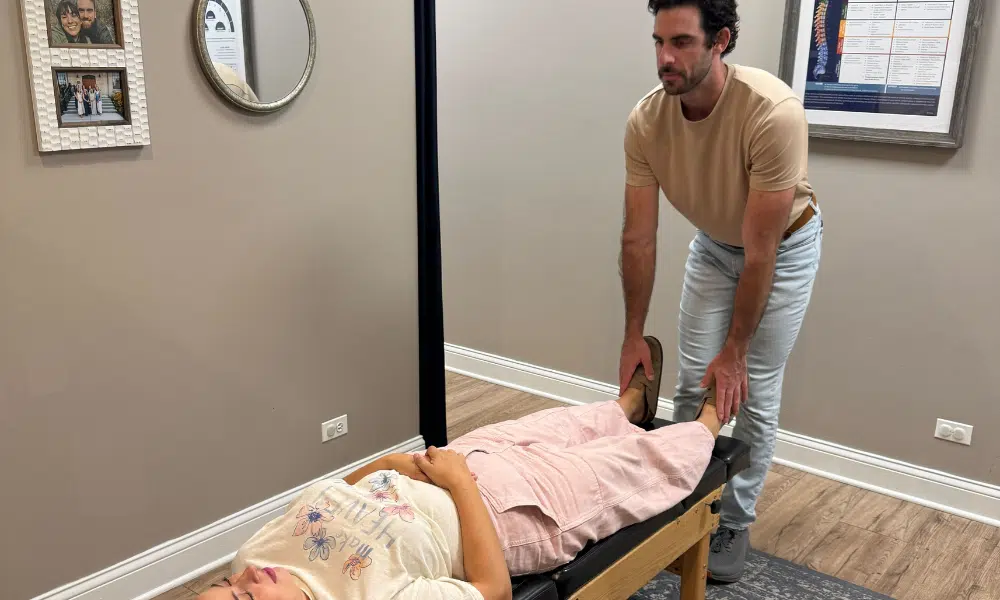
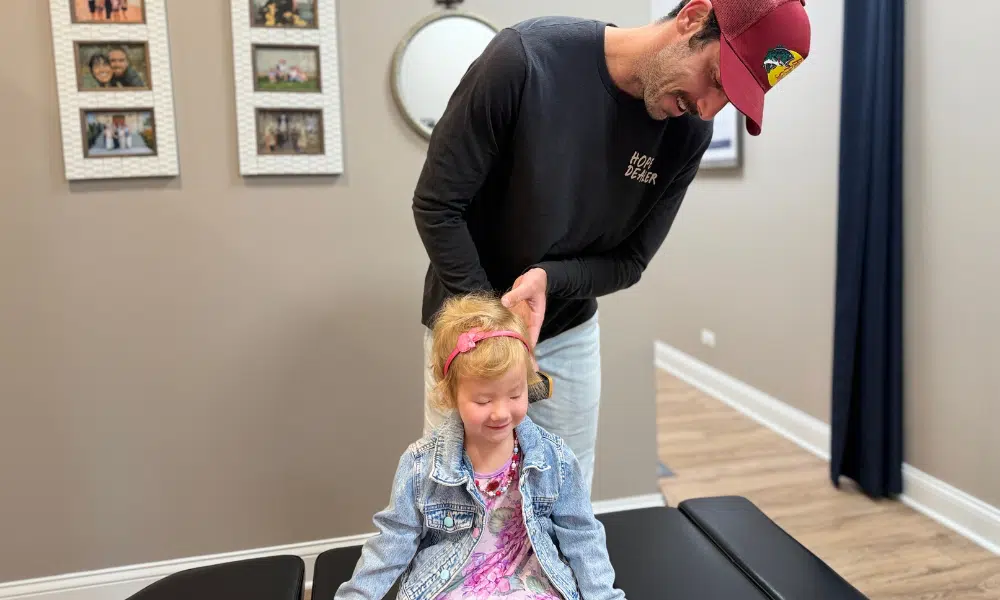
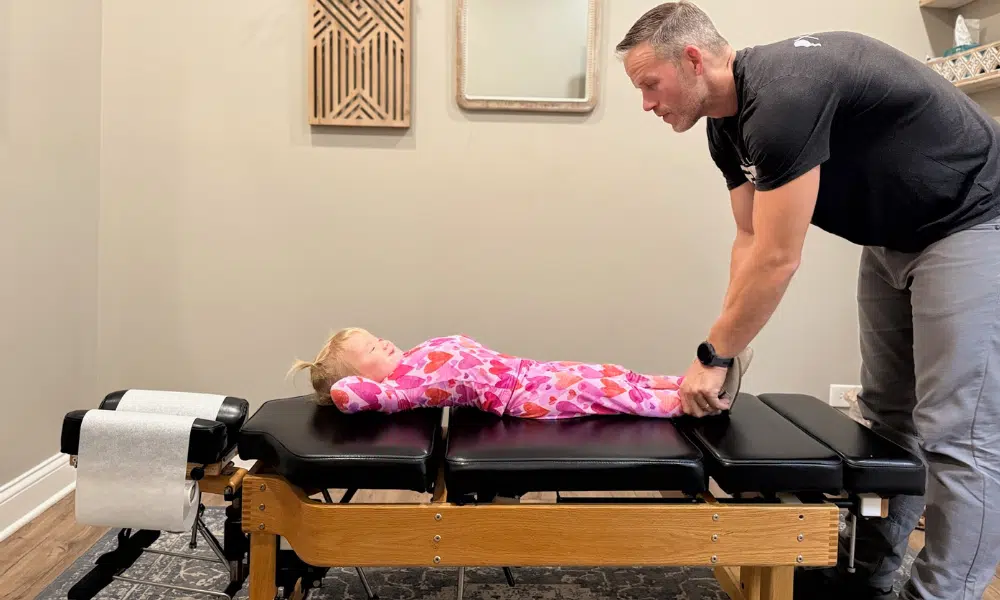
For years, coordination issues, anxiety, fatigue, and unexplained physical symptoms were brushed off as personality traits or stress. Coping strategies helped on the surface, but they required constant effort, turning everyday tasks into exhausting mental work.
What most resources on adult dyspraxia miss is that these challenges aren’t isolated problems. They’re connected through long-standing nervous system dysfunction, often shaped by early developmental stress. The body adapts to keep functioning, but those adaptations come at a cost.
The issue isn’t being “broken.” It’s a nervous system stuck in survival mode—and that can change.
Understanding Dyspraxia: More Than Just Coordination Difficulties
Dyspraxia, formally called Developmental Coordination Disorder (DCD), is a neurodevelopmental condition that affects motor coordination and movement. It affects approximately 5-6% of adults and is about four times more common in males. Despite assumptions, Dyspraxia has nothing to do with intelligence.
Here’s what the textbooks miss: Dyspraxia isn’t a standalone motor problem. It’s a manifestation of how your nervous system developed and adapted from the very beginning. The same nervous system controlling motor skills also regulates digestion, sleep, emotional responses, and cognitive function. When there’s interference in nervous system communication, you get a cluster of symptoms that seem unrelated but share the same root cause.
This isn’t about weak muscles or faulty joints. It’s about disrupted communication between your brain and body. The hardware works fine; the signal quality is often the problem.
Adult Dyspraxia Symptoms: The Complete Picture
Movement and Coordination Challenges
Fine motor skills—writing by hand, typing, buttoning shirts, applying makeup—require unexpectedly intense focus and take longer than they should. Gross motor difficulties affect balance and whole-body coordination. Walking through crowds means constantly bumping into people. Sports feel impossible. Many adults struggle to drive because the multiple simultaneous tasks can become overwhelming. Spatial awareness issues mean misjudging distances and knocking things over. Poor posture and low muscle tone contribute to chronic fatigue.
Cognitive and Executive Function Impacts
Time management is a constant struggle—you underestimate how long tasks take and manage deadlines poorly. Organizational skills suffer across the board. Working memory difficulties mean forgetting things mid-conversation or losing your train of thought. Learning new motor skills takes far longer than it does for others. Problems with sense of direction make navigation challenging.
