Your child woke up sneezing. Their nose is running, their eyes are puffy, and they look miserable. The first question every parent asks: Is this a cold, or are these allergies?
It’s one of the most common diagnostic puzzles in pediatric health, and for good reason. The symptoms overlap almost perfectly. But knowing the difference isn’t just about picking the right medicine at the pharmacy. For kids who deal with this repeatedly, the distinction, and especially the pattern, points to something much deeper about how their immune system and nervous system are working together.
This article will walk you through everything you need to distinguish between a cold and allergies, including a symptom comparison most parents find immediately helpful. Then we’ll go a step further: if your child’s allergies keep coming back, or if they seem to be sick constantly and you can’t figure out why, there’s a neurological explanation that most pediatric offices never address.
What’s Actually Happening When Symptoms Strike
Before you can tell these two apart, it helps to understand what’s driving each one.
A common cold is a viral infection; rhinovirus is the most frequent culprit, though over 200 different viruses can trigger it. The virus enters your child’s upper respiratory tract, and their immune system mounts a defense.
That defense is what produces the familiar misery: congestion, runny nose, sore throat, coughing, low energy, and sometimes a low-grade fever. Colds are contagious, spread through droplets and surface contact, and they run their course as the immune system does its job.
Allergies work differently. There’s no virus involved. Instead, the immune system encounters something harmless, pollen, dust mites, pet dander, mold spores, and treats it like a threat.
Immune cells release a chemical called histamine, which triggers inflammation and fluid production in the nasal passages, eyes, and throat. The sneezing, runny nose, and congestion that follow are almost identical to cold symptoms, but they’re caused by an overreactive immune response rather than an infection.
That distinction, overreaction versus infection, matters a lot more than most parents realize. We’ll come back to why.
Allergies vs Cold: Symptom-by-Symptom Comparison
Here’s where most parents start, and rightly so. Some symptoms clearly favor one condition over the other.
Symptoms That Point Strongly Toward Allergies:
- Itchy eyes (red, watery, and persistently uncomfortable), this is one of the most reliable allergy markers and is uncommon with colds
- Itchy nose, throat, or skin, itchiness in general is histamine-driven and strongly suggests an allergic response
- Sneezing in rapid bursts, with colds, sneezing tends to be more spaced out; with allergies, it often comes in quick succession
- Clear, thin nasal discharge that keeps coming, allergy mucus tends to stay clear and watery
- Symptoms that improve indoors or worsen outdoors during certain seasons
- No fever, allergies don’t cause fever; if your child has one, it’s a sign of infection
Symptoms That Point Toward A Cold:
- Fever (even mild), colds sometimes cause a low-grade fever, but allergies never do
- Body aches, muscle soreness, fatigue, and the immune response to a virus can make the whole body feel run-down
- Sore throat, more common with colds than allergies, though post-nasal drip from either can cause mild throat irritation
- Thick, yellow or green mucus, mucus color does change over the course of a cold as white blood cells accumulate; color alone doesn’t confirm infection, but a shift from clear to colored often signals one
- Gradual onset, cold symptoms typically build over a day or two as the virus takes hold
- Someone else in the house is also sick; colds are contagious; allergies are not
Shared symptoms that don’t help you decide:
Runny nose, nasal congestion, sneezing, coughing, and general fatigue can appear in both conditions. Don’t try to make the call on these alone.
How Long Do Symptoms Last? Duration Is Your Biggest Clue
If there’s one question that cuts through the uncertainty fastest, it’s this: how long has this been going on?
A cold follows a fairly predictable timeline. Symptoms peak around days 2–3, then gradually improve. Most children feel significantly better within 7–10 days and are fully recovered by 14 days. If your child is still symptomatic at the two-week mark, it’s unlikely to still be the original cold.
Allergies don’t have an endpoint. As long as your child is being exposed to the allergen, pollen season, a dusty classroom, or a home with pets, symptoms persist. They don’t resolve in two weeks. They don’t resolve at all until the trigger is removed or managed. This is why children with undiagnosed seasonal allergies often look like they’ve had a cold for a month straight.
The other timing clue is how quickly symptoms start. Cold symptoms have an incubation period of 1–3 days after viral exposure before they appear. Allergy symptoms can begin within minutes of exposure to the allergen. If your child walks into a backyard full of freshly cut grass and, within 20 minutes, their eyes are streaming, and they can’t stop sneezing, that’s an allergic reaction, not a cold.
Can Your Child Have Both at the Same Time?
Yes, and it’s more common than many parents expect.
