Tinnitus in children is more common than most parents realize. Research shows that anywhere from 6% to 36% of children with normal hearing experience tinnitus at some point, and about 15% of children deal with it on a chronic basis.
What makes tinnitus in children so tricky is that many kids don’t even report it. Younger children may not have the words to describe what they’re hearing, while older kids might assume the sounds are normal because they’ve never known anything different. And when a child does speak up, conventional medicine often has limited answers beyond “wait and see” or sound therapy.
But here’s what most parents aren’t told: tinnitus isn’t just an ear problem. Emerging research points to the Autonomic Nervous System, which controls everything from heart rate to digestion to how your child processes sound, as a major factor in why tinnitus develops and persists. That neurological connection is exactly where we need to look for real, lasting answers.
What Is Tinnitus in Children?
Tinnitus is the perception of sound when no external sound source is present. In children, this can show up as ringing, buzzing, humming, hissing, clicking, whooshing, or even a roaring sound. The noise may be constant or come and go, affect one ear or both, and range from a low hum to a high-pitched ring.
There are two main types of tinnitus:
- Subjective tinnitus is the most common form, where only the child can hear the sound. It’s caused by changes in how the auditory nervous system processes signals.
- Objective tinnitus is rare and involves a physical sound produced within the body, usually from blood flow or muscle contractions, that a doctor can sometimes detect during an examination.
Most children with tinnitus have otherwise normal hearing test results, which is one reason it often gets overlooked. But just because a standard hearing test comes back normal doesn’t mean the auditory nervous system is functioning the way it should. That distinction matters more than most people realize.
Signs of Tinnitus in Children
One of the biggest challenges with pediatric tinnitus is that children often don’t complain about it. Some kids have lived with these sounds for so long that they think everyone hears them. Others lack the vocabulary to explain what’s happening.
Here are signs parents should watch for:
- Your child mentions hearing ringing, buzzing, or other sounds that aren’t there
- Difficulty concentrating in school, especially in quiet environments
- Trouble falling asleep or staying asleep
- Covering their ears frequently or being bothered by everyday sounds
- Increased anxiety, irritability, or emotional outbursts
- Avoiding quiet rooms or always wanting background noise
- Complaints of ear pain or pressure without an active infection
In more severe cases, tinnitus can interfere with a child’s sleep, concentration, and emotional well-being. When the sounds are persistent and distressing, they can create a cascade of secondary problems that affect everything from school performance to behavior at home.
What many parents also notice, and this is an important pattern, is that tinnitus often doesn’t show up alone. These kids frequently have a history of other challenges like recurring ear infections, sensory processing difficulties, anxiety, sleep issues, or difficulty with focus and attention. When you see multiple symptoms stacking up like that, it’s a signal that something deeper is going on with the nervous system.
What Causes Tinnitus in Children?
Conventional medicine identifies several common causes of tinnitus in children:
- Earwax buildup: Impacted earwax can block the ear canal and disrupt normal sound transmission, triggering tinnitus symptoms.
- Ear infections: Children are particularly susceptible to middle ear infections due to their smaller and more horizontal Eustachian tubes. Repeated infections can contribute to both tinnitus and hearing changes.
- Noise exposure: Headphones, loud toys, concerts, and sporting events can damage the delicate hair cells in the inner ear. Once damaged, these hair cells don’t regenerate.
- Hearing loss: Even mild hearing loss, sometimes undetected, can trigger the brain to compensate by amplifying its own internal signals, creating phantom sounds.
- Medications: Certain medications, including some antibiotics and anti-inflammatory drugs, are known to be ototoxic, meaning they can affect the inner ear and cause tinnitus.
- Head injury or concussion: Physical trauma to the head can damage auditory pathways and trigger tinnitus.
- TMJ disorders: Problems with the jaw joint can refer pain and sounds to the ear due to the close proximity of these structures.
These are all valid causes, and any child experiencing tinnitus should be evaluated by their pediatrician and, if needed, an audiologist or ENT specialist to rule out underlying medical conditions.
But here’s the question most providers aren’t asking: why is this child’s auditory system reacting this way in the first place? And why do so many children with tinnitus also struggle with anxiety, sleep problems, and sensory sensitivities?
The Nervous System Connection Most Doctors Miss
This is where we need to go deeper than what conventional approaches typically explore. Tinnitus isn’t always just a problem with the ear; it’s a problem with how the brain and nervous system process auditory signals.
Studies have demonstrated that tinnitus patients consistently exhibit decreased parasympathetic activity and increased sympathetic tone, as measured by heart rate variability (HRV) testing. In simple terms, the nervous system is stuck with the gas pedal (sympathetic “fight or flight”) pushed down and the brake pedal (parasympathetic “rest, digest, regulate”) not working well enough to bring things back into balance.
This is exactly what we call nervous system dysregulation, and it’s the same pattern we see driving dozens of other childhood health challenges.
