Your child curls up in pain after having a small snack, feeling as though their stomach is on fire, even though they only need to have a bowel movement. Doctors conduct numerous tests but find nothing wrong, labeling the issue as “functional” or “anxiety-related.” You leave yet another appointment without any answers, while your child continues to suffer.
Here’s what nobody has told you yet: visceral hypersensitivity is real, it’s measurable, and it has a neurological cause that most doctors never look for.
Visceral hypersensitivity is considered to be the cornerstone of children with chronic gut pain, Irritable Bowel Syndrome (IBS), which affects up to 15% of adolescents, and functional gastrointestinal conditions. It’s one of the most frustrating conditions parents face because the pain is genuine and severe, yet standard tests come back normal.
Understanding what’s actually happening in your child’s nervous system, and why, is the first step toward finding real answers.
What Is Visceral Hypersensitivity?
Visceral hypersensitivity is a condition in which the internal organs, particularly the digestive tract, develop an abnormally low pain threshold. Everyday sensations that shouldn’t register as pain suddenly become intensely painful.
To understand this, think about what happens when you get a sunburn. Suddenly, the lightest touch on your skin feels excruciating. Warm water that would normally feel pleasant hurts. Your skin hasn’t fundamentally changed; your nervous system is misinterpreting normal sensations as threats.
Visceral hypersensitivity is the same phenomenon, but in the gut. Your child’s digestive organs aren’t necessarily structurally damaged. Instead, the nervous system has become sensitized, turning the volume way up on normal gut signals until ordinary digestion feels like an emergency.
There are two distinct components to this hypersensitivity:
- Hyperalgesia is when pain that would normally register as mild becomes dramatically amplified. A slight gas cramp that most kids wouldn’t notice sends your child to the floor.
- Allodynia is when sensations that shouldn’t cause pain at all, like food moving through the intestines, a full bladder, or the natural urge to have a bowel movement, become painful.
Both components involve the same underlying mechanism: the nervous system’s pain-processing pathways have been recalibrated in the wrong direction.
Visceral Hypersensitivity Symptoms in Children
The symptoms of visceral hypersensitivity can look different from child to child, which is part of why it’s so hard to pin down. Many parents spend years assuming something structural must be wrong before learning this is a nervous system issue.
Common symptoms include:
- Recurring abdominal pain or cramping that seems out of proportion to any visible cause
- Pain triggered by normal eating or drinking
- Bloating and distension that causes significant discomfort, constipation, or diarrhea (or alternating between both)
- Nausea often without vomiting
- Pain when the bladder is full
- Overall food avoidance because eating reliably triggers pain.
What makes this condition particularly exhausting is its inconsistency. Some days are manageable. Others are devastating. The pain can be sharp, dull, burning, or cramping; it changes. And because it often coincides with stress, transitions, or illness, parents and doctors alike can mistakenly attribute everything to anxiety.
Children with difficult neurological situations, including Autonomic Nervous System challenges, cerebral palsy, and hypoxic-ischemic encephalopathy, appear especially prone to visceral hypersensitivity, likely because nervous system dysfunction is already present and amplifies gut-pain signaling.
The Gut-Brain Connection: Why Pain Signals Get Amplified
To understand visceral hypersensitivity, you need to understand that the gut has its own nervous system.
The enteric nervous system contains over 100 million nerve cells lining the gastrointestinal tract, more neurons than exist in either the spinal cord or the peripheral nervous system. Scientists sometimes call this the “second brain.” It operates semi-independently, constantly sending signals up to the brain about what’s happening in the gut.
That two-way communication highway between your digestive system and your brain is called the gut-brain axis. Under normal conditions, most of those gut signals are processed at a subconscious level; you don’t feel your stomach emptying or your intestines contracting. The brain filters them out.
But when the gut-brain axis is dysregulated, that filtering breaks down. The brain stops screening out normal gut signals and starts interpreting them as threats. Signals that should never reach conscious awareness suddenly get flagged as pain. The alarm system won’t shut off.
Research shows that this dysregulation can involve both:
- Peripheral sensitization (the nerves within the gut itself become hypersensitive)
- Central sensitization (the brain’s pain-processing centers become overactive).
Specific brain regions, such as the anterior cingulate cortex, show heightened activation during visceral hypersensitivity when gut stimuli are applied; the brain is literally responding more intensely to the same input.
Serotonin plays a major role here, too. About 95% of the body’s serotonin is produced in the gut, where it regulates motility and pain perception. When the nervous system is dysregulated, serotonin signaling is disrupted, directly affecting how gut pain is processed and transmitted.
The critical question isn’t just what the gut-brain axis looks like when it’s dysregulated, it’s why it becomes dysregulated in the first place. And that’s where conventional medicine stops short.
What Causes Visceral Hypersensitivity in Children?
Mainstream medicine acknowledges several contributing factors to visceral hypersensitivity: post-infectious gut changes after a viral illness, psychological stress, anxiety, a history of colic as an infant, and genetic predisposition toward functional pain conditions.
