If you’re pregnant and concerned about autism risk, you’re not alone. With Autism Spectrum Disorder now affecting 1 in 31 children, many expectant parents search for answers about the signs of autism during pregnancy.
Here’s the truth: there’s no definitive test that can diagnose autism before birth.
But you’re not left in the dark. Research has identified specific risk factors and prenatal indicators that help you understand your child’s risk profile. More importantly, there’s a lot you can do about it.
What most doctors won’t tell you is that autism doesn’t just “happen” at age two. The neurological foundation begins much earlier, often during pregnancy itself. Understanding these early warning signs and the nervous system factors behind them empowers you to take proactive steps from day one.
Can Autism Be Diagnosed During Pregnancy?
No, autism cannot be definitively diagnosed during pregnancy. Most children receive an autism diagnosis between ages 3 and 4, when behavioral patterns and developmental delays become apparent.
Autism isn’t a condition you can see on a genetic test. It’s a complex neurodevelopmental pattern that unfolds as the nervous system develops. The behavioral signs we associate with autism are actually the end result of neurological patterns that begin forming much earlier.
Recent research has identified interesting patterns. A groundbreaking study found that routine second-trimester ultrasounds can reveal subtle anatomical differences in fetuses who later develop autism. Researchers discovered specific variations in the head, heart, and kidneys in approximately 30% of fetuses later diagnosed with autism, three times higher than the general population.
The severity of these anatomical differences seemed to correlate with the severity of autism signs later. Other studies using fetal MRI have identified differences in brain structures like the amygdala and insula in babies who develop autism.
While these findings don’t provide a yes-or-no answer, they tell us something important: autism has neurological roots that begin forming before birth. That means there may be ways to support optimal nervous system development starting during pregnancy.
Understanding Autism as a Nervous System Condition
Most conventional approaches view autism primarily as a genetic brain condition. While genetics play a role, this perspective misses something critical: autism is fundamentally a condition of nervous system dysfunction.
Think about autism’s core features. Children with autism struggle with sensory processing, social communication, and reading emotional cues. Many experience digestive issues, sleep problems, and motor coordination challenges. Their immune systems often don’t function optimally.
What do these signs have in common? They’re all controlled by the nervous system, specifically, the vagus nerve.
The vagus nerve is the longest cranial nerve, running from the brainstem through the neck into the chest and abdomen. It’s the master regulator of the Autonomic Nervous System, controlling digestion, heart rate, immune response, sensory processing, emotional regulation, sleep cycles, and motor coordination.
When the vagus nerve and autonomic function are disrupted, a condition called dysautonomia, you see exactly the pattern of challenges that define autism. These aren’t separate signs. They’re all signs that the nervous system isn’t properly regulating critical functions.
This is what makes autism a body-based condition that affects the brain, rather than purely a brain-based condition. As we say at PX Docs: “It begins in the body, ends up in the brain.”
When a child’s nervous system is stuck in sympathetic dominance or “fight-or-flight” mode, their body can’t properly handle sensory information, regulate emotions, digest food, or develop communication skills. The gas pedal is stuck down, and the brake pedal (the Parasympathetic Nervous System controlled by the vagus nerve) isn’t working.
The “Perfect Storm”: How Autism Risk Builds During Pregnancy
Autism rarely develops from one single factor. Instead, it typically develops through what we call The “Perfect Storm,” a convergence of multiple factors that accumulate and overwhelm the developing nervous system during vulnerable windows.
This “Perfect Storm” often begins before birth.
Prenatal Stress and the Electrical Connection
Your umbilical cord doesn’t just deliver nutrients; it’s an electrical connection between your nervous system and your baby’s. When you experience prenatal stress, stress hormones like cortisol cross the placenta and affect your baby’s developing nervous system.
If you’re experiencing chronic stress, anxiety, or trauma during pregnancy, your baby’s nervous system is being ‘bathed’ in stress hormones during its most critical developmental period. Their nervous system learns this stressed state is “normal.” They’re being programmed for sympathetic dominance before birth.
