For over 70 million people worldwide living with dysautonomia, the condition can have a profound impact on daily life. For parents, watching their child navigate the daily struggles of this disorder is often both heartbreaking and frustrating.
From constant fatigue and dizziness to unpredictable digestive issues and brain fog, this invisible illness can significantly disrupt a child’s quality of life, leaving families searching desperately for answers and real solutions.
Dysautonomia is a term used to describe a group of conditions that affect the Autonomic Nervous System (ANS), which controls involuntary functions like heart rate, blood pressure, digestion, and temperature regulation. When the ANS isn’t functioning properly, it can lead to a wide range of symptoms that vary in severity and frequency from child to child.
If you’re a parent of a child with dysautonomia, you’ve likely asked the question: “Does this ever go away?”
The truth is, there’s no simple answer, and every child’s journey is unique. But take a deep breath and know this: there is so much hope. We’ve seen children not only improve but completely transform, getting back to life, completely drug-free. We’ve even seen some release the diagnosis entirely.
Most importantly, these kids start enjoying what they love again — playing, laughing, connecting, sports, school — and simply being a kid.
So while there may not be a quick fix or one-size-fits-all answer, true healing is possible. And we’re here to walk with you every step of the way.
In this article, we’ll dive deep into the world of dysautonomia — what causes it, the symptoms to watch for, and how PX Docs’ Neurologically-Focused Chiropractic Care offers a unique and natural approach to getting to the root of this challenging condition.
What is Dysautonomia?
Dysautonomia is an umbrella term for a group of conditions that involve dysfunction of the Autonomic Nervous System (ANS). The ANS is responsible for regulating involuntary functions that keep our bodies in balance, such as:
- Heart rate and blood pressure
- Digestion and bowel movements
- Breathing and respiratory rate
- Body temperature
- Sweating and other glandular functions
When the autonomic nervous system (ANS) isn’t functioning properly, it can create a wide range of symptoms that impact multiple body systems. Because the severity and frequency of these symptoms can vary so widely from one child to another, dysautonomia can be incredibly difficult to recognize, diagnose, and manage — especially within the traditional medical model.
Even when a diagnosis is made, treatment options are often limited and focused solely on symptom management. Rarely do they address the underlying reason why the nervous system is dysregulated in the first place.
In fact, the nervous system’s central role is often completely overlooked, leaving families with more questions than answers and few long-term solutions.
There are several types of dysautonomia, each with its own set of characteristics and challenges. Some of the most common forms include:
- Postural Orthostatic Tachycardia Syndrome (POTS): A condition that affects an estimated 6.8% of children and causes a rapid increase in heart rate upon standing, often accompanied by dizziness, fatigue, and lightheadedness.
- Neurocardiogenic Syncope (NCS): Also known as vasovagal syncope, NCS involves sudden drops in blood pressure that can lead to fainting or near-fainting episodes.
- Multiple System Atrophy (MSA): A progressive neurodegenerative condition that affects the Autonomic Nervous System, leading to problems with balance, coordination, and other functions.
- Familial Dysautonomia (FD): A rare genetic condition that affects the development and function of the autonomic and sensory nervous systems, causing a range of signs from birth.
Dysautonomia can impact various aspects of a child’s life, from their physical abilities and cognitive function to their emotional well-being and social interactions. Some of the most common ways dysautonomia affects the body include:
- Cardiovascular system: Abnormal heart rate, blood pressure fluctuations, and poor circulation
- Gastrointestinal system: Nausea, vomiting, bloating, constipation, and diarrhea
- Respiratory system: Shortness of breath, difficulty breathing, and air hunger
- Nervous system: Brain fog, headaches, migraines, and cognitive impairment
- Musculoskeletal system: Chronic pain, joint hypermobility, and muscle weakness
- Endocrine system: Hormonal imbalances, temperature regulation issues, and sweating abnormalities
By understanding the complexities of dysautonomia and its impact on the body, parents and healthcare providers can work together to develop care plans that address the unique needs of each child living with this challenging condition.
Signs of Dysautonomia
Dysautonomia can manifest in a wide range of signs and symptoms that affect various body systems.