These are real. But they’re incomplete. They describe triggers and correlations. They don’t explain the underlying mechanism that makes one child’s nervous system vulnerable to developing hypersensitivity in the first place.
The answer lies in the Autonomic Nervous System, specifically, in what happens when a child’s nervous system gets locked into a state of chronic stress activation.
The Autonomic Nervous System has two branches:
- The sympathetic branch is your child’s gas pedal; it accelerates the body into a state of fight-or-flight.
- The parasympathetic branch is the brake pedal; it brings the body into rest-and-digest, calm-and-heal.
In a healthy, well-regulated nervous system, these two branches balance each other moment to moment.
But when the nervous system becomes dysregulated, the gas pedal gets stuck. The child lives in a state of chronic sympathetic dominance, elevated stress hormones, heightened inflammatory responses, reduced gut motility, and a gut-brain axis running on high alert. In this state, visceral pain thresholds drop. The gut becomes sensitized. Everything hurts more.
The “Perfect Storm” of How Birth Trauma and Early Stress Sensitize the Gut
Here’s the question that should be asked of every child with chronic visceral hypersensitivity: When did the nervous system first get knocked out of balance?
At PX Docs, we call this the “Perfect Storm,” a convergence of early-life stressors that overwhelm a developing nervous system and create lasting dysregulation. These stressors happen during the most critical window of neurological development, when the nervous system is most plastic and most vulnerable.
- Prenatal stress and maternal health play a significant role in wiring the developing nervous system. When a mother experiences prolonged stress during pregnancy, elevated cortisol and stress hormones cross the placenta. The fetal nervous system develops in a chemical environment that primes it for threat-detection rather than calm regulation. Prenatal stress doesn’t just affect mood; it shapes how the nervous system will process pain for years to come.
- Birth trauma and interventions are among the most underrecognized contributors to visceral hypersensitivity. C-sections, forceps delivery, vacuum extraction, prolonged labor, and emergency interventions all create physical stress on the infant’s delicate upper cervical spine and brainstem. This region is the control center for the vagus nerve, the primary nerve that regulates gut function, digestion, motility, and the gut-brain axis.
- Early childhood stressors compound the damage. Colic in infancy, chronic reflux, constipation, frequent ear infections cared for with repeated antibiotics, each of these creates additional neurological stress that pushes the Sympathetic Nervous System harder and suppresses the parasympathetic. The gut microbiome gets disrupted. Gut motility slows. The nervous system becomes increasingly sensitized.
By the time a child is old enough to report that eating hurts, that a full bladder feels like fire, or that they dread mealtimes, the nervous system sensitization has often been building for years.
How Subluxation Disrupts the Gut-Brain Axis
There’s a piece of this puzzle that almost no gastroenterologist will ever mention to you.
Subluxation is a term used in Neurologically-Focused Chiropractic Care to describe neurological interference, a disruption in the normal communication between the brain, the spinal cord, and the body. It’s not merely a structural misalignment. It’s a dysfunction in how the nervous system processes and transmits information.
When subluxation is present in the upper cervical spine and brainstem region, which it commonly is following birth trauma and early physical stress, the vagus nerve is directly affected. The vagus nerve controls gastric motility, digestive enzyme secretion, stomach acid production, the gut’s inflammatory response, and bidirectional signaling between the gut and the brain.
A compromised vagus nerve can’t properly regulate any of those functions. Gut motility slows. The digestive tract becomes inflamed. The brain loses its ability to filter and modulate gut-pain signals. The result is a nervous system stuck in sympathetic dominance, with a gut that’s chronically sensitized and a brain that keeps misinterpreting normal gut activity as a threat.
This neurological cascade is what drives visceral hypersensitivity in many children, not just stress, not just anxiety, not just a post-infectious gut flare. It’s a nervous system that got knocked out of regulation early in life and has been operating in a hypervigilant state ever since.
The distinction matters because it points to a completely different solution.
INSiGHT Scans: Seeing the Nervous System Dysfunction Behind Gut Pain
One of the most powerful tools in Neurologically-Focused Chiropractic Care is INSiGHT Scans, a non-invasive technology that objectively measures nervous system function.