Research backs this up. Studies have found that high levels of maternal psychological distress during pregnancy are associated with altered fetal brain development and increased neurodevelopmental risk. After natural disasters, children born to mothers who experienced significant stress show higher autism rates, even when genetics and nutrition are the same.
Maternal Health Conditions
Several maternal conditions during pregnancy are linked to increased autism risk:
- Gestational diabetes creates metabolic instability and inflammation, affecting fetal development. Research shows gestational hyperglycemia can suppress important proteins involved in brain development and create persistent oxidative stress.
- Maternal obesity is associated with chronic systemic inflammation and altered metabolism, both of which affect the intrauterine environment.
- Autoimmune conditions are characterized by chronically activated immune systems. Inflammatory molecules called cytokines can cross the placenta and affect the baby’s developing brain. Mothers of children with autism often have elevated C-reactive protein (an inflammation marker) during pregnancy.
Environmental Exposures
Air pollution exposure during pregnancy, particularly fine particulate matter, is strongly associated with neurodevelopmental challenges. Heavy metals like mercury, lead, and arsenic are potent neurotoxins. Pesticides and endocrine disruptors found in food, water, and household products can affect critical hormonal signaling.
Certain medications during pregnancy also show associations with autism risk. Valproic acid (used for epilepsy) has strong evidence. SSRIs and other medications taken during pregnancy have shown mixed results in research, with some studies suggesting a modest increased risk during critical development periods.
Advanced Parental Age
Both maternal and paternal age show an association with increased autism risk. Research has found that mothers over 35 and fathers over 40 have a 40-60% higher autism risk in offspring. The mechanisms aren’t entirely clear, but they may involve accumulated genetic mutations in reproductive cells or age-related factors affecting fetal development.
What Genetic Testing Can and Cannot Tell You
Many expectant parents wonder if genetic testing can predict autism. Genetic testing during pregnancy can detect certain conditions associated with increased autism risk:
- Fragile X syndrome: The most common inherited cause of intellectual condition, associated with autism in 5% of cases
- Chromosomal abnormalities: Like 1p36 deletion or duplications detectable through chromosomal microarray analysis
- Down syndrome: Up to 39% of people with Down syndrome have autism characteristics
- Tuberous sclerosis: About 45-60% also have autism or other intellectual situations
- PTEN mutations: About 25-50% of children show autism signs
Testing methods include carrier screening (blood test), chorionic villus sampling (CVS), amniocentesis, and non-invasive prenatal testing (NIPT).
The Critical Limitation
Even if testing reveals one of these conditions, it doesn’t definitively mean your child will have autism. And normal genetic testing doesn’t mean they won’t.
Why? Because autism isn’t caused by a single gene. Over 100 genes and chromosomal variations have been associated with autism, but none cause it 100% of the time. Even identical twins don’t both develop autism in all cases.
This tells us: genetics load the gun, but environment and physiology pull the trigger. Genetic vulnerability plus the “Perfect Storm” factors determine whether autism develops.
What no prenatal test can tell you is the state of your baby’s developing nervous system. There’s no test measuring vagus nerve development, autonomic function, or dysautonomia in utero. Yet these neurological factors are often more predictive than genetic testing alone.
Birth Interventions and Autism Risk
Here’s what conventional medicine rarely discusses: birth interventions and birth trauma significantly impact your baby’s neurological development.
Modern birth interventions can dramatically increase the mechanical forces applied to the most vulnerable part of a baby’s anatomy: the upper neck and brainstem, exactly where the vagus nerve exits the skull.
- Cesarean section delivery shows an increased association with autism in multiple studies. Babies born via C-section often show patterns of upper cervical tension and nervous system dysregulation.
- Forceps and vacuum extraction apply intense forces directly to the baby’s head and neck, the location where the vagus nerve exits. This trauma can create subluxation, nervous system dysfunction from mechanical stress to the spine and brainstem.
