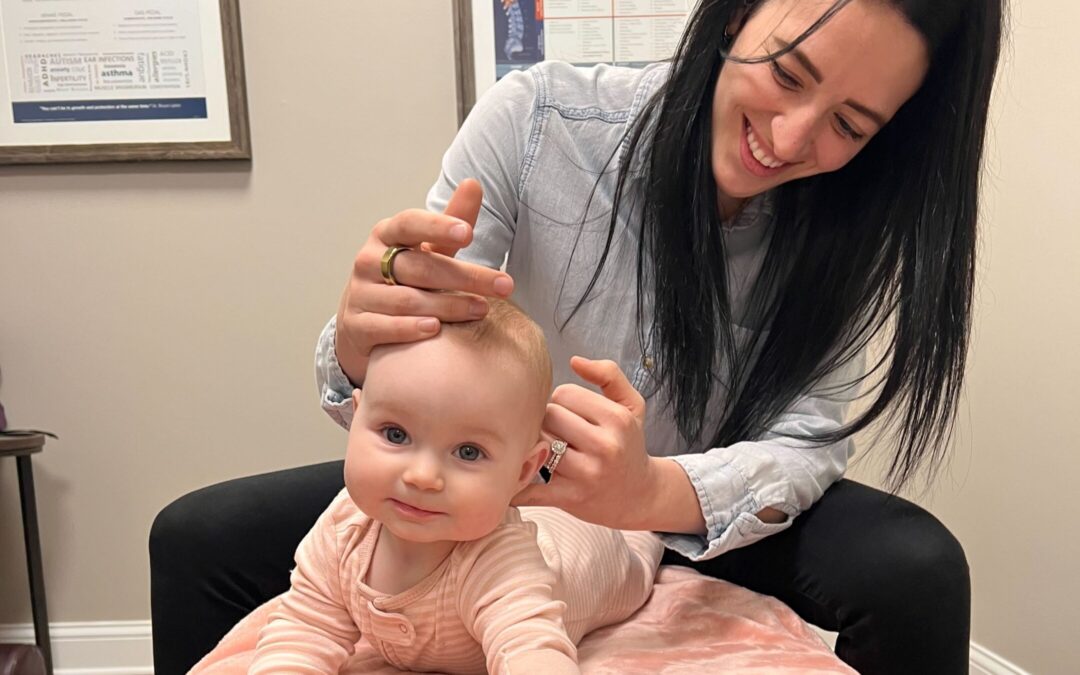
Living with sensory processing issues is challenging for both children and families. Such was the case for Aria and her family. According to her incredible parents, she was often an extremely unhappy little girl. She refused to be in unfamiliar places with unfamiliar people around her. When her family did try to go out, as they would occasionally try to, it would often end in Aria melting down because of sensory overload.
With Sensory Processing Disorder (SPD), the nervous system finds it challenging to receive, interpret, and respond appropriately to input from the senses. Today, 1 in every 6 children experiences sensory issues, but pediatricians frequently tell parents, “It’s just a phase, they’ll grow out of it.” In reality, early intervention is key to avoiding sensory struggles spiraling into long-term issues.
What Exactly is Sensory Processing Disorder?
Sensory Processing Disorder is a condition where children have difficulty processing sensory information from their environment and their own bodies.
Imagine entering a crowded, noisy carnival filled with glaring lights, potent smells, screaming kids, and rides spinning out of control. Instead of being an exciting and enjoyable environment as it is for most children, kids with sensory issues would immediately experience an overwhelmed nervous system and sensory overload. For children with Sensory Processing Disorder, that’s what daily life often feels like as their nervous system struggles to filter and regulate normal input most of us take for granted.
SPD can involve any of the senses:
- Auditory: noise and volume sensitivity
- Visual: bothered by bright or flickering lights
- Olfactory: strong odors are bothersome
- Gustatory: picky about food textures
- Tactile: irritated by certain fabrics or tags
- Vestibular: poor balance and coordination
- Proprioceptive: challenges sensing limbs in space
Out of all seven (7) senses, when it comes to pediatric neurodevelopment and overall brain function, proprioception is by far the most important.
While Sensory Processing Disorder frequently occurs with Autism Spectrum Disorder, they are separate conditions. Unlike autism’s pervasive developmental delays, children with sensory challenges may exhibit age-appropriate skills in some areas and pronounced sensory-based struggles in others.
Sadly, traditional pediatrician’s lack of answers or guidance leaves many parents confused and kids struggling as they await an explanation for their child’s frequent meltdowns, sleep challenges, picky eating, and other sensory issues.
Signs of Sensory Processing Disorder
Children with sensory issues might have what we call heightened oversensitivity or undersensitivey. In other words, they might be very sensitive to things like touch, sound, or smell, or they might not react much at all to any of those sensations. Sometimes, they even seek out sensory experiences because they need more input, leading to sensory-seeking behavior. Lots of kids have a mix of these sensory issues.
Signs of Oversensitivity (Hypersensitivity)
These children have overactive reactions to ordinary sensory input. Common signs include:
Infants:
- Excessive crying
- Difficulty feeding
Toddlers and Preschoolers:
- Extreme responses to textures, sounds, lights, smells, temperatures
- Frequent emotional meltdowns and tantrums
- Dislikes being touched unexpectedly
School-aged Children:
- Bothered by clothing tags and fabrics
- Avoids crowded, noisy places
- Covers eyes or ears frequently
All ages of children with hypersensitivity and sensory overload tend to struggle with sleep, digestion, constipation, and even respiratory or immune challenges.