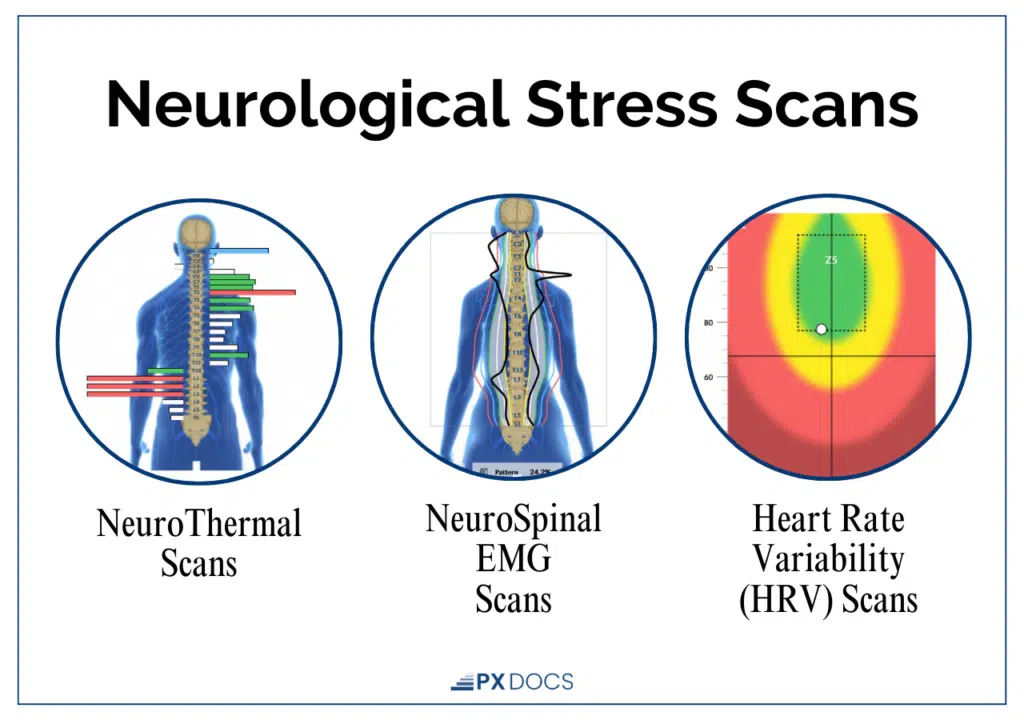
These scans include three components.
- The NeuroThermal scan measures skin temperature patterns along the spine, revealing areas of autonomic imbalance where the sympathetic nervous system is overactivated.
- The sEMG (Surface Electromyography) scan measures neuro-motor tension, the tension held in the paraspinal muscles as a result of nerve interference.
- The Heart Rate Variability (HRV) scan measures the overall balance and adaptability of the autonomic nervous system.
In children with visceral hypersensitivity and chronic gut pain, these scans frequently reveal significant dysfunction at the thoracic and upper lumbar spinal levels, exactly where the nerves controlling gut function, motility, and the gut-brain axis exit the spine. They also commonly show upper cervical dysfunction, where vagus nerve involvement is most pronounced.
This gives parents something they’ve rarely had: objective evidence of a neurological pattern that correlates with their child’s symptoms. It’s not a diagnosis of a disease. It’s a window into nervous system function that helps explain why their child’s gut is hypersensitive and provides a clear starting point for addressing it.
The PX Docs Approach
At PX Docs, we approach visceral hypersensitivity from the foundation up, starting with the nervous system.
Neurologically-Focused Chiropractic Care uses gentle, precise adjustments to address subluxation and restore proper nervous system communication. The goal is to shift the Autonomic Nervous System away from chronic sympathetic dominance and toward parasympathetic regulation, activating the brake pedal so the gut can return to rest-and-digest function.
Clinical observations from Dr. Ebel’s practice show a consistent pattern: as nervous system regulation improves, gut function begins to normalize. Motility improves. Sensitivity decreases. Children who have avoided foods for years start tolerating them again. The hypersensitivity was never just about the gut; it was about a nervous system that finally learned it was safe.
This doesn’t mean chiropractic care replaces gastroenterology, dietary approaches, or mind-body therapies. It means it addresses the neurological foundation that makes all of those other approaches more effective if necessary. When the nervous system is better regulated, the gut-brain axis functions more effectively, and every other intervention builds on a stronger foundation.
If your child has been told they have visceral hypersensitivity, functional abdominal pain, or chronic gut pain with no clear structural cause, the nervous system deserves a thorough assessment. To find a trained Neurologically-Focused Pediatric Chiropractor near you, visit the PX Docs directory and connect with a provider who can assess your child’s nervous system function directly.
Your Child’s Gut Pain Has a Cause, And a Path Forward
Visceral hypersensitivity doesn’t have to be a permanent diagnosis. It’s not a life sentence of managing symptoms and avoiding foods.
Nervous systems can change. That’s the fundamental principle of neuroplasticity. When the underlying neurological dysfunction is identified and addressed directly, when subluxation is corrected, when the vagus nerve regains function, when the autonomic nervous system returns to balance, the gut-brain axis can recalibrate. Pain thresholds can normalize. Digestion can improve.
Parents who’ve spent years chasing answers deserve to know that a neurological root cause exists and that Neurologically-Focused Chiropractic Care is designed to address it. As always, we encourage you to work alongside your child’s gastroenterologist and medical team, because a whole-child approach that addresses the nervous system foundation and the gut directly gives your child the best possible chance of real, lasting improvement. Find a PX Doc near you through our directory and take the first step toward understanding your child’s nervous system from the ground up.