- Labor induction, prolonged labor, and fetal distress all indicate the baby’s nervous system is experiencing significant stress before birth.
The Neurological Impact
When birth trauma damages or dysregulates vagus nerve function, you’re setting up the nervous system to struggle with regulatory functions. If a baby experiences trauma affecting vagus nerve function, they can’t latch properly, develop colic and digestive issues, can’t calm and sleep well, and become overwhelmed by sensory input.
We often see a pattern: difficult birth → feeding challenges → colic → chronic ear infections → sensory sensitivities → eventual autism diagnosis. It’s not random; it’s a nervous system dysfunction that started at birth.
This isn’t about blame. Many interventions are necessary. This information provides understanding so you can monitor for early signs and take proactive steps to support neurological health.
Early Warning Signs vs. Definitive Diagnosis
Autism doesn’t suddenly appear at age two. The neurological dysfunction is typically present much earlier, but manifests differently in infancy.
Early post-birth indicators of nervous system stress include:
- Difficulty latching and feeding
- Colic and excessive crying
- Digestive distress (reflux, constipation)
- Sleep disruption
- Limited eye contact and poor responsiveness
- Sensory sensitivities
- Motor tone abnormalities
- Developmental delays
Here’s the pattern: “They don’t grow out of it, they grow into it.”
- Colic at 2 months becomes chronic constipation at 6 months
- Constipation becomes sensory sensitivity at 18 months
- Sensory issues become ADHD or autism signs by age 3-5
The neurology doesn’t change. The nervous system dysfunction just gets different diagnostic labels as developmental demands increase.
What Parents Can Do
Understanding how autism risk builds through nervous system stress means you’re not powerless.
During Pregnancy:
- Manage stress through mindfulness, movement, and adequate sleep
- Optimize nutrition: folate (400-800 mcg daily), omega-3 fatty acids, and iron
- Minimize environmental toxins and chemical exposures
- Talk through your birth preferences early, and partner with a provider who respects and aligns with your vision
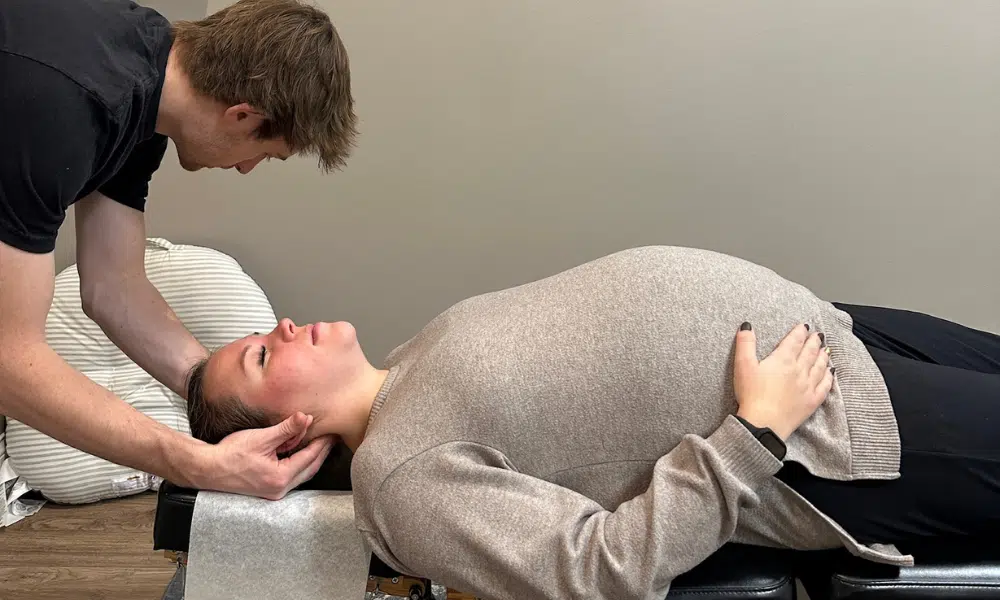
- Prenatal chiropractic care can help keep your nervous system calm, balanced, and adaptable during pregnancy.