Social and Emotional Effects
Social anxiety develops when you’ve spent years hiding coordination difficulties. You avoid situations where challenges might be exposed. In the workplace, you’re often underachieving relative to your intelligence because you’re slower than colleagues despite working twice as hard. Relationship challenges arise when partners don’t understand why everyday tasks are so difficult. Low self-esteem develops after years of being labeled “clumsy,” “disorganized,” or “lazy.”
Physical and Mental Health Connections
Chronic fatigue is almost universal—you sleep 8-10 hours and wake exhausted. This is neurological, not psychological. Your nervous system can’t shift into recovery mode.
Anxiety and depression are significantly more common, partly reactive but also neurological—when your nervous system is stuck in sympathetic dominance, anxiety is a symptom. Sleep disturbances, sensory processing sensitivities, and digestive issues (IBS, reflux, constipation) frequently accompany Dyspraxia.
Here’s the critical piece conventional medicine misses: your vagus nerve—connecting your brain to your digestive system—runs through your upper cervical spine, shoulders, chest, and abdomen. When there’s interference in that pathway, it affects both coordination and digestion. Your symptoms don’t exist in isolation. That’s dysautonomia, nervous system dysregulation affecting multiple body systems simultaneously.
Why Dyspraxia Rarely Comes Alone
ADHD (Attention Deficit Hyperactivity Disorder) is one of the most common co-occurring conditions, with substantial overlap in executive function impairments. Dyslexia, Autism Spectrum Disorder, Dyscalculia, anxiety, depression, and Sensory Processing Disorder all appear more frequently alongside Dyspraxia than in the general population.
Conventional medicine cares for these as separate conditions requiring separate care plans—occupational therapy for Dyspraxia, medication for ADHD, CBT for anxiety, and different therapy for Sensory Processing issues. You end up with a team of specialists, but nobody looks at the whole picture.
When you understand they all stem from nervous system dysregulation, it becomes clear: it’s not separate conditions randomly clustering together. It’s one nervous system struggling across multiple domains: motor control, attention, emotional regulation, and sensory processing. The same neurological interference disrupting motor coordination also disrupts attention and emotional regulation.
Address the root cause, and you create the foundation for improvement across all areas.
The Root Cause: Understanding the “Perfect Storm”
Conventional medicine says, “Dyspraxia is a lifelong condition”—learn to cope, build compensatory strategies, adapt to limitations. Each symptom gets its own specialist and care plan, but nobody asks why these problems cluster together. The underlying nervous system dysfunction never gets addressed.
At PX Docs, we call this combination “The Perfect Storm,” prenatal stress, birth trauma, and early childhood stressors creating a cascading effect during critical development windows. Think of it like stressing a plant while it’s sprouting—it doesn’t grow quite right.
1. Prenatal Stress: The Nervous System’s First Programming
The foundation often begins before a person is even born. When a mother experiences fertility challenges, chronic stress, anxiety, or unresolved trauma during pregnancy, elevated stress hormones like cortisol can cross the placenta and influence fetal nervous system development.
2. Birth Stress & Early Physical Trauma
Birth trauma is often the most significant contributor when it comes to dyspraxia because of how directly it impacts the brain–body communication system at its most vulnerable point. Forceps, vacuum extraction, emergency C-section, or prolonged labor all create abnormal pulling, twisting, or compressive forces on a newborn’s head and neck. This strain frequently concentrates in the upper cervical spine—exactly where the brainstem sits and where the vagus nerve exits the skull.
The brainstem acts as the primary relay station for motor planning, coordination, muscle tone, balance, and sensory integration. When stress or misalignment (subluxation) occurs in this area, signals traveling between the brain and the body can become distorted or delayed. For a developing nervous system, even subtle interference here can disrupt the timing, sequencing, and integration required for coordinated movement—challenges that are hallmarks of dyspraxia.
3. Early Childhood Stressors & Toxic Load
Early childhood stressors continue to shape nervous system development in powerful ways. Frequent antibiotic use can disrupt the gut–brain connection, chronic ear infections often require repeated medical interventions that add physical and neurological stress, and disrupted attachment patterns can keep a child’s nervous system stuck in a state of vigilance. Add in environmental toxin exposure and other modern stressors, and the result is a nervous system that never fully settles into regulation—creating ongoing patterns of dysregulation that can impact development, behavior, coordination, and resilience well into adulthood.