Here’s why this matters specifically for tinnitus: the auditory system doesn’t operate in isolation. Sound signals travel from the ear to the brainstem, and from there they connect to the limbic system (which controls emotions) and the Autonomic Nervous System (which controls involuntary body functions). When the nervous system is in a state of chronic sympathetic dominance, the brain’s auditory processing centers become hyperexcited and hypersensitive. Normal neural activity gets amplified and misinterpreted as sound.
Research published in Scientific Reports confirms that tinnitus is associated with autonomic dysfunction, specifically vagal withdrawal and sympathetic overactivity. The vagus nerve, which is the longest cranial nerve and the primary driver of parasympathetic function, plays a direct role in this picture. When vagus nerve function is compromised, the body can’t properly regulate its stress response, inflammatory pathways, and sensory processing, including the interpretation of auditory signals.
This is also why vagus nerve stimulation (VNS) is now being studied as a treatment for tinnitus. Researchers have found that stimulating the vagus nerve can help reverse the neuroplastic changes in auditory processing that contribute to tinnitus perception. Science is catching up with what we’ve been observing clinically for years: when you address vagus nerve dysfunction, many seemingly unrelated symptoms begin to improve together.
How “The Perfect Storm” Sets the Stage for Tinnitus in Children
When we see a child struggling with tinnitus, especially alongside other challenges like anxiety, sensory sensitivities, sleep difficulties, or a history of chronic ear infections, we look at the full picture of what that child’s nervous system has been through. We call this “The Perfect Storm.”
The “Perfect Storm” describes how a sequence of early-life stressors can stack up and overwhelm a child’s developing nervous system:
- Prenatal stress and maternal health challenges. High levels of maternal stress during pregnancy expose the developing fetus to elevated cortisol and stress hormones. This can shift the baby’s autonomic nervous system toward sympathetic dominance before they’re even born, affecting how the auditory and sensory systems develop during critical windows.
- Birth trauma and interventions. Procedures like C-sections, forceps delivery, vacuum extraction, induction, and prolonged labor can create physical stress on the infant’s upper cervical spine and brainstem, the exact region where auditory nerve pathways pass through and where the vagus nerve originates. Injury or tension in this area can disrupt how the nervous system processes sound from the very beginning.
- Early childhood stressors. Repeated ear infections (and the rounds of antibiotics that follow), chronic inflammation, exposure to environmental toxins, and ongoing stress all add to the load on a nervous system that’s already struggling to regulate. Each additional stressor compounds the problem.
This cascade creates what we call subluxation, not just a structural misalignment, but a state of neurological interference involving misalignment, fixation, and disrupted communication between the brain and body. When subluxation affects the upper cervical and brainstem regions, it can directly impact auditory processing, vagus nerve function, and the autonomic nervous system’s ability to regulate sensory input.
The result? A child whose nervous system is stuck in a state of dysautonomia, chronic imbalance between the sympathetic and parasympathetic branches, creating the exact neurological environment where tinnitus thrives.
How Tinnitus in Children Is Diagnosed
If your child reports hearing sounds that others can’t hear, or if you notice any of the signs mentioned earlier, the first step is an evaluation with your pediatrician. From there, they may refer you to:
- An audiologist who will perform a comprehensive hearing evaluation, assess the characteristics of the tinnitus, and evaluate how much it’s affecting your child’s daily life.
- An ENT specialist (otolaryngologist) who can examine the ear structures, rule out infections, structural issues, or other medical causes, and order additional testing if needed.
Diagnosis is primarily based on your child’s description of their symptoms, combined with hearing tests and sometimes imaging studies to rule out underlying conditions. Standard tests include pure tone audiometry, tympanometry (to assess middle ear function), and otoacoustic emissions testing.
What’s often missing from this process, though, is any assessment of nervous system function. Standard hearing tests tell you what the ear is doing, but they don’t tell you why the auditory system is misbehaving, and they don’t measure the autonomic nervous system imbalances that research has linked to tinnitus.
A Neurological Approach to Tinnitus in Children
This is where Neurologically-Focused Chiropractic Care offers something that other approaches don’t, the ability to assess and address nervous system function directly.
It’s important to note that our INSiGHT scanning technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for tinnitus or any other condition, not even back pain. Instead, these INSiGHT Scans help us track down the root cause of nervous system dysfunction and dysregulation, and build customized care plans and adjusting protocols to help shift the nervous system back into a state of balance, regulation, and resilience.
Our INSiGHT scanning technology includes three key assessments:
- Heart Rate Variability (HRV) Analysis measures the balance between the sympathetic (“fight or flight”) and parasympathetic (“rest, regulate, and digest”) branches of the autonomic nervous system. This is the same measurement researchers use to identify autonomic dysfunction in tinnitus patients.
- Surface Electromyography (sEMG) assesses the electrical activity of muscles along the spine, identifying areas of tension and altered neuromuscular function, particularly important in the upper cervical region where auditory nerve pathways are concentrated.
- Thermal Scanning uses infrared sensors to measure temperature differences along the spine, which can reveal areas of dysautonomia and neurological stress.