Some of the most common symptoms experienced by children with dysautonomia include:
- Fatigue and weakness
- Dizziness and lightheadedness, especially when standing up (orthostatic intolerance)
- Rapid heartbeat (tachycardia) or slow heartbeat (bradycardia)
- Chest pain or discomfort
- Shortness of breath or difficulty breathing
- Nausea, vomiting, bloating, and abdominal pain
- Constipation or diarrhea
- Difficulty regulating body temperature (feeling too hot or too cold)
- Excessive sweating or an inability to sweat
- Headaches and migraines
- Brain fog, difficulty concentrating, and memory problems
- Blurred vision or vision changes
- Tremors or muscle twitches
- Anxiety, depression, and mood swings
For many children with dysautonomia, the unpredictable nature of their symptoms can be one of the most challenging aspects of living with the condition. Symptoms may come and go without warning, making it difficult to plan activities or maintain a consistent routine. This can lead to feelings of frustration, isolation, and a greatly reduced quality of life.
In addition to the physical signs, dysautonomia can also have a profound impact on a child’s emotional and social well-being. The constant fatigue, pain, and other symptoms can make it challenging to keep up with schoolwork, participate in extracurricular activities, and maintain friendships. This can lead to feelings of loneliness, anxiety, and depression, further compounding the difficulties faced by children with dysautonomia.
With the right support and care focused on the root cause, children with dysautonomia can do more than just manage their symptoms — they can experience real healing, regain their energy and resilience, and get back to thriving in the life they were meant to live.
What Causes Dysautonomia?
Understanding the causes and contributing factors associated with dysautonomia is essential for parents seeking answers and lasting solutions. Research suggests that a combination of maternal factors, epigenetics, and postnatal experience can contribute to the development of Autonomic Nervous System dysfunction..
In our clinical experience at PX Docs, we’ve seen these same patterns emerge time and time again through the detailed case histories we collect and the INSiGHT scans we perform. In fact, our perspective is that research often lags behind what’s already been evident in practice. Long before the studies are published, parents are bringing us the stories, and the stressors, that line up with what we call The “Perfect Storm behind dysautonomia and so many other chronic neurological challenges.
One key component of “The Perfect Storm” is prenatal stress. Studies have shown that maternal stress during pregnancy can have a significant impact on fetal brain development, potentially affecting the development of the Autonomic Nervous System. When a mother experiences chronic stress, her body releases higher levels of stress hormones, such as cortisol, which can cross the placenta and affect the developing fetus. This exposure can alter the way the baby’s nervous system develops, making it more susceptible to dysregulation and dysfunction later in life.
Another important factor in the development of dysautonomia is birth trauma. Complications during labor and delivery, such as prolonged labor, forceps or vacuum extraction, or cesarean section, can cause physical stress and injury to the infant’s delicate nervous system. This trauma can lead to subluxation, which is tension or imbalance within the neurospinal system that interferes with proper nerve function. When subluxation occurs, it can disrupt the proper functioning of the Autonomic Nervous System, directly leading to dysautonomia and other health challenges.
In addition to prenatal stress and birth trauma, early childhood stressors can also contribute to the development of dysautonomia. These stressors may include:
- Chronic illnesses or infections
- Exposure to environmental toxins
- Nutritional deficiencies
- Physical or emotional trauma
- Antibiotic overuse and gut dysbiosis
When a child experiences these stressors, their nervous system may become stuck in a state of “fight or flight,” leading to chronic tension, inflammation, and imbalance. This sympathetic dominance can interfere with the child’s ability to rest, digest, and heal, creating a vicious cycle of stress and dysfunction that may ultimately lead to dysautonomia.
Other potential causes and risk factors for dysautonomia include:
- Autoimmune conditions, such as lupus, rheumatoid arthritis, and Sjögren’s syndrome
- Infections, such as Lyme disease, Epstein-Barr virus, and COVID-19
- Genetic factors, such as mutations in genes involved in Autonomic Nervous System development and function
By understanding these connected factors that can contribute to the development of dysautonomia, parents and healthcare providers can work together to prevent or mitigate the impact of “The Perfect Storm,” and provide targeted interventions to support the health and well-being of children with this challenging condition.