Children with allergies actually have a higher risk of catching frequent respiratory infections. Chronic nasal congestion from allergies creates an environment where viruses spread more easily. Inflamed, irritated nasal passages lose some of their natural protective function. And when you add nervous system dysregulation to the picture, which we’ll explain shortly, immune defense can be compromised in ways that make both conditions worse simultaneously.
The pattern to watch for: your child starts with what looks like classic allergy symptoms, then seems to get worse after a week, with new symptoms like fever, body aches, or thicker discharge. That can mean a secondary infection layered on top of an allergic reaction.
If you’re unsure, always consult a trusted healthcare provider. Sorting out what’s driving the symptoms is important for choosing appropriate care.
When Should You See a Doctor?
For either condition, watch for the following:
- Fever above 103°F or fever that lasts more than 3 days
- Symptoms that worsen rather than improve after 7–10 days
- Ear pain or significant ear congestion (possible ear infection)
- Facial pain or pressure around the sinuses that doesn’t ease (possible sinus infection)
- Difficulty breathing, wheezing, or chest tightness, both colds and allergies can trigger asthma, which requires prompt attention
- Signs present for more than 3 weeks without a clear explanation
For children whose allergy symptoms return every season, get triggered by the same environments consistently, or who seem to be “always sick,” a more thorough evaluation is worth pursuing. The chronic pattern is telling you something.
Why Some Kids Get Allergies and Others Don’t
This is where the conversation gets important.
Every child is exposed to pollen. Every child breathes in dust mites and pet dander. So why does one child develop chronic allergies while another doesn’t? The standard answer, “genetics and environment”, is partially true but very incomplete. It leaves out a critical variable: how well their immune system is regulated.
The immune system doesn’t operate in isolation. It’s tightly controlled by the nervous system, and specifically by the Autonomic Nervous System, the branch of the nervous system which regulates automatic functions like heart rate, digestion, inflammation, and immune response.
When the autonomic nervous system is balanced and working well, the immune system responds appropriately. It identifies real threats, mounts a defense, and stands down when the threat is gone. Harmless substances like pollen are recognized as harmless.
But when the nervous system is stuck in a state of chronic stress and sympathetic dominance, what we call the gas pedal of the nervous system being stuck on, the immune system loses that regulatory balance. It becomes hyperreactive, treating harmless substances as threats and mounting unnecessary inflammatory responses. That hyperreactivity shows up as allergies.
This isn’t a fringe idea. Research shows that prenatal stress increases immunoglobulin E (IgE) in newborns’ blood, a direct marker of heightened allergy risk, before the child has even encountered a single allergen. The immune system’s tendency to overreact is being shaped by nervous system stress that began in utero.
The Root Cause Most Parents Never Hear About
At PX Docs, we look at chronic allergies, especially in children who also struggle with recurring ear infections, gut issues, sleep problems, or sensory processing challenges, through the lens of what we call “The perfect Storm”.
The “Perfect Storm” describes how a combination of early neurological stressors accumulates during critical windows of development, creating lasting dysfunction in the nervous system. These stressors often include:
- Prenatal stress and elevated maternal cortisol affect fetal nervous system development
- Birth trauma and interventions, C-sections, forceps or vacuum delivery, prolonged or stalled labor, induction, and more that create physical stress and tension in the upper cervical spine
- Early childhood exposures, including frequent antibiotics, environmental toxins, poor sleep, and nutritional gaps
None of these factors alone would necessarily cause lasting problems. But their cumulative effect can push a developing nervous system into a chronic state of sympathetic dominance, and keep it there.
When sympathetic dominance becomes the baseline rather than a temporary stress response, the consequences affect every system in the body. Digestion is impaired. Sleep suffers. The immune system becomes dysregulated, prone to overreaction in the form of allergies, eczema, and recurring infections, while simultaneously struggling to mount adequate defenses against actual pathogens.
This is why so many parents notice their child doesn’t just have allergies. They also have chronic congestion, frequent colds, gut issues, and trouble sleeping. These aren’t separate problems. They’re the same underlying nervous system dysregulation, expressed across multiple systems.
The Nervous System–Immune System Connection
The vagus nerve is the primary communication highway between the brain and the body’s major organs, including the organs and tissues responsible for immune regulation. When vagus nerve function is compromised, that communication breaks down.
One of the consequences: the immune system doesn’t receive the proper brake signals that tell it when to stand down. An allergen shows up, histamine gets released, and the system has trouble returning to baseline. The result is prolonged, excessive inflammatory responses, the kind that keep children miserable for weeks every spring and fall.