Signs of Undersensitivity (Hyposensitivity):
In contrast, these children crave intense sensory input to satisfy sensory needs. Common signs include:
Toddlers and Preschoolers:
- Constantly touches people and textures
- Enjoys bear hugs and crashing play
- Fails to respond to loud sounds
School-aged Children:
- Chews on clothing or hands
- Poor sense of smell
- Risk-taking on playground equipment
Most children struggling with Sensory Processing Disorder exhibit elements of both hypersensitivity and hyposensitivity.
Recognizing Sensory Issues
Determining whether a child has sensory issues requires distinguishing them from regular developmental phases. If a child is persistently bothered by certain sensations or seeks them beyond the normal level, then evaluating them for Sensory Processing Disorder is necessary.
Sensory processing challenges can significantly impact a child’s health and development, and these effects can compound over time. Some of the most common impacts include:
- Learning and Concentration: Sensory sensitivities such as noise and light can overwhelm children in classroom settings, severely affecting their academic performance.
- Social and Emotional: Misinterpreting social cues and experiencing emotional dysregulation from sensory triggers can limit a child’s ability to make friends and can also contribute to anxiety or depression.
- Family Dynamics: Coping with unpredictable sensory-induced meltdowns can take a toll on parents and siblings, testing their patience and disrupting routines.
- Physical Issues: Sensory-motor coordination deficits may lead to clumsiness, delayed gross motor skills, and speech sound production problems.
- Other Developmental Delays: Sensory dysfunction, combined with associated learning and behavior challenges, can often cause speech, language, and even cognitive delays.
What Causes Sensory Processing Disorder?
While the conventional narrative paints an unclear picture of what causes Sensory Processing Disorder or overlooks it altogether, our “Perfect Storm” framework of cumulative stressors spanning from pregnancy through early childhood creates a series of stressors that lead to sensory challenges.
These developmental stressors include:
- High stress, high risk pregnancy and prenatal period
- Birth trauma and interventions
- Sleep challenges, colic, and constipation
- Early antibiotic use and nutritional deficiencies
- Exposure to environmental toxins
Under this model, the accumulated challenges from both prenatal stress and birth trauma chronically over-stimulates the sympathetic “fight-or-flight” nervous system, often leaving it “stuck” on and shifted into overdrive. Meanwhile, the counter-balancing parasympathetic nervous system, the “rest and digest” side, becomes suppressed and shut down.
This imbalance is called dysautonomia. If left unresolved, it leads to excessive neurological tension, known as subluxation, that directly disrupts sensory processing circuits. Essentially, the nervous system gets stuck in a hypersensitive sensory overload state, unable to return to baseline.
Subluxation, Dysautonomia, And The Vagus Nerve
To better understand the root causes of sensory dysfunction, it’s important to examine three key terms: subluxation, dysautonomia, and vagus nerve dysfunction.
- Subluxation refers to the build-up of tension, altered proprioception, and dysfunction or interference within the nervous system. This tension commonly interferes with the transmission of sensory signals.
- Dysautonomia occurs when the Autonomic Nervous System remains in a state of sympathetic dominance and loses its ability to return to a normal, regulated state. This can lead to problems with parasympathetic and vagal tone, which is essential for proper regulation of bodily functions.
- The Vagus Nerve is responsible for managing important parasympathetic functions, including immune responses, digestion, and social engagement behaviors. When vagal tone is low, these functions and sensory modulation can be impaired.
Adjustments release this stuck tension on the Sympathetic Nervous System and also seeks to stimulate or activate the Parasympathetic Nervous System and vagal tone, restoring the nervous system to an improved state of balance and function. Over time children then can often demonstrate improved emotional regulation, social cognition, learning behaviors, and physiologic balance.
Once Aria started Neurologically-Focused Chiropractic Care, her parents could not believe the positive changes they witnessed. She went from screaming and crying when anyone greeted her to smiling ear to ear, happily greeting anyone she met. Her sleep and speech significantly improved as well.
Chiropractic Care and Sensory Processing Disorder
The good news for parents whose children are struggling with Sensory Processing Disorder is that we now have cutting-edge technology that allows us to measure and assess nervous system dysfunction, subluxation, and dysautonomia directly. Our PX Docs network uses a set of advanced technologies called the INSiGHT Scans, which include thermal scanning, surface EMG, and heart rate variability (HRV) testing to objectively locate regions of subluxation and neurological dysfunction. These INSiGHT Scans are also used to continually monitor and assess progress as the care plan continues.
Optimal results come from addressing the real root cause of Sensory Processing Disorder and its resulting symptoms versus taking the “watch and wait” approach of conventional medicine. Also, if you’ve already been working with an incredible PT or OT on sensory processing therapies and have reached a plateau or are not seeing as fast of progress as you’d like, it could be that subluxation and dysautonomia are holding your child back from experiencing optimal results.
Sensory challenges should not shape a child’s future or disrupt family dynamics on a daily basis. With appropriate neurological care, a child’s nervous system can regain adaptability and move towards reaching developmental milestones, fostering socialization and enhancing focus without interference. Check out the PX Docs Directory to find a local PX Doc and get your child scheduled for a consultation and INSiGHT Scans today!