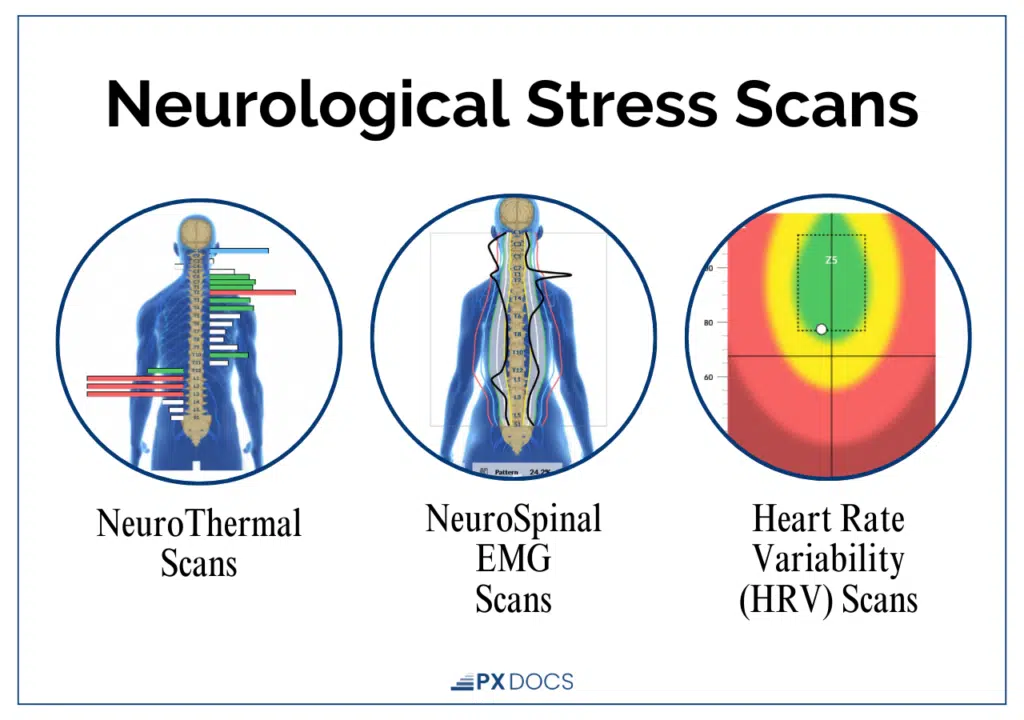
What makes these scans so valuable is their ability to detect nervous system dysfunction that standard medical tests simply aren’t designed to find. For many families, this objective assessment finally provides the clarity they’ve been searching for.
When subluxation and nervous system dysregulation are identified, Neurologically-Focused Chiropractic Care works to restore proper communication between the brain and body. By addressing the neurological interference that’s driving sympathetic dominance and vagus nerve dysfunction, we’re working to create the conditions where the nervous system can begin to self-regulate again, including how it processes auditory information.
Unlike external tools or temporary strategies aimed at “stimulating” the vagus nerve, this approach focuses on removing the interference that’s disrupting its function in the first place. When that interference is reduced, the vagus nerve doesn’t need to be forced to activate—it can naturally come back online, improving tone, adaptability, and overall nervous system balance from the inside out.
What Parents Can Do Right Now
Whether you’re just beginning to explore what’s going on with your child’s tinnitus or you’ve been searching for answers for a while, here are practical steps you can take today:
- Protect their hearing. Limit headphone use, keep volumes at safe levels, and use ear protection at loud events. Prevention of further auditory stress is always important.
- Reduce overall nervous system load. More time outdoors, less screen time, better sleep habits, and reduced intake of sugar and processed foods all help reduce the overall stress burden on a child’s nervous system.
- Pay attention to patterns. Track when the tinnitus is worse, during stress, before bed, after screen time, and during illness. These patterns can provide valuable clues about what’s triggering nervous system overload.
- Don’t dismiss their experience. Children who are told “it’s nothing” or “you’ll grow out of it” often stop reporting symptoms and internalize the distress. Validate what they’re experiencing and let them know you’re working to find answers.
- Get a neurological assessment. If your child’s tinnitus exists alongside other signs of nervous system dysfunction, anxiety, sleep issues, sensory sensitivities, chronic ear infections, gut problems, a comprehensive neurological evaluation can uncover patterns that standard medical testing misses.
Taking the Next Step for Your Child
Tinnitus in children is more than an ear problem. When you understand the nervous system connection, how autonomic imbalance, vagus nerve dysfunction, and subluxation can create the neurological environment where tinnitus develops and persists, a whole new set of possibilities opens up.
Your child isn’t broken. There are real, measurable reasons why their nervous system is generating these phantom sounds, and there are ways to address the root cause rather than just managing symptoms.
If you’re ready to explore a neurological approach for your child’s tinnitus, visit the PX Docs directory to find a trained Neurologically-Focused Chiropractor near you. These practitioners are specifically equipped with INSiGHT scanning technology and the training to identify and address the nervous system dysfunction that may be driving your child’s symptoms.
And as always, continue working with your child’s pediatrician and any specialists involved in their care. The best outcomes happen when families have a complete team addressing all aspects of their child’s health.





