well-being.