The Neurological Mechanism
Subluxation describes three things happening simultaneously: tension, fixation, and neurological interference. This isn’t about bones being “out of place.” It’s when tension and restriction in your neurospinal system disrupt nerve signals between your brain and body. Think of it as static on a phone line—the connection exists, but the message gets scrambled.
The most common site? Your upper cervical spine, where your skull meets your neck. This region houses your brainstem and is where the vagus nerve exits. When subluxation occurs here, it doesn’t just affect coordination; it affects everything that the brainstem and vagus nerve control.
Dysautonomia means your Autonomic Nervous System operates like a car with a stuck gas pedal and broken brakes. The sympathetic system (gas pedal—fight-or-flight) is chronically activated. The parasympathetic system (brake pedal—rest and digest) can’t engage. You’re stuck in sympathetic dominance.
This explains why:
- Coordination suffers (muscles are chronically tense)
- Anxiety persists (biochemically in stress mode)
- Digestion struggles (can’t activate “rest and digest”)
- Sleep is non-restorative (can’t downshift into recovery)
- Fatigue accumulates (burning stress hormones 24/7)
The vagus nerve is the main communication highway between your brain and body, running through your upper cervical spine—exactly where birth trauma and subluxation occur. When there’s interference, vagal tone decreases, affecting digestion, heart rate variability, immune function, emotional regulation, and coordination. This is why adults with Dyspraxia often have digestive issues—the same interference affecting the same nerve that controls both systems.
Getting a Diagnosis: What’s Available and What’s Missing
Conventional diagnosis relies on the Adult Developmental Coordination Disorders/Dyspraxia Checklist (ADC)—a self-report questionnaire—plus observation of motor tasks and medical history. A medical doctor makes the official diagnosis. The entire process is subjective, relying on self-reporting and observation with no objective measurement of nervous system function.
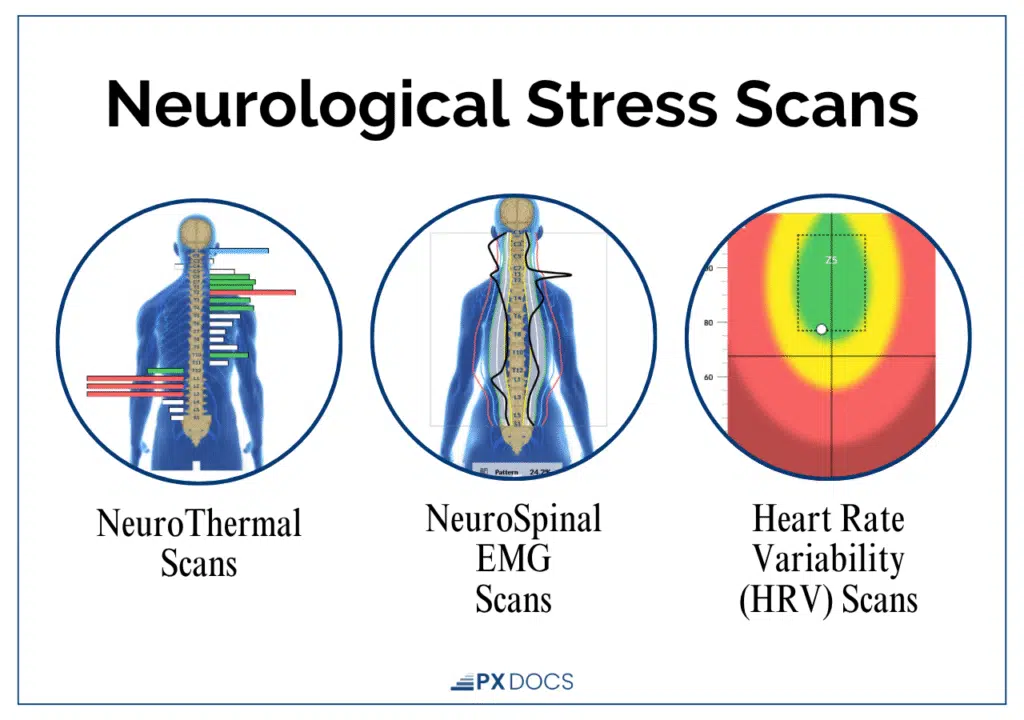
INSiGHT scanning technology provides an objective measurement.