Subluxation, neurological interference in the neurospinal system that disrupts brain-body communication, is a common contributor to this pattern, particularly when it involves the upper cervical vertebrae that sit at the base of the brainstem where the vagus nerve originates. When that area carries chronic tension and restriction, vagus nerve function is compromised, and immune regulation suffers downstream.
This is a neurological problem, not just an allergy problem. Antihistamines manage histamine after it’s released. They don’t address why the immune system is releasing it inappropriately in the first place.
What INSiGHT Scans Reveal About a Child’s Immune Challenges
One of the most powerful tools in Neurologically-Focused Chiropractic Care is INSiGHT scans, objective assessments of nervous system function that measure things like neuromuscular tension, autonomic regulation, and heart rate variability.
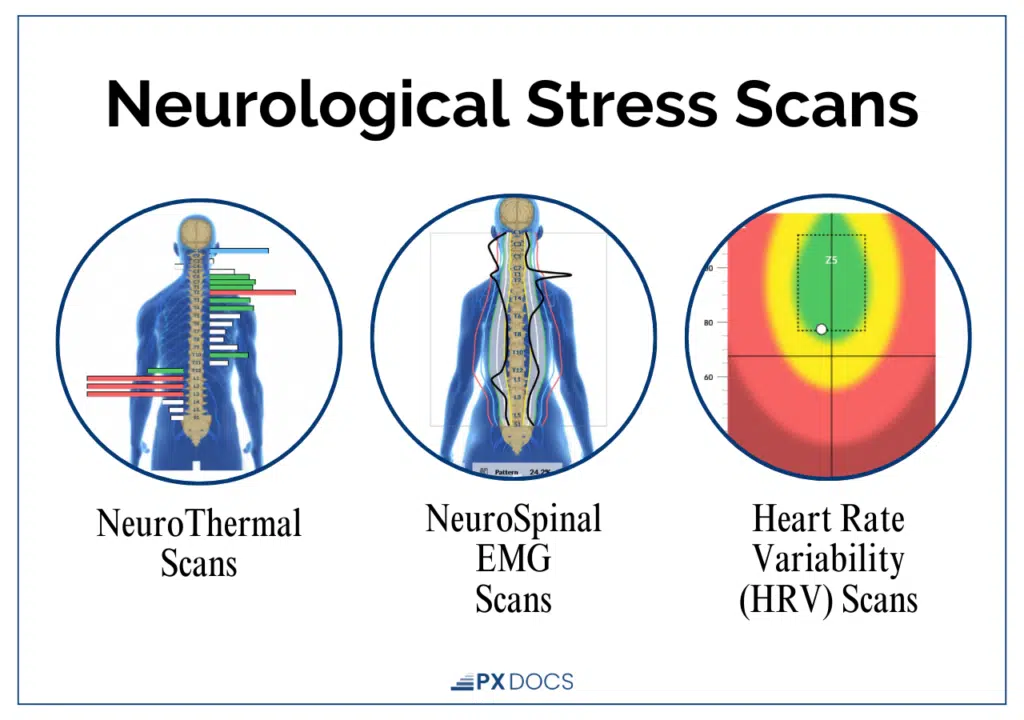
These scans don’t diagnose allergies. What they do is show parents and practitioners whether a child’s nervous system is functioning in a balanced, regulated state, or whether it’s carrying a chronic stress load that predisposes a child to immune dysregulation.
When scans show significant sympathetic dominance and poor vagal tone, it explains a lot:
- Why a child gets sick constantly.
- Why their allergies seem worse than other kids’
- Why antihistamines provide only partial relief.
- Why their sleep and gut function are also struggling.
The scan makes the invisible visible, giving families a starting point for addressing the root driver rather than just suppressing symptoms.
When Allergies Are More Than Just Allergies
Knowing the difference between a cold and allergies gets you to the right medication. But if your child deals with chronic, recurring immune challenges, seasonal allergies every year, a constant runny nose, recurring ear infections, “always sick” patterns, that pattern is telling you something about how their nervous system is running the show.
At PX Docs, we work with families who have tried antihistamines, nasal sprays, and allergy testing. They’ve managed the symptoms without ever getting to the underlying reason their child’s immune system is so reactive in the first place.
If that story sounds familiar, we’d encourage you to find a Neurologically-Focused Pediatric Chiropractor near you through the PX Docs directory. The first step is always an INSiGHT nervous system scan, an objective picture of whether your child’s nervous system is regulated enough to support a healthy, balanced immune response.
Because the goal isn’t managing allergies forever. It’s finding out why they won’t go away.