Does Dysautonomia Go Away? Factors Affecting Prognosis
One of the most common questions we hear from parents of children with dysautonomia is whether the condition can be cured or will eventually go away. While there is no simple answer to this question, understanding the factors that influence long-term outcomes can provide valuable insight and hope for families navigating this challenging journey.
The prognosis for dysautonomia varies widely depending on the specific type of autonomic dysfunction, the underlying causes, and the individual child’s response to care.
While some cases may appear to improve after a short-term trigger like a viral illness or acute stressor, what we see clinically is that dysautonomia is rarely that simple. Even in those cases, the underlying dysregulation within the nervous system often remains and needs to be addressed.
For many children—especially those with chronic or complex patterns—true healing takes time, intention, and a consistent focus on restoring proper nervous system function. The good news is, with the right approach, we see incredible progress and transformation happen every day. There is so much hope when care is focused on root cause healing, not just symptom management.
Factors that can influence the long-term outcomes of dysautonomia include:
- Early intervention and diagnosis
- Addressing underlying causes, such as subluxation and nervous system dysregulation
- Adherence to a comprehensive care plan, including lifestyle modifications and supportive therapies
- Access to knowledgeable and experienced healthcare providers
- Strong support systems, including family, friends, and dysautonomia communities
While there is limited research on the long-term prognosis of pediatric dysautonomia, studies suggest that many children experience significant improvement in symptoms and quality of life with appropriate care and management.
We have seen firsthand the incredible transformations that can occur when children with dysautonomia receive the proper care and support.
Conventional Medical Approaches and Limitations
When a child presents with signs of dysautonomia, healthcare providers may use a variety of diagnostic tests and tools to identify the specific type of autonomic dysfunction and develop an appropriate care plan. Some common diagnostic methods include:
- Tilt table test: This test measures heart rate and blood pressure while the child is tilted at different angles to assess orthostatic intolerance.
- Quantitative Sudomotor Axon Reflex Test (QSART): This test evaluates the function of the nerves that control sweating.
- Heart rate variability (HRV) analysis: This non-invasive test measures the variation in time between each heartbeat to assess Autonomic Nervous System regulation.
- Blood tests: These tests can help rule out other conditions that may be causing signs similar to dysautonomia.
Once a diagnosis of dysautonomia is made, conventional medical care plans typically focus on managing signs and improving quality of life. Some common care options include:
- Medications: Beta-blockers, vasoconstrictors, and other drugs may be prescribed to regulate heart rate, blood pressure, and other autonomic functions.
- Lifestyle changes: Increasing fluid and salt intake, wearing compression garments, and avoiding triggers such as prolonged standing or heat exposure may help manage traits.
- Physical therapy: Exercises and techniques to improve circulation, strengthen muscles, and promote cardiovascular conditioning may be recommended.
While these conventional approaches can sometimes be helpful in managing the symptoms of dysautonomia, they often fall short of addressing the underlying causes of the condition. By focusing primarily on symptom management, rather than identifying and caring for the root causes of autonomic dysfunction, these approaches often provide only temporary relief and fail to promote long-term healing and wellness.
Moreover, many of the medications used to care for dysautonomia can have significant side effects, such as fatigue, dizziness, and gastrointestinal distress, which may further compromise a child’s quality of life. In some cases, these medications may even exacerbate the underlying autonomic imbalance, creating a cycle of dependence and diminishing returns.
The PX Docs Approach of Neurologically-Focused Chiropractic Care
We offer a unique approach to addressing dysautonomia that focuses on the underlying nervous system imbalances and promoting optimal function. Our Neurologically-Focused Chiropractic Care is designed to identify and correct the root causes of autonomic dysfunction, providing a foundation for lasting healing and wellness.
Central to our approach is the use of a cutting-edge diagnostic tool that allows us to assess the function of the Autonomic Nervous System and pinpoint areas of subluxation and dysregulation. By providing a detailed picture of a child’s neurological health, these scans enable our doctors to develop targeted, personalized care plans that address the specific needs of each individual.