- HRV (Heart Rate Variability) measures stress adaptation and shows whether you’re stuck in fight-or-flight.
- Surface EMG reveals neuromuscular tension patterns and subluxation indicators.
- Thermal scanning shows autonomic function and whether your sympathetic and parasympathetic systems are balanced.
These scans provide visual proof of what’s happening in your nervous system. This objective data allows for customized care plans tailored to your specific patterns and provides a baseline for tracking progress.
From Management to Root Cause
Occupational therapy, physical therapy, speech therapy, vision therapy, and even cognitive-based approaches can play an important role in supporting skills, function, and daily life. They help children adapt, practice, and build strategies to navigate challenges—and for many families, they’re a necessary part of the journey.
However, these therapies are designed to work with a regulated nervous system. When underlying nervous system stress and subluxation aren’t addressed, progress can be slower, harder to maintain, or plateau altogether. In those cases, therapy often becomes compensatory—teaching the child how to work around dysfunction rather than resolving what’s driving it.
When the nervous system is brought back into a state of regulation and safety, these same therapies tend to work more efficiently and effectively. Skills integrate faster, carry over more naturally, and require less constant effort. That’s not because the therapies were missing something—it’s because the foundation they rely on was finally restored.
Neurologically-Focused Chiropractic Care
This is where the conversation shifts to resolution. It’s important to note that this technology does not diagnose medical conditions, and Neurologically-Focused Chiropractic Care is certainly not a treatment or cure for Dyspraxia or any other condition, not even back pain. Instead, care focuses on restoring proper nervous system function.
Gentle, precise adjustments target subluxation where interference occurs. This isn’t bone-focused—it’s neurologically-focused. The goal is to remove interference and restore proper nerve signal transmission. When subluxation is addressed, brain-body communication improves. Your nervous system can reorganize and regulate better. The dysautonomia begins to resolve.
Here’s what we’ve seen in practice: when you address the root cause first, everything else works better. Occupational therapy becomes more effective. Physical therapy gains stick. Anxiety management techniques work because your nervous system isn’t biochemically stuck in stress mode.
Comprehensive support matters too: regular exercise, organizational tools, workplace accommodations, stress management, nutritional support, and adequate sleep all support nervous system healing. But these strategies become easier to implement when your nervous system isn’t in constant fight-or-flight mode.
Your Nervous System Can Heal
Conventional medicine says Dyspraxia is lifelong. But that perspective misses neuroplasticity—your nervous system’s ability to reorganize and heal at any age. When you remove neurological interference, your nervous system can function better.
You’re not broken. Your nervous system is stuck. And stuck can be unstuck.
Recovery doesn’t happen overnight, but with consistent care addressing subluxation, change happens in layers. Foundational functions often improve first: better sleep, easier digestion, reduced anxiety. These “neurological soft signs” show your nervous system is regulating better. Motor coordination improvements follow as brain-body communication strengthens.
This isn’t about perfection. It’s about reducing the exhaustion from constant compensation. It’s about your nervous system working with you instead of against you.
Next Steps: Getting the Help You Deserve
You’ve adapted long enough. It’s time to address the root cause.
PX Docs providers are trained in Neurologically-Focused Chiropractic Care for nervous system dysfunction. They’re equipped with INSiGHT scanning technology to objectively measure your nervous system function. Your first visit includes a comprehensive assessment with INSiGHT scans that show exactly what’s happening—where interference exists, how severe the dysautonomia is, and where subluxation patterns appear.
Care plans are individualized based on your specific nervous system patterns. PX Docs providers work collaboratively with your existing therapy team — care complements occupational therapy and physical therapy by addressing the foundation.Search for a PX Docs provider through our directory. You deserve to understand why you’ve struggled. You deserve care that addresses root causes, not just symptoms.