After Birth: If your baby has risk factors or shows early signs, the most important thing is to support neurological health immediately. The nervous system has its greatest capacity for change during the first year.
At PX Docs offices, we use INSiGHT scans, specialized, safe, non-invasive neurological scanning that can objectively measure your baby’s nervous system function from days old. These scans identify nervous system dysfunction before it manifests as developmental delays.
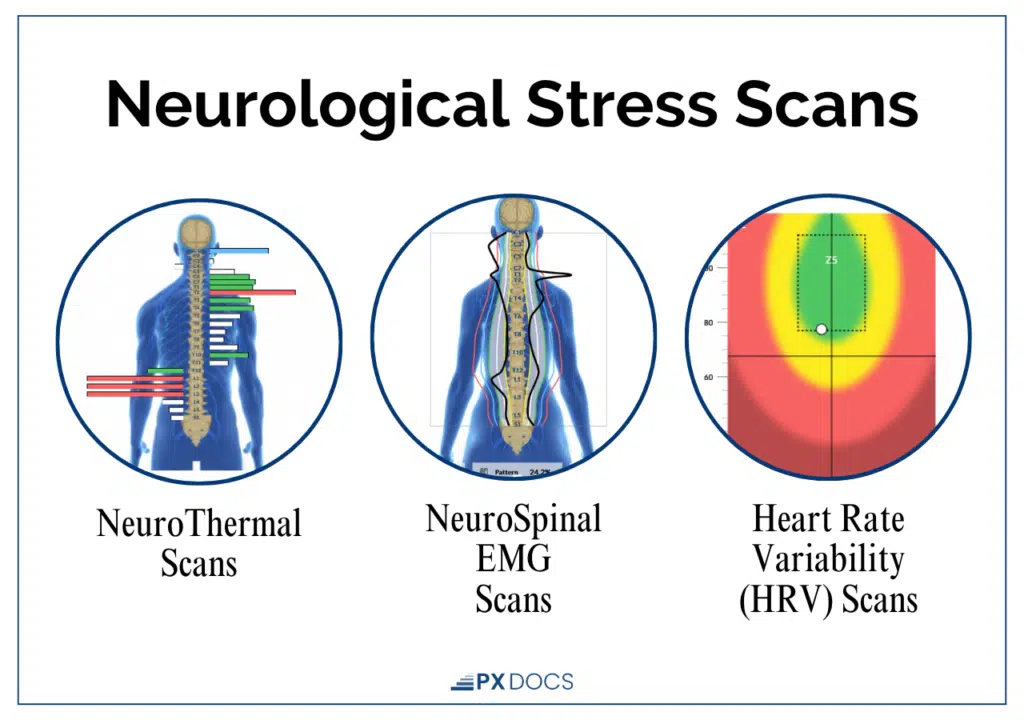
By removing subluxation and supporting vagus nerve function through Neurologically-Focused Chiropractic Care, we address the neurological foundation affecting every body system. This is why parents report improvements not just in one area but across sleep, digestion, immune function, and sensory regulation.
We’re not curing autism. We’re addressing the nervous system dysfunction and allowing the body to heal from the inside out.
Conclusion
While there’s no prenatal test for autism, risk factors are identifiable. The revolutionary insight is that autism begins with nervous system dysfunction, and the “Perfect Storm” framework provides answers conventional medicine misses.
You can take action during pregnancy to support optimal nervous system development. You can be vigilant after birth for early warning signs. And you can seek neurological assessment during that critical first year when the nervous system has the greatest capacity for healing.
If you’re pregnant and concerned about autism risk, or if your baby is showing early signs, don’t wait. Connect with a PX Docs provider who can assess your baby’s neurological health. Find a provider near you through the PX Docs directory.
Remember: they don’t grow out of it, they grow into it. Unless we address the nervous system foundation early. That’s where healing begins, and where hope becomes reality.