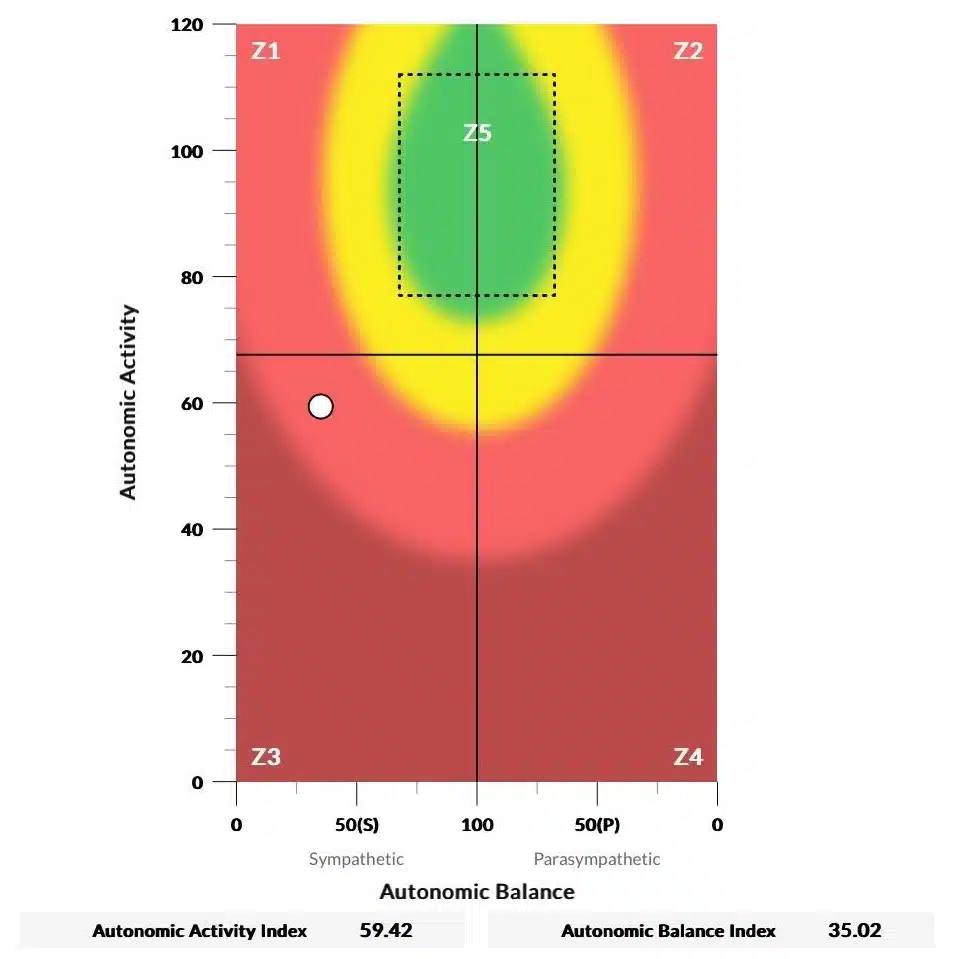
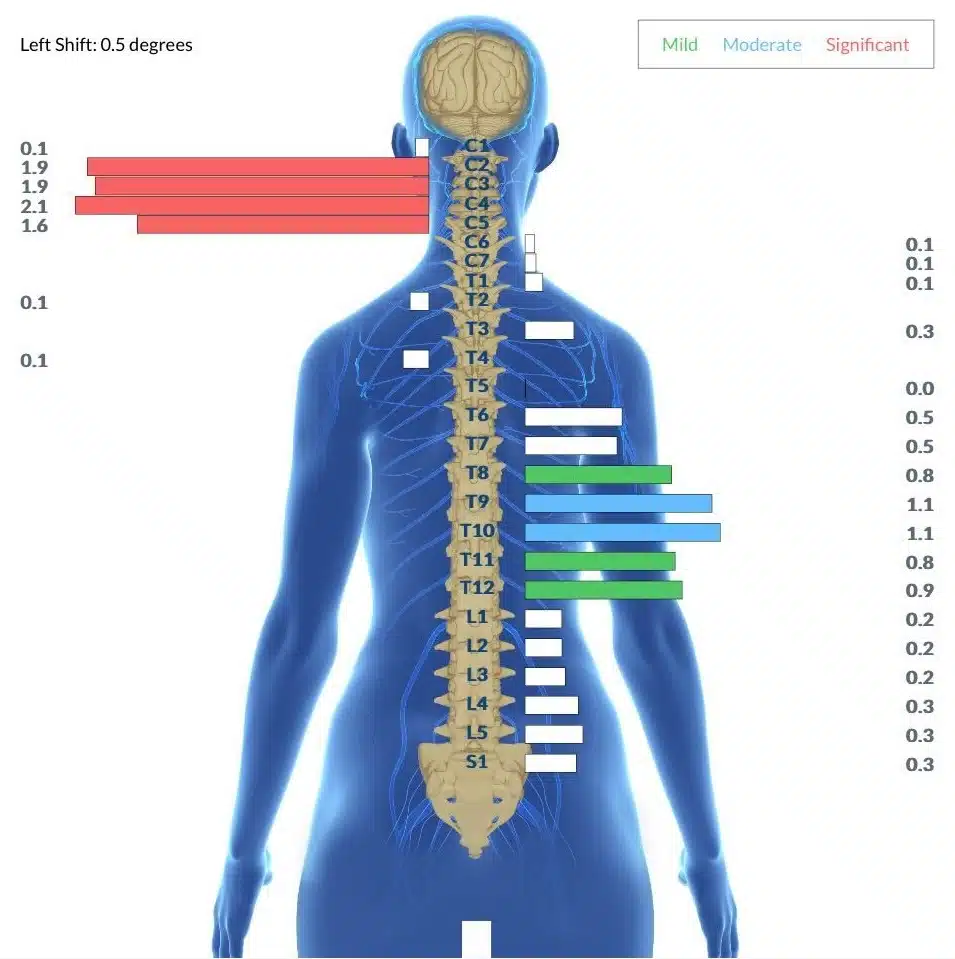
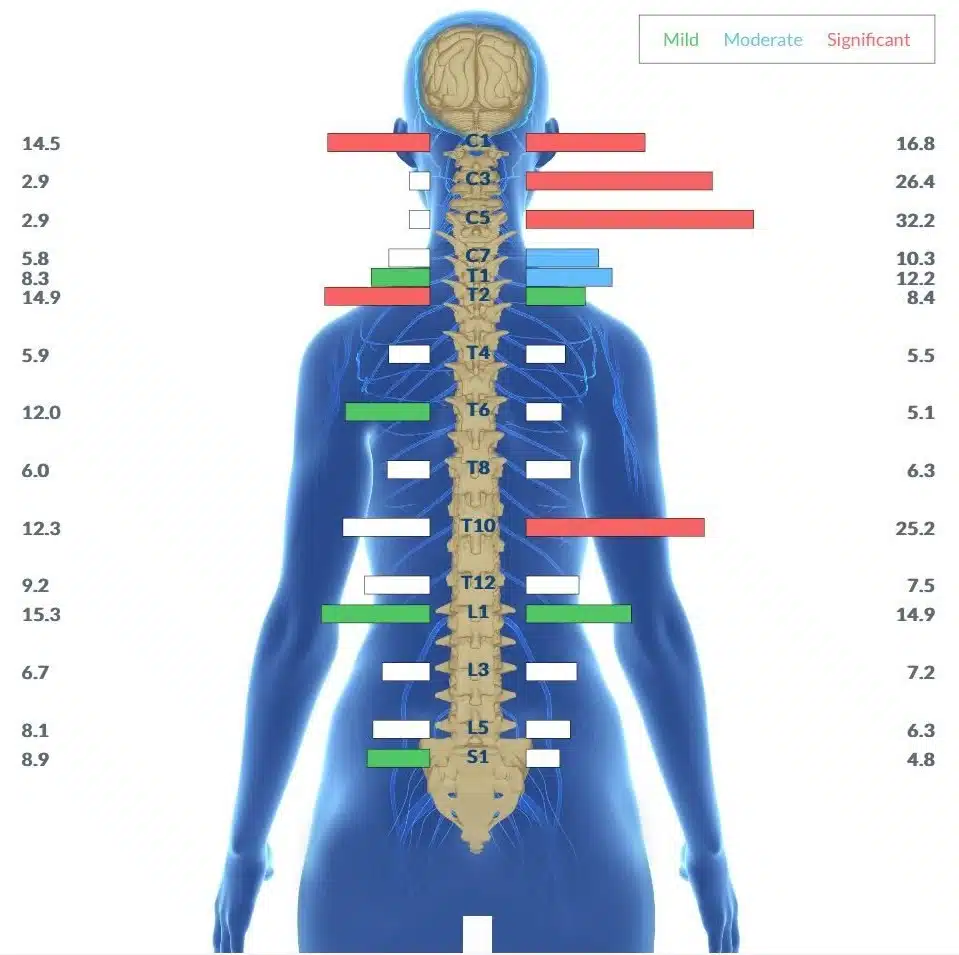
By addressing the underlying causes of dysautonomia, rather than simply managing symptoms, Neurologically-Focused Chiropractic Care offers a promising alternative for children struggling with this complex condition. Our approach has helped countless families find relief from and get to the root cause of the debilitating symptoms of dysautonomia, allowing children to regain their health, vitality, and quality of life.
Living with Dysautonomia: Practical Tips and Coping Strategies
While Neurologically-Focused Chiropractic Care is foundational for true healing and regulation of the nervous system, there are also practical, day-to-day steps that can support your child’s overall well-being. These tools won’t get to the root cause solely on their own—but when paired with the right care, they can help your child feel better, recover faster, and regain more of their life and joy. Here are some of the strategies we share with the families we serve:
- Stay hydrated: Drinking plenty of fluids, particularly water and electrolyte-rich beverages, can help maintain blood volume and reduce signs of orthostatic intolerance.
- Increase salt intake: Adding extra salt to your child’s diet (under the guidance of a healthcare provider) can help retain fluids and improve blood pressure regulation.
- Pace activities: Encourage your child to listen to their body and take breaks as needed rather than pushing through fatigue or other signs.
- Use compression garments: Wearing compression stockings or abdominal binders can help improve circulation and reduce pooling of blood in the legs.
- Prioritize sleep: Ensuring that your child gets adequate, quality sleep can help improve energy levels, mood, and overall functioning.
- Manage stress: Incorporating stress-reducing activities such as deep breathing, meditation, or gentle yoga can help regulate the Autonomic Nervous System and improve symptoms.
- Seek support: Connecting with other families affected by dysautonomia, joining support groups, and building a strong network of friends and loved ones can provide invaluable emotional support and practical assistance.
And one last tip — advocate boldly. Just remember, you know your child best. Don’t be afraid to ask the hard questions, push for real answers, and remind every provider that they work for you. Keep seeking until you find a team, like the PX Docs, that truly listens and is committed to your child’s long-term healing.
Hope, Resilience, and the Path Forward
Living with dysautonomia can be a challenging and overwhelming experience for children and families alike. The unpredictable signs, the constant need for adaptation and flexibility, and the lack of widespread understanding and support can make the journey feel isolating and hopeless at times.
However, we have seen time and again the incredible resilience, strength, and determination of the families we serve. We have witnessed children who were once bedridden with fatigue and pain reclaim their lives and pursue their passions. We have seen parents who felt helpless and alone find community, support, and empowerment through shared experiences and knowledge.
While the path forward may not always be clear or easy, we believe that every child with dysautonomia deserves the opportunity to thrive and live the best life possible. By embracing a drug-free, Neurologically-Focused approach to care, families can find hope, healing, and a renewed sense of possibility. If you are a parent of a child with dysautonomia, we invite you to take the first step towards reclaiming your child’s health and well-being by visiting the PX Docs Directory and finding a qualified Neurologically-Focused Chiropractor in your area. With compassionate, knowledgeable care and unwavering support, your family can navigate the challenges of dysautonomia with confidence and resilience, knowing that you are not alone on this journey.